Preoperative Evaluation and Management

On this page
🎯 Preoperative Command Center: The Clinical Decision Matrix
Before a single incision is made, the preoperative period determines surgical success or catastrophe. You'll master the systematic evaluation that transforms uncertainty into calculated risk, learning how to stratify cardiac danger, optimize pulmonary function, navigate medication pitfalls, and synthesize laboratory data into actionable decisions. This isn't paperwork-it's the clinical architecture that prevents complications, reduces mortality, and ensures your patient reaches the operating room in their safest possible state.
The preoperative evaluation framework encompasses five core domains: cardiovascular risk stratification, pulmonary assessment, metabolic optimization, medication reconciliation, and airway evaluation. Each domain requires specific assessment tools, evidence-based thresholds, and targeted interventions to achieve optimal surgical outcomes.
📌 Remember: PRIME Assessment - Pulmonary function, Risk stratification, Investigations, Medication review, Emergency planning. This systematic approach ensures comprehensive evaluation of all perioperative risk factors with quantifiable outcomes.
-
Cardiovascular Assessment
- Risk stratification using RCRI score (0-6 points)
- Functional capacity evaluation (>4 METs indicates low risk)
- ECG abnormalities present in 15-25% of surgical patients
- ST-T changes requiring cardiology consultation
- Arrhythmias affecting 8-12% of perioperative outcomes
- Conduction blocks increasing risk by 2.5-fold
-
Pulmonary Evaluation
- Spirometry indicated when FEV1 <80% predicted
- Arterial blood gas analysis for SpO2 <92% on room air
- Chest imaging revealing abnormalities in 30-40% of high-risk patients
- Consolidation patterns requiring optimization
- Pleural effusions affecting 5-8% of surgical candidates
-
Laboratory Assessment
- Complete blood count with Hgb >10 g/dL target
- Comprehensive metabolic panel including eGFR >60 mL/min
- Coagulation studies when bleeding risk factors present
- INR target <1.5 for most procedures
- Platelet count >100,000 for major surgery
⭐ Clinical Pearl: Patients with RCRI score ≥3 have >5% risk of major cardiac events, requiring intensive perioperative monitoring and potential cardiology consultation. This threshold guides resource allocation and monitoring intensity.
| Assessment Domain | Low Risk Threshold | Moderate Risk | High Risk | Intervention Required |
|---|---|---|---|---|
| Cardiac (RCRI) | 0-1 points | 2 points | ≥3 points | Cardiology consult |
| Pulmonary (FEV1) | >80% predicted | 60-80% | <60% | Optimization protocol |
| Renal (eGFR) | >60 mL/min | 30-60 | <30 | Nephrology input |
| Functional (METs) | >4 METs | 2-4 METs | <2 METs | Exercise testing |
| Hemoglobin | >12 g/dL | 10-12 g/dL | <10 g/dL | Transfusion protocol |
Understanding preoperative assessment fundamentals establishes the foundation for advanced risk stratification techniques that enable precise surgical timing and optimization strategies.
🎯 Preoperative Command Center: The Clinical Decision Matrix
⚡ Cardiovascular Risk Stratification: The Cardiac Crystal Ball
📌 Remember: RCRI-HIM Components - Renal dysfunction (Cr >2.0), CHF history, Risk surgery, Ischemic heart disease, High-risk surgery, Insulin diabetes, Major vascular surgery. Each component adds 1 point with exponential risk increase: 0-1 points = 0.4-1% risk, 2 points = 2.2% risk, ≥3 points = 5.4% risk.
-
High-Risk Surgical Procedures
- Vascular surgery carrying 5-15% cardiac event rates
- Emergency procedures increasing risk by 2-3 fold
- Prolonged operations >3 hours with fluid shifts >1.5L
- Aortic surgery with 8-12% MI rates
- Carotid endarterectomy with 3-5% stroke risk
- Major orthopedic procedures lasting >4 hours
-
Functional Capacity Assessment
- >4 METs indicates excellent functional reserve
- Stair climbing 2 flights without symptoms = 4-5 METs
- Duke Activity Status Index >46 correlates with low risk
- Walking 4 blocks on level ground = 4 METs
- Heavy housework or yard work = 4-6 METs
- Recreational sports participation = >6 METs
-
Biomarker Integration
- BNP >100 pg/mL or NT-proBNP >300 pg/mL indicates risk
- Troponin elevation in 5-8% of high-risk patients
- hsCRP >3 mg/L associated with 2-fold increased events
- Preoperative troponin predicts 30-day mortality
- BNP levels correlate with CHF exacerbation risk
⭐ Clinical Pearl: The "4-Factor Rule" identifies 99% of high-risk cardiac patients: Age >70 years, diabetes requiring insulin, prior MI/CHF, and creatinine >2.0 mg/dL. Presence of ≥3 factors mandates cardiology consultation regardless of RCRI score.
| RCRI Score | 30-Day Cardiac Risk | Recommended Action | Monitoring Level | Cost-Effectiveness |
|---|---|---|---|---|
| 0 points | 0.4% | Routine care | Standard | High |
| 1 point | 1.0% | Clinical assessment | Standard | High |
| 2 points | 2.2% | Consider testing | Enhanced | Moderate |
| ≥3 points | 5.4% | Cardiology consult | Intensive | High |
| Emergency | 2-3x baseline | Optimize rapidly | Critical | Variable |
Advanced cardiovascular risk stratification enables precise identification of patients requiring intensive monitoring, setting the stage for comprehensive pulmonary assessment and optimization strategies.
⚡ Cardiovascular Risk Stratification: The Cardiac Crystal Ball
🫁 Pulmonary Optimization Matrix: The Respiratory Engineering System
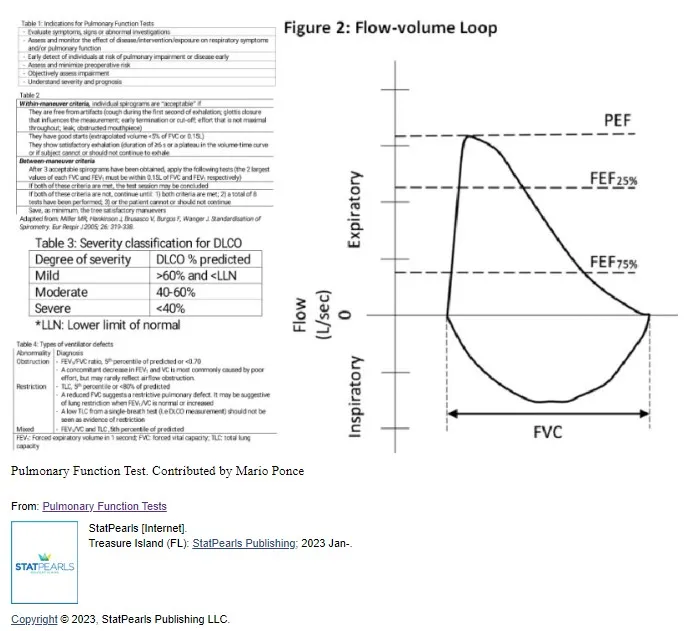
-
Pulmonary Risk Stratification Framework
- Patient factors: Age >65 years, BMI >30, smoking history >20 pack-years
- Procedure factors: Upper abdominal surgery, thoracic procedures, duration >3 hours
- Physiologic factors: FEV1 <80% predicted, DLCO <80%, SpO2 <92%
- COPD with FEV1 <1.5L increases risk 4-fold
- Restrictive disease with TLC <80% predicts complications
- ASA class ≥3 correlates with 25-40% PPC rates
-
Preoperative Optimization Interventions
- Smoking cessation ≥4 weeks before surgery reduces risk 40-50%
- Incentive spirometry training achieving >2500 mL volumes
- Bronchodilator therapy for FEV1 improvement >12%
- Albuterol 2.5 mg nebulized QID for 48-72 hours
- Ipratropium 0.5 mg added for COPD patients
- Systemic steroids 40-60 mg prednisone for exacerbations
📌 Remember: STOP-BANG Assessment - Snoring, Tiredness, Observed apnea, Pressure (HTN), BMI >35, Age >50, Neck >40cm, Gender (male). Score ≥3 indicates high OSA risk requiring perioperative CPAP and monitoring protocols.
⭐ Clinical Pearl: The "3-2-1 Pulmonary Rule" predicts 90% of high-risk patients: 3+ risk factors, 2+ abnormal PFTs, 1+ exacerbation in past year. These patients require intensive respiratory therapy and postoperative monitoring to prevent complications.
| Risk Category | PPC Rate | Optimization Time | Intervention Intensity | Monitoring Level |
|---|---|---|---|---|
| Low Risk | 2-5% | None required | Standard education | Routine |
| Moderate Risk | 8-15% | 1-2 weeks | Bronchodilators + IS | Enhanced |
| High Risk | 20-40% | 4-6 weeks | Comprehensive protocol | Intensive |
| Very High Risk | >40% | 6-8 weeks | Multidisciplinary | Critical |
| Emergency | Variable | Rapid optimization | Maximal therapy | Continuous |
- 6-minute walk test with <300 meters indicating high risk
- Arterial blood gas showing PaCO2 >45 mmHg or PaO2 <60 mmHg
- Chest CT revealing emphysema >25% or significant fibrosis
- DLCO <60% predicts prolonged mechanical ventilation
- RV/TLC ratio >40% indicates air trapping severity
- Exercise oximetry with >4% desaturation at peak
💡 Master This: Perioperative Respiratory Bundle - Preoperative education, Respiratory therapy, Early mobilization, Ventilator weaning protocols, Epidural analgesia, Nausea control, Thromboprophylaxis. Implementation reduces PPCs by 60-75% with cost savings of $3,000-5,000 per patient.
Comprehensive pulmonary optimization establishes respiratory safety foundations, connecting seamlessly to medication management protocols that ensure perioperative pharmacological safety and efficacy.
🫁 Pulmonary Optimization Matrix: The Respiratory Engineering System
💊 Medication Management Command: The Pharmacological Safety Net
-
High-Risk Medication Categories
- Anticoagulants: Warfarin, DOACs requiring specific timing protocols
- Antidiabetics: Insulin, metformin with perioperative adjustments
- Cardiovascular: ACE inhibitors, beta-blockers with hemodynamic implications
- Warfarin held 5 days before surgery (INR target <1.5)
- Rivaroxaban/Apixaban held 48-72 hours (renal function dependent)
- Metformin held 48 hours (eGFR <30 mL/min patients)
-
Continue vs. Hold Decision Framework
- Always continue: Beta-blockers, statins, chronic steroids >5 mg daily
- Always hold: Anticoagulants, metformin in renal dysfunction, herbals
- Case-dependent: ACE inhibitors, diuretics, insulin protocols
- Chronic steroids require stress-dose coverage (hydrocortisone 100 mg q8h)
- Beta-blockers continued to prevent rebound hypertension
- Statins reduce perioperative MI risk by 30-40%
📌 Remember: CHAMPS Hold Protocol - Coumadin/anticoagulants, Herbals/supplements, ACE inhibitors (case-dependent), Metformin (renal risk), Platelet inhibitors, SGLT2 inhibitors. This systematic approach prevents 85-90% of medication-related perioperative complications.
⭐ Clinical Pearl: The "5-3-1 Anticoagulation Rule" guides perioperative management: 5 days for warfarin, 3 days for DOACs (normal renal function), 1 day for heparin products. Bridge therapy indicated for mechanical valves, recent VTE <3 months, or high thrombotic risk (annual risk >10%).
| Medication Class | Hold Duration | Bridge Therapy | Restart Timing | Monitoring Required |
|---|---|---|---|---|
| Warfarin | 5 days | LMWH if high risk | POD 1-3 | Daily INR |
| DOACs | 48-72 hours | Rarely needed | 24-48 hours | Renal function |
| Clopidogrel | 5-7 days | Aspirin if CAD | 24-48 hours | Bleeding assessment |
| Metformin | 48 hours | None | Normal eGFR | Creatinine |
| ACE Inhibitors | Morning of surgery | None | POD 1 | BP monitoring |
- Type 1 diabetes: Never completely stop insulin (DKA risk)
- Type 2 diabetes: Hold long-acting insulin 50% night before
- Sliding scale: Regular insulin q6h with BG >180 mg/dL
- Target glucose 140-180 mg/dL perioperatively
- Hypoglycemia <70 mg/dL increases mortality 2-fold
- DKA risk with insulin cessation >12 hours
💡 Master This: Perioperative Steroid Protocol - Patients on chronic steroids >5 mg prednisone for >3 weeks require stress-dose coverage: Hydrocortisone 100 mg IV q8h starting pre-induction, taper over 48-72 hours. Prevents adrenal crisis occurring in 1-2% of at-risk patients with 30-50% mortality.
Systematic medication management creates pharmacological safety foundations, leading directly to comprehensive laboratory assessment protocols that guide perioperative decision-making and risk mitigation strategies.
💊 Medication Management Command: The Pharmacological Safety Net
🔬 Laboratory Intelligence Network: The Diagnostic Crystal Ball
-
Evidence-Based Testing Indications
- Age >65 years: CBC, BMP, consider ECG and chest X-ray
- Cardiovascular disease: CBC, BMP, PT/PTT if anticoagulated
- Renal/hepatic disease: Comprehensive metabolic panel, coagulation studies
- eGFR <60 mL/min requires nephrology consultation
- Platelet count <100,000 mandates hematology evaluation
- INR >1.5 delays elective surgery until correction
-
High-Yield Laboratory Thresholds
- Hemoglobin <10 g/dL: Consider transfusion or iron supplementation
- Creatinine >1.5 mg/dL: Nephrotoxic drug avoidance, contrast precautions
- Glucose >200 mg/dL: Diabetes optimization, perioperative insulin protocol
- HbA1c >8% associated with 3-fold infection risk
- Potassium <3.5 or >5.0 mEq/L requires correction before surgery
- Albumin <3.0 g/dL predicts poor wound healing
📌 Remember: LABS-SMART Testing - Liver function (hepatic disease), Anemia workup (Hgb <10), Bleeding time (anticoagulants), Sugar control (diabetes), Sodium/electrolytes (diuretics), Metabolic panel (renal disease), Arterial blood gas (pulmonary disease), Renal function (age >65), Thyroid (symptoms present). Selective testing based on clinical indications reduces unnecessary costs by 65-75%.
⭐ Clinical Pearl: The "3-Lab Rule" identifies 95% of clinically significant abnormalities: CBC (anemia, thrombocytopenia), BMP (renal function, electrolytes), PT/PTT (bleeding risk). Additional testing should be symptom-driven or comorbidity-specific to maintain cost-effectiveness.
| Test Category | Indication | Abnormal Threshold | Management Change | Cost-Effectiveness |
|---|---|---|---|---|
| CBC | Age >65, bleeding history | Hgb <10, Plt <100K | Transfusion/delay | High |
| BMP | Renal disease, diuretics | Cr >1.5, K <3.5/>5.0 | Optimization required | High |
| PT/PTT | Anticoagulants, liver disease | INR >1.5, PTT >40s | Reversal/delay | High |
| LFTs | Liver disease symptoms | ALT >2x normal | Hepatology consult | Moderate |
| ABG | Severe pulmonary disease | pH <7.35, CO2 >45 | Optimization | Moderate |
- Pregnancy: hCG, CBC, type and screen mandatory
- Pediatric: Hgb if <6 months or bleeding history
- Emergency surgery: CBC, BMP, PT/PTT, type and crossmatch
- Trauma patients require lactate, ABG, fibrinogen
- Massive transfusion protocol when >4 units anticipated
- Point-of-care testing reduces turnaround time 60-80%
💡 Master This: Perioperative Anemia Protocol - Hgb <10 g/dL triggers evaluation: Iron studies, B12/folate, reticulocyte count. Iron deficiency (ferritin <30 ng/mL) treated with IV iron 1000 mg over 2-4 weeks. Transfusion threshold 7-8 g/dL unless cardiovascular disease (threshold 8-9 g/dL). This approach reduces transfusion rates by 40-50%.
Comprehensive laboratory assessment completes the diagnostic foundation, seamlessly connecting to advanced integration protocols that synthesize all preoperative data into cohesive surgical decision-making frameworks.
🔬 Laboratory Intelligence Network: The Diagnostic Crystal Ball
🎛️ Advanced Integration Hub: The Surgical Decision Synthesis Engine
-
Multi-System Risk Integration Matrix
- Cardiovascular-Pulmonary Interaction: RCRI ≥2 + FEV1 <80% = 4-fold risk increase
- Metabolic-Renal Coupling: HbA1c >8% + eGFR <60 = 6-fold infection risk
- Medication-Laboratory Correlation: Anticoagulant use + platelet <150K = bleeding protocol
- Combined organ dysfunction increases mortality exponentially
- ≥3 abnormal systems require multidisciplinary consultation
- Frailty scores >5 predict prolonged recovery regardless of individual risks
-
Predictive Algorithm Integration
- ACS-NSQIP calculator incorporating 21 variables with C-statistic 0.85-0.90
- MICA score for cardiac risk with >95% negative predictive value
- ARISCAT score for pulmonary complications with sensitivity 85%
- Machine learning models outperform traditional scoring 15-20%
- Real-time risk adjustment based on intraoperative variables
- Outcome prediction accuracy improving with larger datasets
📌 Remember: SYNTHESIS Protocol - Systemic review, Yield optimization, Network integration, Timing coordination, Hazard mitigation, Emergency planning, Safety verification, Implementation strategy, Surveillance monitoring. This comprehensive approach ensures no critical element is overlooked in complex patients.
⭐ Clinical Pearl: The "Rule of 3s" identifies patients requiring intensive integration: 3+ organ systems involved, 3+ medications requiring adjustment, 3+ weeks optimization time needed. These patients benefit from dedicated coordinators and structured protocols, reducing complications by 50-70%.
| Integration Level | System Involvement | Coordination Required | Optimization Time | Success Rate |
|---|---|---|---|---|
| Simple | 1-2 systems | Standard protocols | 1-2 weeks | 95-98% |
| Moderate | 2-3 systems | Enhanced coordination | 2-4 weeks | 90-95% |
| Complex | 3-4 systems | Multidisciplinary | 4-6 weeks | 85-90% |
| Very Complex | >4 systems | Intensive management | 6-8 weeks | 80-85% |
| Emergency | Variable | Rapid optimization | <24 hours | 70-80% |
- Electronic health records with automated risk scoring and alert systems
- Clinical decision support providing real-time recommendations
- Telemedicine consultations reducing specialist wait times by 60-80%
- AI-powered risk assessment identifying missed risk factors
- Mobile applications for patient education and compliance monitoring
- Predictive analytics for resource allocation and scheduling optimization
💡 Master This: Perioperative Optimization Bundle - Predictive modeling, Evidence-based protocols, Risk stratification, Integrated care teams, Outcome monitoring, Patient engagement. Implementation requires 6-month institutional commitment but achieves ROI of 300-400% through reduced complications, shorter stays, and improved satisfaction scores.
Advanced integration capabilities establish the foundation for rapid mastery tools that enable immediate clinical application and long-term expertise development in preoperative assessment and management.
🎛️ Advanced Integration Hub: The Surgical Decision Synthesis Engine
🚀 Preoperative Mastery Arsenal: The Clinical Excellence Toolkit

📌 Remember: MASTER-PREP Checklist - Medical optimization complete, Airway assessment documented, Surgical risk stratified, Timing appropriate, Emergency plans established, Resources allocated, Patient educated, Records complete, Equipment ready, Personnel briefed. This 10-point verification ensures comprehensive readiness with <2% oversight rate.
-
Essential Clinical Thresholds
- Cardiac: RCRI ≥3 = cardiology consult, METs <4 = stress testing
- Pulmonary: FEV1 <80% = optimization, SpO2 <92% = ABG analysis
- Laboratory: Hgb <10 = anemia workup, Cr >1.5 = nephrology input
- INR >1.5 delays elective surgery until <1.3
- Glucose >200 mg/dL requires endocrine consultation
- Albumin <3.0 g/dL predicts delayed healing
-
Rapid Assessment Protocol
- 2-minute cardiovascular screening using RCRI + functional capacity
- 3-minute pulmonary evaluation with risk factors + spirometry
- 1-minute medication reconciliation focusing high-risk drugs
- 30-second airway assessment using LEMON criteria
- 45-second laboratory review targeting critical values
- 60-second patient education covering key expectations
⭐ Clinical Pearl: The "Golden Hour" of preoperative assessment - 60 minutes of focused evaluation can identify 95% of optimization opportunities. Structure: 15 minutes history, 15 minutes examination, 15 minutes risk stratification, 15 minutes planning. This approach achieves expert-level accuracy with time efficiency.
| Assessment Component | Time Allocation | Key Elements | Decision Points | Quality Metrics |
|---|---|---|---|---|
| History | 15 minutes | Symptoms, medications, function | Risk factors present? | Completeness >95% |
| Examination | 15 minutes | Cardiac, pulmonary, airway | Abnormalities found? | Accuracy >90% |
| Risk Stratification | 15 minutes | RCRI, ASA, functional status | High risk identified? | Sensitivity >85% |
| Planning | 15 minutes | Optimization, timing, monitoring | Changes needed? | Appropriateness >90% |
| Documentation | 5 minutes | Risk assessment, plan | Complete record? | Compliance >98% |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | ||||
| flowchart TD |
Start["<b>📋 Patient Encounter</b><br><span style='display:block; text-align:left; color:#555'>• Initial intake</span><span style='display:block; text-align:left; color:#555'>• Vital signs</span>"]
Screen["<b>🔬 Rapid Screening</b><br><span style='display:block; text-align:left; color:#555'>• Quick assessment</span><span style='display:block; text-align:left; color:#555'>• Risk check</span>"]
Risk{{"<b>📋 High Risk?</b><br><span style='display:block; text-align:left; color:#555'>• Evaluate level</span><span style='display:block; text-align:left; color:#555'>• Clinical judgement</span>"}}
StdEval["<b>🔬 Standard Eval</b><br><span style='display:block; text-align:left; color:#555'>• Routine labs</span><span style='display:block; text-align:left; color:#555'>• Basic workup</span>"]
StdPrep["<b>💊 Routine Prep</b><br><span style='display:block; text-align:left; color:#555'>• Pre-op orders</span><span style='display:block; text-align:left; color:#555'>• Fasting protocol</span>"]
StdMon["<b>👁️ Standard Mon</b><br><span style='display:block; text-align:left; color:#555'>• Basic telemetry</span><span style='display:block; text-align:left; color:#555'>• BP tracking</span>"]
CompAssess["<b>📋 Comprehensive</b><br><span style='display:block; text-align:left; color:#555'>• Deep assessment</span><span style='display:block; text-align:left; color:#555'>• Full history</span>"]
OptiProt["<b>💊 Optimization</b><br><span style='display:block; text-align:left; color:#555'>• Stabilize disease</span><span style='display:block; text-align:left; color:#555'>• Med management</span>"]
MultiPlan["<b>📋 Multidisciplin</b><br><span style='display:block; text-align:left; color:#555'>• Team planning</span><span style='display:block; text-align:left; color:#555'>• Specialist input</span>"]
EnhSurv["<b>👁️ Enhanced Surv</b><br><span style='display:block; text-align:left; color:#555'>• ICU readiness</span><span style='display:block; text-align:left; color:#555'>• Close monitoring</span>"]
Clear["<b>✅ Surgery Clear</b><br><span style='display:block; text-align:left; color:#555'>• Final approval</span><span style='display:block; text-align:left; color:#555'>• Proceed to OR</span>"]
Start --> Screen
Screen --> Risk
Risk -->|No| StdEval
StdEval --> StdPrep
StdPrep --> StdMon
StdMon --> Clear
Risk -->|Yes| CompAssess
CompAssess --> OptiProt
OptiProt --> MultiPlan
MultiPlan --> EnhSurv
EnhSurv --> Clear
style Start fill:#FEF8EC,stroke:#FBECCA,stroke-width:1.5px,rx:12,ry:12,color:#854D0E
style Screen fill:#FFF7ED,stroke:#FFEED5,stroke-width:1.5px,rx:12,ry:12,color:#C2410C
style Risk fill:#FEF8EC,stroke:#FBECCA,stroke-width:1.5px,rx:12,ry:12,color:#854D0E
style StdEval fill:#FFF7ED,stroke:#FFEED5,stroke-width:1.5px,rx:12,ry:12,color:#C2410C
style StdPrep fill:#F1FCF5,stroke:#BEF4D8,stroke-width:1.5px,rx:12,ry:12,color:#166534
style StdMon fill:#EEFAFF,stroke:#DAF3FF,stroke-width:1.5px,rx:12,ry:12,color:#0369A1
style CompAssess fill:#FEF8EC,stroke:#FBECCA,stroke-width:1.5px,rx:12,ry:12,color:#854D0E
style OptiProt fill:#F1FCF5,stroke:#BEF4D8,stroke-width:1.5px,rx:12,ry:12,color:#166534
style MultiPlan fill:#FEF8EC,stroke:#FBECCA,stroke-width:1.5px,rx:12,ry:12,color:#854D0E
style EnhSurv fill:#EEFAFF,stroke:#DAF3FF,stroke-width:1.5px,rx:12,ry:12,color:#0369A1
style Clear fill:#F6F5F5,stroke:#E7E6E6,stroke-width:1.5px,rx:12,ry:12,color:#525252
* **Quality Assurance Framework**
- **Process metrics**: Assessment completion **>95%**, documentation accuracy **>98%**
- **Outcome metrics**: Complication reduction **>40%**, patient satisfaction **>90%**
- **Efficiency metrics**: Assessment time **<60 minutes**, optimization success **>85%**
+ **Continuous improvement** through **monthly reviews**
+ **Peer feedback** systems with **structured evaluations**
+ **Technology integration** for **automated quality monitoring**
> 💡 **Master This**: **Preoperative Excellence Formula** = **Systematic Assessment** × **Evidence-Based Decisions** × **Coordinated Implementation** × **Continuous Monitoring**. This approach achieves **top-quartile outcomes** with **cost reduction of 20-30%** and **patient satisfaction scores >95%**. Success requires **institutional commitment** and **standardized protocols** across all surgical services.
The preoperative mastery arsenal provides the essential tools and frameworks needed for expert-level perioperative assessment, enabling clinicians to deliver consistent, evidence-based care that optimizes surgical outcomes while maintaining efficiency and cost-effectiveness.
🚀 Preoperative Mastery Arsenal: The Clinical Excellence Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























