Spinal Basics & Anatomy - Backbone Block Blueprint
- Definition: Local anesthetic (LA) injection into subarachnoid space (intrathecal).
- Mechanism: Blocks nerve roots in CSF → sensory, motor, sympathetic blockade.
- Pros: Rapid onset, dense block. Cons: Hypotension, Post-Dural Puncture Headache (PDPH).
- Key Layers Pierced (Midline Approach):
- Skin
- Subcutaneous tissue
- Supraspinous ligament
- Interspinous ligament
- Ligamentum flavum
- Dura mater
- Arachnoid mater 📌 Mnemonic: Skinny Sailors Seek Islands Like Distant Atolls.
- Target Space: Subarachnoid space (contains Cerebrospinal Fluid - CSF: clear, colorless).
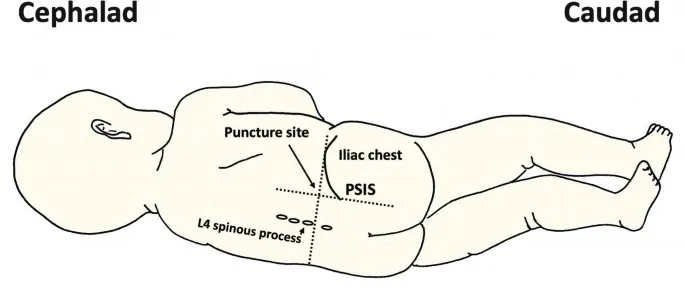
- Vertebral Level (Adults): L3-L4 or L4-L5 interspace. (Spinal cord typically ends L1-L2).
⭐ Tuffier's line, connecting the highest points of iliac crests, typically crosses the L4 vertebral body or L4-L5 interspace.
 oka
oka
Spinal Pharmacology - Potions & Properties
- Local Anesthetics (LAs): Primarily amides.
- Bupivacaine (0.5% Heavy): 7.5-15 mg (1.5-3 mL). Long duration.
- Lidocaine (5% Heavy): 50-100 mg. Fast onset. ⚠️ Risk of Transient Neurological Symptoms (TNS).
- Ropivacaine: Similar to bupivacaine, less cardiotoxic.
- Key LA Properties:
- Baricity: Governs CSF spread.
- Hyperbaric (LA + Dextrose): Sinks. Most common.
- Isobaric (LA in Saline): Limited spread by injection volume.
- Hypobaric (LA in Distilled Water): Floats.
- $pK_a$: Affects onset (lower $pK_a$ closer to physiological pH = faster onset).
- Lipid Solubility: ↑ solubility = ↑ potency & ↑ duration.
- Baricity: Governs CSF spread.
- Adjuvants: Enhance block quality & duration.
- Opioids: Fentanyl (10-25 mcg), Morphine PF (100-200 mcg). Enhance analgesia.
- Clonidine: (15-75 mcg). Prolongs block, provides sedation.
⭐ Bupivacaine is the most commonly used spinal anesthetic due to its long duration of action and dense sensory block, making it suitable for a wide range of surgical procedures.
Spinal Technique & Block Management - Perfecting the Poke
-
Prep: IV access, monitors (ECG, NIBP, SpO2), consent.
-
Positioning: Sitting or lateral decubitus (L3-L4, L4-L5).
-
Needles: Quincke (cutting), Whitacre/Sprotte (pencil-point, ↓PDPH). Sizes: 22-27G.

-
Procedure:
-
Factors Affecting Block Height:
- Major: Baricity (hyperbaric > isobaric > hypobaric), patient position post-injection, LA dose/volume, injection site.
- Minor: CSF volume, needle bevel direction, speed of injection, age, pregnancy.
- 📌 Mnemonic: Baricity, Position, Dose, Site (BPDS - "Block Placement Determines Spread")
-
Physiological Effects:
- CVS: Sympathetic block (T1-T4) → ↓BP, ↓HR. Treat hypotension with fluids, vasopressors (phenylephrine, ephedrine).
- Resp: Usually minimal. High block (>T4) → intercostal paralysis. Apnea if brainstem hypoperfusion.
⭐ PDPH risk is significantly reduced by using smaller gauge, pencil-point needles (e.g., Whitacre 25-27G) and orienting the bevel of cutting needles parallel to dural fibers.
Spinal Complications & Troubleshooting - Navigating Pitfalls
- Immediate:
- Hypotension (most common): IV fluids, vasopressors (phenylephrine 50-100 mcg; ephedrine 5-10 mg).
- Bradycardia: Atropine 0.4-0.6 mg IV.
- High/Total Spinal: Airway support, O₂, cardiovascular support.
- Nausea/Vomiting.
- Early (days):
- PDPH: Postural headache. Conservative (fluids, analgesics, caffeine). Epidural Blood Patch (EBP) if severe. 📌 PDPH: Posture Dependent Painful Headache.
- Urinary Retention: Monitor; catheterize if needed.
- Transient Neurological Symptoms (TNS).
- Late (weeks+):
- Neurological Injury: Direct trauma, hematoma, infection (meningitis, abscess).
- Cauda Equina Syndrome (CES): ⚠️ Urgent MRI! Bowel/bladder dysfunction, saddle anesthesia.
- Arachnoiditis.

⭐ Using smaller gauge (e.g., 25-27G) pencil-point needles (Whitacre, Sprotte) significantly ↓ PDPH risk compared to cutting needles (Quincke).
High‑Yield Points - ⚡ Biggest Takeaways
- Spinal anesthesia involves injection into the subarachnoid space, usually at L3-L4 or L4-L5.
- Hypotension is the most frequent complication from sympathetic blockade.
- Post-dural puncture headache (PDPH) risk is reduced by atraumatic (pencil-point) needles.
- Key absolute contraindications: Local infection, raised ICP, severe hypovolemia, coagulopathy.
- Baricity of local anesthetic (e.g., hyperbaric bupivacaine) governs its spread.
- Sequence of nerve fiber blockade: Sympathetic (B) → Sensory (Aδ, C) → Motor (Aα).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

