Intranatal Care Intro - Setting the Stage
- Intranatal Care (INC): Care from true labour onset to placental expulsion.
- Labour (Parturition): Expulsion of foetus & placenta.
- Eutocia: Normal. Dystocia: Abnormal.
- Labour Onset Signs:
- Progressive, painful uterine contractions.
- Show (blood-mucus).
- Cervical dilatation & effacement.
- Bag of forewaters.
- True Labour: Regular, progressive contractions; cervical changes; pain radiates; not relieved by sedatives.
- False Labour: Irregular; no cervical change; pain localized; relieved by sedatives.
⭐ Progressive cervical effacement & dilatation signify true labour.
Labour's Journey - Stages & Events
- Stage 1 (Cervical Dilation): True pains to full cervical dilation (10 cm). Effacement & dilation.
- Latent: 0-4 cm (P: 6-8h, M: 4-6h).
- Active: 4-10 cm (P: 1.2 cm/hr, M: 1.5 cm/hr).
- Stage 2 (Fetal Expulsion): Full dilation to fetal expulsion. Cardinal movements.
- Duration: P: 1-2h, M: 30m-1h (longer with epidural).
⭐ Crowning: Widest part of fetal head visible at introitus, no recession.
- Stage 3 (Placental Expulsion): Fetal expulsion to placenta expulsion. Separation & expulsion.
- Duration: 5-15 min (max 30 min).
- Signs: 📌 CUG (Cord lengthens, Uterus globular, Gush of blood).
- Stage 4 (Observation): 1-4h post-placenta.
- Monitor: Uterine tone, vitals, PPH.

Partograph Power - Monitoring Labour

- Graphical tool for monitoring labour: FHR, cervical dilatation (X), descent (O), contractions, maternal vitals.
- WHO Modified Partograph: Plotting begins at 4 cm cervical dilatation (active phase).
- Alert Line: Crossed if cervical dilatation is < 1 cm/hr. Signals need for careful reassessment, possible conservative measures (e.g., hydration, amniotomy).
- Action Line: Typically 4 hours to the right of Alert Line. Crossing indicates need for decisive action (e.g., oxytocin augmentation, Caesarean section).
⭐ The partograph is a key tool to prevent prolonged labour, a major cause of maternal/neonatal morbidity.
Safe Arrivals - Newborn & Maternal Care
- Maternal Care (AMTSL - Active Management of Third Stage of Labour): Prevents PPH.
- Oxytocin 10 IU IM (within 1 min of birth).
- Controlled Cord Traction (CCT).
- Uterine massage post-placental delivery.
- Newborn Care:
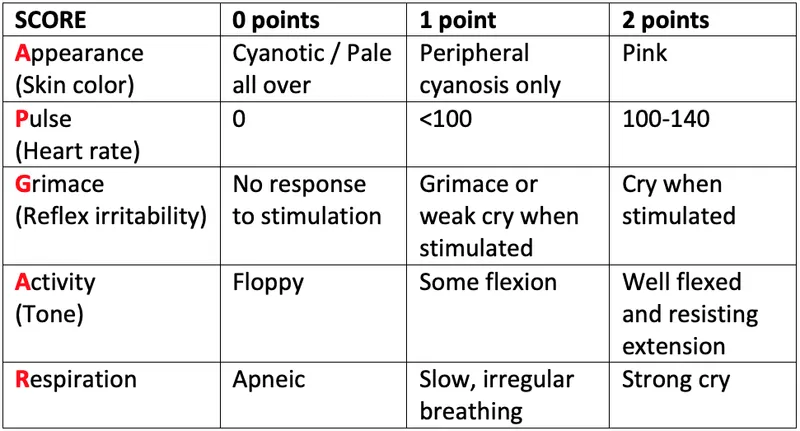
- APGAR Score: At 1 & 5 min. Assesses 5 vital signs. Score <7 distress, <4 severe.
- Neonatal Resuscitation (NRP): See flowchart for initial steps. Golden minute for ventilation.
⭐ AMTSL reduces Postpartum Hemorrhage (PPH) incidence by ~60%.
High‑Yield Points - ⚡ Biggest Takeaways
- AMTSL (oxytocin, CCT, uterine massage) is key to prevent Postpartum Hemorrhage (PPH).
- Partograph monitors labor: alert line for observation, action line for intervention.
- Essential Newborn Care (ENC): immediate drying/warming, early breastfeeding, Vitamin K, cord care.
- Median episiotomy is preferred, performed at crowning to prevent severe tears.
- Six Cleans (hands, surface, perineum, blade, cord tie/clamp, towel) ensure aseptic delivery.
- Magnesium sulfate is the first-line drug for intrapartum eclampsia management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

