Overview & Pathogenesis - Leafy Skin Split
- Pemphigus Foliaceus (PF): A chronic, superficial autoimmune blistering disease affecting the skin.
- Core Pathogenesis:
- Autoantibodies (IgG, often IgG4) target Desmoglein 1 (DSG1), a keratinocyte adhesion molecule.
- Leads to acantholysis (separation of keratinocytes).
- Results in intraepidermal split within the superficial epidermis (subcorneal or upper granular layer).
- 📌 Foliaceus = Fragile, Flakes (superficial, "leaf-like" scales).
⭐ Pemphigus foliaceus is the most common autoimmune blistering disease in certain endemic regions of Brazil (Fogo Selvagem).
Clinical Features - Scaly Crusty Rash
- Morphology:
- Superficial, fragile blisters (often ruptured, rarely seen intact).
- Leads to scaly, crusted erosions.
- Characteristic "cornflake" like scales.
- Well-demarcated lesions.
- Distribution:
- Primarily affects seborrheic areas:
- Scalp (often initial site)
- Face (malar region, forehead)
- Chest (V-area)
- Upper back
- Primarily affects seborrheic areas:
- Mucous Membranes: Typically spared (key differentiator from Pemphigus Vulgaris).
- Symptoms:
- Pruritus (itching) is common and can be intense.
- Burning sensation may occur.
- Variants:
- Fogo Selvagem (Endemic Pemphigus Foliaceus): Brazil, rural areas.
- Pemphigus Erythematosus (Senear-Usher Syndrome): Overlap with lupus erythematosus; facial lesions, +ANA.
⭐ Nikolsky sign is often positive in Pemphigus Foliaceus, though blisters are very superficial.
Diagnosis - Spotting the Split
Key investigations aim to identify the specific level of epidermal split and the presence of pathogenic autoantibodies:
- Skin Biopsy: Crucial for diagnosis.
- Lesional skin (Histopathology - HPE): Shows characteristic subcorneal or intragranular acantholysis (epidermal cell separation).
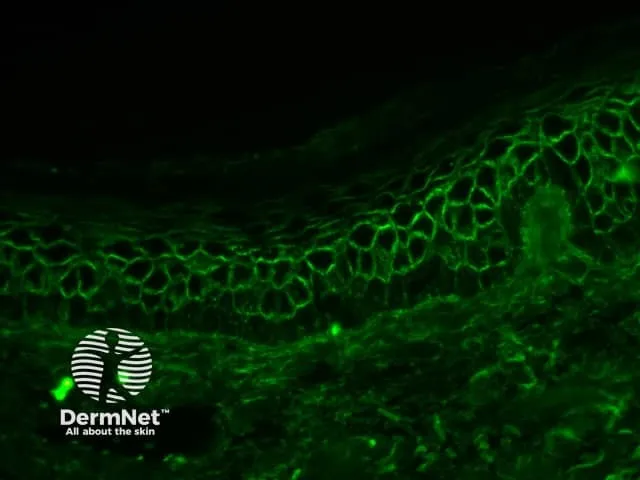
- Perilesional skin (Direct Immunofluorescence - DIF): Gold standard; reveals intercellular IgG and C3 deposition in the superficial epidermis, creating a "chicken-wire" pattern.
⭐ Direct immunofluorescence showing intercellular IgG deposition in the superficial epidermis is key for diagnosis.
- Serum Tests:
- Indirect Immunofluorescence (IIF): Detects circulating anti-Desmoglein 1 (anti-DSG1) IgG autoantibodies.
- ELISA (Enzyme-Linked Immunosorbent Assay): Confirms presence and quantifies anti-DSG1 antibodies; useful for diagnosis and monitoring disease activity.
- Tzanck Smear:
- Rapid test showing acantholytic cells (Tzanck cells); less specific but can be suggestive.
DDx & Management - Calm the Chaos
Differential Diagnosis:
| Condition | Key Differentiators (vs PF) |
|---|---|
| Impetigo | Bacterial, superficial, honey-colored crusts |
| Subcorneal Pustular Dermatosis | Sterile pustules, chronic, annular/serpiginous |
| Dermatitis Herpetiformis | Intense pruritus, grouped vesicles, IgA at DEJ |
| Pemphigus Vulgaris | Deeper intraepidermal split, oral lesions common |
| Seborrheic Dermatitis (severe) | Greasy scales, scalp/face/chest distribution |
⭐ Unlike Pemphigus Vulgaris, Pemphigus Foliaceus generally has a better prognosis and lower mortality rate.
High‑Yield Points - ⚡ Biggest Takeaways
- Superficial autoimmune blistering disease; targets Desmoglein 1 (DSG1).
- Histopathology: subcorneal split with acantholytic cells in the upper epidermis.
- Clinical: crusted, scaly erosions on seborrheic areas (face, scalp, chest); mucosa is spared.
- Nikolsky sign is typically positive.
- DIF: intercellular IgG and C3 deposition in a "fish-net" or "chicken-wire" pattern in superficial epidermis.
- Endemic form in South America is Fogo Selvagem; associated with black fly bites (Simulium).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

