Pemphigus Vulgaris: Intro - Skin's Betrayal Saga
- Autoimmune intraepidermal blistering disease.
- Antibodies target desmosomal proteins: Desmoglein 3 (Dsg3) primarily in mucosal; Dsg1 in skin.
- Loss of keratinocyte adhesion (acantholysis).
- Incidence: 0.1-0.5 per 100,000; higher in Ashkenazi Jews, Mediterranean, Indian populations.
- Mean age of onset: 40-60 years.
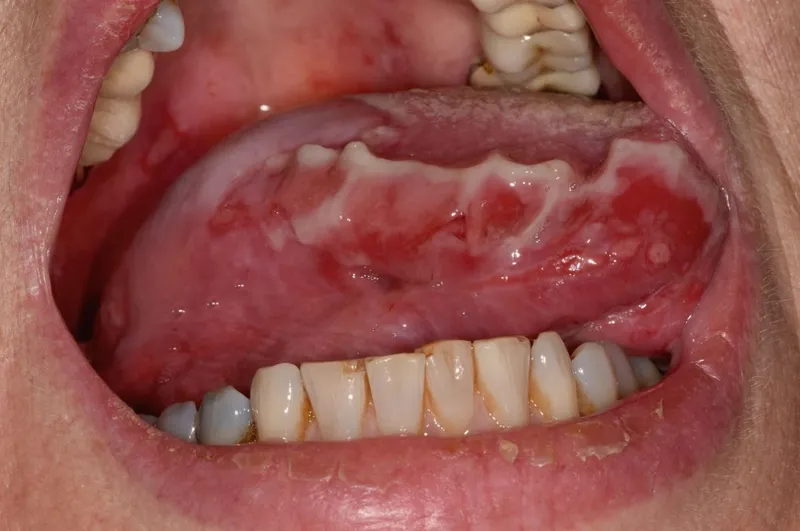
⭐ Nikolsky's sign: Gentle rubbing of perilesional skin causes blister formation or extension of existing blister. Indicates active disease and epidermal fragility due to acantholysis. Common in Pemphigus Vulgaris but not specific.
Pemphigus Vulgaris: Clinical Features - Blistering Blues
- Primary Lesions: Flaccid, thin-walled bullae (blisters) on normal or erythematous skin.
- Easily rupture, leaving painful erosions.
- Content: Clear fluid.
- Mucosal Involvement:
- Oral mucosa is the first site in ~50-70% of cases.
- Painful erosions, difficulty eating.
- Other mucous membranes: conjunctiva, nasal, pharyngeal, laryngeal, esophageal, genital.
- Skin Involvement:
- Common sites: Scalp, face, neck, axillae, groin, trunk, pressure points.
- Lesions can be widespread.
- Key Signs:
- Nikolsky's sign: Gentle rubbing of perilesional/normal skin induces blistering or epidermal separation.
- Asboe-Hansen sign (Bulla spread sign): Lateral pressure on an intact bulla extends it to adjacent skin.
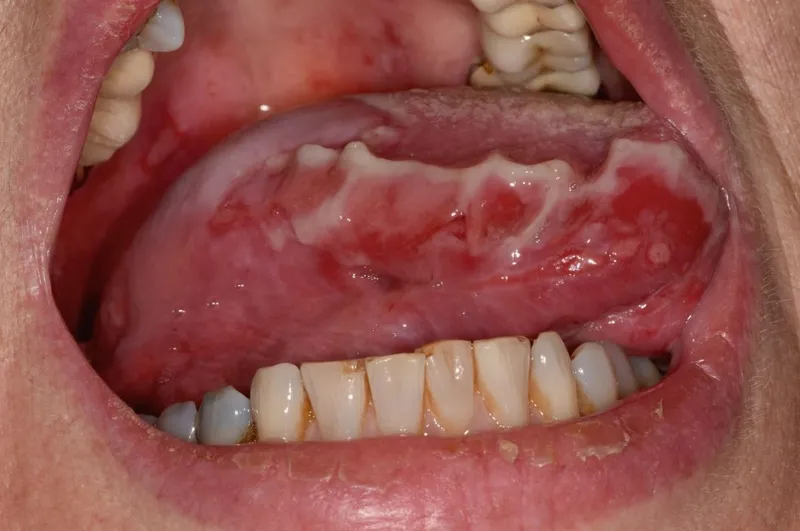
⭐ Exam Favourite: Oral lesions are often the initial manifestation and can precede cutaneous lesions by months.
- General Symptoms: Pain, burning, pruritus (less common), malaise, weight loss if severe oral involvement affects nutrition.
- No significant scarring, but post-inflammatory hyperpigmentation is common after healing of erosions.
📌 Mnemonic: PEMPHIGUS = Painful, Erosions, Mucosal (often first), Positive Nikolsky, Hot (no fever unless infected), Intraepidermal, Generalized, Uncommon, Serious autoimmune disease.
Pemphigus Vulgaris: Diagnosis - Unmasking the Villain
- Histopathology (HPE): (Lesional skin biopsy)
- Intraepidermal, suprabasal blister formation.
- Acantholysis: Loss of keratinocyte adhesion.
- Basal cell layer remains attached to dermis, resembling a 'row of tombstones'.
- Tzanck Smear:
- Rapid bedside test from blister fluid/base.
- Shows acantholytic cells (rounded keratinocytes, large nuclei).
- Immunofluorescence:
- Direct (DIF): (Perilesional skin) Gold Standard.
⭐ Shows characteristic intercellular "fish-net" or "chicken-wire" pattern of IgG (mainly IgG1 & IgG4) and C3 deposits throughout the epidermis.
- Indirect (IIF): (Serum) Detects circulating anti-Desmoglein (Dsg1, Dsg3) autoantibodies. Titers often correlate with disease severity.
- Direct (DIF): (Perilesional skin) Gold Standard.
- ELISA:
- More sensitive for detecting and quantifying specific anti-Dsg1 and anti-Dsg3 antibodies. Useful for monitoring response to therapy.

Pemphigus Vulgaris: Management - Calming the Chaos
- Systemic Corticosteroids: Mainstay. Prednisolone 1-1.5 mg/kg/day, then slow taper. IV pulse therapy (Dexamethasone/Methylprednisolone) for severe flares.
- Immunosuppressive Adjuvants (steroid-sparing):
- Azathioprine (AZA): 1-3 mg/kg/day.
- Mycophenolate Mofetil (MMF): 1-2 g/day.
- Others: Cyclophosphamide, Methotrexate for refractory cases.
- Biologics:
- Rituximab (anti-CD20 mAb): Increasingly first-line or for refractory disease. Protocols: RA (1g IV x2, 2 weeks apart) or Lymphoma (375mg/m² weekly x4).
- Supportive Care: Essential.
- Wound care, nutritional support, analgesia.
- Prophylaxis: PPIs, Vitamin D/Calcium, PCP (with high-dose/prolonged steroids).
⭐ Rituximab has shown superior efficacy and steroid-sparing effects, often leading to prolonged remission in Pemphigus Vulgaris.
Pemphigus Vulgaris: Complications & Outlook - The Aftermath
- Complications:
- Secondary infections (bacterial, fungal) common.
- Steroid side-effects: Cushingoid features, osteoporosis, PUD, ↑glucose.
- Electrolyte imbalance.
- Outlook:
- Chronic, relapsing course typical.
- Mortality ↓ with therapy, but significant.
⭐ Secondary infection is the most common cause of death in Pemphigus Vulgaris patients receiving immunosuppressive therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- Pemphigus Vulgaris is an autoimmune disease causing intraepidermal blisters due to acantholysis.
- Autoantibodies target desmoglein 3 (mucosal dominant) and desmoglein 1 (mucocutaneous).
- Oral mucosa is commonly the first site involved and lesions are often painful.
- Characterized by flaccid blisters on skin and erosions on mucous membranes.
- Nikolsky's sign (gentle rubbing causes skin to blister) is typically positive.
- Histopathology shows a suprabasal split with acantholytic cells and tombstone appearance of basal cells.
- Direct immunofluorescence (DIF) reveals intercellular IgG/C3 deposition in a "fishnet" pattern throughout the epidermis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

