Overview & Pathogenesis - IgA's Linear Attack
- Definition: Rare autoimmune subepidermal blistering disease characterized by linear IgA deposits along the basement membrane zone (BMZ).
- Epidemiology: Bimodal age of onset: childhood (typically <5 years) and adults (typically >60 years).
- Etiology:
- Idiopathic: Most common form.
- Drug-induced: 📌 Vancomycin is classic; others include NSAIDs, captopril, lithium, penicillins, cephalosporins.
- Pathophysiology: Autoantibodies (IgA class) target antigens in the BMZ.
- Main targets: LAD-1 (a 120-kDa ectodomain of BPAG2/BP180), LABD97 (a 97-kDa protein).
- Less common: Type VII collagen.
⭐ Vancomycin is the most frequently implicated drug in drug-induced Linear IgA Bullous Dermatosis (LABD).
Clinical Picture - Strings of Pearls
- Cutaneous Lesions:
- Tense vesicles & bullae, often on an erythematous or urticarial base.
- Annular or polycyclic configuration.
- "String of pearls" sign: new vesicles cluster at the periphery of older, resolving lesions (characteristic).

- Pruritus: Common, can be intense.
- Distribution:
- Adults: Predominantly trunk and limbs.
- Children: Lower abdomen, buttocks, perineum (often widespread).
- Mucosal Involvement (common, 50-70%):
- Oral mucosa (most frequent): Painful erosions, vesicles.
- Ocular (serious): Conjunctivitis, symblepharon, potential for blindness.
- Other sites: Nasal, pharyngeal, laryngeal, esophageal, genital mucosa.
- Age-Specific Variants:
- Childhood LABD: Often more widespread, prominent perineal involvement ("sausage-shaped" bullae); may remit spontaneously.
- Adult LABD: Tends to be chronic and relapsing.
⭐ The "string of pearls" sign, though not exclusive, is highly suggestive of LABD.
Diagnosis & Differentials - Spotting the Line
- Skin Biopsy (perilesional):
- Subepidermal blister.
- Neutrophils predominant at dermoepidermal junction (DEJ).
- Eosinophils may be present.
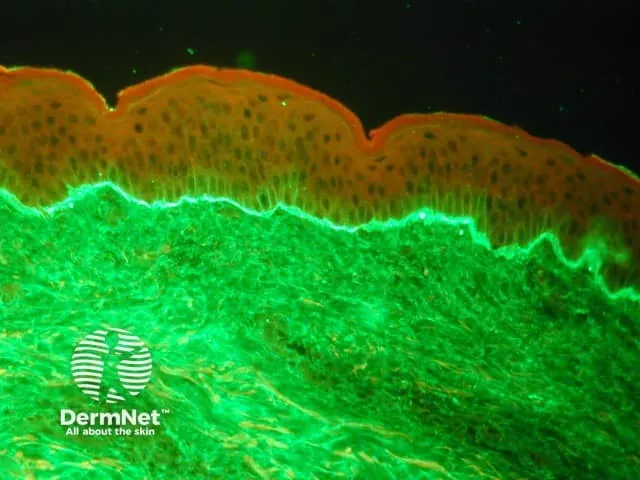
- Direct Immunofluorescence (DIF) (perilesional skin):
- Gold Standard.
- Continuous linear IgA deposition along Basement Membrane Zone (BMZ).
- C3 may also be present.
- Indirect Immunofluorescence (IIF) (serum):
- Detects circulating IgA anti-BMZ antibodies.
- Sensitivity ~50-70%; lower than DIF.
- Salt-Split Skin:
- IgA deposits on epidermal side (roof), dermal side (floor), or both.
- (e.g., LAD-1 antigen: epidermal side).
Differential Diagnosis:
| Condition | Key Differentiators |
|---|---|
| Bullous Pemphigoid | IgG, eosinophils, older adults |
| Dermatitis Herpetiformis | Granular IgA (dermal papillae), celiac assoc., intense pruritus, extensors |
| Epidermolysis Bullosa Acq. | IgG (Type VII collagen), trauma-induced, acral sites, scarring |
| Pemphigoid Gestationis | Pregnancy-associated, IgG |
| Cicatricial Pemphigoid | Mucosal dominant, scarring, IgG |
⭐ Direct immunofluorescence showing a continuous linear band of IgA at the dermoepidermal junction is the diagnostic hallmark of LABD.
Management & Prognosis - Calming the Chain
- General: Symptomatic relief (wound care, anti-pruritics). Drug-induced: Stop offending drug.
- First-line: Dapsone (Adults: 50-200 mg/day; Children: 1-2 mg/kg/day). ⚠️ Monitor G6PD, methemoglobinemia.
⭐ Dapsone is the treatment of choice for Linear IgA Bullous Dermatosis.
- Alternatives/Adjuncts:
- Sulfapyridine/Sulfasalazine (dapsone intolerance).
- Systemic Corticosteroids (Prednisolone 0.5-1 mg/kg/day) for severe cases or dapsone failure.
- Immunosuppressants (Azathioprine, MMF), IVIG for refractory disease.
- Prognosis:
- Childhood: Often self-limiting (spontaneous remission <2 yrs).
- Adult: More chronic/relapsing course; remission possible. ⚠️ Ocular involvement can lead to blindness.
- Complications: Scarring (mucosal, laryngeal), ocular damage, secondary infections.
High‑Yield Points - ⚡ Biggest Takeaways
- Autoimmune subepidermal blistering disease characterized by tense bullae.
- Pathognomonic: Continuous linear IgA deposition along the basement membrane zone (BMZ) on direct immunofluorescence.
- Two clinical variants: childhood (Chronic Bullous Disease of Childhood - CBDC) and adult.
- CBDC often presents with annular lesions and the "cluster of jewels" or "string of pearls" sign.
- Drug-induced LABD is a significant subtype, commonly associated with vancomycin.
- Dapsone is the first-line treatment; sulfapyridine or corticosteroids are alternatives_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

