STA Basics - Ideal Filler Facts
- Definition: Soft Tissue Augmentation (STA) involves injecting materials to augment soft tissues.
- Goals: Volume restoration (e.g., lips, cheeks), facial contouring, wrinkle/scar correction.
- Ideal Filler Properties:
- Biocompatible, non-immunogenic, non-migratory.
- Reversible/biodegradable, consistent/predictable results.
- Cost-effective, long-lasting (not permanent), easy to inject.
⭐ Hyaluronic acid (HA) fillers are popular due to their reversibility with hyaluronidase enzyme an antidote effect for HA fillers..
Filler Classification - Material Matrix
By Duration of Effect:
| Class | Material | Duration | Examples | Pro / Con |
|---|---|---|---|---|
| Temporary | Hyaluronic Acid (HA) | <6-12 mos | Restylane | Reversible / Short-acting |
| Temporary | Collagen | <6-12 mos | Zyderm | Natural / Allergy test |
| Semi-Permanent | Calcium Hydroxylapatite (CaHA) | 1-2 yrs | Radiesse | Collagenesis / Nodules |
| Semi-Permanent | Poly-L-Lactic Acid (PLLA) | 1-2 yrs | Sculptra | Gradual / Sessions |
| Permanent | Polymethylmethacrylate (PMMA) | >2 yrs | Bellafill | Permanent / Irreversible |
| Permanent | Silicone | >2 yrs | Silikon 1000 | Permanent / Migration |
- Autologous: Fat, PRP
- Biological: Hyaluronic Acid (HA), Collagen
- Synthetic: CaHA, PLLA, PMMA
⭐ Hyaluronic acid fillers are popular due to their reversibility with hyaluronidase.
Hyaluronic Acid - HA Gold Standard
- Most common filler; natural glycosaminoglycan (GAG) in ECM.
- Properties: Highly hydrophilic, viscoelastic.
- Mechanism: Achieves volume expansion; stimulates neocollagenesis.
- Cross-linking (e.g., BDDE) enhances longevity & G' (stiffness/firmness).
- Types: Monophasic (homogenous) vs. Biphasic (particulate).
- Advantages: Reversible with hyaluronidase; good safety profile.
- 📌 Hyaluronidase: Typical dose 5-10 units/0.1mL HA (nodules); 200-300 units (vascular occlusion).
- Disadvantages: Temporary results (biodegradable).

⭐ G' (elastic modulus) is a key HA property: higher G' provides more lift and projection (e.g., cheeks), lower G' for superficial lines.
Other Fillers - Notable Alternatives
- Calcium Hydroxylapatite (CaHA; Radiesse): CaHA microspheres. Biostimulatory, radio-opaque. For deep folds, volume. Longevity: 12-18 months.
- Poly-L-Lactic Acid (PLLA; Sculptra): Induces collagenesis. Gradual effect over 2-3 sessions. Requires specific dilution & injection.
- Polymethylmethacrylate (PMMA; Bellafill): Permanent PMMA microspheres in bovine collagen (skin test required). Granuloma risk.
- Autologous Fat: Natural, for large volumes. Disadvantages: unpredictable resorption, more invasive procedure.
⭐ PLLA (Sculptra): Optimal results often need 3 sessions (4-6 weeks apart).
Injection Strategy - Safe Shots Guide
- Pre-procedure: Consent, photos, anesthesia (topical/local).
- Techniques: Linear threading, fanning, cross-hatching, serial puncture, layering. Needle for precision, cannula for safety.
- Depth: Dermal, subdermal, supraperiosteal-varies by product/area.
- ⚠️ Danger Zones: Facial a., angular a., infraorbital a./n., mental a./n., temporal vessels. Know these!
- Post-procedure: Ice, avoid pressure/massage.
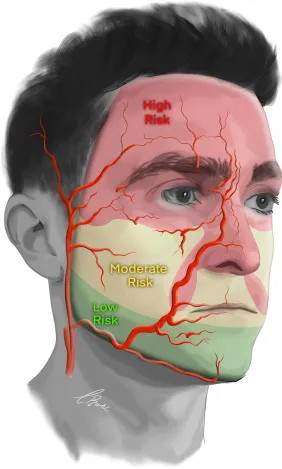
⭐ Slow injection technique and thorough anatomical knowledge are paramount to prevent vascular occlusion.
Adverse Events - Filler Mishap Rx
- Early: Bruising, swelling, erythema, pain, asymmetry, Tyndall effect (superficial HA), infection, hypersensitivity.
- ⚠️ Vascular Occlusion (VO): Critical Emergency!
- Signs: Severe pain, blanching, livedo reticularis, impending necrosis, visual changes.
- Rx: See flowchart. Key: High-dose pulsed hyaluronidase.
- Late: Nodules, granulomas, biofilms, migration.
⭐ Immediate, aggressive use of high-dose pulsed hyaluronidase is crucial for suspected Hyaluronic Acid (HA) filler vascular occlusion to prevent necrosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Hyaluronic acid (HA): most common, reversible (hyaluronidase), Tyndall effect if superficial.
- Calcium hydroxylapatite (CaHA): longer-lasting, stimulates collagen, radiopaque.
- Poly-L-lactic acid (PLLA): biostimulatory, gradual results over months, requires multiple sessions.
- Autologous fat: biocompatible, variable resorption, technique-dependent.
- Vascular occlusion: critical emergency, causes necrosis; manage with hyaluronidase for HA.
- Common sites: nasolabial folds, lips, cheeks, marionette lines.
- Avoid NSAIDs pre-procedure to minimize bruising.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

