Vasculitis Basics - Vessel Villains
- Inflammation & necrosis of blood vessel walls, leading to impaired blood flow & organ damage.
- Classification (Chapel Hill Consensus Conference - CHCC):
- Large-vessel vasculitis (LVV): Giant cell arteritis (GCA), Takayasu arteritis (TAK).
- Medium-vessel vasculitis (MVV): Polyarteritis nodosa (PAN), Kawasaki disease (KD).
- Small-vessel vasculitis (SVV):
- ANCA-associated vasculitis (AAV): Microscopic polyangiitis (MPA), Granulomatosis with polyangiitis (GPA), Eosinophilic granulomatosis with polyangiitis (EGPA).
- Immune complex SVV: IgA vasculitis (Henoch-Schönlein purpura), Cryoglobulinemic vasculitis.
⭐ The Chapel Hill Consensus Conference (CHCC) nomenclature is widely used for classifying vasculitides based on vessel size and etiology.
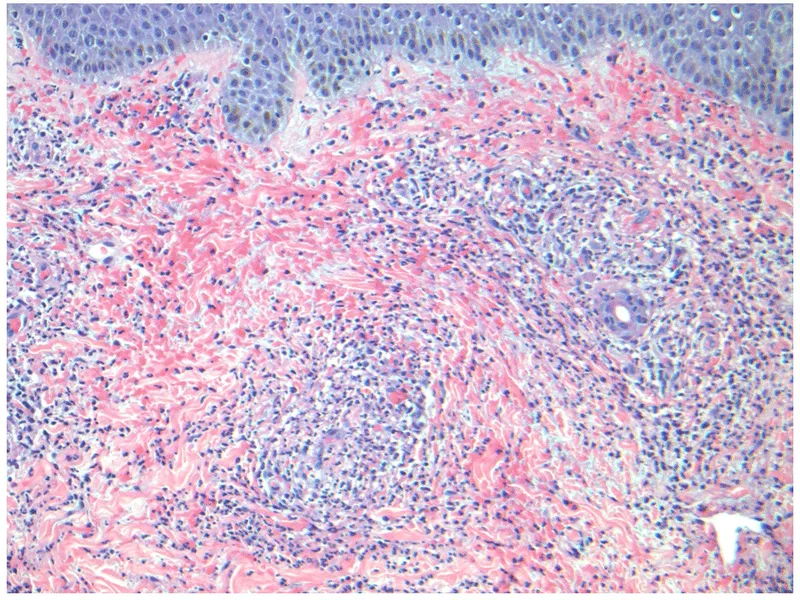
- Pathogenesis: Immune complex deposition, anti-neutrophil cytoplasmic antibodies (ANCAs), direct T-cell mediated injury. 📌 Mnemonic (ANCA): Anti-Neutrophil Cytoplasmic Antibodies target enzymes in neutrophils (MPO, PR3).
Clinical Clues - Skin Deep & More
-
Cutaneous Manifestations:
- Palpable purpura: Non-blanching, raised lesions; hallmark, often on lower extremities & dependent areas.
⭐ Palpable purpura, especially on lower extremities, is the most common cutaneous manifestation of small vessel vasculitis.
- Livedo reticularis/racemosa: Net-like, violaceous pattern.
- Nodules, papules, vesicles, bullae, ulcers, digital gangrene.
- Urticarial vasculitis: Persistent wheals (>24h), often painful/burning, may leave pigmentation.
-
Systemic Clues (Variable):
- Constitutional: Fever, malaise, weight loss, arthralgia, myalgia.
- Renal: Hematuria, proteinuria (e.g., IgA vasculitis, ANCA-associated vasculitis).
- GI: Abdominal pain, melena (e.g., IgA vasculitis).
- Pulmonary: Cough, hemoptysis, dyspnea (e.g., ANCA-associated vasculitis).
- Neurological: Mononeuritis multiplex, peripheral neuropathy, headache, stroke.
- Ocular: Episcleritis, uveitis, retinal vasculitis.
-
📌 Mnemonic (HSP features): "Henoch's Shönlein Purpura" - Hematuria, Stomach ache (abdominal pain), Palpable purpura, Arthritis (often Ankles/knees).
Diagnostic Drilldown - Finding the Fire
- Essential Labs:
- CBC (anemia, thrombocytosis), ↑↑ESR/CRP.
- Urinalysis (RBCs, casts, proteinuria).
- Renal function (Creatinine), LFTs.
- Hepatitis B/C serology, Cryoglobulins (check with purpura, arthralgia, weakness).
- ANCA (Key for Small Vessel Vasculitis):
⭐ A positive ANCA test is highly suggestive of certain small vessel vasculitides: c-ANCA/PR3 for GPA and p-ANCA/MPO for MPA and EGPA.
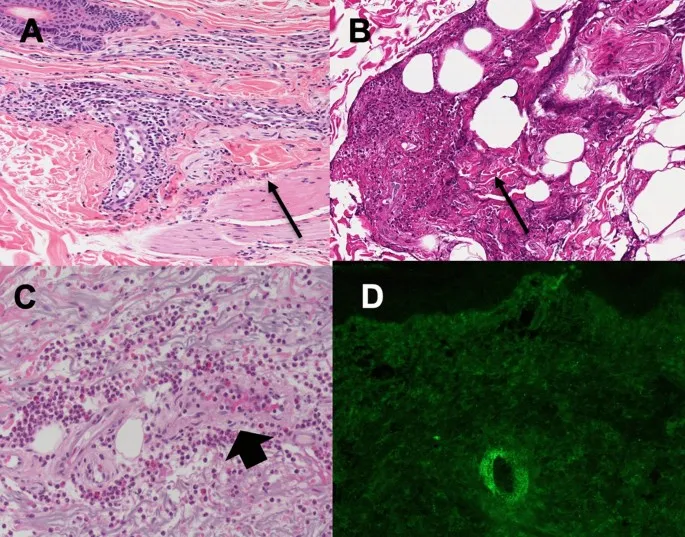
- Biopsy (Gold Standard):
- Site: Skin (newest purpuric lesion for LCV), Kidney (pauci-immune GN in ANCA+), Nerve, Lung.
- DIF: IgA deposition (IgA Vasculitis), C3.
- Targeted Imaging:
- CXR/HRCT Chest (nodules, infiltrates, hemorrhage - GPA, EGPA, MPA).
- Angiography (medium/large vessels: aneurysms, stenosis - PAN, Takayasu).
- Doppler US (GCA: temporal artery 'halo sign').
High-Yield Syndromes - Rogues' Gallery
- Kawasaki Disease
- Fever >5d + 📌 CRASH & Burn (Conjunctivitis, Rash, Adenopathy, Strawberry tongue, Hand/foot edema).
- Risk: Coronary aneurysms.
- Rx: IVIG 2g/kg + Aspirin (80-100mg/kg/d → 3-5mg/kg/d).
⭐ Kawasaki disease requires prompt treatment with IVIG and high-dose aspirin to prevent coronary artery aneurysms.
- Henoch-Schönlein Purpura (HSP) / IgA Vasculitis
- Tetrad: Palpable purpura (buttocks/legs), Arthritis, Abd pain, Renal (IgA nephropathy).
- Post-URI.

- Behçet's Disease
- Recurrent oral & genital ulcers, uveitis.
- Pathergy test (+). HLA-B51.
- Polyarteritis Nodosa (PAN)
- Medium-vessel; spares lungs. Hep B assoc.
- Livedo reticularis, nodules, renal (no GN), neuropathy. "Rosary bead" angiography.
High‑Yield Points - ⚡ Biggest Takeaways
- Palpable purpura: Hallmark of Leukocytoclastic Vasculitis (LCV).
- Henoch-Schönlein Purpura (HSP): IgA deposition, classic triad (purpura, arthritis, abdominal pain), often post-URI.
- Polyarteritis Nodosa (PAN): Associated with Hepatitis B, affects medium vessels; presents with nodules, livedo reticularis.
- GPA (Wegener’s): c-ANCA positive; involves upper/lower respiratory tract and kidneys.
- EGPA (Churg-Strauss): Asthma, eosinophilia, p-ANCA positive.
- Microscopic Polyangiitis (MPA): p-ANCA positive; causes pauci-immune glomerulonephritis and pulmonary capillaritis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

