Impetigo Overview - Skin's Sticky Situation
- Definition: Highly contagious, superficial bacterial skin infection, primarily affecting the epidermis.
- Etiology:
- Staphylococcus aureus (most common, ~80%), often MRSA.
- Streptococcus pyogenes (Group A Strep, GAS).
- Mixed infections are also common.
- Epidemiology:
- Predominantly affects children (peak 2-5 yrs).
- More prevalent in summer/fall; favors warm, humid climates.
- Risk factors: Poor hygiene, pre-existing skin trauma (e.g., insect bites, eczema, abrasions).
- Transmission: Highly contagious via direct contact.
- Pathophysiology: Bacteria invade compromised skin → proliferate within epidermis → produce toxins (e.g., exfoliative toxins by S. aureus causing bullae in bullous impetigo).

⭐ Impetigo is the most common bacterial skin infection in children worldwide.
Clinical Presentation - Crusts, Bullae, Ulcers
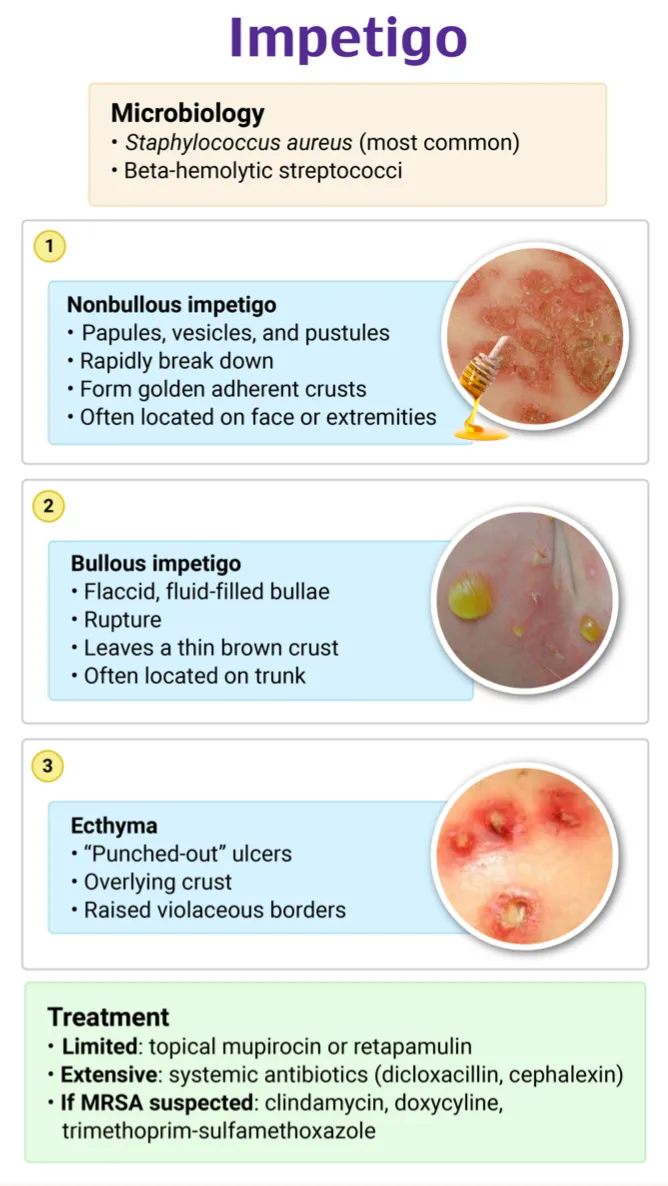
| Feature | Non-bullous Impetigo (Impetigo Contagiosa, ~70% cases) | Bullous Impetigo |
|---|---|---|
| Etiology | Primarily S. aureus; also S. pyogenes, mixed. | Exclusively S. aureus (exfoliative toxins ETA, ETB) |
| Key Lesion | Vesicles/pustules → rupture → Honey-colored crusts. | Flaccid bullae (1-2 cm; clear/cloudy fluid) → rupture → thin, varnish-like crust or collarette of scale. |
| Sites | Face (perioral, perinasal), extremities. | Trunk, extremities, intertriginous areas, diaper area (neonates). |
| Other | Pruritus common. Regional lymphadenopathy may occur. | Nikolsky sign usually negative. Less surrounding erythema. |
- Ecthyma:
- Deeper, ulcerative form extending into the dermis.
- Presents as "punched-out" ulcers covered by thick, adherent crusts.
- Heals with scarring.
- Etiology: Often S. pyogenes; S. aureus can be involved.
- Common on lower extremities, sites of neglect/poor hygiene.
Diagnosis & DDx - Spotting the Signs
Diagnosis: Primarily clinical, based on characteristic lesions.
Diagnostic Pathway:
Investigations (if atypical, widespread, recurrent, MRSA suspected, or Rx failure):
- Gram stain: Gram-positive cocci (clusters/chains). From moist lesion base or bulla fluid.
- Culture & Sensitivity: Identifies organism & guides Rx; crucial for MRSA.
Differential Diagnosis (DDx):
- Non-bullous Impetigo:
- Herpes simplex (grouped vesicles, often painful)
- Tinea corporis (annular, central clearing, active scaly border)
- Atopic dermatitis (eczematous plaques, intense pruritus)
- Scabies (burrows, intense nocturnal pruritus)
- Bullous Impetigo:
- Bullous insect bites
- Bullous pemphigoid (tense bullae, elderly)
- Epidermolysis bullosa (inherited, friction-induced)
- Burns
- Ecthyma:
- Cutaneous leishmaniasis
- Vasculitic ulcers
- Pyoderma gangrenosum
⭐ While diagnosis is usually clinical, bacterial culture is crucial for identifying MRSA and guiding antibiotic therapy in complicated cases.
Management & Complications - Healing & Hazards
- General Measures: Gentle cleansing, crust removal. Good personal hygiene, hand washing. Avoid scratching. School/daycare exclusion until lesions dry or 24h post-antibiotics.
- Topical Therapy (for limited, localized non-bullous or few bullous lesions):
- Mupirocin 2% ointment/cream (TID for 5-7 days).
- Retapamulin 1% ointment (BID for 5 days).
- Fusidic acid 2% cream (TID for 5-7 days).
- Systemic Antibiotics (for extensive disease, >5 lesions, ecthyma, bullous impetigo, oral cavity involvement, systemic symptoms, or outbreaks; typically 7 days):
- Standard: Dicloxacillin, Cephalexin.
- MRSA suspected/confirmed: Clindamycin, Doxycycline (contraindicated <8 yrs), TMP-SMX. 📌 Mnemonic: "Try Drugs for Clean MRSA" (TMP-SMX, Doxycycline/Minocycline, Clindamycin, Linezolid).
- Complications:
- Post-Streptococcal Glomerulonephritis (PSGN): After S. pyogenes impetigo; latent period 1-3 weeks. Antibiotics may not prevent.
- Cellulitis, lymphangitis.
- Staphylococcal Scalded Skin Syndrome (SSSS) (with toxin-producing S. aureus).
- Scarlet fever (with GAS).
- Rheumatic fever: NOT a complication of cutaneous streptococcal infections.
⭐ Unlike streptococcal pharyngitis, antibiotic treatment of streptococcal impetigo does not reliably prevent the development of post-streptococcal glomerulonephritis (PSGN).
High-Yield Points - ⚡ Biggest Takeaways
- Impetigo is a highly contagious, superficial bacterial skin infection, common in children.
- Predominantly caused by Staphylococcus aureus; also Streptococcus pyogenes.
- Non-bullous impetigo (most common) shows honey-colored, stuck-on crusts.
- Bullous impetigo is caused by S. aureus exfoliative toxin A, forming flaccid bullae.
- Typically affects the face (perioral, perinasal) and extremities.
- Post-streptococcal glomerulonephritis (PSGN) can follow streptococcal impetigo; rheumatic fever does not.
- Management includes topical mupirocin for localized cases or systemic antibiotics for extensive disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

