SLE Basics - Lupus Unmasked
- Definition: Systemic Lupus Erythematosus (SLE) is a chronic, relapsing-remitting, multisystem autoimmune disease characterized by diverse mucocutaneous and systemic manifestations.
- Key Pathogenesis:
- Autoantibody formation: ANA (most sensitive), anti-dsDNA (correlates with disease activity, nephritis), anti-Sm (highly specific).
- Immune complex deposition: Type III Hypersensitivity leading to vasculitis and tissue damage.
- Complement activation: ↓C3, ↓C4.
- Genetic predisposition: Associated with HLA-DR2, HLA-DR3.
- Environmental triggers: UV light exposure, certain drugs (e.g., hydralazine, procainamide, isoniazid), infections.
- Epidemiology: Affects predominantly women of childbearing age (Female:Male ratio ≈ 9:1).
⭐ Anti-Sm (Smith antigen) antibody is highly specific for SLE, though less sensitive than ANA.
Skin Deep Lupus - Rash Decisions
- Gilliam Classification of Cutaneous LE (CLE):
- Acute Cutaneous LE (ACLE):
- Localized: Malar "butterfly" rash (spares nasolabial folds).
- Generalized: Widespread maculopapular rash on sun-exposed areas.
- Strongly associated with systemic disease activity.
- Subacute Cutaneous LE (SCLE):
- Highly photosensitive, non-scarring, non-indurated lesions.
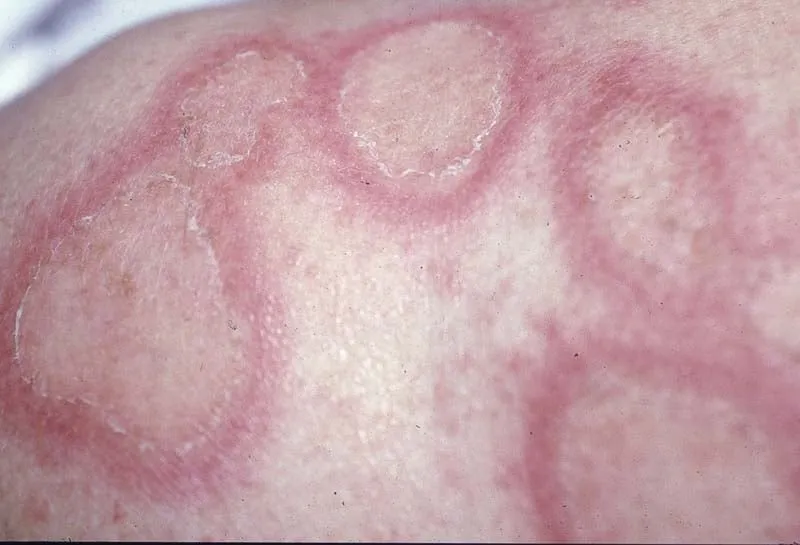
- Forms: Papulosquamous (psoriasiform) or annular/polycyclic.
- Often Anti-Ro/SSA positive; can be drug-induced (e.g., HCTZ, terbinafine).
- Chronic Cutaneous LE (CCLE):
- Discoid LE (DLE) - most common CCLE:
- Erythematous indurated plaques, adherent scale, follicular plugging.
- Leads to atrophy, scarring, dyspigmentation.
- Sites: Face, scalp (scarring alopecia), ears.
- 📌 DLE: A SCAR (Atrophy, Scale, Central hypopigmentation/depigmentation, Active erythematous border, Rim of hyperpigmentation, Follicular plugging).
- Other forms: LE profundus (panniculitis), Chilblain lupus, Tumid lupus.
- Discoid LE (DLE) - most common CCLE:
- Acute Cutaneous LE (ACLE):
- Other Mucocutaneous Manifestations:
- Painless oral/nasal ulcers.
- Non-scarring diffuse alopecia ("lupus hair").
- Raynaud's phenomenon, Livedo reticularis, cutaneous vasculitis.

⭐ The malar rash in ACLE characteristically spares the nasolabial folds, a key diagnostic clue.
Spotting SLE - Lupus Detectives
- EULAR/ACR Criteria (2019):
- Entry: ANA titer ≥1:80.
- Score ≥10 for classification.
- Mucocutaneous: Non-scarring alopecia (2), Oral ulcers (2), SCLE/DLE (4), Acute cutaneous lupus (6).
- Investigations:
-
Skin Biopsy (lesional): Interface dermatitis, liquefaction degeneration, epidermal atrophy, thickened BM (PAS+).
-
DIF/LBT: Granular IgG, IgM, C3 at DEJ. Lesional (>90%), sun-exposed non-lesional (SLE ~50-70%).
-
Serology: ANA (>95%), Anti-dsDNA (activity, nephritis), Anti-Sm (specific). 📌 'S'm 'S'pecific, d'S'dna 'S'evere. Low C3/C4.
- Others: Anti-Ro/SSA (SCLE, neonatal lupus), Anti-La/SSB, Anti-U1 RNP, Anti-histone (drug-induced).
-
- Diagnostic Flow (Simplified):
⭐ A positive Lupus Band Test (IgG at DEJ) in sun-exposed, non-lesional skin is highly suggestive of systemic lupus erythematosus.
Managing the Wolf - Skin Shield
- General: Photoprotection (broad-spectrum sunscreen SPF $ \ge 30-50 $, protective clothing, sun avoidance), Smoking cessation, Vitamin D.
- Topical (CLE):
- Corticosteroids: Potent (clobetasol - DLE); mid-potency. Risk: atrophy.
- Calcineurin inhibitors: Tacrolimus, pimecrolimus (face, steroid-sparing).
- Systemic (Severe CLE/SLE):
- Antimalarials: HCQ ($ \le 5 \text{ mg/kg/day} $ actual body weight) or Chloroquine. 1st line CLE & mild SLE. Ophthalmology screen (retinal toxicity).
- Systemic Corticosteroids: Prednisolone for flares/severe disease, tapered.
- Immunosuppressants: MTX, AZA, MMF (refractory CLE, steroid-sparing).
- Biologics: Belimumab, Rituximab, Anifrolumab (refractory/severe SLE).
- Other: Dapsone, Thalidomide (refractory DLE, teratogenicity/neuropathy risk).
⭐ Hydroxychloroquine is a cornerstone in managing cutaneous lupus; requires baseline and annual ophthalmological screening after 5 years (or sooner with risk factors).
High‑Yield Points - ⚡ Biggest Takeaways
- Malar rash: Classic photosensitive "butterfly" erythema, spares nasolabial folds.
- Discoid Lupus (DLE): Erythematous plaques, scale, follicular plugging; causes scarring alopecia, dyspigmentation.
- Subacute Cutaneous LE (SCLE): Highly photosensitive, non-scarring; strong anti-Ro/SSA association.
- Lupus profundus: Deep, firm nodules (panniculitis); may result in lipoatrophy.
- Oral ulcers: Typically painless, common on palate/buccal mucosa.
- Key Serology: ANA >95%; anti-dsDNA & anti-Sm highly specific.
- Drug-induced SLE: Anti-histone Ab positive; skin signs less common.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

