Syphilis: Introduction - The Great Mimic
- Chronic, systemic, sexually transmitted infection (STI).
- Caused by spirochete Treponema pallidum subsp. pallidum.
- Dubbed "The Great Mimic" or "Great Imitator" due to its varied clinical presentations, affecting any organ.
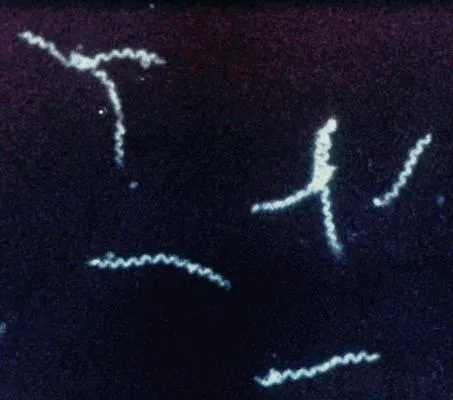
⭐ Syphilis can mimic numerous other diseases, often delaying diagnosis if not considered in differential diagnoses across specialties a true "great imitator" indeed!
Syphilis: Transmission - Stealthy Spread
- Sexual Contact: Predominant route; direct contact with active, moist lesions (chancre, condyloma lata, mucous patches).
- Vertical (Mother-to-Child): Transplacental transmission to fetus during pregnancy, leading to congenital syphilis.
- Rare Routes: Blood transfusion (now very rare due to screening), accidental direct inoculation (e.g., needlestick).

⭐ The highest risk of syphilis transmission occurs during the primary and secondary stages due to the high number of spirochetes present in early lesions like chancres and condylomata lata.
Syphilis: Clinical Stages - A Multi-Act Drama
- Incubation: 9-90 days (avg. 3 wks).

-
Primary (Painless Ulcer)
- Key: Painless chancre (indurated) at inoculation site.
- Regional non-tender lymphadenopathy. Heals in 3-6 wks.
-
Secondary (Systemic Spread; "Great Imitator")
- Rash: Non-pruritic, maculopapular (palms & soles classic).
- Condyloma lata (moist areas). Mucous patches.
- Generalized lymphadenopathy, fever.
⭐ "Moth-eaten alopecia" & "nickel and dime lesions" are characteristic.
-
Latent (Silent Phase)
- Asymptomatic, positive serology.
- Early: < 1 yr. Late: > 1 yr / unknown.
-
Tertiary (Late Complications)
- Gumma: Granulomas (skin, bone, viscera).
- Cardiovascular: Aortitis, aneurysm.
- Neurosyphilis: (Any stage) Meningovascular, General Paresis, Tabes Dorsalis.
- 📌 Argyll Robertson pupil (ARP: Accommodation Reflex Present, Pupillary absent).
Syphilis: Congenital Form - Innocent Victims
- Transmitted transplacentally, typically after 4th month of gestation.
- Early (≤2 years):
- Rhinitis ("snuffles"), maculopapular rash (palms/soles), hepatosplenomegaly.
- Osteochondritis (Parrot's pseudoparalysis), Wimberger's sign (medial tibial metaphysis).
- Late (>2 years): Stigmata
- Hutchinson's Triad: Interstitial keratitis, Hutchinson's teeth, 8th nerve deafness. 📌 (HIE)
- Mulberry molars, saddle nose, saber shins, Clutton's joints (painless knee synovitis).
⭐ Hutchinson's teeth (centrally notched, widely-spaced, peg-shaped permanent upper incisors) are a pathognomonic late sign of congenital syphilis an exam favourite question
Syphilis: Diagnostic Clues - Unmasking the Spirochete
- Direct Methods:
- Dark Field Microscopy (DFM): Live spirochetes (chancre, condyloma lata).
- PCR: For CSF, amniotic fluid, blood.
- Serological Tests:
- Non-Treponemal (NTT): VDRL, RPR. Screening, monitor Rx response (titers). 📌 BFP: Pregnancy, Autoimmune, Malaria, recent Immunization/Infection (PAMI).
- Treponemal (TT): FTA-ABS, TPPA. Confirmatory. Usually lifelong positive.
- Neurosyphilis: CSF: ↑cells (lymphocytic pleocytosis), ↑protein. CSF-VDRL (specific), CSF FTA-ABS (sensitive).
⭐ A reactive CSF-VDRL is diagnostic of neurosyphilis, though it has low sensitivity.

Syphilis: Treatment Plan - Eradicating the Enemy
Effective syphilis eradication hinges on Penicillin G, with dosage and duration tailored to disease stage. Doxycycline is key for penicillin-allergic patients.
⚠️ JHR: Acute febrile reaction post-Rx (fever, chills); self-limiting. Antipyretics for relief.
⭐ Benzathine Penicillin G (BPG) yields poor CSF penetration; thus, not used for neurosyphilis. Aqueous Pen G is vital.
High‑Yield Points - ⚡ Biggest Takeaways
- Primary syphilis: Presents with a painless chancre at the inoculation site, caused by Treponema pallidum.
- Secondary syphilis: Characterized by a diffuse maculopapular rash (critically involving palms and soles), condylomata lata, and generalized lymphadenopathy.
- Tertiary syphilis: Manifests as gummas, cardiovascular syphilis (e.g., aortitis), or neurosyphilis (e.g., tabes dorsalis, general paresis).
- Congenital syphilis: Key features include Hutchinson's triad (interstitial keratitis, notched incisors, 8th nerve deafness), mulberry molars, and saber shins.
- Diagnosis: Dark-field microscopy for early lesions; Serology includes non-treponemal tests (VDRL, RPR) for screening and treponemal tests (FTA-ABS, TPPA) for confirmation.
- Treatment: Penicillin G is the drug of choice for all stages of syphilis.
- Jarisch-Herxheimer reaction: An acute, self-limiting febrile reaction often occurs after initiating Treponema pallidum treatment, especially with penicillin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

