Intro to IBDs & GC - Skin Deep Genes
- Inherited Blistering Diseases (IBDs): Group of genetic disorders; cause skin fragility & recurrent blisters.
- Key Types:
- Epidermolysis Bullosa (EB)
- Hailey-Hailey disease (benign familial pemphigus)
- Darier disease (keratosis follicularis)
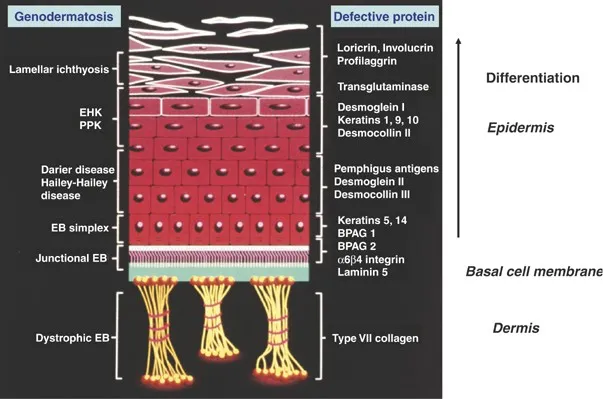
- Genetic Basis: Mutations in genes encoding structural skin proteins (e.g., keratins, collagen).
- Genetic Counseling (GC) is Vital:
- Confirms diagnosis (molecular testing).
- Assesses recurrence risk for future pregnancies.
- Guides family planning, prenatal diagnosis.
- Provides psychosocial support.
⭐ Genetic counseling is crucial not only for probands but also for at-risk family members in IBDs.
Key IBDs Overview - The Fragile Layers
📌 EB Types Mnemonic: Simple Junctions Destroy Kindness (Simplex, Junctional, Dystrophic, Kindler).
| Disease (Subtype) | Gene(s) | Protein Affected | Inheritance | Key Clinical Features |
|---|---|---|---|---|
| EB Simplex (EBS) | KRT5, KRT14 | Keratin 5, 14 | AD | Non-scarring blisters (hands/feet); intraepidermal. |
| Junctional EB (JEB) | LAMA3, LAMB3, LAMC2 | Laminin-332 | AR | Severe neonatal blisters; high mortality (Herlitz); lamina lucida. |
| Dystrophic EB (DEB) | COL7A1 | Type VII collagen | AD/AR | Scarring, milia, nail dystrophy, "mitten" hands (RDEB); sublamina densa. |
| Kindler Syndrome | FERMT1 | Kindlin-1 | AR | Photosensitivity, poikiloderma, acral blisters; mixed planes. |
| Hailey-Hailey Disease | ATP2C1 | SERCA2b (Golgi Ca$^{2+}$ pump) | AD | Intertriginous vesicles/erosions; "dilapidated brick wall". |
| Darier Disease | ATP2A2 | SERCA2 (ER Ca$^{2+}$ pump) | AD | Greasy papules (seborrheic); nail V-nicking; corps ronds/grains. |
⭐ Dystrophic Epidermolysis Bullosa (DEB) is associated with mutations in the COL7A1 gene, leading to defective type VII collagen.
Genetic Counseling Process - Decoding Blueprints
- Assessment & Diagnosis:
- Pedigree analysis.
- Confirm diagnosis: Skin biopsy, Immunofluorescence (IF) mapping, Electron Microscopy (EM), Molecular genetic testing (mutation ID).
- Risk & Inheritance:
- Explain inheritance patterns (AD, AR, X-linked).
- Calculate recurrence risk.
- Reproductive Options & Testing:
- Carrier testing (relatives).
- PND: CVS (10-13 wks), Amniocentesis (15-20 wks).
- Preimplantation Genetic Diagnosis (PGD) with IVF.
- Counseling Core:
- Ethical, Legal, Social Implications (ELSI).
- Informed consent.
- Psychosocial support.
⭐ Preimplantation Genetic Diagnosis (PGD) offers an option for couples at high risk of having a child with a severe IBD to select unaffected embryos before pregnancy.
Psychosocial Support - More Than Skin Deep
- IBDs severely impact Quality of Life (QoL):
- Pain, pruritus, disfigurement, functional limits.
- Psychological toll:
- Anxiety, depression, social isolation.
- Significant caregiver stress.
- Essential Multidisciplinary Team (MDT):
- Dermatologist, genetic counselor, psychologist, social worker, nurses, pain specialists.
- Key: Patient support groups & resources.

⭐ A multidisciplinary approach is essential in managing IBDs, addressing not just the physical symptoms but also the significant psychosocial impact on patients and families.
High‑Yield Points - ⚡ Biggest Takeaways
- Inheritance patterns (AR, AD, X-linked) determine recurrence risks (e.g., 25% for AR, 50% for AD).
- Molecular diagnosis via gene testing (e.g., gene panels) is crucial for accurate counseling.
- Discuss Prenatal Diagnosis (PND) and Preimplantation Genetic Diagnosis (PGD) options.
- Carrier testing for relatives is vital in autosomal recessive conditions.
- De novo mutations are frequent and significantly alter recurrence risk.
- Explain concepts of genetic heterogeneity and phenotypic variability to families.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

