Isoenzyme Fundamentals - Same Job, Different Style
- Definition: Different molecular forms of an enzyme catalyzing the same reaction.
- Origin:
- Encoded by distinct genes (true isoenzymes).
- Arise from post-translational modifications.
- Distinct Properties:
- Vary in amino acid sequence.
- Differ in physical (electrophoresis, heat stability), chemical, and immunological traits.
- May have different kinetic values ($K_m$, $V_{max}$), affecting substrate affinity/efficiency.
- Tissue Specificity: Often unique to specific tissues or organelles.
- Clinical Use: Crucial as diagnostic markers due to tissue-specific expression.
⭐ Isoenzymes catalyze the same reaction but differ in amino acid sequence, leading to distinct electrophoretic mobility and immunological properties, vital for clinical identification.
Creatine Kinase (CK) Crew - Heartfelt Markers
- Dimer: Two subunits - M (Muscle), B (Brain).
- Isoenzymes:
- CK-MM (Muscle): ~98% total CK.
- Source: Skeletal muscle.
- ↑ in: Rhabdomyolysis, muscular dystrophy, strenuous exercise.
- CK-MB (Myocardium): <6% total CK. Cardiac muscle. Key MI marker.
- Rises: 4-6 hrs post-MI.
- Peaks: 12-24 hrs.
- Normalizes: 48-72 hrs.
- Useful for re-infarction detection.
- CK-BB (Brain):
- Source: Brain, GI tract, GU tract.
- ↑ in: CNS damage (stroke, injury), certain cancers (e.g., prostate).
- CK-MM (Muscle): ~98% total CK.
- CK-MB Relative Index:
- Formula: $ \frac{CK-MB \text{ mass}}{\text{Total CK activity}} \times 100% $
- 📌 CK-MB: Myocardial Band.
⭐ A CK-MB relative index > 6% is highly suggestive of myocardial injury, offering greater specificity for MI than CK-MB levels alone.
Lactate Dehydrogenase (LDH) League - Damage Detectives
- Catalyzes lactate $ ightleftharpoons $ pyruvate. Tetramer of H (Heart) & M (Muscle) subunits.
- 5 Isoenzymes:
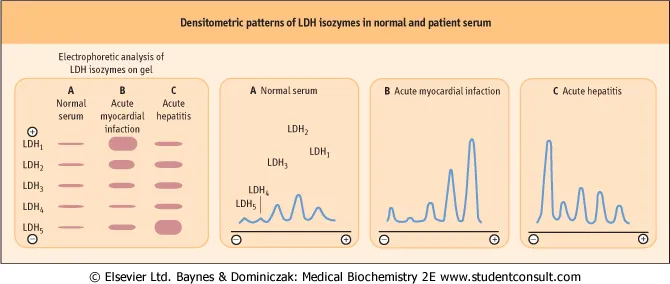
Isoenzyme (Subunits) Predominant Tissue(s) Clinical Significance (↑ LDH) LDH-1 (H4) Heart, RBCs, Kidney MI (late), Hemolytic/Pernicious Anemia LDH-2 (H3M1) Heart, RBCs Highest in serum normally LDH-3 (H2M2) Lungs, Pancreas, Lymphoid Pulm. issues, Lymphoma, Leukemia LDH-4 (H1M3) Liver, Sk. Muscle Non-specific liver/muscle damage LDH-5 (M4) Liver, Sk. Muscle Hepatitis, Cirrhosis, Muscle injury - General Marker: Tissue injury, hemolysis, widespread malignancy.
- MI Diagnosis:
- Rises 12-24 hrs post-MI, peaks 48-72 hrs, normalizes 7-12 days.
- Useful for delayed diagnosis.
⭐ Flipped Pattern: In MI, LDH-1 > LDH-2 (normally LDH-2 > LDH-1).
- 📌 Mnemonic (LDH 1-5 Tissues): R.H.L.L.S - "Red cells/Renal, Heart, Lungs, Liver, Skeletal muscle."
Other Clinically Key Isoenzymes - The Specialists
- Alkaline Phosphatase (ALP)
- Sources: Liver, Bone, Intestine, Placenta.
- Heat: Liver/Placental (Regan) stable; Bone labile. 📌 Bone Burns, Liver Lives.
- ↑ Cholestasis, Paget's, pregnancy, bone mets. Regan: paraneoplastic.
- Acid Phosphatase (ACP)
- Prostatic (PAP): Metastatic prostate Ca marker.
- Tartrate-Resistant (TRAP):
⭐ TRAP: Key diagnostic marker for Hairy Cell Leukemia.
- Amylase
- P-type (pancreas, specific for pancreatitis), S-type (saliva).
- ↑ Acute pancreatitis, mumps, renal failure, DKA.
- Gamma-Glutamyl Transferase (GGT)
- ↑ Hepatobiliary disease, chronic alcohol use. Confirms hepatic origin of ↑ALP.
- 5'-Nucleotidase (5'-NT)
- Specific for hepatobiliary obstruction. Differentiates liver vs. bone source of ↑ALP.
High‑Yield Points - ⚡ Biggest Takeaways
- Isoenzymes: Multiple forms of an enzyme; same reaction, different properties & tissue distribution.
- Clinical utility: Key diagnostic markers for specific organ damage (e.g., heart, liver).
- CK-MB: Highly specific for Myocardial Infarction (MI); rises in 4-6 hours, peaks at 24 hours.
- LDH isoenzymes: LDH1 (heart), LDH5 (liver/muscle); LDH1 > LDH2 (flipped ratio) strongly suggests MI.
- ALP isoenzymes differentiate liver vs. bone origin; Amylase/Lipase for pancreatitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

