ICD: Definition & Pathophysiology - Skin's Angry Reaction
- Definition: Non-allergic skin inflammation from direct chemical/physical injury.
- Epidemiology: Most common contact dermatitis (≈80% cases); major occupational hazard in India (e.g., wet work, chemicals).
- Pathophysiology:
- Direct cytotoxic effect on keratinocytes.
- Non-immunological, dose-dependent reaction.
- Skin barrier disruption (lipid lamellae, proteins).
- Innate immune activation (release of cytokines, chemokines).
⭐ ICD is a non-allergic inflammatory reaction of the skin caused by direct injury from an offending agent, accounting for approximately 80% of all contact dermatitis cases.
oka
ICD: Etiology & Risk Factors - Trouble Makers List
Common Irritants:
| Irritant Type | Examples/Sources |
|---|---|
| Strong Irritants | Acids (e.g., hydrochloric), Alkalis (e.g., caustic soda) |
| Weak/Cumulative Irritants | Soaps, Detergents, Solvents, Water (wet work), Cutting oils, Cement |
- Host Factors:
- Atopy (eczema)
- Age (extremes: very young, elderly)
- Site (thin skin, e.g., eyelids; occluded areas)
- Environmental/Occupational Factors:
- Occupation (healthcare, cleaning, construction, hairdressing)
- Climate (low humidity, cold weather)
⭐ Chronic exposure to 'wet work,' involving frequent hand washing or prolonged contact with water, is a major occupational risk factor for developing irritant hand dermatitis.
ICD: Clinical Features - Skin's SOS Signals
| Feature | Acute ICD | Chronic ICD |
|---|---|---|
| Symptoms | Burning, stinging, pain > itching | Itching, dryness, fissuring pain |
| Signs/Morphology | Erythema, edema, vesicles, bullae, erosions; well-demarcated | Dryness, scaling, lichenification, hyperkeratosis, fissures; ill-defined borders |
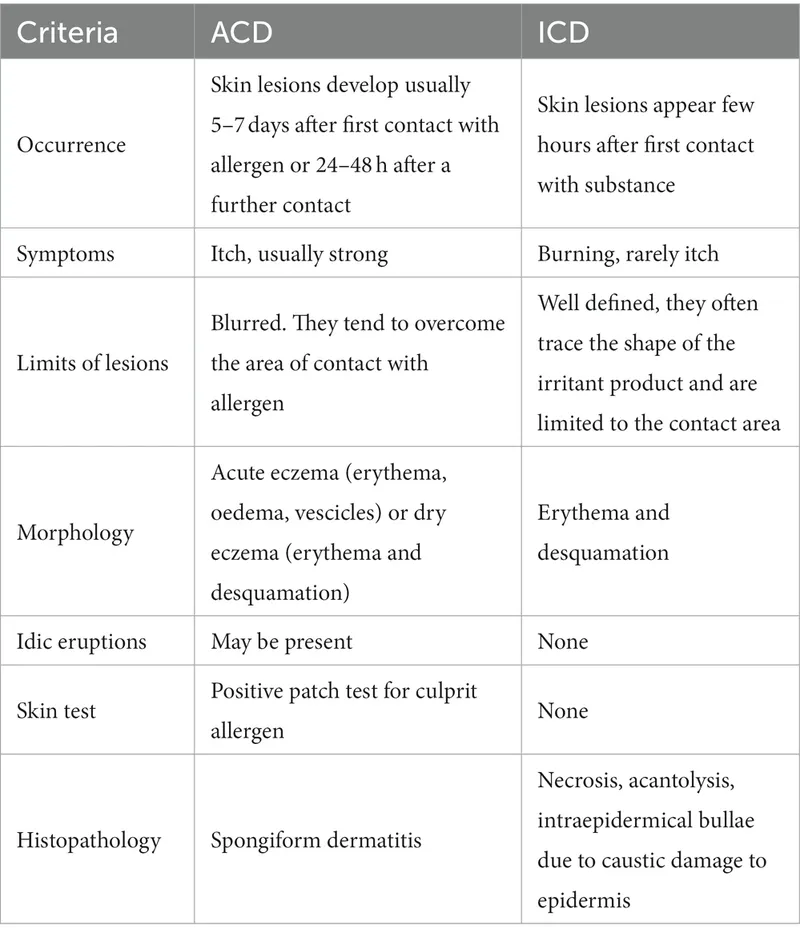
⭐ In acute ICD, symptoms like burning and stinging often predominate over itching, which is more characteristic of allergic contact dermatitis (ACD).
ICD: Diagnosis & Differentials - Spotting the Irritant
- Diagnostic Approach:
- History: Crucial. Identify potential irritants, exposure (duration, concentration, occlusion).
- Clinical Exam: Erythema, edema, vesicles (acute); scaling, lichenification, fissures (chronic). Often well-demarcated.
- Patch Testing:
- Primarily to exclude concomitant Allergic Contact Dermatitis (ACD).
- Typically negative to allergens in pure ICD.
⭐ Patch testing in suspected ICD is primarily performed to exclude an overlapping allergic contact dermatitis, as pure ICD will yield negative patch test results to allergens.
- Key Differentials: ACD, atopic dermatitis, seborrheic dermatitis, psoriasis, tinea.
ICD: Management & Prevention - Soothe & Shield Plan
- Main Goals: Alleviate symptoms, resolve dermatitis, prevent recurrence.
- Core Strategies:
- Irritant Identification & Avoidance: Paramount for resolution.
- Skin Barrier Restoration: Emollients (liberal, frequent use), barrier creams, gentle cleansing.
- Pharmacological Therapy:
- Topical Corticosteroids (TCS): Potency tailored to site; e.g., medium potency (e.g., triamcinolone 0.1%) for trunk/limbs, low potency (e.g., hydrocortisone 1%) for face/flexures. Short-term use for acute flares.
- Topical Calcineurin Inhibitors (TCIs): Off-label option, especially for sensitive areas or long-term intermittent use.
- Systemic Therapy: Oral corticosteroids or immunosuppressants for severe, widespread cases.
- Preventive Measures:
- Patient education on irritants and skin care.
- Use of appropriate personal protective equipment (PPE).
⭐ The cornerstone of managing irritant contact dermatitis is the identification and complete avoidance of the causative irritant, coupled with diligent skin barrier repair using emollients.
High‑Yield Points - ⚡ Biggest Takeaways
- Non-immunologic inflammation from direct cytotoxic effect; no prior sensitization required.
- Most common contact dermatitis, more prevalent than allergic type.
- Acute: erythema, vesicles, bullae, burning, stinging. Chronic: scaling, lichenification, fissures.
- Lesions are sharply demarcated, typically on exposed areas (e.g., hands).
- Patch test is negative, differentiating from Allergic Contact Dermatitis (ACD).
- Management: irritant avoidance, emollients, and topical corticosteroids.
- Common irritants: soaps, detergents, solvents, acids, alkalis, chronic wet work.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

