Etiopathogenesis & Intro - The Gluten Itch
- Autoimmune, chronic, recurrent blistering disease.
- Characterized by intense pruritus (the "gluten itch").
- Strongly linked to gluten sensitivity and Celiac Disease (CD):
- Nearly 100% of patients have histological CD.
- ~75% are symptomatic for CD.
- Pathogenesis: Gluten ingestion triggers IgA antibody production against epidermal transglutaminase (eTG/TG3).
- Leads to granular IgA deposits at the dermal-epidermal junction.
- Genetic predisposition: HLA-DQ2 (most common) and HLA-DQ8.
- 📌 Mnemonic: "Dairy Queen: 2 much 8 gluten makes me itch."
⭐ Dermatitis Herpetiformis is considered a cutaneous manifestation of celiac disease; virtually all patients have gluten-sensitive enteropathy.
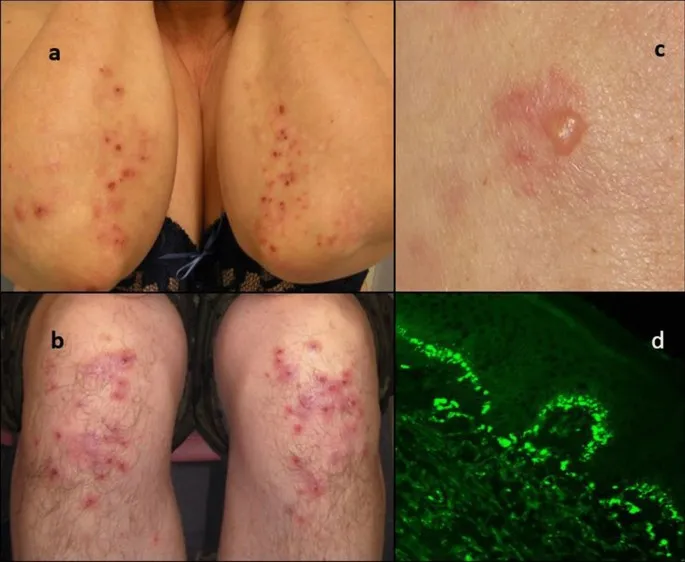
Clinical Features - Rash on the Double
- Pruritus: Hallmark is intense, paroxysmal itching.
- Often a burning or stinging sensation.
- Can precede skin lesions by hours to days.
- Lesions: Typically symmetrical and grouped.
- Manifest as erythematous papules, vesicles, and urticarial plaques.
- Bullae are less common and rarely intact due to intense scratching.
- Excoriations are frequently seen.
- Distribution (📌 SSEKB Mnemonic):
- Extensor surfaces: Elbows, knees.
- Buttocks, scalp, posterior nuchal area, shoulders.
- Scalp, Shoulders, Elbows, Knees, Buttocks.
- Mucosal involvement: Rare.
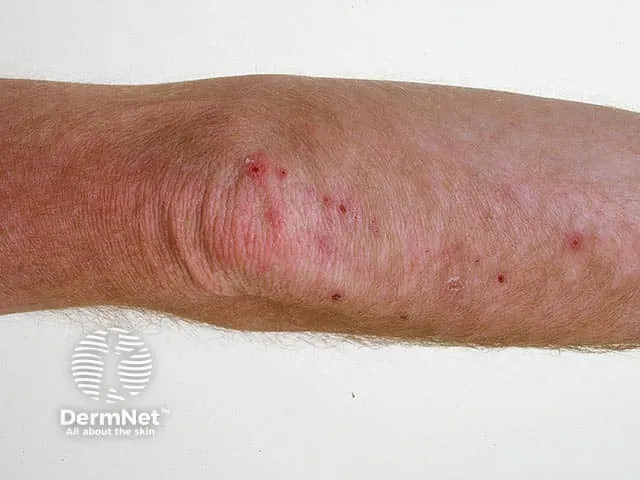
⭐ The intense pruritus in Dermatitis Herpetiformis is often described as out of proportion to the visible skin lesions.
Diagnosis - Pinpointing the Problem
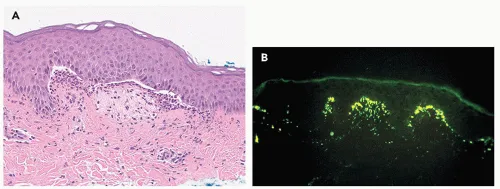
- Gold Standard: Skin biopsy of perilesional skin for Direct Immunofluorescence (DIF).
- Shows granular IgA deposits in dermal papillae at the dermo-epidermal junction (DEJ).
⭐ Direct Immunofluorescence (DIF) of perilesional skin revealing granular IgA deposits at the dermal-epidermal junction is pathognomonic for Dermatitis Herpetiformis.
- Histopathology (Lesional skin):
- Subepidermal vesicles/blisters.
- Neutrophilic microabscesses at tips of dermal papillae.
- Serology:
- IgA anti-tissue transglutaminase (tTG), IgA anti-endomysial (EMA) antibodies, IgA anti-deamidated gliadin peptide (DGP).
- Support diagnosis and monitor GFD adherence.
- Celiac Disease Screening:
- All patients should be evaluated.
- Duodenal biopsy often shows villous atrophy.
Diagnostic Workflow:
Management & Complications - Diet & Drug Duo
Primary Management:
- Lifelong strict Gluten-Free Diet (GFD):
- Improves skin & gut symptoms.
- Reduces medication need.
- ↓ risk of intestinal lymphoma.
Pharmacological Therapy (Rapid Symptom Control):
- Dapsone:
- Dose: 50-200 mg/day (titrate to lowest effective dose).
- Rapid itch relief (24-48h).
- ⚠️ Screen for G6PD deficiency before starting (risk of hemolysis).
- Side Effects (SE): 📌 Hemolysis, Agranulocytosis, Methemoglobinemia, Peripheral neuropathy. Monitor CBC.
- Alternatives: Sulfapyridine, sulfasalazine.
- Topical corticosteroids: For symptomatic relief.
Management Algorithm:
Complications:
- Associated celiac disease: Malabsorption, osteoporosis.
- ↑ Risk of non-Hodgkin's lymphoma (especially intestinal if GFD not strictly followed).
⭐ While Dapsone provides rapid symptomatic relief in Dermatitis Herpetiformis, a strict lifelong gluten-free diet is the cornerstone of management and addresses the underlying gut pathology.
High‑Yield Points - ⚡ Biggest Takeaways
- Strong association with celiac disease (gluten-sensitive enteropathy).
- Intensely pruritic papules and vesicles, often grouped (herpetiform).
- Symmetrical distribution on extensor surfaces (elbows, knees, buttocks, scalp).
- Direct Immunofluorescence (DIF): Granular IgA deposits in dermal papillae is pathognomonic.
- Dapsone provides rapid relief of itching and lesions.
- Strict lifelong gluten-free diet is essential for management and prevents complications.
- Histopathology: Subepidermal bullae with neutrophilic abscesses at papillary tips.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

