Respiratory and Airway Management

On this page
🫁 The Respiratory Command Center: Airway Architecture Mastery
Mastering airway management means understanding the elegant architecture from nasal passages to alveoli, recognizing how the larynx guards against aspiration, navigating the unique challenges of pediatric anatomy, and integrating physiology with rapid clinical assessment. You'll build a mental map of the respiratory system's structural hierarchy, learn why children aren't just small adults when securing airways, and develop the pattern recognition that separates competent from exceptional airway practitioners in high-stakes moments.
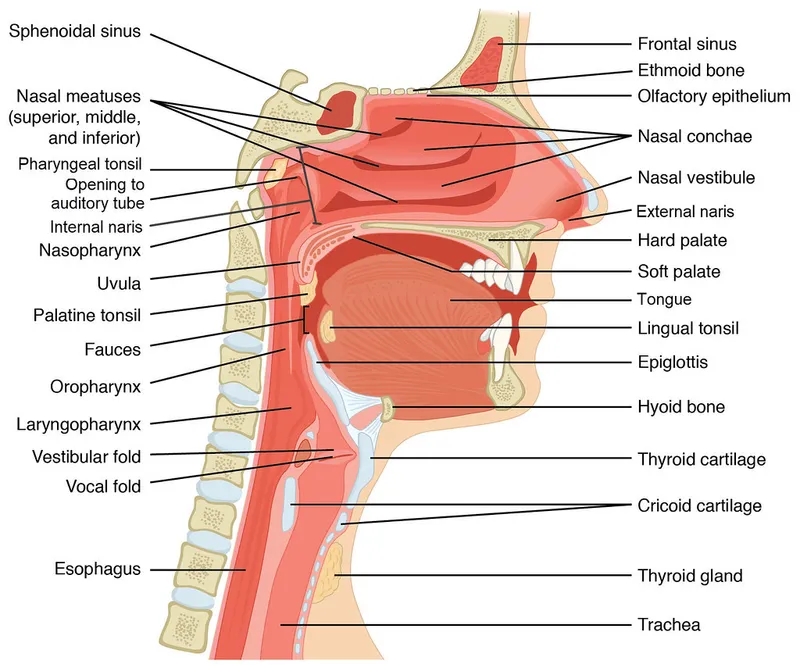
The respiratory system represents one of medicine's most elegant engineering marvels, where form follows function with mathematical precision. Understanding this anatomical blueprint transforms every clinical encounter from guesswork into predictable pattern recognition.
📌 Remember: NOSE - Nares filter, Olfaction detects, Sinuses resonate, Eustachian connects (nasal cavity processes 15,000 liters of air daily with 99% particle filtration efficiency)
Nasal Cavity: The Primary Processing Plant
The nasal cavity functions as a sophisticated air conditioning unit, processing inspired air through three critical mechanisms:
-
Filtration Architecture
- Vibrissae capture particles >10 micrometers (85% efficiency)
- Turbulent flow through conchae increases contact time by 300%
- Mucus blanket traps particles 0.5-10 micrometers (95% efficiency)
- Ciliary escalator moves mucus at 1-2 cm/minute
- Complete clearance cycle: 15-20 minutes
-
Thermal Regulation
- Inspired air reaches 37°C within 0.25 seconds
- Vascular plexus adjusts flow based on ambient temperature
- Heat exchange efficiency: >90% in temperatures down to -40°C
-
Humidification System
- Achieves 100% relative humidity at body temperature
- Daily water loss: 250-350 mL through respiratory tract
- Goblet cell density: 6,000-8,000 cells/mm²
| Structure | Length (mm) | Function | Clinical Significance | Pathology Impact |
|---|---|---|---|---|
| Superior Concha | 15-20 | Olfaction | Anosmia risk | 60% smell loss |
| Middle Concha | 25-35 | Drainage | Sinusitis pathway | 80% blockage rate |
| Inferior Concha | 35-45 | Humidification | Rhinitis target | 90% swelling |
| Nasal Septum | 45-55 | Airflow division | Deviation >15° | 70% obstruction |
| Nasopharynx | 35-40 | Transition zone | Adenoid enlargement | 50% airway compromise |
Pharyngeal Regions: The Airway Crossroads
The pharynx serves as the critical junction where respiratory and digestive pathways intersect, creating both functional advantages and clinical vulnerabilities:
-
Nasopharynx (C1-C2 level)
- Adenoid tissue peaks at age 6-8 years (15-20mm diameter)
- Eustachian tube openings at 45° angle in adults vs 10° in children
- Temperature regulation continues: ±2°C of body temperature
-
Oropharynx (C2-C3 level)
- Mallampati classification predicts intubation difficulty
- Tongue base occupies 40% of oropharyngeal volume
- Palatine tonsils: 15-25mm in healthy adults
-
Hypopharynx (C3-C6 level)
- Pyriform sinuses: 2-3mm wide channels
- Vallecula depth: 8-12mm (critical for laryngoscopy)
- Cricopharyngeus muscle: 2-4mm thick sphincter
💡 Master This: The pharynx transitions from respiratory epithelium (nasopharynx) to stratified squamous epithelium (oropharynx/hypopharynx), reflecting the shift from air conditioning to protection against mechanical trauma. This transition zone at the soft palate represents the boundary between upper and lower respiratory tract infections.
Understanding nasal and pharyngeal anatomy provides the foundation for recognizing airway obstruction patterns. Connect this anatomical knowledge through laryngeal structure mastery to understand complete upper airway dynamics.
🫁 The Respiratory Command Center: Airway Architecture Mastery
🎯 Laryngeal Fortress: The Airway's Guardian Gate
📌 Remember: LARYNX - Levels three protect, Arytenoids articulate, Recurrent nerves control, Young anatomy differs, Nerve injury paralyzes, X-ray shows position (larynx descends 1 vertebral level per decade after age 30)
Laryngeal Cartilage Framework: Structural Engineering
The laryngeal skeleton provides rigid support while allowing dynamic movement through precisely engineered joints:
-
Thyroid Cartilage (Largest)
- Dimensions: 18mm height, 12mm anteroposterior depth
- Angle: 90° in males, 120° in females (creates voice pitch difference)
- Ossification begins: 25-30 years (affects emergency airway access)
- Superior horns: 15-20mm length
- Inferior horns: 8-12mm length, articulate with cricoid
-
Cricoid Cartilage (Only Complete Ring)
- Signet ring shape: 5-7mm anterior, 20-25mm posterior
- C6 vertebral level (critical landmark for cricothyroidotomy)
- Complete ossification: 65-70 years
- Narrowest part of adult airway: 15-20mm diameter
- Pediatric narrowest point: 4-6mm at cricoid level
-
Arytenoid Cartilages (Mobile Vocal Cord Controllers)
- Pyramid shape: 15mm height, 8mm base
- Vocal process: 5-7mm projection (vocal cord attachment)
- Muscular process: 6-8mm projection (muscle attachment)
| Cartilage | Dimensions | Ossification Age | Clinical Significance | Injury Impact |
|---|---|---|---|---|
| Thyroid | 18×12mm | 25-30 years | Palpable landmark | Voice change 80% |
| Cricoid | 5-7mm anterior | 65-70 years | Cricothyrotomy site | Airway stenosis 60% |
| Arytenoid | 15×8mm | 30-35 years | Vocal cord mobility | Paralysis 90% |
| Epiglottis | 35×25mm | Never fully | Aspiration protection | Swallow dysfunction 70% |
| Corniculate | 3-5mm | 40-45 years | Arytenoid support | Minimal impact <5% |
The larynx operates through three functionally distinct levels, each with specific anatomical features and clinical implications:
-
Supraglottis (Above Vocal Cords)
- Epiglottis: 35×25mm leaf-shaped cartilage
- False vocal cords: 8-10mm wide protective folds
- Ventricles: 10-15mm deep recesses (mucus production)
- Rich lymphatic drainage (high infection spread risk)
- Loose areolar tissue allows rapid swelling
-
Glottis (Vocal Cord Level)
- True vocal cords: 15-20mm length in adults
- Glottic opening: 23mm anteroposterior, 13mm transverse
- Posterior glottis: 8mm wide (arytenoid cartilage area)
- Vocal cord tension: 0.5-2.0 kg force range
- Vibration frequency: 85-255 Hz (fundamental frequency)
-
Subglottis (Below Vocal Cords to Cricoid)
- Length: 20-25mm in adults
- Diameter: 15-20mm (narrowest adult airway point)
- Mucosa: 2-3mm thick (prone to edema)
- 1mm edema reduces diameter by 44% in infants
- 3mm edema reduces diameter by 75% in adults
⭐ Clinical Pearl: The posterior glottis (arytenoid area) represents only 20% of the glottic opening but accounts for 50% of vocal cord mobility disorders. Recurrent laryngeal nerve injury affects the posterior cricoarytenoid muscle, the only vocal cord abductor, leading to bilateral cord paralysis and airway obstruction.
💡 Master This: Laryngeal level anatomy determines intubation strategy. Supraglottic devices sit above the cords, glottic visualization requires direct or video laryngoscopy, and subglottic stenosis necessitates smaller endotracheal tubes. The cricothyroid membrane (between thyroid and cricoid cartilages) provides emergency surgical airway access when upper levels are compromised.
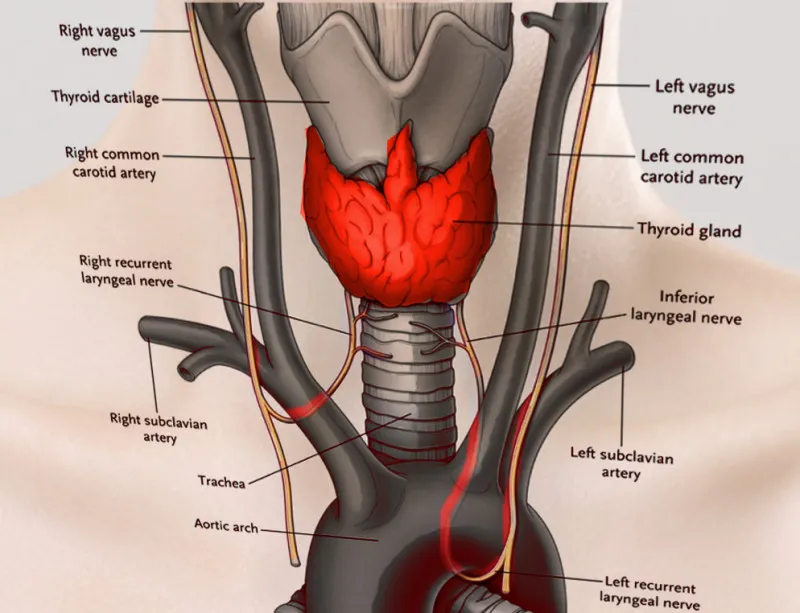
Understanding laryngeal architecture reveals why airway management requires precise anatomical knowledge. Connect this structural foundation through pediatric airway differences to understand age-specific management strategies.
🎯 Laryngeal Fortress: The Airway's Guardian Gate
🧒 Pediatric Airway Universe: Small Spaces, Big Challenges
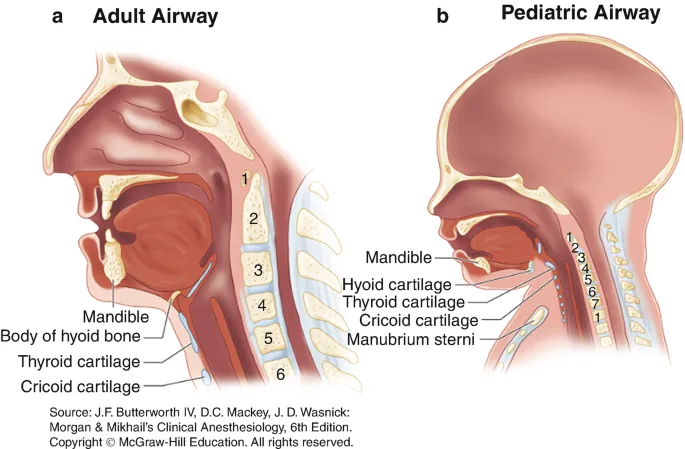
Pediatric airways represent scaled-down versions of adult anatomy with critical proportional differences that fundamentally alter clinical management strategies.
📌 Remember: KIDS - Keep head neutral, Infants have large occiput, Diameter matters most, Subglottic narrowest (pediatric airway resistance follows Poiseuille's law: resistance ∝ 1/radius⁴, making small changes catastrophic)
Anatomical Proportional Differences
Pediatric airway anatomy differs from adults in predictable patterns that create both advantages and vulnerabilities:
-
Head and Neck Proportions
- Occiput: 25% larger relative to body (vs 15% in adults)
- Neck length: 40% shorter proportionally
- Tongue: 50% larger relative to oral cavity
- Creates natural sniffing position in infants
- Requires shoulder roll for optimal positioning
- Tongue displacement more difficult during laryngoscopy
-
Laryngeal Position and Size
- Larynx position: C3-C4 (vs C5-C6 in adults)
- Epiglottis: 45° angle (vs 30° in adults)
- Vocal cord length: 6-8mm (vs 15-20mm in adults)
- Higher, more anterior position
- Omega-shaped epiglottis (stiffer, less flexible)
- Requires straight blade for visualization
-
Airway Dimensions by Age
- Newborn tracheal diameter: 4-5mm
- 1-year-old: 5-6mm
- 5-year-old: 7-8mm
- Adult size reached: 12-14 years
- Subglottic area: 1/3 adult size at birth
- Cricoid ring: narrowest point until age 8-10
| Age Group | Tracheal Diameter | ETT Size | Cricoid Diameter | Resistance Factor |
|---|---|---|---|---|
| Newborn | 4-5mm | 3.0-3.5mm | 4.5mm | 16× adult |
| 6 months | 5-6mm | 3.5-4.0mm | 5.5mm | 8× adult |
| 1 year | 6-7mm | 4.0-4.5mm | 6.5mm | 4× adult |
| 5 years | 7-8mm | 5.0-5.5mm | 7.5mm | 2× adult |
| 10 years | 9-10mm | 6.0-6.5mm | 9.5mm | 1.5× adult |
The mathematical relationship between airway diameter and resistance creates exponential clinical consequences in pediatric patients:
-
Resistance Calculations (Poiseuille's Law)
- Adult trachea (20mm): Baseline resistance = 1 unit
- Infant trachea (4mm): Resistance = 625 units (25× diameter difference⁴)
- 1mm edema in infant: 4mm → 2mm = 16× resistance increase
- 2mm edema: Complete obstruction risk
- 0.5mm edema: 44% area reduction
-
Work of Breathing Impact
- Infant baseline: 3× adult work/kg
- With 1mm edema: 48× adult work/kg
- Respiratory failure threshold: 10× baseline work
- Fatigue onset: 15-30 minutes vs 2-4 hours in adults
- Reserve capacity: 25% vs 75% in adults
⭐ Clinical Pearl: The cricoid ring serves as the functional narrowest point in children under 8-10 years, unlike adults where the vocal cords are narrowest. This explains why uncuffed tubes were traditionally used in young children and why cuffed tubes must be 0.5mm smaller to prevent subglottic trauma.
Age-Specific Equipment Selection
Pediatric airway management requires precise equipment sizing based on anatomical development patterns:
-
Endotracheal Tube Sizing
- Uncuffed formula: (Age + 4) ÷ 4 = ETT size
- Cuffed formula: (Age + 3.5) ÷ 4 = ETT size
- Depth formula: ETT size × 3 = depth at lip
- Always prepare ±0.5mm sizes
- Cuff pressure: <20 cmH₂O (vs <25 cmH₂O adults)
-
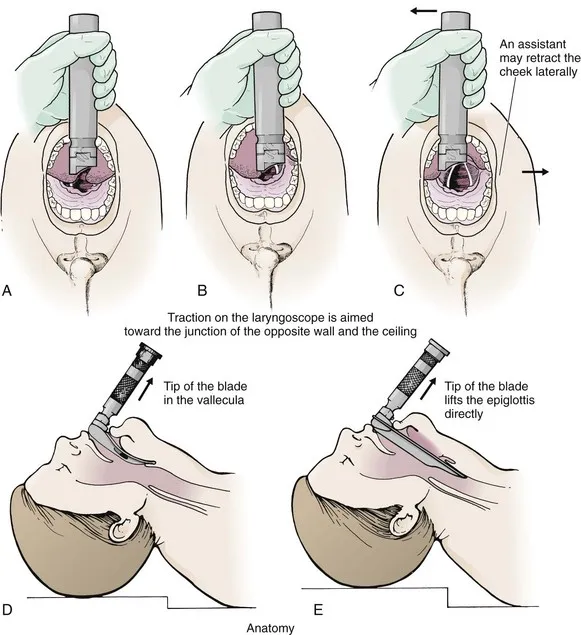
Laryngoscope Blade Selection
- Straight blades: Preferred until age 3-4 years
- Miller 0: Premature infants
- Miller 1: Term infants to 2 years
- Miller 2: 2-6 years
- Curved blades: Mac 2 for >4 years
- Handle length: Short handle for infants
-
Mask Ventilation Considerations
- Dead space: 2-3 mL/kg (vs 1 mL/kg adults)
- Seal pressure: 15-20 cmH₂O maximum
- Tidal volume: 6-8 mL/kg (same as adults)
- Rate: 20-30/min infants, 15-20/min children
- Avoid excessive pressure: barotrauma risk 5× higher
💡 Master This: Pediatric airway management follows the "small margins, big consequences" principle. A 1mm error in tube size selection can mean the difference between successful ventilation and complete obstruction. The age-based formulas provide starting points, but clinical assessment of individual anatomy remains paramount for safe management.
Pediatric airway anatomy demonstrates how proportional changes create exponential clinical challenges. Connect these size-dependent principles through tracheal and bronchial architecture to understand complete respiratory tree management.
🧒 Pediatric Airway Universe: Small Spaces, Big Challenges
🌳 Tracheobronchial Tree: The Respiratory Highway System
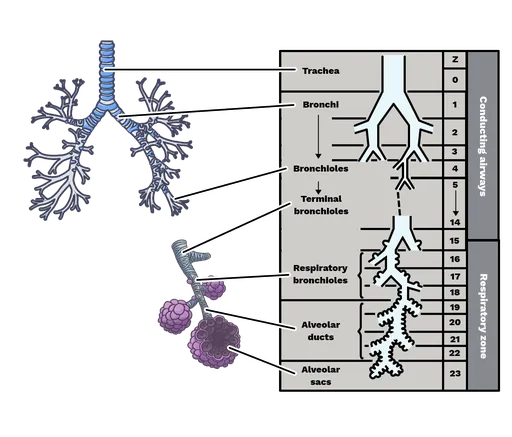
The tracheobronchial tree represents a masterpiece of fluid dynamics engineering, where each generation of branching follows mathematical principles to optimize airflow distribution and gas exchange efficiency.
📌 Remember: TREE - Trachea has C-rings, Right bronchus straighter, Each generation doubles, Exchange starts generation 17 (trachea divides into 2¹ main bronchi, then 2² lobar bronchi, continuing to 2²³ alveolar sacs)
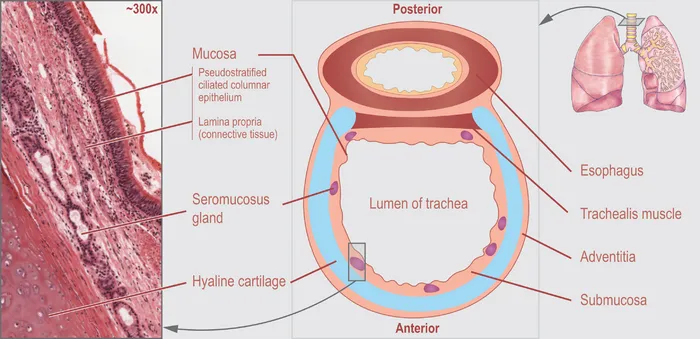
Tracheal Architecture and Characteristics
The trachea serves as the central conduit, engineered for structural stability while maintaining flexibility:
-
Structural Specifications
- Length: 10-12 cm adults (4-5 cm children)
- Diameter: 15-20 mm adults (4-5 mm newborns)
- C-shaped cartilage rings: 16-20 rings total
- Ring height: 4-5 mm each
- Posterior membrane: 6-8 mm wide (trachealis muscle)
- Cartilage coverage: 270° of circumference
-
Anatomical Relations
- Begins: C6 vertebral level (cricoid cartilage)
- Ends: T5 vertebral level (carina)
- Carina angle: 60-70° (widens with age)
- Right main bronchus: 25° from vertical
- Left main bronchus: 45° from vertical
- Aspiration preferentially affects right lung (75% of cases)
-
Vascular Supply and Innervation
- Arterial supply: Inferior thyroid, bronchial arteries
- Venous drainage: Thyroid venous plexus
- Innervation: Recurrent laryngeal, sympathetic chains
- Sensory innervation: Vagus nerve branches
- Cough reflex threshold: 1-2 μg/mL capsaicin
| Structure | Dimensions | Function | Clinical Significance | Pathology Impact |
|---|---|---|---|---|
| Tracheal rings | 4-5mm height | Structural support | Stenosis risk 15% | Airway collapse |
| Posterior membrane | 6-8mm width | Flexibility | Compression site | External pressure |
| Carina | 60-70° angle | Flow division | Aspiration pattern | Right lung 75% |
| Right bronchus | 25° angle | Ventilation path | Foreign body route | Obstruction 80% |
| Left bronchus | 45° angle | Ventilation path | Compression risk | Cardiac enlargement |
The respiratory tree follows precise mathematical branching patterns that optimize both airflow and gas exchange:
-
Generation Classification
- Generations 0-16: Conducting zone (anatomical dead space)
- Generations 17-19: Transitional zone (respiratory bronchioles)
- Generations 20-23: Respiratory zone (alveolar region)
- Total surface area: 70 m² (tennis court size)
- Alveolar number: 300-500 million
- Gas exchange area: 50-100 m² (functional)
-
Airflow Characteristics by Generation
- Trachea (Generation 0): Reynolds number >4000 (turbulent)
- Main bronchi (Generations 1-2): Reynolds 2000-4000 (transitional)
- Segmental bronchi (Generations 3-5): Reynolds <2000 (laminar)
- Velocity decreases: 150 cm/s → 0.5 cm/s
- Cross-sectional area increases: 2.5 cm² → 10,000 cm²
- Resistance distribution: 80% in first 8 generations
Bronchial Asymmetry and Clinical Implications
The right and left bronchial trees exhibit systematic differences that create predictable clinical patterns:
-
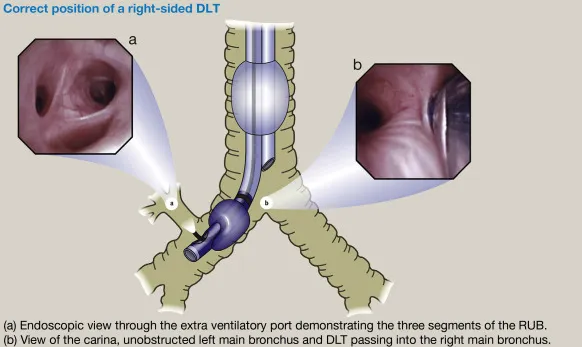
Right Main Bronchus Characteristics
- Shorter: 2.5 cm vs 5 cm left
- Wider: 15 mm vs 11 mm left
- Straighter: 25° vs 45° from vertical
- Foreign body aspiration: 85% right-sided
- Endotracheal tube malposition: 90% right main bronchus
- Right upper lobe collapse: Common with right main intubation
-
Left Main Bronchus Characteristics
- Longer course: 5 cm before first branch
- Narrower diameter: 11 mm average
- Greater angulation: 45° from tracheal axis
- Compression risk: Enlarged left atrium, aortic arch
- Ventilation challenges: Higher resistance, longer path
- Selective intubation: More difficult, requires 45° turn
-
Lobar and Segmental Patterns
- Right lung: 3 lobes, 10 segments
- Left lung: 2 lobes, 8-10 segments (variable)
- Segment identification: Critical for targeted procedures
- Bronchoscopy navigation: Requires anatomical precision
- Selective blockade: Segment-specific anesthesia
- Pathology localization: CT-bronchoscopy correlation
⭐ Clinical Pearl: The right main bronchus angle of 25° makes it the preferential path for aspirated material and malpositioned endotracheal tubes. During intubation, advancing the tube >23 cm at the teeth in adults risks right main bronchus intubation with subsequent left lung collapse.
💡 Master This: Tracheobronchial anatomy follows Weibel's model of dichotomous branching, where each generation approximately doubles the number of airways while halving individual airway diameter. This creates exponential increases in total cross-sectional area, explaining why peripheral resistance is minimal despite millions of small airways.
Understanding tracheobronchial architecture reveals the engineering principles behind respiratory efficiency. Connect this anatomical foundation through respiratory physiology to understand how structure enables optimal gas exchange function.
🌳 Tracheobronchial Tree: The Respiratory Highway System
⚡ Respiratory Physiology Engine: Gas Exchange Mastery
Respiratory physiology represents the ultimate optimization of gas transport, where mechanical ventilation, diffusion gradients, and circulatory integration create seamless oxygen delivery and carbon dioxide removal.
📌 Remember: BREATH - Boyle's law drives flow, Resistance opposes movement, Elastance stores energy, Alveoli exchange gases, Time constants determine filling, Hemoglobin carries oxygen (respiratory mechanics follow P = V/C + R×Flow, where compliance and resistance determine ventilation patterns)
Ventilation Mechanics: The Bellows System
Respiratory mechanics operate through coordinated pressure changes that drive bidirectional airflow with mathematical precision:
-
Pressure Relationships
- Atmospheric pressure: 760 mmHg (sea level baseline)
- Pleural pressure: -5 mmHg (inspiration) to -8 mmHg (expiration)
- Alveolar pressure: 0 mmHg (end-inspiration/expiration)
- Transpulmonary pressure: 5-8 mmHg (maintains lung inflation)
- Pressure gradient: 1-2 mmHg drives 500 mL tidal volume
- Maximum inspiratory pressure: -120 mmHg (healthy adults)
-
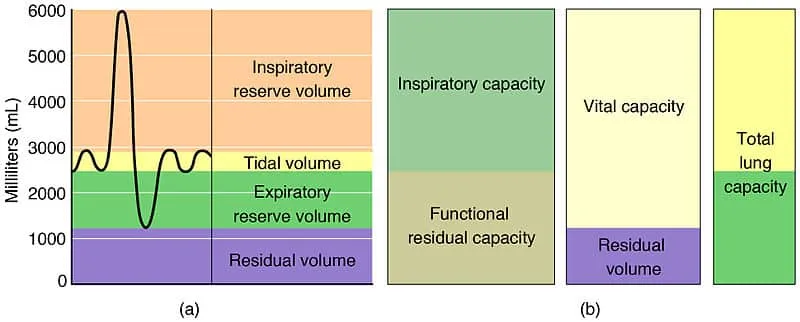
Lung Volumes and Capacities
- Tidal Volume (TV): 500 mL (6-8 mL/kg)
- Inspiratory Reserve Volume (IRV): 3,000 mL
- Expiratory Reserve Volume (ERV): 1,100 mL
- Residual Volume (RV): 1,200 mL (never exhaled)
- Functional Residual Capacity (FRC): 2,300 mL (ERV + RV)
- Total Lung Capacity (TLC): 5,800 mL (all volumes combined)
-
Compliance and Elastance
- Static compliance: 200 mL/cmH₂O (normal lungs)
- Dynamic compliance: 150-180 mL/cmH₂O (frequency-dependent)
- Chest wall compliance: 200 mL/cmH₂O
- Total respiratory compliance: 100 mL/cmH₂O (combined system)
- Elastance: 10 cmH₂O/L (reciprocal of compliance)
- Surface tension: 50 dynes/cm (without surfactant)
| Parameter | Normal Value | Clinical Range | Significance | Disease Impact |
|---|---|---|---|---|
| Tidal Volume | 500 mL | 400-600 mL | Minute ventilation | ARDS: ↓50% |
| FRC | 2,300 mL | 2,000-2,600 mL | Oxygen reserve | Obesity: ↓30% |
| Compliance | 200 mL/cmH₂O | 150-250 mL/cmH₂O | Work of breathing | Fibrosis: ↓70% |
| Resistance | 2 cmH₂O/L/s | 1-3 cmH₂O/L/s | Airflow limitation | Asthma: ↑500% |
| Dead Space | 150 mL | 120-180 mL | Ventilation efficiency | COPD: ↑200% |
Alveolar gas exchange operates through Fick's law of diffusion, optimized by enormous surface area and minimal barrier thickness:
-
Diffusion Barrier Architecture
- Alveolar-capillary membrane: 0.5 micrometers thick
- Surface area: 70 m² (tennis court equivalent)
- Capillary volume: 75 mL (sheet of blood)
- Transit time: 0.75 seconds (rest) to 0.25 seconds (exercise)
- Diffusion completion: 0.25 seconds for O₂, 0.1 seconds for CO₂
- Safety margin: 3× reserve for oxygen transfer
-
Gas Partial Pressures (Sea Level)
- Inspired air: O₂ 159 mmHg, CO₂ 0.3 mmHg
- Alveolar air: O₂ 104 mmHg, CO₂ 40 mmHg
- Arterial blood: O₂ 95 mmHg, CO₂ 40 mmHg
- Venous blood: O₂ 40 mmHg, CO₂ 46 mmHg
- A-a gradient: 5-15 mmHg (normal), >20 mmHg (abnormal)
- Oxygen extraction: 25% at rest, 75% maximum exercise
Ventilation-Perfusion Relationships
Optimal gas exchange requires precise matching of ventilation (V̇) and perfusion (Q̇) throughout the lung:
-
V̇/Q̇ Ratio Distribution
- Normal V̇/Q̇: 0.8-1.0 (ideal matching)
- Apex V̇/Q̇: 3.0 (high ventilation, low perfusion)
- Base V̇/Q̇: 0.6 (high perfusion, low ventilation)
- Dead space: V̇/Q̇ >1.0 (ventilation without perfusion)
- Shunt: V̇/Q̇ <0.1 (perfusion without ventilation)
- Silent unit: V̇/Q̇ = 0 (neither ventilation nor perfusion)
-
Regional Distribution Factors
- Gravity effects: 0.25 cmH₂O/cm height pressure gradient
- Zone 1 (apex): PA > Pa > Pv (minimal perfusion)
- Zone 2 (middle): Pa > PA > Pv (pulsatile flow)
- Zone 3 (base): Pa > Pv > PA (continuous flow)
- Perfusion increases: 10-fold from apex to base
- Ventilation increases: 2-fold from apex to base
- Gas exchange efficiency: Highest in Zone 3
-
Compensatory Mechanisms
- Hypoxic pulmonary vasoconstriction: Diverts blood from poorly ventilated areas
- Bronchodilation: CO₂ >45 mmHg triggers airway dilation
- Collateral ventilation: Pores of Kohn provide alternative pathways
- Response time: 30-60 seconds for vascular changes
- Effectiveness: 80% compensation for mild V̇/Q̇ mismatch
- Failure threshold: V̇/Q̇ mismatch >50% of lung
⭐ Clinical Pearl: The A-a oxygen gradient increases 2.5 mmHg per decade after age 40, reflecting age-related V̇/Q̇ mismatch. A gradient >20 mmHg in young adults or >30 mmHg in elderly patients suggests significant pulmonary pathology requiring investigation.
💡 Master This: Respiratory physiology follows optimization principles where structure matches function. The enormous surface area (70 m²), minimal diffusion distance (0.5 μm), and precise V̇/Q̇ matching create a system with 300% reserve capacity that maintains 98% oxygen saturation even during moderate exercise or mild disease.
Understanding respiratory physiology reveals how anatomical design enables optimal gas exchange. Connect these physiological principles through clinical airway assessment to understand practical patient evaluation strategies.
⚡ Respiratory Physiology Engine: Gas Exchange Mastery
🎯 Clinical Airway Arsenal: Rapid Assessment Mastery
📌 Remember: ASSESS - Anatomy predicts difficulty, Scoring systems quantify risk, Space measurements matter, Emergency plans essential, Safety margins critical, Success depends on preparation (difficult airway incidence: 1-18% depending on population and definition criteria)
Systematic Airway Evaluation Framework
Clinical airway assessment follows a structured approach that combines anatomical measurements with functional testing:
-
Primary Assessment Parameters
- Mallampati Classification: Class I-IV visibility scale
- Thyromental Distance: >6.5 cm (normal), <6 cm (difficult)
- Mouth Opening: >3 cm (normal), <2.5 cm (restricted)
- Neck Extension: >35° (adequate), <15° (limited)
- Mandibular Protrusion: Upper teeth behind lower (adequate)
- Dentition Assessment: Loose teeth, caps, bridges
-
Advanced Predictive Measurements
- Sternomental Distance: >12.5 cm (normal)
- Neck Circumference: >43 cm (increased difficulty)
- Wilson Score: 0-10 scale (>2 predicts difficulty)
- STOP-BANG Score: Sleep apnea screening (>3 high risk)
- El-Ganzouri Score: Multifactorial assessment (>4 difficult)
- Simplified Airway Risk Index: 7-factor model
| Assessment Tool | Normal Range | Difficult Threshold | Sensitivity | Specificity | Clinical Utility |
|---|---|---|---|---|---|
| Mallampati | Class I-II | Class III-IV | 65% | 70% | First-line screening |
| Thyromental Distance | >6.5 cm | <6 cm | 80% | 85% | High predictive value |
| Mouth Opening | >3 cm | <2.5 cm | 75% | 80% | Equipment selection |
| Neck Extension | >35° | <15° | 70% | 75% | Positioning strategy |
| Wilson Score | 0-2 | >2 | 85% | 90% | Comprehensive assessment |
Beyond static measurements, functional testing reveals dynamic airway characteristics that influence management success:
-
Respiratory Function Evaluation
- Vital Capacity: >15 mL/kg (adequate reserve)
- Maximum Inspiratory Pressure: >-25 cmH₂O
- Oxygen Saturation: >95% on room air
- Desaturation rate: 1-2%/minute (normal), >5%/minute (rapid)
- Apnea tolerance: 8-10 minutes (healthy), 2-3 minutes (compromised)
- Preoxygenation effectiveness: >87% end-tidal oxygen
-
Cardiovascular Stability Markers
- Blood Pressure: Systolic >90 mmHg, MAP >65 mmHg
- Heart Rate: 60-100 bpm (stable), >120 bpm (stress response)
- Perfusion Indicators: Capillary refill <2 seconds
- Shock Index: HR/SBP <0.9 (normal), >1.0 (concerning)
- Lactate Level: <2 mmol/L (normal), >4 mmol/L (severe)
- Base Deficit: ±2 mEq/L (normal), >6 mEq/L (significant)
Risk Stratification and Decision Algorithms
Systematic risk stratification enables evidence-based technique selection and resource allocation:
-
Low-Risk Profile (<5% difficult intubation probability)
- Mallampati I-II + Normal measurements + No comorbidities
- Standard approach: Direct laryngoscopy, MAC 3-4 blade
- Backup plan: Video laryngoscopy readily available
- Success rate: >95% first attempt
- Complication rate: <2% significant events
- Time to intubation: 30-60 seconds average
-
Moderate-Risk Profile (5-15% difficult intubation probability)
- Mallampati III or 1-2 abnormal measurements
- Enhanced approach: Video laryngoscopy first-line
- Backup plan: Supraglottic airway + Fiberoptic capability
- Success rate: 85-90% first attempt
- Complication rate: 5-8% significant events
- Time to intubation: 60-120 seconds average
-
High-Risk Profile (>15% difficult intubation probability)
- Mallampati IV + Multiple abnormal measurements + Comorbidities
- Advanced approach: Awake intubation or Surgical airway
- Backup plan: Immediate surgical capability
- Success rate: 60-75% standard techniques
- Complication rate: 15-25% significant events
- Time to secure airway: 3-10 minutes average
⭐ Clinical Pearl: The combination of Mallampati Class IV + thyromental distance <6 cm + mouth opening <2.5 cm creates a 85% probability of difficult intubation, warranting awake fiberoptic intubation or surgical airway preparation before induction.
💡 Master This: Clinical airway assessment transforms from subjective impression to objective risk stratification through systematic measurement and scoring. The goal is not to predict every difficult airway, but to identify high-risk patients who require advanced planning and alternative techniques to prevent cannot intubate, cannot ventilate scenarios.
Understanding clinical airway assessment provides the foundation for safe airway management. This systematic approach to patient evaluation ensures appropriate technique selection and resource preparation for optimal outcomes across all clinical scenarios.
🎯 Clinical Airway Arsenal: Rapid Assessment Mastery
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























