Electrosurgery - Shocking Science Stuff
- Uses high-frequency (HF) alternating current (0.5 - 4 MHz) to cut, coagulate, desiccate, or fulgurate tissue. Avoids neuromuscular stimulation (faradic effect < 100 kHz).
- Tissue Effects: Depend on waveform, power, time, electrode.
- Cutting: Continuous waveform; rapid heating, vaporization.
- Coagulation: Interrupted waveform; slower heating, protein denaturation.
- Fulguration: Non-contact sparking; superficial charring.
- Desiccation: Direct contact; deeper tissue dehydration.
- Modes:
- Monopolar: Current path: active electrode → patient → dispersive (grounding) pad.
- ⚠️ Risk: Grounding pad burns if poor contact/small size.
- Bipolar: Current confined between two closely spaced electrode tips. No grounding pad needed; generally safer.
- Preferred for delicate tissues & patients with pacemakers.
- Monopolar: Current path: active electrode → patient → dispersive (grounding) pad.
- 📌 Cutting Continues (Continuous waveform for cutting).
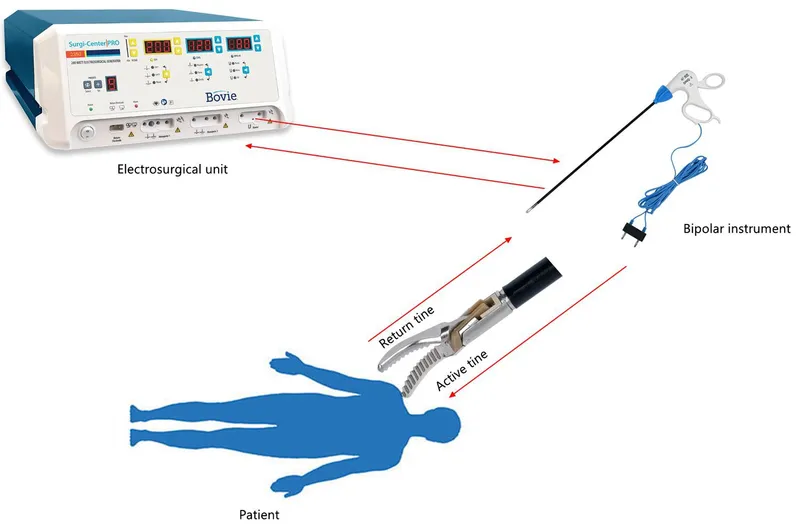
⭐ Bipolar electrosurgery is generally preferred in patients with cardiac pacemakers or implantable cardioverter-defibrillators (ICDs) to minimize electromagnetic interference and current diversion through the device lead system.
Electrosurgery - Zap That Lesion!
Utilizes high-frequency AC ($> \textbf{100}$ kHz, typically 0.5-2.5 MHz) for controlled tissue destruction or cutting via heat.
- Modes:
- Monopolar: Active electrode delivers current; patient completes circuit via dispersive plate. Risk of burns if poor contact.
- Bipolar: Current confined between electrode tines. No dispersive plate. Safer for pacemakers/ICDs.
- Waveforms & Tissue Effects:
- Damped (interrupted, high voltage): Dehydration, coagulation. For desiccation, fulguration, coagulation.
- Undamped (continuous): Vaporization, cutting. For electrosection.
| Technique | Current | Electrode | Depth | Key Uses |
|---|---|---|---|---|
| Electrodesiccation | Damped | Touches | Superficial | Warts, SKs, acrochordons, molluscum |
| Electrofulguration | Damped | Spark Gap | Superficial | Fine surface ablation, similar to desiccation |
| Electrocoagulation | Damped | Touches | Deeper | Hemostasis, telangiectasias, pyogenic granulomas |
| Electrosection | Undamped | Touches | Cutting | Biopsies, excisions (nevi, skin tags), debulking |
⭐ In electrosection, a pure "cutting" current (fully filtered, undamped) produces the least lateral heat damage, ideal for obtaining biopsy specimens with minimal thermal artifact.
Electrosurgery - Handle With Care!
Electrosurgery uses high-frequency electrical current for cutting, coagulation, desiccation, or fulguration. Safety is paramount.
-
Key Safety Principles:
- Dispersive Electrode (Return Pad):
- Large, well-vascularized area (e.g., thigh).
- Avoid bony prominences, scars, metal implants.
- Ensure full, firm contact. ⚠️ Prevents burns.
- Pacemakers/ICDs:
- Bipolar mode strongly preferred.
- Monopolar: short bursts, lowest power, orient current path away from device. Cardiology input.
- Flammable Agents: Ensure alcohol preps are completely dry.
- Smoke Evacuation: Mandatory; smoke contains carcinogens, irritants.
- Dispersive Electrode (Return Pad):
-
Common Modes:
- Monopolar: Active electrode delivers current; passes through patient to dispersive pad.
- Cutting: Continuous waveform. Coagulation: Interrupted.
- Bipolar: Current confined between instrument tips. No dispersive pad. Safer for delicate areas, pacemakers.
- Monopolar: Active electrode delivers current; passes through patient to dispersive pad.
-
Potential Complications:
- Burns (active or dispersive site).
- Surgical smoke hazards.
- Fire/Explosion (rare).
- Electromagnetic interference with devices.
-
Contraindications:
- Absolute: Patient refusal.
- Relative: Pregnancy (cautious use, avoid pelvis/fetus).
⭐ Bipolar electrosurgery is generally safer in patients with pacemakers/ICDs as the electrical current is confined between the instrument tips, minimizing systemic passage.
High‑Yield Points - ⚡ Biggest Takeaways
- Electrosurgery utilizes high-frequency alternating current for tissue destruction (e.g., cutting, coagulation).
- Monopolar mode requires a dispersive (patient return) electrode; current passes through the patient.
- Bipolar mode confines current between two active electrodes; safer, no dispersive plate needed.
- Cutting current is continuous (undamped); coagulation current is intermittent (damped waveform).
- Fulguration creates a spark to superficial tissue; desiccation dehydrates tissue via direct contact.
- Key risks include burns, pacemaker interference (especially with monopolar), and surgical smoke hazards.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

