Occupational Infections: Introduction - Bugs on the Job
- Infections acquired or worsened due to workplace biological agent exposure.
- Key risk factors:
- Contact: Infected animals/humans, contaminated materials.
- Environment: Soil, water, air.
- Host: Skin breaks, immunosuppression.
- High-risk occupations: Healthcare, agriculture, veterinary, laboratory, sanitation.
- Common transmission: Inhalation, ingestion, skin/mucous membrane contact.
- Prevention pillars: PPE, hygiene, vaccination, engineering controls.
⭐ Many occupational infections are zoonotic (e.g., Anthrax, Brucellosis, Leptospirosis), particularly affecting agricultural and animal handling professions.
Occupational Bacterial Infections - Skin's Tiny Terrors
- Key risk: Contact with animals, animal products, soil, contaminated water.
- Erysipeloid:
- Erysipelothrix rhusiopathiae; from fish, meat.
- Violaceous, well-defined, tender plaque (hands/fingers).
- Tx: Penicillin.
- Cutaneous Anthrax:
- Bacillus anthracis; from animal hides, wool.
- Painless papule → vesicle → ulcer → central black eschar; surrounding edema.
- Tx: Ciprofloxacin, Doxycycline.
⭐ The characteristic painless black eschar of cutaneous anthrax is a key diagnostic clue.
- Tuberculosis Cutis:
- Mycobacterium tuberculosis.
- Forms: Lupus vulgaris (apple-jelly nodules), Scrofuloderma, TB verrucosa cutis (prosector's wart).
- Tx: Anti-TB drugs.
- Atypical Mycobacteria (M. marinum):
- "Fish tank granuloma"; from contaminated water.
- Papules/nodules (hands), sporotrichoid spread. Culture at 25-33°C.
- Tx: Clarithromycin.
- Brucellosis:
- Brucella spp.; from infected animals/dairy.
- Non-specific skin lesions; systemic symptoms (fever, arthralgia).
- Tx: Doxycycline + Rifampin.
Occupational Fungal & Viral Infections - Spores & Spots at Work
Fungal Infections:
- Sporotrichosis ("Rose Gardener's Disease"): Sporothrix schenckii.
- Occ: Gardeners, florists, farmers, miners.
- Feat: Nodules, ulcers along lymphatics (lymphocutaneous spread).
- Dermatophytoses (Ringworm): Trichophyton, Microsporum spp.
- Occ: Animal handlers (e.g., T. verrucosum from cattle), farmers, athletes.
- Feat: Annular, scaly lesions.
- Candidiasis: Candida albicans.
- Occ: Wet work (dishwashers, bakers), healthcare.
- Feat: Intertrigo, paronychia.
Viral Infections:
- Orf (Contagious Pustular Dermatitis): Parapoxvirus.
- Occ: Sheep/goat handlers.
- Feat: Papulovesicular lesions, targetoid appearance; self-limiting.
- Milker's Nodule: Parapoxvirus.
- Occ: Cattle handlers.
- Feat: Firm, painless nodules on hands.
- Herpetic Whitlow: Herpes Simplex Virus (HSV).
- Occ: Healthcare workers.
- Feat: Painful vesicles on fingers.
- Molluscum Contagiosum: Poxvirus.
- Occ: Wrestlers, swimmers.
- Feat: Pearly, umbilicated papules.
📌 Orf from Ovine (sheep), Milker's from Moo-cows.
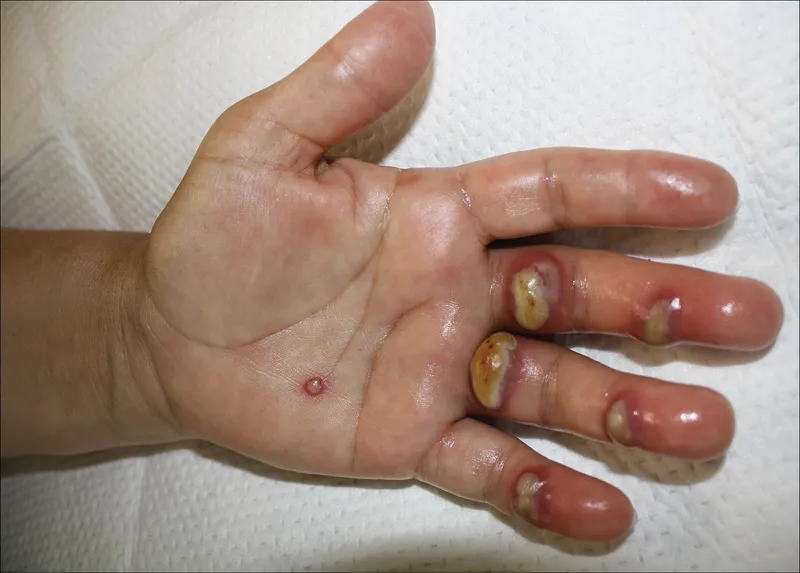
⭐ Sporotrichosis classically presents with lymphocutaneous spread - lesions track along lymphatic channels, often described as "sporotrichoid" spread.
Occupational Parasitic Infestations & Prevention - Unwelcome Workplace Guests
- Key Infestations & Risks:
- Scabies: (S. scabiei) Healthcare/animal workers. Nocturnal pruritus, burrows. Tx: Permethrin 5% cream, oral Ivermectin.
- Pediculosis: (Lice) Workers with close contact/shared gear. Itching, nits. Tx: Permethrin 1% lotion.
- Cutaneous Larva Migrans (CLM): (Hookworm larvae) Farmers, gardeners, plumbers. Serpiginous, intensely pruritic tracks. Tx: Albendazole, Ivermectin.
- Myiasis: (Fly larvae) Outdoor workers. Painful, boil-like lesions with central punctum. Tx: Occlusion, surgical removal.
- Leishmaniasis (Cutaneous): (Leishmania spp.) Forestry/agricultural workers (endemic areas). Chronic non-healing skin ulcers.
- General Prevention Strategies:
- Personal Protective Equipment (PPE): Gloves, appropriate footwear, coveralls.
- Personal Hygiene: Frequent handwashing, regular bathing.
- Environmental Measures: Pest control, proper sanitation, vector control.
- Health Education: Awareness of risks, early symptom reporting.
- Prompt diagnosis & treatment of affected individuals to prevent spread.

⭐ Cutaneous Larva Migrans is frequently acquired by skin contact (e.g., walking barefoot) with soil contaminated by dog or cat feces containing hookworm larvae; common in agricultural workers and gardeners.
High‑Yield Points - ⚡ Biggest Takeaways
- Erysipeloid: E. rhusiopathiae in butchers, fishermen; violaceous, sharply demarcated hand lesions.
- Orf: Parapoxvirus from sheep/goats; targetoid nodule, central umbilication/crusting.
- Milker's Nodule: Parapoxvirus from cattle; similar to Orf, often firmer, less inflamed lesions.
- Cutaneous Anthrax: B. anthracis from animal products; painless papule to black eschar with marked edema.
- Tuberculosis Cutis Verrucosa: M. tuberculosis in pathologists, butchers; warty, hyperkeratotic plaque.
- Herpetic Whitlow: HSV on fingers of healthcare workers; painful grouped vesicles.
- Sporotrichosis: S. schenckii in gardeners; nodules along lymphatics (lymphocutaneous).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


