Purine Synthesis - Building Blocks of Life
- De novo pathway: Primary route for purine nucleotide formation, mainly in the liver.
- Starting material: Ribose-5-phosphate, converted to PRPP (Phosphoribosyl pyrophosphate).
- Key intermediate: IMP (Inosine Monophosphate) - the parent purine nucleotide.
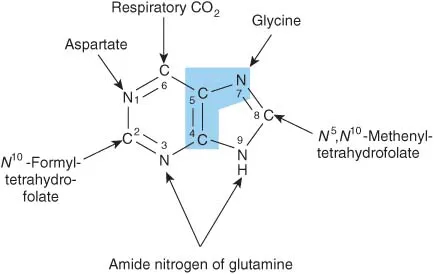
- Purine ring sources:
- Aspartate (N1)
- N10-Formyl-THF (C2, C8)
- Glutamine (N3, N9)
- Glycine (C4, C5, N7)
- $CO_2$ (C6) 📌 Mnemonic for sources: "Glycine, Aspartate, Glutamine, $CO_2$, Formyl-THF" (GAG-CF).
- Rate-limiting enzyme: Glutamine PRPP amidotransferase.
- Subject to feedback inhibition by AMP, GMP, and IMP.
- Activated by PRPP.
⭐ IMP is the common precursor from which AMP and GMP are synthesized, representing a critical branch point in purine metabolism.
Purine Degradation - The Uric Acid Trail
- Endogenous (cell turnover) and dietary purine nucleotides (AMP, GMP) are catabolized to uric acid.
- Key Enzymes & Conversions:
- Adenosine Deaminase (ADA): Converts Adenosine $\rightarrow$ Inosine. (📌 ADA deficiency causes Severe Combined Immunodeficiency - SCID).
- Purine Nucleoside Phosphorylase (PNP): Inosine $\rightarrow$ Hypoxanthine; Guanosine $\rightarrow$ Guanine. (Deficiency impairs T-cell immunity).
- Guanase: Guanine $\rightarrow$ Xanthine.
- Xanthine Oxidase (XO): Catalyzes Hypoxanthine $\rightarrow$ Xanthine, then Xanthine $\rightarrow$ Uric Acid. A molybdenum-containing enzyme.
- Uric acid is the final product, excreted mainly by kidneys. Elevated levels cause gout.

⭐ Xanthine Oxidase (XO) is the primary target for urate-lowering therapy in gout; Allopurinol and Febuxostat are key inhibitors.
Purine Disorders - When Metabolism Goes Wrong
- Gout:
- Cause: Hyperuricemia (↑ uric acid > 6.8 mg/dL).
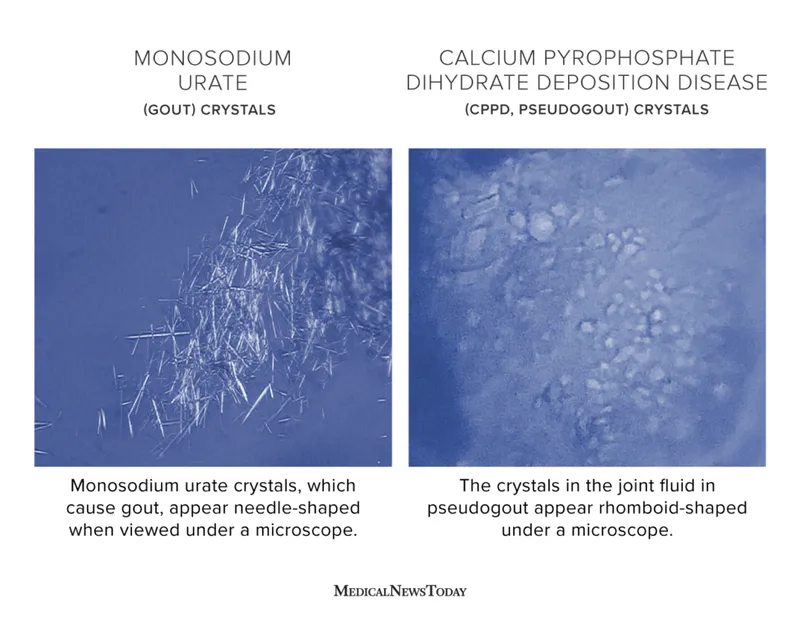
- Patho: Monosodium urate (MSU) crystal deposition in joints (podagra) & soft tissues (tophi).
- Rx: Allopurinol (xanthine oxidase inhibitor).
- Lesch-Nyhan Syndrome (LNS):
- Defect: HGPRT deficiency (X-linked recessive).
- Features: Hyperuricemia, gout, dystonia, choreoathetosis, self-mutilation, intellectual disability. 📌 HGPRT: He's Got Purinic Rage & Tics.
- Adenosine Deaminase (ADA) Deficiency:
- Defect: ADA enzyme.
- Result: dATP accumulation, toxic to lymphocytes.
- Clinical: Severe Combined Immunodeficiency (SCID) - B & T cell defect.
⭐ ADA deficiency is a major cause of autosomal recessive SCID.
- Purine Nucleoside Phosphorylase (PNP) Deficiency:
- Defect: PNP enzyme.
- Result: dGTP accumulation.
- Clinical: Impaired T-cell function; recurrent infections.
- Xanthinuria:
- Defect: Xanthine oxidase deficiency.
- Result: ↑ xanthine, ↓ uric acid.
- Clinical: Xanthine kidney stones.
Purine Pharmacology - Drug Targets & Therapies
- Xanthine Oxidase Inhibitors:
- Allopurinol, Febuxostat: ↓ Uric acid production. For gout, tumor lysis syndrome.
- Uricosuric Agents:
- Probenecid, Lesinurad: ↑ Renal uric acid excretion.
- Recombinant Uricases:
- Rasburicase, Pegloticase: Convert uric acid to allantoin. For refractory gout.
- Antimetabolites (Inhibit Purine Synthesis):
- Azathioprine (prodrug), 6-Mercaptopurine (6-MP), 6-Thioguanine (6-TG):
- 📌 Thiopurines; inhibit de novo synthesis. Used in ALL, IBD.
- Mycophenolate Mofetil: Inhibits IMP Dehydrogenase. For transplant rejection.
- Azathioprine (prodrug), 6-Mercaptopurine (6-MP), 6-Thioguanine (6-TG):
- Other Purine Analogs:
- Cladribine, Fludarabine (anticancer).
- Acyclovir, Ganciclovir (antiviral).
⭐ Allopurinol inhibits xanthine oxidase, reducing uric acid. It also inhibits metabolism of azathioprine/6-MP, requiring their dose reduction to prevent toxicity.
High‑Yield Points - ⚡ Biggest Takeaways
- De novo purine synthesis needs PRPP, glycine, aspartate, glutamine, CO2, THF; mainly in liver.
- HGPRT deficiency: Lesch-Nyhan syndrome (Hyperuricemia, Gout, Pissed off, Retardation, DysTonia).
- ADA deficiency: SCID due to ↑dATP, toxic to lymphocytes.
- Xanthine oxidase (hypoxanthine → xanthine → uric acid) inhibited by allopurinol, febuxostat.
- Gout: hyperuricemia; acute: NSAIDs, colchicine, steroids; chronic: allopurinol.
- Tumor Lysis Syndrome: ↑uric acid, ↑K+, ↑PO43-, ↓Ca2+; manage: hydration, allopurinol/rasburicase.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

