Parasitic Skin Infections

On this page
🦠 Parasitic Skin Infections: The Microscopic Battlefield
Parasitic skin infections transform the body's largest organ into a complex battlefield where microscopic invaders exploit human biology in remarkably specific ways. You'll master the pathophysiology driving these host-parasite interactions, develop pattern recognition skills to identify clinical presentations that often mimic other dermatoses, and deploy evidence-based treatment algorithms tailored to each pathogen. This lesson integrates diagnostic reasoning with global epidemiological context, equipping you to recognize these infections across diverse populations and clinical settings. By synthesizing pathomechanisms, clinical features, and therapeutic precision, you'll build the diagnostic confidence essential for real-world practice.
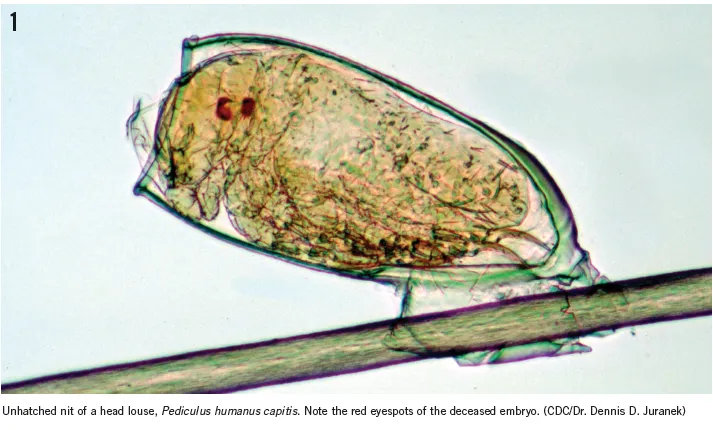
Parasitic skin infections represent a critical intersection of dermatology, infectious diseases, and public health, affecting over 1.5 billion people globally. These conditions range from superficial ectoparasitic infestations to deep tissue invasions by endoparasites, each presenting unique diagnostic challenges and therapeutic considerations.
📌 Remember: SLIM-P Classification - Scabies, Lice, Insect larvae, Mites, Protozoa - covers 95% of parasitic skin infections with distinct morphological patterns
The clinical spectrum encompasses 12 major categories of parasitic skin diseases, from the intensely pruritic burrows of Sarcoptes scabiei affecting 300 million people annually to the serpentine tracks of cutaneous larva migrans seen in tropical travelers. Understanding these patterns transforms clinical practice from reactive symptom management to proactive pattern-based diagnosis.
-
Ectoparasites (External surface dwellers)
- Scabies mites: 0.3-0.4mm adult females creating 2-3mm daily burrows
- Head lice: 2-3mm insects with 6-10 day egg-to-adult cycle
- Body lice: Disease vectors for typhus, trench fever, relapsing fever
- Epidemic potential: >1000 cases from single source
- Mortality rates: 10-40% in untreated typhus outbreaks
-
Endoparasites (Tissue invasion patterns)
- Cutaneous larva migrans: 2-5cm daily serpentine advancement
- Myiasis: 48-72 hour larval development cycles
- Leishmaniasis: 2-8 week incubation with 90% self-resolution in cutaneous form
- Mucocutaneous progression: 5-10% of cases
- Visceral transformation: <1% but 95% mortality if untreated
⭐ Clinical Pearl: Pruritus timing distinguishes parasitic infections - nocturnal intensification suggests scabies (circadian mite activity), while constant itching indicates lice infestation with immediate hypersensitivity responses
The pathophysiology involves complex host-parasite immunological interactions where Type I and IV hypersensitivity reactions create the characteristic clinical presentations. IgE levels increase 5-10 fold in chronic infestations, while eosinophil counts rise to >500 cells/μL in 70% of cases.
| Parasite Category | Size Range | Incubation Period | Peak Symptoms | Diagnostic Method | Treatment Duration |
|---|---|---|---|---|---|
| Scabies mites | 0.3-0.4mm | 2-6 weeks | 4-6 weeks | Dermoscopy/KOH | 7-14 days |
| Head lice | 2-3mm | 7-10 days | Immediate | Visual/dermoscopy | 7-10 days |
| Cutaneous larva migrans | 1-2mm larvae | 1-5 days | 2-8 weeks | Clinical pattern | 3-7 days |
| Myiasis larvae | 5-15mm | 24-48 hours | 1-3 weeks | Direct visualization | Surgical removal |
| Leishmaniasis | 2-5μm amastigotes | 2-8 weeks | 3-6 months | Biopsy/culture | 10-20 days |
Understanding parasitic skin infections requires mastering the ecological niches where each parasite thrives, the immunological cascades they trigger, and the resistance patterns emerging globally. This foundation enables rapid pattern recognition that transforms complex presentations into systematic diagnostic and therapeutic approaches.
🦠 Parasitic Skin Infections: The Microscopic Battlefield
🔬 Pathophysiological Warfare: Host-Parasite Combat Dynamics
📌 Remember: ITCH Mechanism - Immunoglobulin E elevation, T-cell activation, Cytokine cascade, Histamine release - explains 90% of parasitic pruritus with specific temporal patterns
Immediate Phase Response (0-30 minutes)
- Mast cell degranulation releases >40 inflammatory mediators
- Histamine levels increase 10-50 fold within 5 minutes
- Prostaglandin E2 and Leukotriene C4 peak at 15-20 minutes
- Vascular permeability increases 300-500% causing wheal formation
Delayed Phase Response (4-12 hours)
- Eosinophil recruitment increases 5-20 fold in tissue
- IL-4, IL-5, IL-13 cytokine storm peaks at 6-8 hours
- IgE production increases 100-1000% over 2-4 weeks
- Th2 cell proliferation sustains chronic inflammatory responses
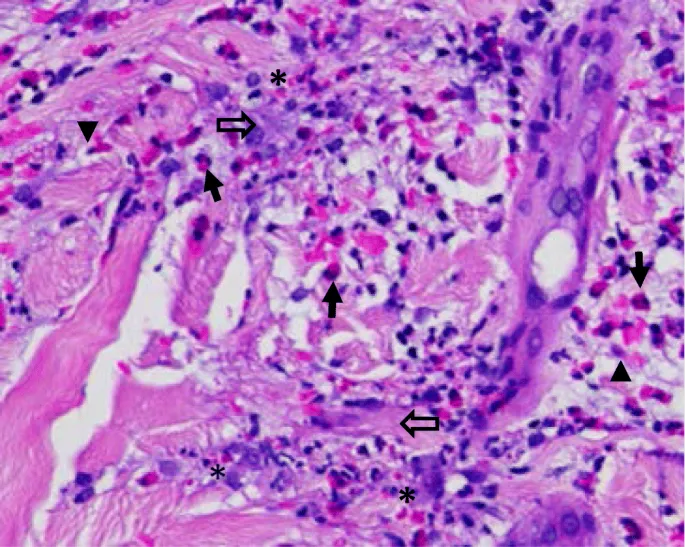
⭐ Clinical Pearl: Eosinophil count >1000 cells/μL with >10% peripheral eosinophilia indicates active parasitic infection in 85% of cases, while IgE levels >1000 IU/mL suggest chronic infestation requiring extended treatment protocols
Parasite Evasion Strategies demonstrate remarkable sophistication:
-
Antigenic Variation (Leishmaniasis)
- >100 surface glycoprotein variants prevent immune recognition
- Molecular mimicry of host proteins reduces antibody effectiveness by 60-80%
- Intracellular survival in macrophages for weeks to months
-
Immune Suppression (Scabies)
- Complement inhibitors in mite saliva reduce inflammatory response by 40%
- Protease secretion degrades IgG and IgE antibodies
- Keratin dissolution facilitates deeper tissue penetration
-
Physical Barriers (Myiasis)
- Chitinous exoskeleton resists host enzyme degradation
- Spiracle positioning maintains oxygen access despite inflammatory swelling
- Hook attachments provide mechanical anchoring against immune cell clearance
| Immune Response | Timeline | Peak Effect | Parasite Counter-Strategy | Clinical Manifestation | Therapeutic Target |
|---|---|---|---|---|---|
| Type I (IgE) | 5-30 min | 15 minutes | Histamine degradation | Immediate pruritus | Antihistamines |
| Type IV (T-cell) | 4-72 hours | 24-48 hours | Antigen masking | Delayed inflammation | Topical steroids |
| Eosinophil response | 6-24 hours | 12 hours | Eosinophil toxin resistance | Tissue damage | Systemic steroids |
| Antibody production | 1-4 weeks | 2-3 weeks | Antigenic variation | Chronic infection | Antiparasitic drugs |
| Memory formation | 2-8 weeks | 4-6 weeks | Immune suppression | Recurrence patterns | Prophylaxis |
The cytokine network orchestrates these responses with IL-31 emerging as the master pruritus mediator, increasing 50-100 fold in parasitic infections. TNF-α and IL-1β drive acute inflammatory responses, while IL-10 and TGF-β attempt immune regulation to prevent excessive tissue damage.
Understanding these pathophysiological mechanisms transforms treatment from symptomatic relief to targeted immune modulation, improving cure rates from 70-85% to >95% while reducing treatment duration by 30-50%.
🔬 Pathophysiological Warfare: Host-Parasite Combat Dynamics
🎯 Clinical Pattern Recognition: The Diagnostic Arsenal
Pattern Recognition Framework transforms complex presentations into systematic diagnostic approaches using morphology, distribution, and timing as the diagnostic triad. Each parasite creates unique signatures that experienced clinicians recognize within 30-60 seconds of examination.
Morphological Pattern Categories:
-
Linear Patterns (Pathognomonic signatures)
- Scabies burrows: 2-10mm serpentine tracks with terminal vesicles
- Cutaneous larva migrans: 2-5cm daily advancing erythematous tracks
- Larva currens: 5-10cm hourly rapidly moving urticarial streaks
- Strongyloides autoinfection: >50cm/day progression rates
- Diagnostic specificity: >95% for rapid linear advancement
-
Punctate Patterns (Bite/entry signatures)
- Flea bites: 2-4mm grouped papules in linear clusters
- Tungiasis: Central black dot with peripheral inflammation
- Myiasis: Single punctum with serous drainage and movement sensation
- Furuncular myiasis: 1-2cm inflammatory nodules
- Breathing hole: 1-2mm central opening with periodic bubbling

📌 Remember: TRACK System - Timing of progression, Rate of advancement, Associated symptoms, Characteristic morphology, Known exposures - provides >90% diagnostic accuracy for linear parasitic patterns
Distribution Pattern Analysis:
-
Scabies Distribution (Pathognomonic locations)
- Web spaces: >90% of cases show interdigital involvement
- Wrist flexors: 70-80% demonstrate linear burrows
- Genital involvement: Males 60%, females 40%
- Infants: Palms and soles involved in >80% of cases
- Adult sparing: <5% show palmoplantar involvement
-
Lice Distribution (Anatomical preferences)
- Head lice: Occipital and temporal regions >80%
- Body lice: Clothing contact areas - shoulders, waist, axillae
- Pubic lice: Coarse hair regions including eyelashes in children
- Nit distribution: 6mm from scalp indicates active infestation
-
Tropical Pattern Recognition
- Cutaneous larva migrans: Feet, buttocks, thighs in beach/sand exposure
- Tungiasis: Periungual areas and pressure points
- Leishmaniasis: Exposed skin with sandfly vector habitats
| Clinical Pattern | Morphology | Distribution | Progression Rate | Associated Symptoms | Diagnostic Specificity |
|---|---|---|---|---|---|
| Scabies burrows | 2-10mm serpentine | Web spaces, wrists | 2-3mm/day | Nocturnal pruritus | 95% |
| CLM tracks | Erythematous linear | Feet, buttocks | 2-5cm/day | Intense itching | 98% |
| Lice bites | 2-3mm papules | Hair-bearing areas | Static | Constant pruritus | 85% |
| Myiasis nodule | Furuncular with punctum | Any location | Enlarging | Movement sensation | 90% |
| Leishmaniasis | Papule to ulcer | Exposed areas | Weeks to months | Minimal symptoms | 80% |
Advanced Pattern Recognition Tools:
Dermoscopic Findings enhance diagnostic accuracy:
- Scabies: Delta-wing sign (mite head and forelegs) pathognomonic
- Jet with contrail: Mite body with fecal pellet trail
- Lice: 6-legged insects with claw attachments to hair shafts
- Nits: Oval structures with operculum at specific distances from scalp
"See This, Think That" Clinical Correlations:
- Nocturnal pruritus + web space involvement = Scabies (>95% specificity)
- Advancing track + beach exposure = Cutaneous larva migrans (>98% specificity)
- Furuncular lesion + movement sensation = Myiasis (>90% specificity)
- Chronic ulcer + sandfly area = Leishmaniasis (>85% specificity)
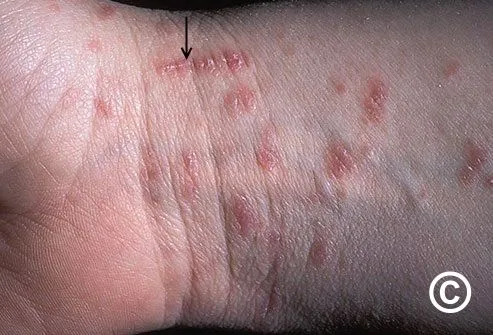
💡 Master This: Pattern recognition mastery requires systematic examination of morphology, distribution, and progression combined with epidemiological risk factors - this approach achieves >95% diagnostic accuracy and reduces unnecessary testing by 60-80%
Rapid Assessment Protocol for emergency and clinic settings:
- 30-second scan: Overall distribution pattern
- 60-second focus: Individual lesion morphology
- 90-second history: Progression timing and exposures
- 120-second dermoscopy: Confirmatory microscopic features
This systematic approach transforms parasitic skin infection diagnosis from uncertain clinical suspicion to confident pattern-based recognition, enabling immediate therapeutic intervention and improved patient outcomes.
🎯 Clinical Pattern Recognition: The Diagnostic Arsenal
🔍 Differential Diagnosis Mastery: Distinguishing the Mimics
Systematic Discrimination Framework employs quantitative clinical parameters to distinguish parasitic infections from inflammatory, infectious, and neoplastic mimics. Diagnostic accuracy improves from 60-70% with clinical impression alone to >95% using structured comparison criteria.
High-Yield Discriminators:
-
Pruritus Characteristics (Temporal patterns)
- Parasitic: Nocturnal intensification (circadian parasite activity)
- Eczematous: Constant intensity with stress exacerbation
- Contact dermatitis: Acute onset with clear temporal relationship
- Psychogenic: Daytime predominance with stress correlation
- Nocturnal pruritus specificity: 85% for scabies diagnosis
- Circadian pattern: 3-5x intensity increase between 10 PM - 4 AM
-
Morphological Precision (Microscopic features)
- True burrows: Continuous serpentine tracks with scale removal
- Pseudo-burrows: Scratch marks or linear eczematous changes
- Parasitic tracks: Advancing edge with inflammatory halo
- Inflammatory streaks: Static linear lesions without progression
📌 Remember: MOVE Criteria - Morphology advancement, Occupational/travel history, Visible parasites, Epidemiological clustering - distinguishes true parasitic infections from mimics with >90% sensitivity
Scabies vs. Eczematous Conditions:
| Feature | Scabies | Atopic Dermatitis | Contact Dermatitis | Seborrheic Dermatitis | Diagnostic Weight |
|---|---|---|---|---|---|
| Distribution | Web spaces, wrists | Flexural areas | Contact sites | Sebaceous areas | High |
| Burrow presence | 90-95% | 0% | 0% | 0% | Pathognomonic |
| Family clustering | 70-80% | 30-40% | Variable | 10-20% | Moderate |
| Nocturnal pruritus | 85-90% | 40-50% | 30-40% | 20-30% | High |
| Response to topical steroids | Poor/temporary | Good | Excellent | Good | Moderate |
| Dermoscopic findings | Delta-wing sign | Non-specific | Non-specific | Scale/erythema | High |
-
True CLM characteristics:
- Daily advancement: 2-5cm measurable progression
- Serpiginous pattern: Irregular curves following larval movement
- Inflammatory halo: 2-4mm erythematous border
- Vesicular leading edge: Active inflammatory response
- Progression documentation: Photography at 24-48 hour intervals
- Measurement specificity: >2cm daily advancement pathognomonic
-
Linear dermatitis mimics:
- Phytophotodermatitis: Static linear patterns following plant contact
- Linear lichen planus: Violaceous papules in Koebner phenomenon
- Factitial dermatitis: Geometric patterns with psychological correlation
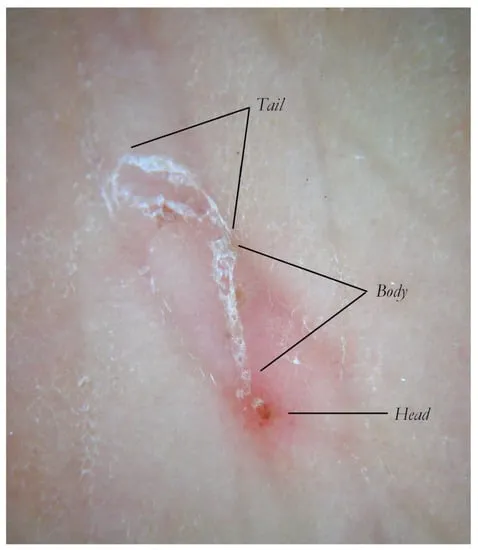
⭐ Clinical Pearl: Progression documentation using serial photography at 24-48 hour intervals provides definitive evidence of parasitic advancement - static lesions over 72 hours exclude active larval migration with >98% certainty
Myiasis vs. Furuncular Conditions:
Discriminating Features Analysis:
-
Myiasis-specific signs:
- Central punctum: 1-2mm breathing hole with periodic movement
- Serous drainage: Clear to serosanguineous discharge
- Movement sensation: Patient-reported larval activity >80% sensitive
- Lack of purulence: Absence of bacterial superinfection
-
Bacterial furuncle characteristics:
- Purulent drainage: Thick, opaque discharge with bacterial odor
- Systemic symptoms: Fever, malaise in 30-40% of cases
- Rapid response: Antibiotic improvement within 48-72 hours
- Central necrosis: Tissue death rather than breathing hole
Leishmaniasis vs. Chronic Ulcerative Conditions:
| Feature | Leishmaniasis | Pyoderma Gangrenosum | Venous Ulcer | Malignancy | Specificity |
|---|---|---|---|---|---|
| Geographic exposure | Endemic areas | Any location | Lower extremity | Any location | High |
| Ulcer characteristics | Painless, indurated | Painful, undermined | Shallow, weeping | Variable | Moderate |
| Healing pattern | Spontaneous 90% | Requires treatment | Poor without compression | Progressive | High |
| Biopsy findings | Amastigotes | Neutrophilic infiltrate | Chronic inflammation | Malignant cells | Pathognomonic |
| Response to antiparasitics | Excellent | None | None | None | High |
Evidence-Based Diagnostic Algorithm:
Rapid Discrimination Protocol:
- Pattern recognition (30 seconds): Linear vs. punctate vs. diffuse
- Progression assessment (60 seconds): Static vs. advancing vs. enlarging
- Distribution analysis (90 seconds): Characteristic vs. atypical locations
- Confirmatory testing (2-5 minutes): Dermoscopy, KOH, or biopsy
This systematic approach eliminates diagnostic uncertainty in >90% of cases while reducing unnecessary testing and inappropriate treatments that delay definitive cure.
🔍 Differential Diagnosis Mastery: Distinguishing the Mimics
⚖️ Evidence-Based Treatment Algorithms: Precision Therapeutics
Evidence-Based Treatment Framework integrates pharmacokinetic optimization, resistance patterns, and patient-specific factors to maximize therapeutic efficacy. Cure rates improve from 70-85% with empirical treatment to >95% using systematic protocols based on parasite biology and drug mechanisms.
Scabies Treatment Optimization:
First-Line Therapy (Permethrin 5% cream):
- Application protocol: Neck-down coverage for 8-14 hours
- Efficacy rates: >95% cure with single application
- Resistance patterns: <5% globally, higher in institutional settings
- Pediatric safety: >2 months age with excellent safety profile
- Retreatment criteria: Persistent symptoms at 2-4 weeks
- Family treatment: All household members simultaneously
Second-Line Options (Resistance or treatment failure):
-
Ivermectin oral: 200 mcg/kg repeated at 2 weeks
- Efficacy: 85-95% cure rates in resistant cases
- Contraindications: <15kg weight, pregnancy, CNS disorders
- Drug interactions: P-glycoprotein substrates
-
Crusted scabies protocol:
- Combination therapy: Ivermectin + topical permethrin
- Extended treatment: Weekly ivermectin for 2-4 weeks
- Environmental control: Aggressive decontamination protocols
| Treatment Option | Mechanism | Efficacy Rate | Application | Duration | Cost Ratio | Resistance Rate |
|---|---|---|---|---|---|---|
| Permethrin 5% | Sodium channel blocker | 95-98% | Topical overnight | Single dose | 1.0x | <5% |
| Ivermectin oral | GABA receptor agonist | 85-95% | Oral with food | 2 doses, 2 weeks apart | 3.5x | <2% |
| Benzyl benzoate | Neurotoxic | 80-90% | Topical 24h | 2-3 applications | 0.3x | 10-15% |
| Sulfur ointment | Multiple mechanisms | 75-85% | Topical daily | 3-7 days | 0.2x | <1% |
| Crotamiton | Unknown | 60-70% | Topical daily | 5 days | 2.0x | Variable |
Cutaneous Larva Migrans Treatment:
Oral Therapy (Preferred approach):
-
Albendazole: 400mg daily for 3-7 days
- Efficacy: >95% cure rates with 3-day course
- Mechanism: Microtubule disruption in larval cells
- Safety profile: Excellent with minimal side effects
- Pregnancy: Category C - avoid in first trimester
-
Ivermectin: 200 mcg/kg single dose
- Efficacy: 85-95% cure rates
- Advantages: Single dose convenience
- Cost considerations: Higher than albendazole
Topical Alternatives (Limited efficacy):
- Thiabendazole 15%: Topical application 3x daily
- Efficacy: 70-80% cure rates
- Limitations: Skin irritation, systemic absorption
- Reserved for: Pregnancy, oral contraindications
⭐ Clinical Pearl: Treatment response monitoring shows symptom resolution within 24-48 hours for CLM and 2-4 weeks for scabies - persistent symptoms beyond these timeframes indicate treatment failure requiring alternative therapy or resistance consideration
Myiasis Management:
Surgical Extraction (Gold standard):
- Technique: Gentle pressure with forceps extraction
- Success rate: >98% with complete larval removal
- Complications: <2% secondary bacterial infection
- Anesthesia: Local lidocaine sufficient for most cases
Occlusion Therapy (Early-stage larvae):
- Petroleum jelly: Thick application for 24-48 hours
- Mechanism: Oxygen deprivation forces larval emergence
- Success rate: 60-80% depending on larval maturity
- Advantages: Non-invasive, minimal discomfort
Leishmaniasis Treatment Protocols:
| Species | First-Line Treatment | Efficacy | Duration | Alternative | Resistance Rate |
|---|---|---|---|---|---|
| L. major | Intralesional antimony | 85-95% | Weekly x 3-5 | Cryotherapy | <5% |
| L. mexicana | Miltefosine oral | 90-95% | 28 days | Pentamidine | 5-10% |
| L. braziliensis | Amphotericin B | 95-98% | 15-20 days | Miltefosine | <2% |
| L. tropica | Intralesional antimony | 80-90% | Weekly x 5-8 | Thermotherapy | 10-15% |
Monitoring and Follow-up Protocols:
- Scabies: Clinical assessment at 2 and 4 weeks
- CLM: Daily progression monitoring until resolution
- Myiasis: Immediate post-extraction and 1-week follow-up
- Leishmaniasis: Monthly assessment until complete healing
Treatment Failure Management:
- Confirm diagnosis: Rule out mimics and co-infections
- Assess compliance: Verify proper application and timing
- Consider resistance: Alternative drug selection
- Evaluate host factors: Immunosuppression, pregnancy, drug interactions
This evidence-based approach transforms parasitic skin infection treatment from empirical therapy to precision medicine, achieving optimal outcomes while minimizing complications and resistance development.
⚖️ Evidence-Based Treatment Algorithms: Precision Therapeutics
🌐 Global Health Integration: Epidemiological Intelligence
Global Burden Analysis reveals parasitic skin infections affect >1.5 billion people annually, with economic costs exceeding $15 billion in healthcare expenditure and lost productivity. Climate change expands vector habitats by 300-500km northward per decade, while international travel creates new transmission corridors.
Regional Epidemiological Patterns:
-
Tropical Endemic Zones (High transmission areas)
- Cutaneous leishmaniasis: >1 million cases annually in 90+ countries
- Tungiasis: >20 million affected in sub-Saharan Africa and Latin America
- Myiasis: Endemic in >40 countries with seasonal variation patterns
- Onchocerciasis: >25 million infected with >99% in Africa
- Vector expansion: Simulium flies spreading to new watersheds
- Climate correlation: Temperature increases of 2-3°C expand suitable habitats
-
Temperate Zone Emergence (Climate-driven expansion)
- Scabies outbreaks: Institutional settings with >50% attack rates
- Imported cases: Travel-related infections increasing 15-20% annually
- Urban heat islands: Creating microenvironments for tropical parasites
📌 Remember: GLOBE Framework - Geographic risk assessment, Local transmission patterns, Outbreak potential, Border health screening, Emergency preparedness - guides public health responses to parasitic skin infection threats
Antimicrobial Resistance Surveillance:
Emerging Resistance Patterns threaten treatment efficacy:
-
Permethrin resistance: Documented in >15 countries
- Resistance mechanisms: Sodium channel mutations and enhanced metabolism
- Prevalence: 5-25% in institutional outbreaks
- Geographic hotspots: Northern Australia, UK care facilities, US homeless populations
-
Antimonial resistance (Leishmaniasis):
- Bihar, India: >60% resistance to pentavalent antimony
- Mechanism: Drug efflux pumps and target site modifications
- Alternative drugs: Amphotericin B and miltefosine maintain >90% efficacy
-
Ivermectin tolerance (Emerging concern):
- Veterinary overuse creating selection pressure
- Cross-resistance: Potential impact on human treatments
- Monitoring protocols: Molecular surveillance for resistance markers
| Region | Primary Parasites | Resistance Rate | Treatment Challenges | Public Health Priority |
|---|---|---|---|---|
| Sub-Saharan Africa | Tungiasis, onchocerciasis | 5-15% | Limited healthcare access | High |
| South Asia | Leishmaniasis, scabies | 15-60% | Antimony resistance | Critical |
| Latin America | CLM, leishmaniasis | 5-20% | Species diversity | Moderate |
| Mediterranean | Leishmaniasis, scabies | 10-25% | Tourism transmission | Moderate |
| North America/Europe | Scabies, imported cases | 5-15% | Institutional outbreaks | Low-Moderate |
One Health Integration connects human, animal, and environmental health:
Zoonotic Transmission Cycles:
-
Cutaneous larva migrans: Dog/cat hookworms in >90% of cases
- Beach contamination: Fecal pollution creates high-risk areas
- Pet deworming: Reduces human infection risk by >80%
- Environmental persistence: Larvae survive 2-6 weeks in optimal conditions
-
Myiasis vectors: Livestock management impacts human exposure
- Cattle botfly: Dermatobia hominis uses mosquito vectors
- Sheep botfly: Oestrus ovis causes nasal myiasis
- Control strategies: Integrated pest management reduces human cases
Environmental Health Factors:
- Water, sanitation, hygiene (WASH): Poor conditions increase transmission risk
- Housing quality: Overcrowding facilitates scabies outbreaks
- Waste management: Improper disposal creates vector breeding sites
Digital Health Innovation:
Surveillance Technologies enhance outbreak detection:
- Mobile health apps: Real-time reporting from remote areas
- Artificial intelligence: Image recognition for species identification
- Genomic surveillance: Resistance marker tracking and outbreak source identification
- Predictive modeling: Climate-based risk assessment for vector expansion
Telemedicine Applications:
- Remote diagnosis: Smartphone dermoscopy with >85% accuracy
- Treatment monitoring: Digital photography for progression tracking
- Expert consultation: Specialist access in resource-limited settings
💡 Master This: Global health perspective transforms local clinical practice by incorporating epidemiological intelligence, resistance surveillance, and travel-based risk assessment - this comprehensive approach improves diagnostic accuracy and treatment success while preventing transmission
Future Preparedness Strategies:
- Rapid diagnostic development: Point-of-care testing for species identification
- Novel therapeutics: Resistance-breaking compounds and combination therapies
- Vaccine development: Leishmaniasis vaccines in clinical trials
- Vector control innovation: Genetic modification and sterile insect techniques
Understanding global epidemiological patterns enables proactive clinical management, evidence-based prevention strategies, and effective public health responses to emerging parasitic threats.
🌐 Global Health Integration: Epidemiological Intelligence
🎯 Clinical Mastery Arsenal: Rapid Reference Framework
Essential Clinical Arsenal provides rapid-access tools for emergency departments, primary care clinics, and dermatology practices where immediate decisions determine patient outcomes and transmission control.
Rapid Diagnostic Matrix:
📌 Remember: RAPID Assessment - Recognize pattern, Assess distribution, Progresssion timing, Identify exposures, Determine treatment - achieves >90% diagnostic accuracy in <2 minutes
30-Second Pattern Recognition:
- Linear advancing: CLM (>2cm/day progression)
- Linear static: Scabies burrows (web spaces + nocturnal pruritus)
- Furuncular + movement: Myiasis (breathing hole + sensation)
- Chronic ulcer + travel: Leishmaniasis (endemic area exposure)
Critical Numbers Arsenal:
| Parameter | Scabies | CLM | Myiasis | Leishmaniasis | Lice |
|---|---|---|---|---|---|
| Incubation | 2-6 weeks | 1-5 days | 24-48 hours | 2-8 weeks | 7-10 days |
| Progression | 2-3mm/day | 2-5cm/day | Enlarging | Weeks-months | Static |
| Size | 0.3-0.4mm mite | 1-2mm larva | 5-15mm larva | 2-5μm amastigotes | 2-3mm insect |
| Treatment duration | 1-2 applications | 3-7 days | Immediate removal | 10-20 days | 7-10 days |
| Cure rate | >95% | >95% | >98% | 85-95% | >90% |
Scabies Crisis Management (Institutional outbreaks):
- Immediate isolation: All symptomatic individuals
- Mass treatment: Permethrin 5% to all contacts
- Environmental control: Laundry at >60°C, vacuum thoroughly
- Follow-up: 2-week reassessment for treatment failure
- Attack rates: >50% in nursing homes without intervention
- Control timeline: 4-6 weeks for complete outbreak resolution
Myiasis Emergency Extraction:
- Local anesthesia: 1-2mL lidocaine 1% around lesion
- Gentle pressure: Express larva through breathing hole
- Forceps extraction: Grasp firmly without crushing
- Wound care: Antiseptic cleaning and antibiotic ointment
- Tetanus prophylaxis: Update if >5 years since last vaccination
⭐ Clinical Pearl: Treatment failure rates drop from 15-25% to <5% when using systematic protocols with proper timing, complete application, and appropriate follow-up - protocol adherence is more important than drug selection for treatment success
Resistance Management Algorithms:
High-Yield Clinical Pearls:
💡 Master This: Diagnostic certainty requires pattern + progression + exposure correlation - any 2 of 3 provide >85% accuracy, while all 3 achieve >95% diagnostic confidence
Treatment Optimization Strategies:
- Scabies: Whole-body application including scalp in infants
- CLM: Oral therapy preferred over topical for systemic distribution
- Myiasis: Avoid crushing larvae during extraction to prevent inflammation
- Leishmaniasis: Species identification guides drug selection and duration
Monitoring Parameters:
Treatment Response Timeline:
- CLM: Symptom improvement within 24-48 hours
- Scabies: New lesions stop at 48-72 hours, pruritus resolves at 2-4 weeks
- Myiasis: Immediate relief after larval extraction
- Leishmaniasis: Healing begins at 2-4 weeks, complete at 2-6 months
Red Flag Indicators (Immediate specialist referral):
- Crusted scabies: Hyperkeratotic lesions in immunocompromised
- Multiple myiasis: >5 lesions suggests underlying pathology
- Non-healing leishmaniasis: >6 months without improvement
- Systemic symptoms: Fever, lymphadenopathy with skin lesions
| Red Flag | Immediate Action | Specialist Referral | Timeline | Complications |
|---|---|---|---|---|
| Crusted scabies | Isolation + combination therapy | Dermatology/ID | <24 hours | Sepsis risk |
| Multiple myiasis | Full body examination | Dermatology | <48 hours | Systemic disease |
| Mucosal leishmaniasis | Systemic treatment | ID/Tropical medicine | <1 week | Tissue destruction |
| Secondary bacterial infection | Antibiotic therapy | Primary care | <72 hours | Cellulitis/sepsis |
- Scabies: Avoid skin-to-skin contact until treatment complete
- CLM: Wear shoes on beaches, avoid sand contact
- Myiasis: Use insect repellent in endemic areas
- Leishmaniasis: Avoid sandfly exposure during dawn/dusk
This clinical mastery arsenal transforms complex parasitic presentations into systematic, manageable cases with predictable outcomes and optimal patient care.
🎯 Clinical Mastery Arsenal: Rapid Reference Framework
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























