Trauma Anesthesia

On this page
🚨 Trauma Anesthesia: The Critical Care Battlefield
Trauma anesthesia demands split-second decisions where physiology meets chaos and every intervention cascades through multiple organ systems simultaneously. You'll master the systematic approach to securing airways in patients with full stomachs and potential cervical injuries, resuscitating circulation while avoiding the lethal triad, and orchestrating intraoperative care when bleeding, hypothermia, and coagulopathy converge. This lesson builds your framework for recognizing patterns, anticipating complications, and executing protocols that transform unstable trauma patients into surgical survivors.
📌 Remember: CRASH - Coagulopathy, Rapid sequence induction, Acidosis, Shock management, Hypothermia prevention. These five pillars define trauma anesthesia priorities with mortality increasing 15-20% for each untreated component.
The physiological derangements in trauma patients create a perfect storm of anesthetic challenges. Hemorrhagic shock reduces circulating blood volume by 30-40%, while metabolic acidosis (pH <7.25) impairs cardiac contractility and drug metabolism. Hypothermia below 35°C increases mortality by 300% and significantly prolongs surgical bleeding times.
| Parameter | Normal | Mild Trauma | Severe Trauma | Critical Threshold | Mortality Risk |
|---|---|---|---|---|---|
| Blood Loss | 0% | 15-30% | >40% | >50% | 50% increase |
| Base Deficit | 0-2 mEq/L | 3-5 mEq/L | 6-14 mEq/L | >15 mEq/L | 75% mortality |
| Core Temp | 37°C | 35-36°C | 32-34°C | <32°C | 100% mortality |
| Lactate | <2 mmol/L | 2-4 mmol/L | 4-8 mmol/L | >8 mmol/L | 80% mortality |
| INR | 0.9-1.1 | 1.2-1.5 | 1.6-2.0 | >2.5 | Massive bleeding |
- Hemodynamic Instability Patterns
- Class I shock: <15% blood loss, compensated vital signs
- Class II shock: 15-30% loss, tachycardia >100 bpm, narrow pulse pressure
- Urine output decreases to 20-30 mL/hr
- Anxiety and mild confusion emerge
- Class III shock: 30-40% loss, hypotension, altered mental status
- Heart rate >120 bpm, systolic BP <100 mmHg
- Urine output <20 mL/hr, marked confusion
- Class IV shock: >40% loss, profound hypotension, unconsciousness
- Heart rate >140 bpm, systolic BP <70 mmHg
- Negligible urine output, coma
💡 Master This: Trauma-induced coagulopathy occurs in 25% of severe trauma patients within 30 minutes of injury, independent of fluid resuscitation. Early recognition and targeted therapy with tranexamic acid (1g IV) reduces mortality by 1.5% when given within 3 hours.
Understanding trauma anesthesia physiology establishes the foundation for managing airway challenges in the next critical phase of care.
🚨 Trauma Anesthesia: The Critical Care Battlefield
🫁 Airway Command Center: Trauma's First Battleground
📌 Remember: LEMON assessment for difficult airways - Look externally, Evaluate 3-3-2 rule, Mallampati score, Obstruction/obesity, Neck mobility. In trauma, add CRASH factors: Cervical spine, Rapid sequence, Aspiration risk, Shock, Hemorrhage affecting visualization.
The 3-3-2 rule becomes critical in trauma assessment: 3 fingers mouth opening (4-5 cm), 3 fingers thyromental distance (6-7 cm), 2 fingers thyrosternal distance (4 cm). Facial trauma can reduce mouth opening to <2 cm, making direct laryngoscopy impossible and necessitating fiberoptic intubation or surgical airway.
| Airway Challenge | Incidence | Primary Concern | Management Strategy | Success Rate |
|---|---|---|---|---|
| Cervical Injury | 2-5% | Neurological damage | Manual in-line stabilization | 95% |
| Facial Trauma | 15-20% | Difficult visualization | Video laryngoscopy | 85% |
| Laryngeal Injury | 1-2% | Complete obstruction | Surgical airway | 90% |
| Full Stomach | 100% | Aspiration | Rapid sequence induction | 98% |
| Hemodynamic Shock | 30-40% | Cardiovascular collapse | Modified drug doses | 92% |
- Rapid Sequence Induction Modifications
- Etomidate 0.2-0.3 mg/kg: maintains hemodynamic stability in shock
- Ketamine 1-2 mg/kg: preserves sympathetic tone, bronchodilation
- Avoid in traumatic brain injury with elevated ICP
- Maintains respiratory drive if intubation fails
- Succinylcholine 1.5 mg/kg: rapid onset 45-60 seconds
- Contraindicated in burns >48 hours, crush injuries
- Risk of hyperkalemia and cardiac arrest
- Rocuronium 1.2 mg/kg: alternative with 60-90 second onset
- Reversible with sugammadex if needed
- Preferred in suspected hyperkalemia risk
💡 Master This: Cricoid pressure effectiveness is controversial in trauma. BURP maneuver (Backward, Upward, Rightward Pressure) on thyroid cartilage improves laryngeal view in 65% of difficult cases while avoiding potential cervical spine movement from cricoid pressure.
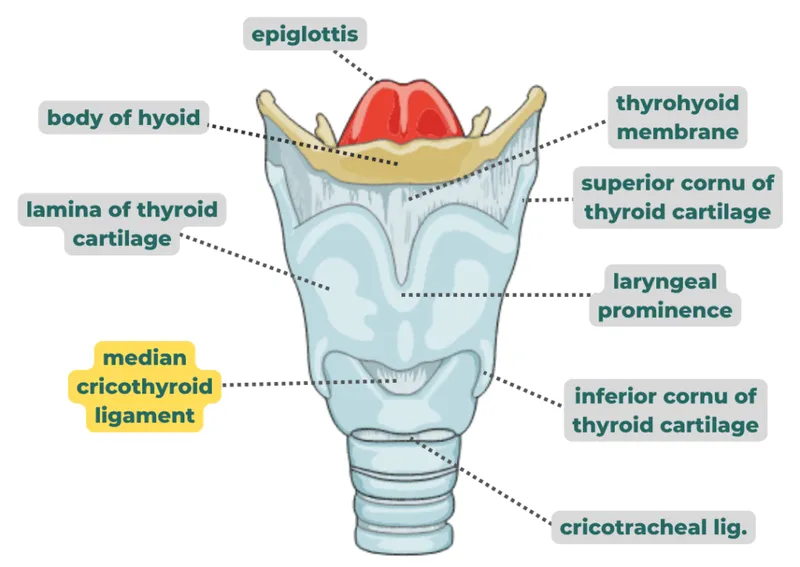
Surgical airway becomes necessary in 2-5% of trauma cases when intubation fails. The cricothyroid membrane measures 8-10 mm vertically and 30 mm horizontally, located between the thyroid and cricoid cartilages. Needle cricothyrotomy provides temporary oxygenation for 30-45 minutes, while surgical cricothyrotomy offers definitive airway control.
Mastering trauma airway management sets the stage for understanding hemodynamic optimization during the critical resuscitation phase.
🫁 Airway Command Center: Trauma's First Battleground
🩸 Hemodynamic Optimization: The Circulation Equation

📌 Remember: HALT the lethal triad - Hypothermia (<35°C), Acidosis (pH <7.25), Lactate elevation (>4 mmol/L), Traumatic coagulopathy (INR >1.5). Each component increases mortality exponentially when combined.
Permissive hypotension targets systolic blood pressure 80-90 mmHg in penetrating trauma and 90-100 mmHg in blunt trauma until hemorrhage control. This strategy reduces bleeding by 40% while maintaining cerebral and coronary perfusion pressure above critical thresholds of 60 mmHg and 40 mmHg respectively.
| Resuscitation Strategy | Target Parameter | Clinical Benefit | Mortality Reduction | Time Window |
|---|---|---|---|---|
| Permissive Hypotension | SBP 80-90 mmHg | Reduced bleeding | 15-20% | Until hemostasis |
| Balanced Transfusion | 1:1:1 ratio | Improved coagulation | 25% | First 24 hours |
| Early TXA | Within 3 hours | Reduced fibrinolysis | 1.5% | 3-hour window |
| Damage Control | <90 minutes | Prevent triad | 30% | Golden hour |
| Goal-Directed Therapy | ScvO2 >70% | Tissue perfusion | 10% | First 6 hours |
- Fluid Resuscitation Hierarchy
- Crystalloids: Normal saline limited to 1-2 liters maximum
- Risk of hyperchloremic acidosis with large volumes
- Lactated Ringer's preferred for balanced electrolytes
- Colloids: Albumin 5% for oncotic pressure maintenance
- Hetastarch avoided due to coagulopathy risk
- Fresh frozen plasma for coagulation factor replacement
- Blood Products: 1:1:1 ratio of PRBC:FFP:Platelets
- Type O negative for emergency transfusion
- Massive transfusion protocol for ongoing bleeding
- Crystalloids: Normal saline limited to 1-2 liters maximum
💡 Master This: Thromboelastography (TEG) provides real-time coagulation assessment in 15 minutes versus 45-60 minutes for traditional coagulation studies. R-time >8 minutes indicates factor deficiency, K-time >3 minutes suggests fibrinogen deficiency, and MA <55 mm indicates platelet dysfunction.
Vasopressor selection in trauma requires understanding of underlying pathophysiology. Norepinephrine 0.1-0.5 mcg/kg/min provides balanced α and β effects for distributive shock, while vasopressin 0.01-0.04 units/min offers non-catecholamine vasoconstriction in catecholamine-resistant shock. Epinephrine is reserved for cardiac arrest scenarios due to increased lactate production.

Advanced monitoring becomes crucial in complex trauma cases. Arterial line placement provides beat-to-beat blood pressure monitoring and frequent blood gas analysis. Central venous pressure monitoring guides fluid therapy, while ScvO2 >70% indicates adequate tissue oxygen delivery. Lactate clearance >10% per hour suggests successful resuscitation.
Understanding hemodynamic optimization principles prepares us for managing the complex anesthetic considerations during trauma surgery.
🩸 Hemodynamic Optimization: The Circulation Equation
⚔️ Intraoperative Anesthesia: The Surgical Theater Strategy
📌 Remember: WARM patient management - Warm fluids and blood products, Avoid hypothermia with forced air warming, Rapid infusion devices for volume replacement, Monitor core temperature continuously. Every 1°C temperature drop increases bleeding by 16% and mortality by 20%.
Anesthetic depth in trauma patients requires careful titration due to altered pharmacokinetics and hemodynamic instability. Hypovolemia increases drug sensitivity by 30-50%, while acidosis prolongs drug elimination. BIS monitoring helps maintain adequate depth (40-60) while avoiding overdose in hemodynamically compromised patients.
| Anesthetic Agent | Trauma Dose | Hemodynamic Effect | Duration Change | Special Considerations |
|---|---|---|---|---|
| Propofol | 0.5-1 mg/kg | Hypotension risk | Prolonged 50% | Avoid in shock |
| Etomidate | 0.1-0.2 mg/kg | Stable BP | Normal | Adrenal suppression |
| Ketamine | 0.5-1 mg/kg | Maintains BP | Normal | Avoid in TBI |
| Sevoflurane | 0.5-1 MAC | Dose-dependent ↓BP | Normal | Rapid emergence |
| Desflurane | 0.5-1 MAC | Sympathetic stimulation | Fastest | Airway irritation |
- Multimodal Analgesia Strategy
- Regional anesthesia: Epidural for thoracic/abdominal trauma
- Contraindicated in coagulopathy (INR >1.5)
- Neuraxial blocks require normal coagulation
- Peripheral nerve blocks: Femoral for femur fractures
- Ultrasound-guided blocks reduce complications by 40%
- Continuous catheters for prolonged analgesia
- Systemic opioids: Fentanyl 2-5 mcg/kg for hemodynamic stability
- Morphine avoided in shock due to histamine release
- Remifentanil for rapid titration and emergence
- Regional anesthesia: Epidural for thoracic/abdominal trauma
💡 Master This: Damage control anesthesia prioritizes physiological restoration over complete surgical repair. Abbreviated procedures lasting <90 minutes prevent hypothermia and coagulopathy progression, with staged repairs performed after 24-48 hours of ICU optimization.
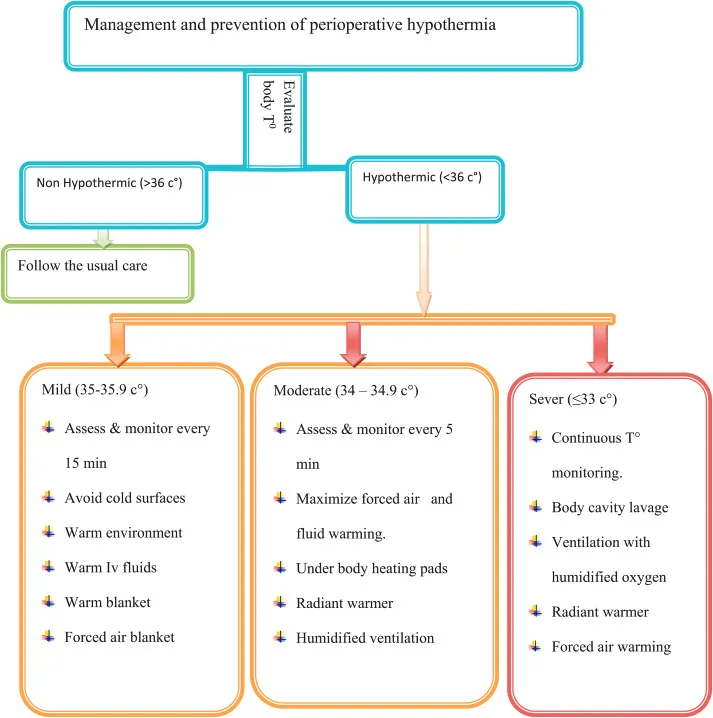
Temperature management becomes critical during prolonged trauma surgery. Forced air warming devices maintain core temperature above 36°C, while fluid warmers heat crystalloids and blood products to 37-40°C. Heat loss occurs through radiation (40%), convection (30%), evaporation (20%), and conduction (10%).
Coagulation monitoring during surgery guides blood product therapy. Point-of-care testing with TEG/ROTEM provides results in 15 minutes versus 45-60 minutes for laboratory studies. Fibrinogen levels <150 mg/dL require cryoprecipitate replacement, while platelet count <50,000 necessitates platelet transfusion.
Ventilator management in trauma patients requires lung-protective strategies. Tidal volumes of 6-8 mL/kg ideal body weight prevent ventilator-induced lung injury, while PEEP 5-10 cmH2O maintains functional residual capacity. Peak pressures <30 cmH2O and plateau pressures <25 cmH2O minimize barotrauma risk.
Mastering intraoperative management sets the foundation for understanding postoperative care and complication prevention.
⚔️ Intraoperative Anesthesia: The Surgical Theater Strategy
🏥 Postoperative Vigilance: The Recovery Command Post

📌 Remember: SOFA score monitoring - Sepsis-related Organ Failure Assessment tracks 6 organ systems with scores 0-4 each. SOFA >11 indicates >80% mortality risk, while daily increases >2 points suggest developing multiple organ dysfunction syndrome.
Respiratory complications occur in 30-40% of major trauma patients, with ARDS developing in 15-20% within 72 hours. Ventilator-associated pneumonia risk increases 1-3% per day of mechanical ventilation, while pulmonary embolism occurs in 2-5% of trauma patients despite prophylaxis.
| Complication | Incidence | Time Frame | Mortality Impact | Prevention Strategy |
|---|---|---|---|---|
| ARDS | 15-20% | 24-72 hours | 40% mortality | Lung-protective ventilation |
| VAP | 1-3% per day | >48 hours | 20% increase | Early extubation |
| Pulmonary Embolism | 2-5% | 3-7 days | 30% mortality | DVT prophylaxis |
| Acute Kidney Injury | 20-25% | 24-48 hours | 50% increase | Fluid optimization |
| Delirium | 40-60% | 24-72 hours | 10% increase | Sleep hygiene |
- Pain Management Optimization
- Multimodal analgesia: Reduces opioid requirements by 30-50%
- Acetaminophen 1g q6h for baseline analgesia
- NSAIDs if renal function normal and no bleeding risk
- Regional techniques: Epidural for thoracic/abdominal trauma
- Continuous peripheral nerve blocks for extremity injuries
- Paravertebral blocks for rib fractures
- Patient-controlled analgesia: Morphine 1-2 mg bolus doses
- Fentanyl preferred in renal dysfunction
- Hydromorphone for morphine allergies
- Multimodal analgesia: Reduces opioid requirements by 30-50%
💡 Master This: Abdominal compartment syndrome develops when intra-abdominal pressure >20 mmHg with organ dysfunction. Bladder pressure monitoring provides accurate measurement, with decompressive laparotomy indicated for sustained pressures >25 mmHg or renal dysfunction.
Neurological monitoring remains crucial even in non-head trauma patients. Delirium occurs in 40-60% of trauma ICU patients, increasing mortality by 10% and ICU stay by 2-4 days. CAM-ICU screening twice daily identifies delirium early, enabling non-pharmacological interventions and medication optimization.
Nutritional support becomes critical within 24-48 hours of injury. Enteral nutrition reduces infectious complications by 30% compared to parenteral nutrition. Protein requirements increase to 1.5-2.0 g/kg/day in trauma patients, while caloric needs rise 20-30% above baseline due to hypermetabolic stress response.
Coagulation management continues postoperatively with daily monitoring of INR, PTT, and platelet count. Thromboprophylaxis with enoxaparin 30 mg BID or heparin 5000 units TID begins within 24 hours unless active bleeding or high bleeding risk contraindications exist.
Understanding postoperative management principles leads us to the final integration of advanced trauma anesthesia concepts.
🏥 Postoperative Vigilance: The Recovery Command Post
🧠 Advanced Integration: The Trauma Anesthesia Nexus
📌 Remember: NEXUS integration - Neurological protection, Endocrine stress response, Xenobiotic metabolism changes, Urogenital dysfunction, Systemic inflammatory response. These interconnected systems require simultaneous optimization rather than sequential management to prevent multi-organ dysfunction syndrome.
Precision medicine in trauma anesthesia incorporates genetic polymorphisms affecting drug metabolism. CYP2D6 variants alter opioid sensitivity by 5-10 fold, while COMT polymorphisms affect catecholamine metabolism and pain sensitivity. Pharmacogenomic testing can guide personalized anesthetic protocols within 2-4 hours using point-of-care platforms.
| Integration Domain | Key Parameters | Monitoring Frequency | Intervention Threshold | Outcome Impact |
|---|---|---|---|---|
| Neuro-Hemodynamic | CPP, ICP, MAP | Continuous | CPP <60 mmHg | 15% mortality reduction |
| Cardio-Pulmonary | ScvO2, CO, EVLW | Every 15 minutes | ScvO2 <70% | 20% complication reduction |
| Metabolic-Endocrine | Glucose, Lactate, Cortisol | Every 2 hours | Glucose >180 mg/dL | 25% infection reduction |
| Coagulation-Perfusion | TEG, Hgb, Base Deficit | Every 30 minutes | BD >-6 mEq/L | 30% bleeding reduction |
| Inflammatory-Immune | WBC, CRP, Procalcitonin | Every 6 hours | PCT >2 ng/mL | 10% sepsis reduction |
- Systems Biology Approach
- Cardiovascular-Respiratory Coupling: Stroke volume variation predicts fluid responsiveness
- SVV >13% indicates preload dependence in mechanically ventilated patients
- Pulse pressure variation correlates with cardiac output changes
- Neuro-Endocrine Integration: Stress hormone modulation affects recovery
- Dexmedetomidine reduces catecholamine surge by 50%
- Regional anesthesia blunts cortisol response by 60%
- Immune-Metabolic Networks: Hyperglycemia impairs neutrophil function
- Tight glucose control (80-110 mg/dL) reduces infection risk by 40%
- Insulin protocols require hourly monitoring in critical patients
- Cardiovascular-Respiratory Coupling: Stroke volume variation predicts fluid responsiveness
💡 Master This: Biomarker-guided therapy using lactate clearance, ScvO2 trends, and base deficit normalization as resuscitation endpoints reduces mortality by 15-25% compared to traditional vital sign-based approaches in severe trauma patients.
Artificial intelligence integration in trauma anesthesia enables predictive analytics for complication prevention. Machine learning algorithms analyzing physiological waveforms can predict hypotensive episodes 5-15 minutes before clinical manifestation, allowing preemptive interventions that maintain tissue perfusion and prevent secondary organ injury.
Telemedicine capabilities extend expert trauma anesthesia consultation to remote facilities. Real-time video consultation with shared monitoring data enables specialist guidance for complex cases, improving outcomes in resource-limited settings by 20-30% while reducing transfer delays and associated morbidity.
Quality improvement metrics in trauma anesthesia focus on process optimization and outcome enhancement. Time-to-intervention benchmarks include airway secured within 10 minutes, hemorrhage control within 60 minutes, and normothermia maintenance throughout perioperative period. Bundle compliance with evidence-based protocols correlates with improved survival rates.
Advanced integration principles culminate in the development of rapid mastery tools for clinical excellence.
🧠 Advanced Integration: The Trauma Anesthesia Nexus
🎯 Clinical Mastery Arsenal: Trauma Anesthesia Command Center
📌 Remember: MASTER protocol - Monitor continuously, Anticipate complications, Systematize interventions, Trend physiological data, Evaluate responses, Reassess and adjust. This 6-step cycle repeats every 5-10 minutes during critical phases of trauma management.
Essential Clinical Thresholds form the foundation of rapid decision-making. Systolic BP <90 mmHg triggers immediate resuscitation, Heart rate >120 bpm suggests ongoing blood loss, Base deficit >-6 mEq/L indicates severe shock, and Lactate >4 mmol/L signals tissue hypoperfusion requiring aggressive intervention.
| Critical Parameter | Normal Range | Mild Derangement | Severe Derangement | Immediate Action |
|---|---|---|---|---|
| Systolic BP | 100-140 mmHg | 90-100 mmHg | <90 mmHg | Fluid/Blood/Pressors |
| Heart Rate | 60-100 bpm | 100-120 bpm | >120 bpm | Bleeding Control |
| Base Deficit | 0 to -2 mEq/L | -3 to -5 mEq/L | >-6 mEq/L | Massive Transfusion |
| Core Temperature | 36-37°C | 35-36°C | <35°C | Active Warming |
| Hemoglobin | 12-16 g/dL | 8-10 g/dL | <8 g/dL | Blood Transfusion |
- Rapid Assessment Framework
- Primary Survey (<2 minutes): ABCDE with immediate life threats
- Airway: Patent vs compromised vs obstructed
- Breathing: Rate, effort, oxygen saturation
- Circulation: Pulse, blood pressure, perfusion
- Disability: Neurological status and spinal protection
- Exposure: Temperature control and injury identification
- Secondary Survey (5-10 minutes): Systematic examination
- Head-to-toe assessment for missed injuries
- Laboratory studies and imaging as indicated
- Monitoring optimization and access establishment
- Primary Survey (<2 minutes): ABCDE with immediate life threats
💡 Master This: Cognitive Load Management - Use standardized checklists, closed-loop communication, and role clarity to reduce decision fatigue and error rates by 40-60% during high-stress trauma scenarios. Simulation training improves team performance and patient outcomes.
Emergency Drug Dosing requires weight-based calculations with immediate availability. Epinephrine 10-100 mcg boluses for cardiac arrest, Norepinephrine 0.1-0.5 mcg/kg/min for distributive shock, Vasopressin 0.01-0.04 units/min for refractory hypotension, and Tranexamic acid 1g IV within 3 hours for hemorrhage control.
Quality Metrics for trauma anesthesia excellence include time-to-airway <10 minutes, time-to-hemorrhage-control <60 minutes, normothermia maintenance >95% of cases, and appropriate transfusion ratios >90% compliance. Morbidity and mortality conferences review every case for continuous improvement and protocol refinement.
This comprehensive trauma anesthesia framework provides the foundation for managing the most challenging cases while maintaining the highest standards of patient care and safety.
🎯 Clinical Mastery Arsenal: Trauma Anesthesia Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























