Dermatomyositis - Violet Violator
- Autoimmune; skin (violaceous rashes) & proximal muscle weakness.
- Key skin signs:
- Heliotrope rash (eyelids).
- Gottron's papules (knuckles, extensor surfaces).
- Other: Shawl/V-sign, mechanic's hands, periungual telangiectasia.
- Muscle: Symmetrical proximal weakness, dysphagia. ↑CK.
- Antibodies: Anti-Mi-2 (classic DM), Anti-Jo-1 (ILD), Anti-MDA5 (amyopathic DM, ↑ILD risk), Anti-TIF1-γ (cancer).
⭐ Strong association with internal malignancy in adults, especially > 40 years (e.g., ovarian, lung).
- Biopsy: Perifascicular atrophy. Tx: Corticosteroids.
Skin & Muscle Signs - Rash & Ache Attack
- Skin Manifestations (Dermato-):
- Pathognomonic:
- Heliotrope Rash: Violaceous eyelid discoloration ± edema.
- Gottron's Papules: Violaceous papules on knuckles (MCP, PIP, DIP).
- Characteristic:
- Gottron's Sign: Erythema over extensors (knees, elbows).
- Shawl Sign (back/shoulders) & V-Sign (neck/chest).
- Holster Sign (lateral thighs).
- Mechanic's Hands: Cracked, rough skin on fingers.
- Periungual changes: Telangiectasias, cuticular hypertrophy.
- Calcinosis cutis (esp. juvenile).
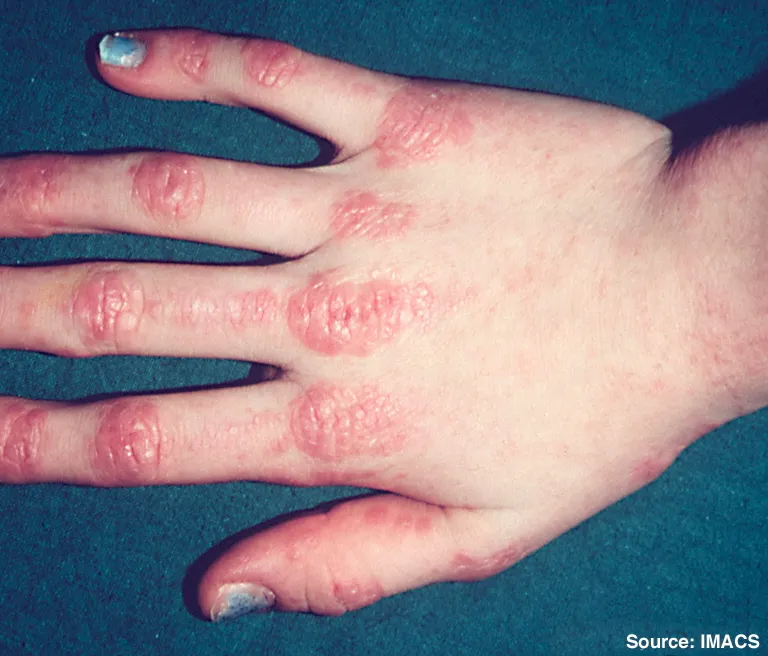
- Pathognomonic:
- Muscle Manifestations (-myositis):
- Symmetrical proximal muscle weakness (hips, thighs, shoulders, neck).
- Myalgia (muscle pain/tenderness).
- Dysphagia (difficulty swallowing).
- 📌 "Rash & Ache Attack" - skin and muscle involvement.
⭐ Gottron's papules are considered pathognomonic for Dermatomyositis.
Diagnostic Workup - Clue Hunt Central
- Bloods:
- ↑ CK (Creatine Kinase), ↑ Aldolase, ↑ LDH, ↑ AST, ↑ ALT.
- ANA (Anti-Nuclear Antibody) often positive.
- Myositis Specific Antibodies (MSAs):
- Anti-Jo-1 (common; ILD, mechanic's hands, arthritis).
- Anti-Mi-2 (classic DM skin signs, good prognosis).
- Anti-MDA5 (CADM, rapidly progressive ILD, skin ulcers).
- Anti-TIF1-γ (cancer-associated DM in adults, severe skin disease).
- Anti-NXP2 (calcinosis in JDM, cancer in adults).
- EMG (Electromyography): Myopathic pattern (↑ insertional activity, fibrillations, small polyphasic MUAPs).
- Biopsy:
- Muscle: Perifascicular atrophy (hallmark), CD4+ T cell & B-cell infiltrates.
- Skin: Interface dermatitis, liquefaction degeneration of basal layer, dermal mucin.
- Imaging:
- MRI: Muscle edema (STIR/T2-weighted images).
- HRCT Chest: For Interstitial Lung Disease (ILD) screening.
- Malignancy Screen: Age-appropriate, crucial due to cancer association.

⭐ Anti-Mi-2 antibodies are highly specific for dermatomyositis and often correlate with classic skin findings and a good response to therapy.
Systemic & Cancer Links - Hidden Threats Unveiled
- Systemic Involvement:
- Pulmonary: Interstitial Lung Disease (ILD) (anti-Jo-1 Ab+), resp. muscle weakness.
- Cardiac: Myocarditis, arrhythmias, heart failure.
- GI: Dysphagia (esophageal), GERD.
- Musculoskeletal: Polyarthralgia, non-erosive arthritis.
- Calcinosis cutis: esp. juvenile DM.
- Malignancy Association (CADM):
- ↑ risk, esp. adults > 40 yrs. Screening vital.
- Malignancy: pre/co/post DM diagnosis.
- Common: Ovary, Lung, Pancreas, Stomach, Colorectal, Lymphoma.
- Abs: Anti-TIF1-γ, anti-NXP2 link to ↑ cancer risk.
⭐ Up to 30% adult DM cases link to malignancy, often within 3 yrs of diagnosis.
Treatment & Outlook - Healing Path Forward
- First-line: Systemic corticosteroids (e.g., Prednisone 1 mg/kg/day).
- Steroid-sparing/Adjuncts: Immunosuppressants (Azathioprine, Methotrexate, Mycophenolate).
- Refractory/Severe Disease: IVIG, Rituximab.
- Skin Lesions: Topical corticosteroids, calcineurin inhibitors, hydroxychloroquine.
- Essential Supportive Care: Strict photoprotection, physiotherapy.
- Malignancy Surveillance: Regular screening vital due to ↑ risk.
- Outlook: Guarded, especially with malignancy, interstitial lung disease (ILD), or cardiac involvement.
⭐ Dermatomyositis patients have a 3-6x increased risk of malignancy, notably ovarian, lung, and gastrointestinal cancers.
High‑Yield Points - ⚡ Biggest Takeaways
- Heliotrope rash (violaceous periorbital edema) and Gottron's papules (violaceous papules on knuckles) are key.
- Symmetrical proximal muscle weakness is a hallmark, affecting daily activities.
- Significant risk of underlying malignancy in adults; screen for ovarian, lung, GI cancers.
- Anti-Mi-2 antibodies are specific for classic DM; Anti-Jo-1 indicates higher ILD risk.
- Elevated muscle enzymes (CK, aldolase) and characteristic EMG/muscle biopsy findings are diagnostic.
- Look for Shawl sign, V-sign, Holster sign, and Mechanic's hands.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

