Bacterial Skin Infections

On this page
🦠 Bacterial Skin Invaders: The Infectious Battlefield
Your skin is the body's largest organ and first line of defense, yet when bacteria breach this barrier, they trigger a spectrum of infections from superficial annoyances to life-threatening emergencies. You'll master the microbiology driving these infections, recognize their distinct clinical patterns, correlate physical findings with diagnostic tests, and deploy evidence-based treatments with precision. By integrating pathophysiology with real-world decision-making, you'll transform pattern recognition into confident clinical action across simple cellulitis to complex necrotizing fasciitis.
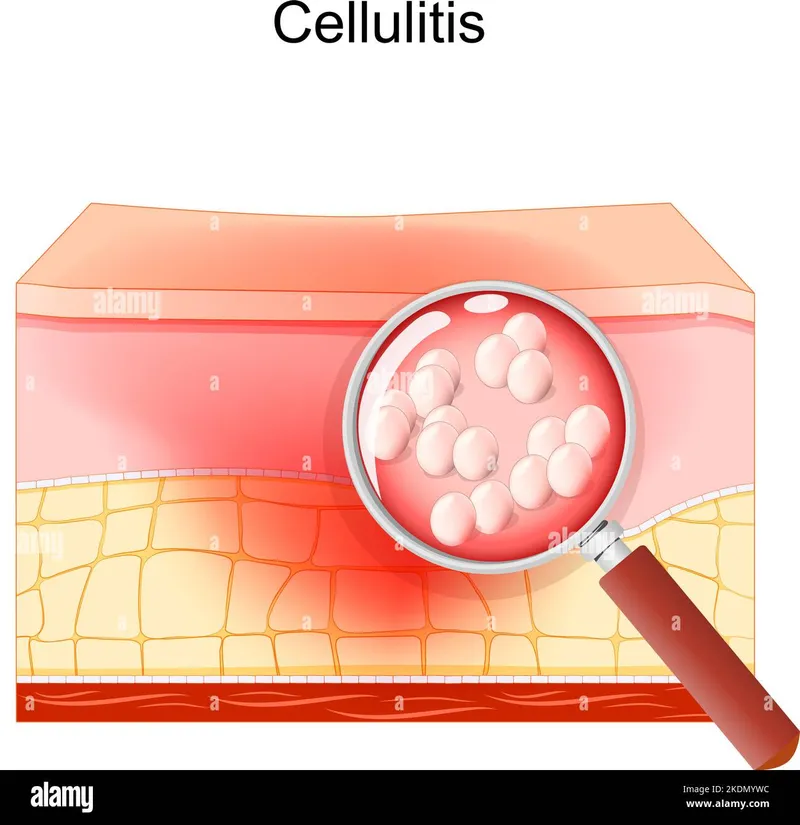
📌 Remember: SKIN classification for infection depth - Superficial (epidermis), Keratin layer involvement, Intradermal spread, Necrotizing deep tissue. Superficial infections like impetigo have >95% cure rates with topical therapy, while deep infections require systemic antibiotics with 48-72 hour response timeframes.
The microbiology of skin infections follows predictable patterns based on anatomical location and patient factors. Staphylococcus aureus dominates in areas with high sebaceous gland density, while Streptococcus pyogenes preferentially invades through breaks in the skin barrier. Methicillin-resistant S. aureus (MRSA) now accounts for >50% of skin and soft tissue infections in many healthcare settings, fundamentally altering treatment approaches.
⭐ Clinical Pearl: The "hot potato" sign - when patients cannot tolerate gentle palpation of inflamed skin - indicates deeper infection requiring immediate systemic therapy. Surface temperature differences >2°C between affected and normal skin suggest significant inflammatory response with >80% correlation to bacterial rather than viral etiology.
| Infection Type | Primary Pathogen | Depth | Treatment Duration | Cure Rate |
|---|---|---|---|---|
| Impetigo | S. aureus, S. pyogenes | Epidermis | 7-10 days | >95% |
| Folliculitis | S. aureus | Hair follicle | 5-7 days | >90% |
| Cellulitis | S. pyogenes, S. aureus | Dermis/subcutaneous | 10-14 days | 85-90% |
| Erysipelas | S. pyogenes | Superficial dermis | 10-14 days | >95% |
| Necrotizing fasciitis | Mixed flora | Deep fascia | 14-21 days | 60-80% |
💡 Master This: Bacterial skin infections follow the "Rule of 48" - most uncomplicated infections show clinical improvement within 48 hours of appropriate antibiotic therapy. Lack of improvement suggests resistant organisms, deeper infection, or alternative diagnosis requiring immediate reassessment and culture-guided therapy modification.
The epidemiology of bacterial skin infections reflects changing resistance patterns and demographic factors. Community-acquired MRSA has emerged as a dominant pathogen, particularly in athletes, military personnel, and immunocompromised patients. These infections often present with central necrosis and surrounding erythema, distinguishing them from typical S. aureus infections.
Connect these foundational concepts through pathophysiology mechanisms to understand how bacterial invasion triggers the inflammatory cascade that produces the clinical manifestations you'll learn to recognize and treat systematically.
🦠 Bacterial Skin Invaders: The Infectious Battlefield
⚔️ Microbial Warfare: Pathogen Arsenal and Host Defense
Staphylococcus aureus represents the master of skin invasion through multiple coordinated mechanisms. The organism produces protein A that binds immunoglobulin Fc regions, effectively camouflaging the bacteria from immune recognition. Simultaneously, alpha-toxin creates pores in host cell membranes, while leukocidin specifically targets and destroys neutrophils attempting to clear the infection.
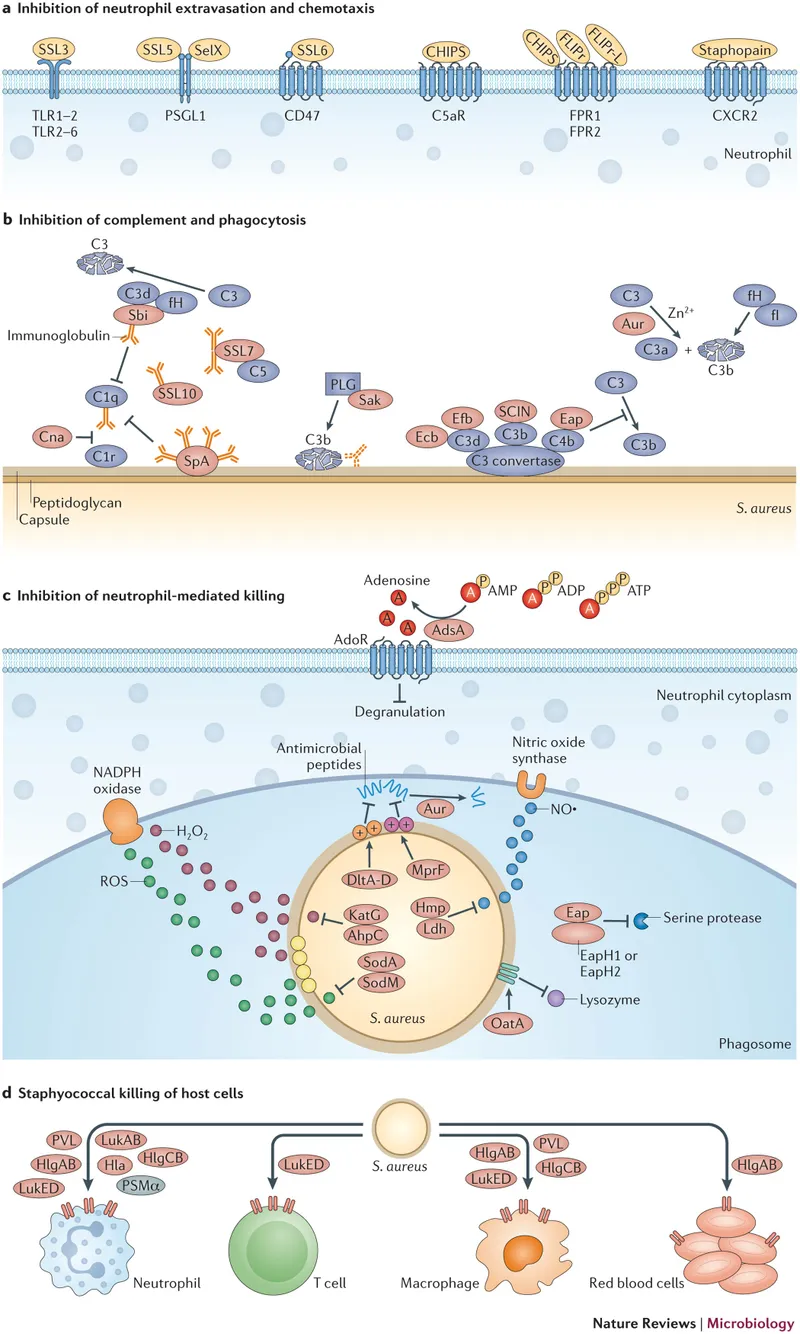
📌 Remember: STAPH virulence arsenal - Staphylokinase (clot dissolution), Toxic shock syndrome toxin, Alpha toxin (membrane damage), Protein A (immune evasion), Hyaluronidase (tissue spread). Each factor contributes to the >40% recurrence rate seen with inadequately treated staphylococcal infections.
Streptococcus pyogenes employs a different strategy focused on rapid tissue destruction and dissemination. The organism secretes streptolysin O and streptolysin S, which lyse red blood cells and create the characteristic hemolytic zones. Streptokinase dissolves fibrin clots that might contain the infection, while DNase breaks down neutrophil extracellular traps (NETs) designed to capture bacteria.
The host inflammatory response follows predictable patterns that correlate with clinical severity. Initial bacterial invasion triggers toll-like receptor activation, leading to nuclear factor-κB upregulation and subsequent cytokine release. Interleukin-1β and tumor necrosis factor-α levels correlate directly with infection severity, with concentrations >100 pg/mL indicating systemic involvement.
⭐ Clinical Pearl: The "ascending lymphangitis" pattern - red streaking extending proximally from infection sites - indicates streptococcal involvement in >85% of cases. This pattern results from bacterial spread through lymphatic channels at rates of 2-4 cm/hour, requiring immediate systemic antibiotic therapy to prevent bacteremia.
| Pathogen | Key Virulence Factor | Mechanism | Clinical Manifestation | Timeline |
|---|---|---|---|---|
| S. aureus | Alpha-toxin | Membrane pore formation | Tissue necrosis | 6-12 hours |
| S. pyogenes | Streptolysin O | RBC lysis | Hemolytic zones | 2-4 hours |
| S. agalactiae | CAMP factor | Synergistic hemolysis | Spreading cellulitis | 12-24 hours |
| P. aeruginosa | Exotoxin A | Protein synthesis inhibition | Blue-green discharge | 4-8 hours |
| C. perfringens | Lecithinase | Phospholipid breakdown | Gas production | 1-6 hours |
💡 Master This: Bacterial load correlates directly with infection severity - <10³ CFU/gram tissue rarely causes infection, 10⁴-10⁵ CFU/gram produces localized infection, while >10⁶ CFU/gram leads to systemic complications in >60% of cases. Understanding this threshold guides debridement decisions and antibiotic duration.
The emergence of antibiotic resistance has fundamentally altered bacterial pathogenesis. MRSA strains carrying the mecA gene produce altered penicillin-binding proteins with <1% affinity for β-lactam antibiotics. Community-acquired MRSA often carries additional virulence genes including Panton-Valentine leukocidin, which creates the characteristic necrotic lesions seen in >70% of CA-MRSA skin infections.
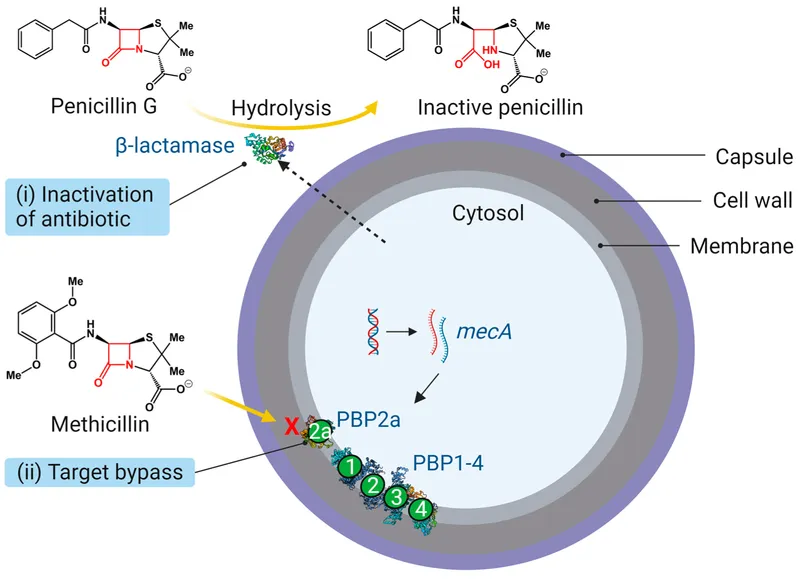
Host factors significantly influence infection susceptibility and progression. Diabetes mellitus impairs neutrophil function and reduces tissue perfusion, increasing infection risk by 3-4 fold. Immunocompromised patients show altered cytokine responses, with IL-6 levels often >10-fold higher than immunocompetent individuals, contributing to systemic toxicity.
Connect these pathophysiological mechanisms through clinical pattern recognition to understand how different bacterial strategies produce the distinct clinical presentations that guide your diagnostic and therapeutic decisions.
⚔️ Microbial Warfare: Pathogen Arsenal and Host Defense
🎯 Clinical Detective Work: Pattern Recognition Mastery
The "SKIN-DEEP" assessment framework provides systematic evaluation of bacterial skin infections:
- Size and shape of lesions
- Kolor and consistency
- Inflammatory signs (warmth, erythema, swelling)
- Necrosis or discharge patterns
- Distribution and dermatomal involvement
- Edema and lymphatic involvement
- Elevation and induration
- Pain and tenderness patterns
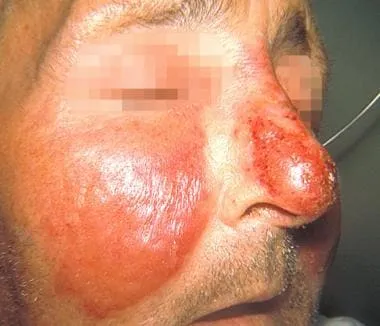
📌 Remember: STAPH vs STREP clinical differentiation - STAPH infections show Suppuration (pus formation), Thick discharge, Abscess formation, Punctate lesions, Honey-crusted appearance. STREP infections demonstrate Spreading erythema, Thin serous discharge, Raised borders, Edematous appearance, Pain out of proportion to findings.
Staphylococcus aureus infections characteristically present with localized suppuration and well-demarcated borders. The classic "golden-yellow" crusting of impetigo occurs in >80% of staphylococcal cases, while the "central punctum" sign - a central hair follicle involvement - appears in >90% of folliculitis cases. Staphylococcal abscesses typically show fluctuance within 24-48 hours and respond to incision and drainage.
Streptococcus pyogenes creates the pathognomonic "butterfly" or "slapped cheek" appearance of erysipelas, with sharply demarcated, raised borders that advance at rates of 2-4 cm per day. The "orange peel" texture (peau d'orange) results from lymphatic obstruction and appears in >70% of erysipelas cases. Associated lymphangitis presents as red streaking in >60% of streptococcal infections.
The "pain-to-appearance ratio" provides crucial diagnostic information. Necrotizing fasciitis characteristically shows severe pain disproportionate to visible changes, with pain scores >8/10 despite minimal surface findings in >85% of early cases. Conversely, superficial infections typically show proportionate pain correlating with visible inflammation.
⭐ Clinical Pearl: The "finger test" - inability to insert a finger between inflamed skin and underlying tissue - indicates deep fascial involvement in >90% of cases. This sign, combined with systemic toxicity (fever >38.5°C, tachycardia >100 bpm), mandates immediate surgical evaluation for necrotizing infection.
| Clinical Feature | Impetigo | Cellulitis | Erysipelas | Necrotizing Fasciitis |
|---|---|---|---|---|
| Border definition | Irregular | Ill-defined | Sharp, raised | Initially normal |
| Pain severity (1-10) | 2-4 | 4-6 | 5-7 | >8 |
| Systemic symptoms | Rare | 20-30% | 40-50% | >90% |
| Lymphangitis | Uncommon | 30-40% | >60% | Variable |
| Response to antibiotics | 24-48 hours | 48-72 hours | 24-48 hours | Poor |
The temporal evolution of lesions offers diagnostic insights. Impetigo progresses from vesicles to pustules to honey-crusted lesions over 2-3 days. Cellulitis shows gradual expansion over 24-72 hours with improving central areas. Necrotizing fasciitis demonstrates rapid progression with tissue color changes from red to purple to black over 6-12 hours.
💡 Master This: The "LRINEC score" (Laboratory Risk Indicator for Necrotizing Fasciitis) uses 6 laboratory parameters to predict necrotizing infection risk. Scores ≥6 indicate >50% probability of necrotizing fasciitis, while scores ≥8 show >75% probability, mandating immediate surgical exploration.
Special populations require modified pattern recognition approaches. Diabetic patients often show minimal inflammatory response despite severe infection, with normal white blood cell counts in >40% of cases. Immunocompromised patients may present with atypical organisms and unusual clinical patterns, requiring broader diagnostic consideration.
Geographic and epidemiologic factors influence pattern recognition. Community-acquired MRSA often presents with central necrosis and surrounding cellulitis, while hospital-acquired infections may show multiple antibiotic resistance patterns. Seasonal variations affect certain pathogens, with Vibrio vulnificus infections occurring predominantly during warm months in coastal areas.
Connect these pattern recognition skills through systematic diagnostic approaches to understand how clinical findings guide laboratory testing and initial therapeutic decisions before definitive pathogen identification.
🎯 Clinical Detective Work: Pattern Recognition Mastery
🔬 Diagnostic Precision: Laboratory and Clinical Correlation
Gram staining remains the cornerstone of rapid bacterial identification, providing results within 15-30 minutes. Gram-positive cocci in clusters suggest Staphylococcus species with >95% accuracy, while gram-positive cocci in chains indicate Streptococcus with >90% specificity. The presence of >25 neutrophils and <10 epithelial cells per high-power field indicates adequate specimen quality for interpretation.
📌 Remember: CULTURE collection technique - Clean surrounding skin with alcohol, Use sterile swab or needle aspiration, Lift crusts or debris for sampling, Transport immediately in appropriate medium, Use anaerobic transport for deep infections, Record antibiotic exposure history, Ensure adequate specimen volume (>1mL for fluid).
Molecular diagnostics have revolutionized bacterial identification, with PCR-based methods providing results in 2-6 hours compared to 24-48 hours for traditional culture. MALDI-TOF mass spectrometry achieves >95% accuracy for species identification within minutes of bacterial growth, while multiplex PCR panels simultaneously detect >20 pathogens and resistance markers.
The Laboratory Risk Indicator for Necrotizing Fasciitis (LRINEC) score provides objective assessment of necrotizing infection probability:
- C-reactive protein >150 mg/L (4 points)
- White blood cell count >25,000/μL (2 points) or <15,000/μL (0 points)
- Hemoglobin <13.5 g/dL (2 points) or <11 g/dL (2 points)
- Sodium <135 mmol/L (2 points)
- Creatinine >141 μmol/L (2 points)
- Glucose >180 mg/dL (1 point)
⭐ Clinical Pearl: Procalcitonin levels >0.5 ng/mL indicate bacterial infection with >85% sensitivity, while levels >2.0 ng/mL suggest severe bacterial infection requiring immediate systemic therapy. Serial measurements guide treatment duration, with >80% reduction indicating adequate response.
| Diagnostic Test | Turnaround Time | Sensitivity | Specificity | Clinical Application |
|---|---|---|---|---|
| Gram stain | 15-30 minutes | 60-80% | >95% | Rapid pathogen identification |
| Standard culture | 24-48 hours | >95% | >98% | Definitive identification |
| Molecular PCR | 2-6 hours | >90% | >95% | Rapid species/resistance |
| MALDI-TOF | <30 minutes | >95% | >98% | Species identification |
| Blood culture | 12-72 hours | >90% | >98% | Systemic infection |
Imaging studies complement laboratory diagnosis in deep infections. Ultrasound detects fluid collections with >85% sensitivity and guides drainage procedures. CT scanning identifies gas formation in >95% of clostridial infections and delineates fascial plane involvement in necrotizing infections. MRI provides superior soft tissue contrast but requires 45-60 minutes for acquisition.
💡 Master This: Biomarker kinetics guide treatment monitoring - CRP peaks at 24-48 hours then declines by >50% within 72 hours of effective therapy. Procalcitonin normalizes within 3-5 days of bacterial clearance. Failure to show >25% reduction in inflammatory markers by 48-72 hours indicates treatment failure or resistant organisms.
Point-of-care testing enables rapid decision-making in emergency settings. Lateral flow assays detect Group A Streptococcus with >85% sensitivity within 10 minutes. Rapid antigen tests identify S. aureus and MRSA with >90% specificity in 15-20 minutes. These tools enable immediate targeted therapy initiation.
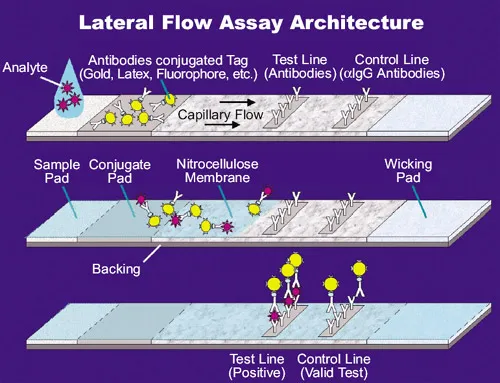
Antimicrobial susceptibility testing guides targeted therapy selection. Automated systems provide results within 6-18 hours for common pathogens. E-test strips offer quantitative MIC determination for challenging organisms. Disk diffusion remains reliable for routine susceptibility with 24-hour turnaround times.
Special considerations apply to specific clinical scenarios. Diabetic foot infections require anaerobic culture in addition to aerobic testing, as >40% contain anaerobic organisms. Immunocompromised patients need fungal culture and atypical organism testing. Post-surgical infections require biofilm-specific testing protocols.
Quality control ensures diagnostic accuracy through daily control organisms, proficiency testing, and correlation studies. False-positive rates should remain <2% for molecular tests, while false-negative rates should stay <5% for culture-based methods.
Connect these diagnostic principles through evidence-based treatment algorithms to understand how laboratory results guide antibiotic selection and duration decisions for optimal patient outcomes.
🔬 Diagnostic Precision: Laboratory and Clinical Correlation
⚖️ Therapeutic Precision: Evidence-Based Treatment Algorithms
The IDSA/ESCMID treatment algorithm stratifies infections by severity and guides initial therapy selection. Mild infections (localized, no systemic signs) receive topical therapy with >85% cure rates. Moderate infections (spreading local signs) require oral antibiotics with >90% success rates. Severe infections (systemic toxicity, immunocompromise) mandate intravenous therapy with >95% response rates when appropriately managed.
📌 Remember: TREAT algorithm for antibiotic selection - Tissue penetration (adequate levels), Resistance pattern coverage, Efficacy for specific pathogen, Adverse effect profile, Treatment duration optimization. Empirical therapy should cover >90% of likely pathogens based on local resistance patterns.
First-line topical therapy for uncomplicated superficial infections includes mupirocin 2% applied three times daily for 7-10 days, achieving >90% cure rates for impetigo. Retapamulin 1% provides alternative coverage with twice-daily dosing and >85% efficacy. Fusidic acid offers excellent staphylococcal coverage but resistance rates vary geographically from 5-40%.
Oral antibiotic selection depends on local resistance patterns and infection characteristics. Cephalexin 500mg four times daily remains first-line for β-lactam-susceptible organisms with >90% cure rates. Clindamycin 300-450mg three times daily provides excellent tissue penetration and anaerobic coverage with >85% success rates for MRSA infections.
⭐ Clinical Pearl: Antibiotic tissue penetration varies significantly - clindamycin achieves skin concentrations 2-4 times serum levels, while doxycycline reaches tissue levels >10 times serum concentrations. Linezolid maintains >95% bioavailability orally with excellent skin penetration, making it ideal for serious MRSA infections.
| Antibiotic | Route | Dosing | Tissue Penetration | MRSA Coverage | Cure Rate |
|---|---|---|---|---|---|
| Mupirocin | Topical | TID × 7-10 days | Excellent | Yes | >90% |
| Cephalexin | Oral | 500mg QID | Good | No | >90% |
| Clindamycin | Oral/IV | 300-450mg TID | Excellent | >85% | >85% |
| Doxycycline | Oral | 100mg BID | Excellent | >90% | >80% |
| Linezolid | Oral/IV | 600mg BID | Excellent | >99% | >95% |
Duration optimization follows evidence-based guidelines to prevent resistance while ensuring cure. Uncomplicated cellulitis requires 5-7 days of therapy with >90% cure rates. Complicated infections need 7-14 days depending on response. Necrotizing infections require 14-21 days with surgical debridement and combination therapy.
💡 Master This: Therapeutic drug monitoring optimizes outcomes for serious infections. Vancomycin trough levels should be 15-20 mg/L for invasive infections, 10-15 mg/L for uncomplicated cases. Daptomycin requires CK monitoring due to myopathy risk >2% at doses >6mg/kg. Linezolid needs CBC monitoring for thrombocytopenia occurring in >10% after >10 days therapy.
Combination therapy provides synergistic effects for severe infections. Vancomycin plus piperacillin-tazobactam covers MRSA plus gram-negatives with >95% empirical coverage. Clindamycin plus ciprofloxacin offers anaerobic plus gram-negative coverage for diabetic foot infections. Daptomycin plus ceftaroline provides enhanced MRSA killing for bacteremic infections.
Resistance-directed therapy addresses emerging patterns. CA-MRSA often remains susceptible to clindamycin (>80%), doxycycline (>90%), and trimethoprim-sulfamethoxazole (>85%). HA-MRSA typically requires vancomycin, linezolid, or daptomycin with >95% susceptibility rates.
Adjunctive therapies enhance treatment outcomes. Surgical debridement improves cure rates by >30% for necrotizing infections. Hyperbaric oxygen provides adjunctive benefit for clostridial infections and diabetic foot ulcers. Immunoglobulin therapy may benefit streptococcal toxic shock syndrome.
Treatment failure occurs in 5-15% of cases and requires systematic evaluation. Inadequate source control, resistant organisms, poor tissue penetration, or alternative diagnosis should be considered. Repeat cultures and imaging studies guide management modifications.
Special populations require modified approaches. Pregnancy limits options to β-lactams and erythromycin, avoiding tetracyclines and fluoroquinolones. Renal impairment necessitates dose adjustments for vancomycin and β-lactams. Pediatric patients require weight-based dosing and age-appropriate formulations.
Connect these treatment principles through comprehensive management strategies to understand how therapeutic decisions integrate with surgical interventions, infection control measures, and long-term prevention strategies for optimal patient outcomes.
⚖️ Therapeutic Precision: Evidence-Based Treatment Algorithms
🔗 Advanced Integration: Multi-System Clinical Mastery
Systemic inflammatory response syndrome (SIRS) develops in >40% of patients with severe skin and soft tissue infections, triggered by bacterial toxins and inflammatory mediators. The cascade begins with toll-like receptor activation, leading to nuclear factor-κB upregulation and subsequent cytokine storm with IL-1β, TNF-α, and IL-6 levels increasing >100-fold within 6-12 hours of severe infection onset.
📌 Remember: SEPSIS criteria for skin infection complications - Systemic signs (fever >38°C or <36°C), Elevated lactate (>2 mmol/L), Pressure drop (SBP <90 mmHg), Source control needed, Infection confirmed/suspected, Support required (vasopressors/ventilation). Early recognition within 1 hour improves survival by >20%.
The cardiovascular system shows profound effects during severe bacterial skin infections. Septic shock occurs in 15-25% of necrotizing fasciitis cases, characterized by distributive shock with high cardiac output but low systemic vascular resistance. Myocardial depression develops through TNF-α-mediated mechanisms, reducing ejection fraction by >30% in severe cases.
Renal complications emerge through multiple mechanisms including hypotension-induced acute tubular necrosis, direct bacterial toxin effects, and inflammatory mediator-induced glomerular damage. Acute kidney injury occurs in >25% of patients with necrotizing infections, with creatinine elevation >50% from baseline indicating significant renal impairment requiring fluid resuscitation and nephrotoxic drug avoidance.
Pulmonary manifestations include acute respiratory distress syndrome (ARDS) in >15% of severe cases, mediated by inflammatory mediator-induced capillary leak and surfactant dysfunction. Ventilation-perfusion mismatch develops with PaO2/FiO2 ratios <300 indicating acute lung injury requiring lung-protective ventilation strategies.
⭐ Clinical Pearl: Streptococcal toxic shock syndrome occurs in <5% of invasive Group A streptococcal infections but carries >30% mortality. The triad of hypotension, multi-organ failure, and erythematous rash with subsequent desquamation requires immediate aggressive fluid resuscitation, vasopressor support, and clindamycin addition to β-lactam therapy for toxin suppression.
| Complication | Incidence | Pathophysiology | Clinical Markers | Management |
|---|---|---|---|---|
| Septic shock | 15-25% | Distributive shock | MAP <65 mmHg | Vasopressors |
| Acute kidney injury | >25% | ATN + inflammation | Cr ↑>50% | Fluid + avoid nephrotoxins |
| ARDS | >15% | Capillary leak | P/F ratio <300 | Lung protection |
| DIC | 10-20% | Consumption + fibrinolysis | Platelets <100K | FFP + platelets |
| Multi-organ failure | >30% | Systemic inflammation | SOFA score >2 | Supportive care |
Endocrine dysfunction manifests as relative adrenal insufficiency in >60% of septic patients, with cortisol levels <25 μg/dL despite stress indicating inadequate adrenal response. Hyperglycemia occurs through stress hormone release and insulin resistance, with glucose levels >180 mg/dL correlating with increased mortality and impaired immune function.
💡 Master This: Biomarker integration guides multi-system management - Procalcitonin >2 ng/mL indicates severe bacterial infection, Lactate >4 mmol/L suggests tissue hypoperfusion requiring immediate resuscitation, SOFA score increases >2 points define sepsis with >10% mortality risk per point increase.
Immunologic considerations reveal complex host-pathogen interactions affecting treatment responses. Immunocompromised patients show altered cytokine profiles with reduced IL-2 and increased IL-10, leading to impaired bacterial clearance and increased complication rates >50%. Diabetes mellitus impairs neutrophil function and complement activation, increasing infection severity and treatment failure rates.
Pharmacokinetic alterations during severe infections affect antibiotic dosing strategies. Increased volume of distribution from capillary leak requires higher loading doses for hydrophilic antibiotics. Altered protein binding affects drug clearance, while organ dysfunction necessitates dose adjustments to prevent toxicity while maintaining therapeutic levels.
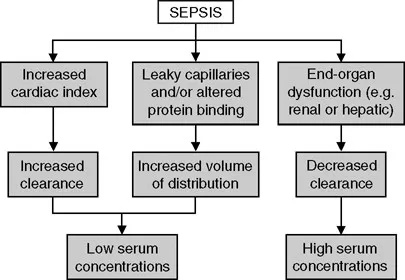
Long-term sequelae of severe bacterial skin infections include chronic pain syndromes in >20% of necrotizing fasciitis survivors, functional impairment requiring rehabilitation in >40%, and psychological effects including PTSD in >15% of cases. Amputation rates range from 10-25% depending on infection severity and treatment timing.
Quality metrics for integrated care include time to antibiotic administration <1 hour, source control within 6-12 hours, lactate clearance >10% within 6 hours, and SOFA score improvement within 48-72 hours. Bundle compliance >80% correlates with improved survival rates and reduced complications.
Connect these multi-system concepts through comprehensive clinical mastery frameworks to understand how bacterial skin infections integrate with critical care medicine, infectious disease management, and long-term patient outcomes.
🔗 Advanced Integration: Multi-System Clinical Mastery
🎯 Clinical Mastery Arsenal: Rapid Assessment and Decision Tools
The RAPID-SKIN Assessment Tool enables comprehensive evaluation within 2-3 minutes:
- Redness extent and progression rate
- Associated systemic signs (fever, tachycardia)
- Pain severity and character (0-10 scale)
- Inflammatory markers (warmth, swelling, induration)
- Discharge characteristics (color, consistency, odor)
- Size measurements and border definition
- Key risk factors (diabetes, immunosuppression)
- Infection depth assessment (superficial vs deep)
- Necrosis or tissue viability concerns
📌 Remember: URGENT red flags requiring immediate action - Uncontrolled pain (>8/10), Rapid progression (>2cm/hour), Gas in tissues (crepitus), Extreme systemic toxicity (shock), Necrotic tissue changes, Temperature >39°C with rigors. Any single criterion mandates emergency surgical consultation and broad-spectrum IV antibiotics within 1 hour.
Essential Clinical Thresholds for rapid decision-making:
- Pain score >7/10 with minimal visible changes = necrotizing infection until proven otherwise
- Temperature gradient >2°C between affected and normal skin = significant bacterial load
- Progression rate >1cm/hour = aggressive pathogen requiring immediate intervention
- White blood cell count >15,000 or <4,000 = systemic involvement
- Lactate >2 mmol/L = tissue hypoperfusion requiring resuscitation
- Procalcitonin >0.5 ng/mL = bacterial infection confirmed
- CRP >100 mg/L = significant inflammatory response
⭐ Clinical Pearl: The "GLASS" test - pressing a clear glass slide against erythematous skin that blanches completely suggests cellulitis, while non-blanching purpura indicates deeper infection or vascular involvement requiring immediate evaluation and broader antibiotic coverage.
| Clinical Scenario | First-Line Treatment | Duration | Success Rate | Escalation Criteria |
|---|---|---|---|---|
| Uncomplicated impetigo | Mupirocin 2% TID | 7-10 days | >90% | No improvement 72h |
| Simple cellulitis | Cephalexin 500mg QID | 7-10 days | >85% | Spreading at 48h |
| MRSA suspected | Clindamycin 450mg TID | 7-14 days | >80% | Systemic signs |
| Severe/systemic | Vancomycin + PCT | 10-14 days | >90% | Organ dysfunction |
| Necrotizing suspected | Vancomycin + PCT + surgery | 14-21 days | 60-80% | Continued necrosis |
- Golden crusts + localized = S. aureus (>90% probability)
- Honey crusts + spreading = S. pyogenes (>85% probability)
- Blue-green discharge = P. aeruginosa (>95% probability)
- Sweet odor + gas = Clostridium species (>90% probability)
- Rapid necrosis + toxicity = S. pyogenes Group A (>80% probability)
- Central necrosis + CA-MRSA risk = Community MRSA (>75% probability)
💡 Master This: Antibiotic Stewardship Decision Tree - Mild infections (localized, no fever) start topical therapy; Moderate infections (local spread, low-grade fever) use narrow-spectrum oral; Severe infections (systemic signs, high fever) require broad-spectrum IV with de-escalation based on culture results within 48-72 hours.
Critical Time Intervals for optimal outcomes:
- Antibiotic initiation: <1 hour for severe infections, <6 hours for moderate
- Surgical evaluation: <2 hours for necrotizing suspicion, <6 hours for non-response
- Culture collection: Before antibiotics when possible, within 24 hours maximum
- Response assessment: 24-48 hours for severe, 48-72 hours for moderate
- De-escalation timing: 48-72 hours based on culture results and clinical improvement
High-Yield Monitoring Parameters:
- Daily pain scores (expect >50% reduction by day 3)
- Lesion measurements (progression should halt by 24-48 hours)
- Temperature trends (defervescence by 48-72 hours)
- Laboratory markers (WBC normalization by 72-96 hours)
- Functional assessment (mobility improvement by 5-7 days)
Complication Prevention Checklist:
- DVT prophylaxis for immobilized patients (>48 hours bed rest)
- Glycemic control for diabetics (target <180 mg/dL)
- Renal function monitoring with nephrotoxic antibiotics
- C. difficile prevention with prolonged broad-spectrum therapy
- Wound care optimization with appropriate dressings and debridement
Discharge Readiness Criteria:
- Afebrile >24 hours without antipyretics
- Pain controlled with oral medications
- Lesion stabilized or improving for >48 hours
- Oral intake adequate for medication absorption
- Follow-up arranged within 48-72 hours
- Patient education completed regarding warning signs
Quality Assurance Metrics:
- Diagnostic accuracy >90% compared to culture results
- Appropriate antibiotic selection >85% based on guidelines
- Treatment duration optimization (avoid <5 days or >14 days without indication)
- Complication rates <5% for uncomplicated infections
- Patient satisfaction scores >90% for communication and outcomes
These rapid assessment and decision tools transform clinical encounters from reactive problem-solving to proactive, systematic management that consistently delivers optimal patient outcomes while maintaining efficiency and evidence-based practice standards.
🎯 Clinical Mastery Arsenal: Rapid Assessment and Decision Tools
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























