Occupational Health

On this page
🏭 Occupational Health: The Workplace Wellness Command Center
Occupational health transforms every workplace into a complex ecosystem where chemical exposures, biological hazards, ergonomic strain, and psychological stress converge to shape worker wellbeing. You'll master the systematic approach to identifying workplace risks, from toxic substances and infectious agents to repetitive motion injuries and mental health challenges, then learn how to deploy targeted interventions that protect millions who spend a third of their lives on the job. This isn't abstract theory-it's the clinical framework that prevents disease before it starts and optimizes human performance where work happens.
The Occupational Health Architecture
Occupational health operates through four interconnected pillars that create comprehensive worker protection:
-
Primary Prevention (85% effectiveness)
- Hazard elimination at source design
- Engineering controls implementation
- Administrative policy development
- Exposure limit establishment: <50% of TLV
- Rotation schedules: maximum 6-hour shifts
- Training frequency: quarterly updates
-
Secondary Prevention (70% early detection rate)
- Health surveillance programs
- Biological monitoring protocols
- Pre-placement examinations
- Baseline spirometry: FEV1 >80% predicted
- Audiometry thresholds: <25 dB hearing level
- Vision screening: 20/40 corrected acuity
📌 Remember: SHIP - Surveillance, Hazard control, Injury prevention, Promotion of health
⭐ Clinical Pearl: Workers in high-risk industries show 3.2x higher rates of respiratory disease when pre-placement screening is inadequate, emphasizing the critical importance of baseline health assessment.
| Component | Primary Focus | Detection Rate | Cost-Effectiveness | Implementation Time | Compliance Rate |
|---|---|---|---|---|---|
| Health Surveillance | Early disease detection | 78% | High | 2-3 months | 92% |
| Hazard Control | Exposure reduction | 85% | Very High | 6-12 months | 87% |
| Medical Screening | Fitness assessment | 82% | Moderate | 1 month | 95% |
| Health Promotion | Wellness enhancement | 65% | High | 3-6 months | 73% |
| Emergency Response | Acute care | 95% | Critical | Immediate | 98% |
Connect these foundational principles through systematic hazard assessment to understand how workplace risks transform into measurable health outcomes.
🏭 Occupational Health: The Workplace Wellness Command Center
⚠️ Workplace Hazard Intelligence: The Risk Recognition Matrix
The Hazard Classification Command System
Physical Hazards: The Environmental Assault Matrix
-
Noise Exposure (>85 dB threshold)
- Sensorineural hearing loss: 16% prevalence in manufacturing
- Tinnitus development: onset at 90 dB continuous exposure
- Communication interference: productivity drops 23%
- Measurement frequency: annual audiometry
- Protection requirement: >90 dB environments
- Recovery time: 14-16 hours post-exposure
-
Vibration Hazards (>2.5 m/s² action level)
- Hand-Arm Vibration Syndrome: affects 2-3 million workers
- Whole-body vibration: spinal disorders increase 40%
- Vascular effects: blanching episodes after 2-5 years
📌 Remember: HAVS progression - History of tingling, Attacks of blanching, Vascular changes, Sensory loss
⭐ Clinical Pearl: Workers exposed to >5 m/s² hand-arm vibration for >2 hours daily develop Stage 1 HAVS within 12-24 months, making early intervention critical for prevention.
| Hazard Type | Exposure Limit | Health Effect | Latency Period | Detection Method | Prevention Efficacy |
|---|---|---|---|---|---|
| Noise | 85 dB TWA | Hearing loss | 5-10 years | Audiometry | 90% |
| Vibration | 2.5 m/s² | HAVS/Back pain | 2-5 years | Clinical exam | 85% |
| Heat | WBGT 28°C | Heat stress | Hours-days | Core temperature | 95% |
| Radiation | 20 mSv/year | Cancer risk | 10-20 years | Dosimetry | 98% |
| Cold | <10°C | Frostbite/hypothermia | Minutes-hours | Temperature monitoring | 92% |
Connect these physical exposures through chemical hazard pathways to understand how multiple workplace stressors create synergistic health risks.
⚠️ Workplace Hazard Intelligence: The Risk Recognition Matrix
🧪 Chemical Warfare: The Toxic Exposure Battlefield
The Toxicokinetic Pathway Framework
Chemical hazards operate through four critical pathways that determine biological impact:
-
Inhalation Route (80% of exposures)
- Alveolar absorption: surface area 70 m²
- Particle size critical: <5 μm reach alveoli
- Gas exchange efficiency: >90% for lipophilic compounds
- Respiratory rate increases: exposure × 2.5
- Minute ventilation: heavy work 50 L/min
- Retention efficiency: varies 20-95% by compound
-
Dermal Absorption (15% of exposures)
- Skin permeability: varies 1000-fold by location
- Penetration enhancers: solvents increase 10-50×
- Surface area exposure: palm = 1% body surface
📌 Remember: ADME - Absorption, Distribution, Metabolism, Excretion determines toxic potential
Heavy Metal Hazards: The Systemic Poisoners
-
Lead Exposure (blood level >40 μg/dL action)
- Neurological effects: IQ drops 2-3 points per 10 μg/dL
- Reproductive toxicity: sperm count ↓30% at 30 μg/dL
- Cardiovascular risk: hypertension increases 40%
- Half-life in blood: 30-35 days
- Bone storage: 90% total body burden
- Chelation threshold: >45 μg/dL in adults
-
Mercury Toxicity (urine >50 μg/L significant)
- CNS effects: tremor onset at 35 μg/L
- Kidney damage: proteinuria at 50 μg/L
- Elemental mercury: 80% lung absorption
⭐ Clinical Pearl: Workers with blood lead >30 μg/dL show measurable cognitive decline within 6 months, while levels >50 μg/dL require immediate removal from exposure and medical evaluation.
| Chemical Class | Exposure Route | Target Organ | Biomarker | Action Level | Health Effect Timeline |
|---|---|---|---|---|---|
| Heavy Metals | Inhalation/Dermal | CNS/Kidney | Blood/Urine levels | Pb: 40 μg/dL | Weeks-months |
| Solvents | Inhalation | CNS/Liver | Breath/Urine metabolites | 50% TLV | Hours-days |
| Pesticides | All routes | CNS/Cholinergic | Cholinesterase activity | 20% depression | Minutes-hours |
| Acids/Bases | Inhalation/Contact | Respiratory/Skin | pH monitoring | Immediate | Seconds-minutes |
| Carcinogens | Inhalation | Multiple organs | DNA adducts | No safe level | Years-decades |
Connect these chemical exposures through biological hazard pathways to understand how infectious agents create additional workplace health risks.
🧪 Chemical Warfare: The Toxic Exposure Battlefield
🦠 Biological Battlefield: The Infectious Agent Arsenal
The Biological Risk Stratification Matrix
Biological hazards operate through transmission pathway analysis that determines containment requirements:
-
Airborne Transmission (particle size <5 μm)
- Tuberculosis: infectivity 5-200 organisms
- SARS-CoV-2: viral load 10³-10⁶ copies/mL
- Aspergillus: spore concentration >1000/m³ hazardous
- Air changes required: 6-12 per hour
- Negative pressure: -2.5 Pa minimum
- HEPA filtration: 99.97% efficiency at 0.3 μm
-
Bloodborne Pathogens (highest transmission risk)
- HIV transmission: 0.3% per needlestick
- Hepatitis B: 30% transmission unvaccinated
- Hepatitis C: 1.8% per exposure average
- Viral survival: HBV 7 days on surfaces
- Infectious dose: HBV 10 virions
- Post-exposure window: <72 hours for prophylaxis
📌 Remember: TORCH pathogens - Toxoplasma, Other (syphilis, VZV), Rubella, CMV, HSV cause occupational reproductive risks
Biosafety Level Requirements: The Containment Hierarchy
⭐ Clinical Pearl: Healthcare workers in high-risk units (ICU, emergency) show 2.5x higher rates of respiratory infections, with vaccination compliance >90% reducing transmission by 70-85%.
| Biosafety Level | Pathogen Examples | Containment Features | PPE Requirements | Training Hours | Incident Rate |
|---|---|---|---|---|---|
| BSL-1 | E. coli K-12 | Open bench work | Gloves, lab coat | 8 hours | <0.1% |
| BSL-2 | Hepatitis B, HIV | Biosafety cabinet | Face protection added | 16 hours | 0.5% |
| BSL-3 | TB, SARS-CoV | Controlled access | Respiratory protection | 40 hours | 0.1% |
| BSL-4 | Ebola, Marburg | Maximum containment | Positive pressure suits | 80+ hours | <0.01% |
Connect these biological hazards through ergonomic risk factors to understand how physical workplace design creates musculoskeletal health challenges.
🦠 Biological Battlefield: The Infectious Agent Arsenal
🏗️ Ergonomic Engineering: The Human-Machine Interface Optimization
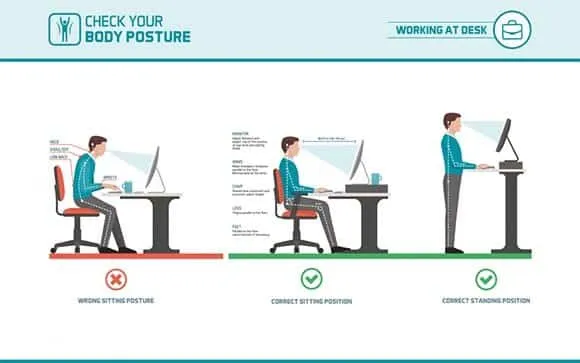
The Biomechanical Load Analysis Framework
Ergonomic hazards create measurable physiological stress through force amplification and repetitive strain:
-
Lifting Biomechanics (NIOSH equation application)
- Safe lifting limit: 23 kg under optimal conditions
- Spinal compression: 3400 N maximum acceptable
- Lifting frequency: >15 lifts/hour increases risk 2.5×
- Horizontal distance: >25 cm from body doubles risk
- Vertical height: knuckle to shoulder optimal zone
- Asymmetric lifting: >30° rotation adds 40% risk
-
Repetitive Motion Thresholds (CTD development)
- Hand/wrist cycles: >10,000 per day high risk
- Force requirements: >4 kg grip with repetition
- Awkward postures: >20° wrist deviation problematic
- Carpal tunnel incidence: 15.7 per 1000 high-risk workers
- Recovery time: nerve conduction 6-12 months
- Return-to-work: 85% success with early intervention
📌 Remember: HARM factors - High force, Awkward posture, Repetition, Mechanical stress
Workstation Design Optimization Matrix
- Visual Display Terminal (VDT) Ergonomics
- Screen distance: 50-70 cm optimal viewing
- Top of screen: at or below eye level
- Keyboard height: elbow angle 90-110°
- Blink rate reduction: 60% during computer work
- Eye strain symptoms: >4 hours continuous use
- Break frequency: 15 minutes every 2 hours
⭐ Clinical Pearl: Workers using non-adjustable workstations show 3.2× higher rates of neck and shoulder disorders, with anthropometric mismatch affecting 85% of standard workstation users.
| Risk Factor | Threshold Value | Health Outcome | Prevalence Rate | Intervention Effectiveness | Cost Impact |
|---|---|---|---|---|---|
| Lifting Force | >23 kg | Low back pain | 42% | 65% reduction | $12,000/case |
| Repetition Rate | >10,000 cycles/day | CTD development | 28% | 70% reduction | $8,500/case |
| Awkward Posture | >20° deviation | Joint disorders | 35% | 60% reduction | $6,200/case |
| Vibration | >2.5 m/s² | HAVS | 15% | 80% reduction | $15,000/case |
| Static Loading | >30% MVC | Muscle fatigue | 55% | 75% reduction | $3,800/case |
Connect these ergonomic stressors through psychosocial risk assessment to understand how workplace mental health factors amplify physical health risks.
🏗️ Ergonomic Engineering: The Human-Machine Interface Optimization
🧠 Psychosocial Pressure Points: The Mental Health Minefield
The Stress Response Amplification System
Psychosocial hazards create measurable physiological changes that compound other occupational risks:
-
Job Demand-Control Model (Karasek framework)
- High demand + Low control = 4× higher cardiovascular risk
- Psychological strain: cortisol elevation 200-400%
- Burnout prevalence: healthcare 50%, manufacturing 35%
- Decision latitude: autonomy reduces stress 60%
- Skill utilization: underuse increases turnover 45%
- Social support: buffers stress impact 30-50%
-
Effort-Reward Imbalance (Siegrist model)
- High effort + Low reward = depression risk 2.5×
- Job insecurity: anxiety disorders increase 80%
- Overcommitment: work-life balance deterioration
- Overtime threshold: >48 hours/week health impact
- Recovery time: 48-72 hours between high-stress periods
- Intervention effectiveness: stress management 40% reduction
📌 Remember: DRIVE stressors - Demands, Reward imbalance, Insecurity, Violence, Effort without recognition
Workplace Violence Risk Assessment Matrix
⭐ Clinical Pearl: Healthcare workers experience 5× higher rates of workplace violence than other industries, with 75% of assaults occurring in psychiatric units and emergency departments, requiring specialized prevention protocols.
| Psychosocial Factor | Risk Threshold | Health Impact | Prevalence | Intervention Success | Economic Cost |
|---|---|---|---|---|---|
| Job Strain | High demand/Low control | CVD risk 4× | 25% | 50% reduction | $3,400/worker |
| Workplace Violence | >2 incidents/year | PTSD 15% | 8% | 70% reduction | $55,000/incident |
| Shift Work | >5 night shifts/month | Sleep disorders 60% | 20% | 40% reduction | $2,100/worker |
| Job Insecurity | Layoff probability >25% | Depression 2.5× | 15% | 35% reduction | $4,700/worker |
| Bullying | Weekly occurrence | Anxiety 3× | 12% | 60% reduction | $6,200/worker |
Connect these psychosocial stressors through comprehensive risk assessment methodologies to understand how systematic evaluation creates effective prevention strategies.
🧠 Psychosocial Pressure Points: The Mental Health Minefield
🎯 Occupational Health Mastery: The Clinical Command Arsenal
The Essential Clinical Arsenal
Rapid Assessment Framework:
- Exposure Assessment: TLV comparison + biological monitoring + environmental sampling
- Health Surveillance: Pre-placement + periodic + post-exposure examinations
- Risk Stratification: High (>50% TLV), Moderate (25-50% TLV), Low (<25% TLV)
- Intervention Hierarchy: Elimination > Substitution > Engineering > Administrative > PPE
📌 Remember: PEACE protocol - Prevent exposure, Evaluate risks, Assess health, Control hazards, Educate workers
⭐ Clinical Pearl: Workplaces implementing comprehensive occupational health programs show 40-60% reduction in injury rates and 25-35% decrease in workers' compensation costs within 2-3 years.
| Intervention Level | Effectiveness | Implementation Cost | Timeline | Sustainability | Worker Acceptance |
|---|---|---|---|---|---|
| Elimination | 95-100% | High initial | 6-18 months | Permanent | 90% |
| Substitution | 80-95% | Moderate | 3-12 months | High | 85% |
| Engineering | 70-90% | Moderate-High | 2-8 months | High | 80% |
| Administrative | 40-70% | Low-Moderate | 1-3 months | Moderate | 65% |
| PPE | 60-85% | Low | Immediate | Low | 60% |
Connect this mastery framework through continuous improvement methodologies to build sustainable workplace health programs that evolve with emerging occupational risks and technological advances.
🎯 Occupational Health Mastery: The Clinical Command Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app























