Direct Laryngoscopy: Basics - Gateway to Glottis
- Definition: Visual examination of the larynx and glottic opening using a rigid laryngoscope.
- Primary Goals:
- Direct visualization for endotracheal intubation.
- Diagnosis of laryngeal pathology.
- Foreign body removal.
- Key Indications:
- Endotracheal intubation (e.g., general anesthesia, respiratory failure).
- Diagnostic evaluation of larynx/pharynx.
- Management of foreign body aspiration.
- Contraindications:
- Absolute: Epiglottitis (risk of complete airway obstruction, unless managed by an expert).
- Relative: Unstable cervical spine injury, severe trismus, significant facial trauma.
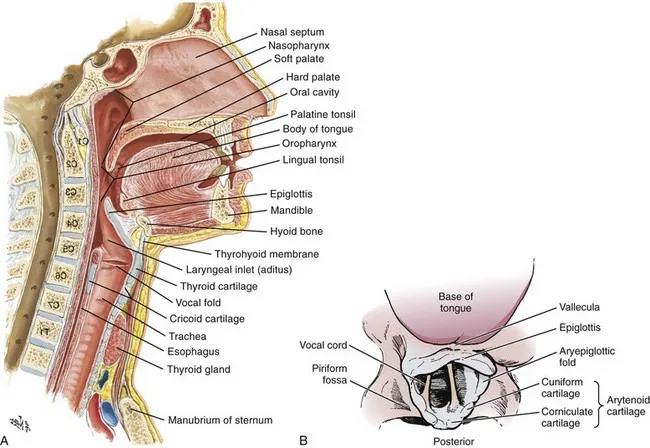
⭐ Direct laryngoscopy provides an unmediated, direct line of sight to the larynx, crucial for intubation.
Laryngoscope Equipment - Choosing Your Weapon
- Handles: Standard/stubby. Check battery.
- Blades:
Feature Macintosh (Mac) Miller Shape Curved Straight Tip Placement Vallecula (indirectly lifts epiglottis) Directly lifts epiglottis Adult Sizes 3-4 2-3 Advantages More tongue space Better view in anterior/floppy epiglottis Common Use Adults Infants, difficult anterior airway 📌 Mnemonic Mac in Vallecula Miller Lifts (epiglottis) 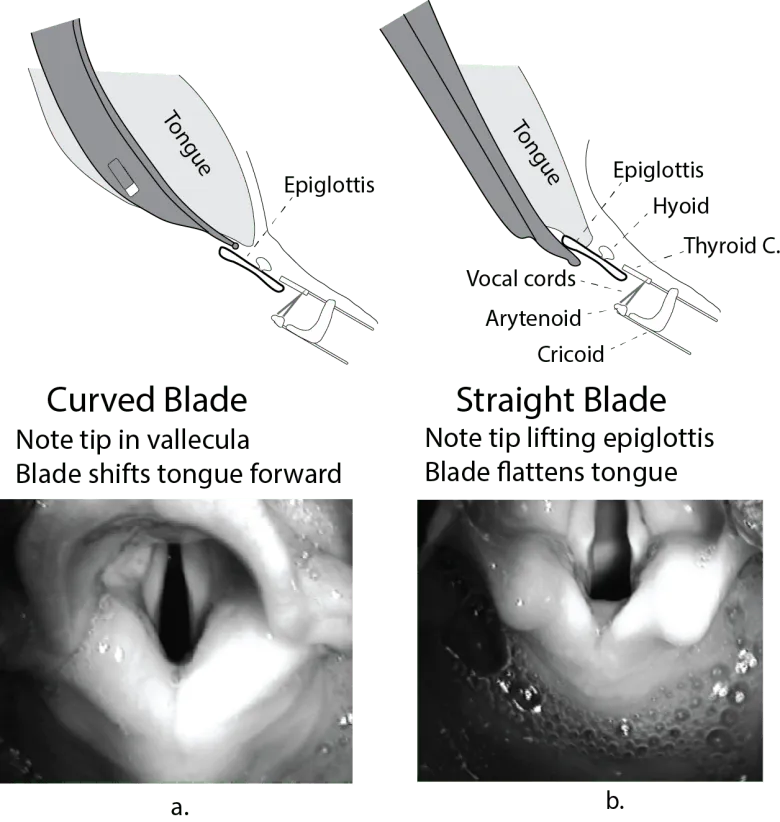
- Adjuncts:
- Stylets: Shape ETT for insertion.
- Magill forceps: Guide ETT, remove foreign bodies.
- Suction: Clear airway, maintain view.
⭐ The Macintosh blade is generally preferred in adults, while the Miller blade is often used in infants and patients with a long, floppy epiglottis or an anterior larynx.
Patient Prep for DL - Setting Up Success
- Airway Assessment (📌 LEMON):
- Look: external (trauma, large incisors, beard).
- Evaluate 3-3-2: IIG >3F, HMD >3F, Thyroid-to-mouth >2F. (F=fingers)
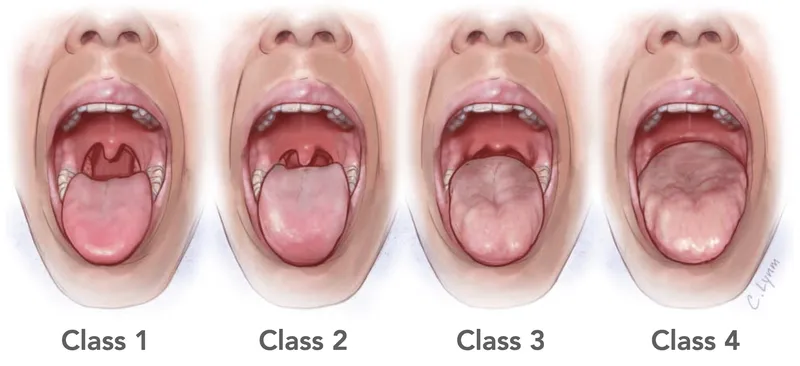
- Mallampati (I-IV).
- Obstruction (tumor, edema) / Obesity.
- Neck mobility (reduced = difficult).
- Difficulty: TMD <6 cm, IIG <3 cm.
- Patient Positioning:
- Sniffing position: head elevated (e.g., on a pad), neck extended.
⭐ The sniffing position aligns the oral, pharyngeal, and laryngeal axes.
- Preoxygenation (Denitrogenation):
- 100% O2 for 3-5 mins OR 4-8 vital capacity breaths.
- Equipment Check:
- Laryngoscope (light), Endotracheal Tube (cuff), Suction ready.
DL Technique & Views - Visualizing Victory
-
Technique Algorithm:
-
Laryngeal View: Cormack-Lehane (Grade I-IV) assesses glottic structures.
⭐ A Cormack-Lehane Grade I view: entire glottis visible, including commissures.
-
View Improvement:
- ELM / BURP: External Laryngeal Manipulation (Backward, Upward, Rightward Pressure on thyroid) (📌 BURP).
-
Sellick's Maneuver (Cricoid Pressure):
- Technique: Firm pressure (30N) on cricoid during RSI.
- Indications: Prevent aspiration.
- Contraindications: Active vomiting, cricotracheal/C-spine injury, foreign body.
DL Complications - Scope Snafus
- Common:
- Dental trauma (teeth, crowns, bridges)
- Lip, tongue, or mucosal injury
- Sore throat, hoarseness
- Serious:
- Hypoxia, hypercarbia (prolonged attempts)
- Esophageal intubation, unrecognized aspiration
- Bronchospasm, laryngospasm (airway reactivity)
- Cardiovascular: Hypertension (↑BP), tachycardia (↑HR), arrhythmias
- Failed intubation, airway trauma
- Difficult/Failed Laryngoscopy Management:
- Immediately call for experienced help
- Utilize alternative airway devices (e.g., LMA, video laryngoscope)
⭐ Dental trauma is the most common complication of direct laryngoscopy.
High‑Yield Points - ⚡ Biggest Takeaways
- Direct Laryngoscopy (DL) is crucial for endotracheal intubation.
- Macintosh blade (curved) fits into the vallecula; Miller blade (straight) directly lifts the epiglottis.
- Optimal patient positioning is the "sniffing position" for axis alignment.
- Cormack-Lehane classification (Grades I-IV) grades the laryngeal view obtained.
- Common complications include dental trauma, sore throat, and laryngospasm.
- BURP maneuver (Backward, Upward, Rightward Pressure) can improve laryngeal view.
- Sellick's maneuver (cricoid pressure) aims to prevent aspiration during RSI (Rapid Sequence Intubation).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


