USGRA Basics - Pixel Perfect Puncture
- Principle: Real-time ultrasound guidance for precise needle placement and local anesthetic (LA) delivery near target nerves.
- Advantages:
- ↑ Success, ↓ block onset time.
- ↓ Complications (vascular puncture, nerve injury).
- ↓ LA volume needed.
- Key Views & Terms:
- In-Plane (IP): Needle shaft & tip seen longitudinally. Preferred.
- Out-of-Plane (OOP): Needle as a dot; harder to track tip.
- Anisotropy: Echogenicity varies with beam angle; affects nerve/needle visibility.
⭐ USGRA allows visualization of LA spread, helping confirm correct placement and avoid intraneural injection, enhancing safety.
USG Machine & Probes - Knobology Know-How
- Components: Transducer, CPU, Display, Control Panel.
- Probes:
- Linear: High frequency (6-15 MHz); superficial nerves/vessels. Superior resolution.
- Curvilinear: Low frequency (2-5 MHz); deeper structures (e.g., paravertebral).
- Phased Array: Small footprint; cardiac, intercostal.
- Key Controls:
- Frequency: ↑ for superficial, ↓ for deep.
- Depth: Adjust view.
- Gain: Overall brightness.
- TGC: Depth-specific brightness.
- Focus: Optimize resolution.
- Probe Maneuvers (📌 P-A-R-T-S): Pressure, Alignment, Rotation, Tilt, Sliding.
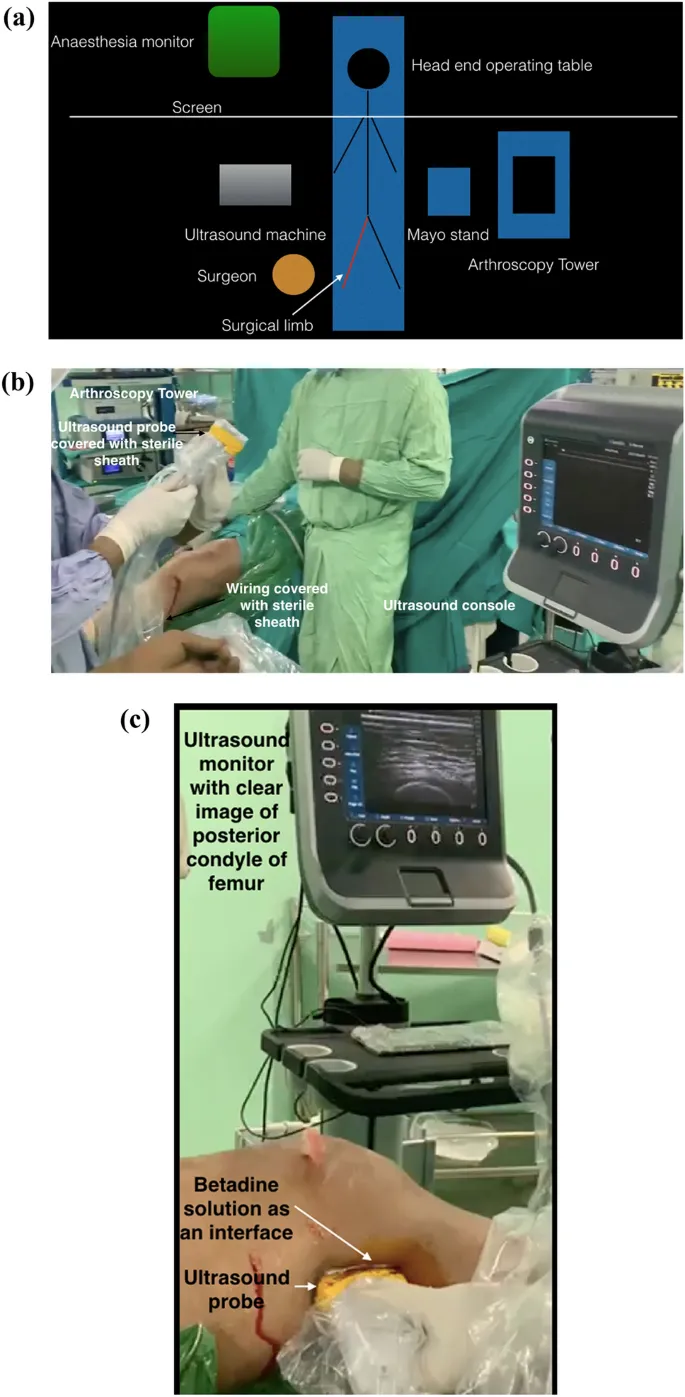
⭐ High-frequency linear probes (>7.5 MHz) are preferred for most peripheral nerve blocks due to superior superficial resolution.
Sonoanatomy for RA - See The Unseen
-
Key Structures & Appearance:
- Nerves: Hyperechoic, honeycomb (fascicular) or hypoechoic (non-fascicular).
- Arteries: Anechoic, round/oval, pulsatile, non-compressible.
- Veins: Anechoic, oval/flat, non-pulsatile, compressible.
- Fascia: Hyperechoic linear structures.
- Bone: Hyperechoic surface with posterior acoustic shadowing.
- Pleura: Hyperechoic, shimmering/sliding line (lung sliding).
- Muscle: Hypoechoic with internal hyperechoic fibroadipose septa.
- Tendon: Hyperechoic, fibrillar pattern, anisotropic.
-
Common Artifacts:
- Shadowing: Signal loss posterior to dense structures (bone, calcification).
- Reverberation: Multiple, equally spaced lines (e.g., needle).
- Anisotropy: Structure's echogenicity changes with ultrasound beam angle (esp. nerves, tendons).
- Enhancement: Increased echogenicity posterior to fluid-filled structures.
⭐ Nerves often appear as a "honeycomb" or "starry night" pattern in transverse view due to hyperechoic connective tissue (perineurium) surrounding hypoechoic nerve fascicles. This is crucial for identification during nerve blocks.
📌 Mnemonic: Bones Are Missing Sound (BAMS) for acoustic shadowing behind bones/calcification.
Needle Guidance Techniques - Point & Shoot
- An Out-Of-Plane (OOP) needle guidance method.
- Needle appears as a hyperechoic dot (cross-section) when intersecting the ultrasound beam.
- Technique Steps:
- Align ultrasound beam over the target structure.
- Insert needle, aiming along the predicted trajectory towards the beam's path.
- Advance needle in small increments.
- Adjust probe (slide, fan, or tilt) to re-localize the needle tip.
- Repeat advancement and re-localization until target is reached.
- Relies heavily on predicting the needle's path relative to the beam.
- Often used for superficial targets or vascular access.
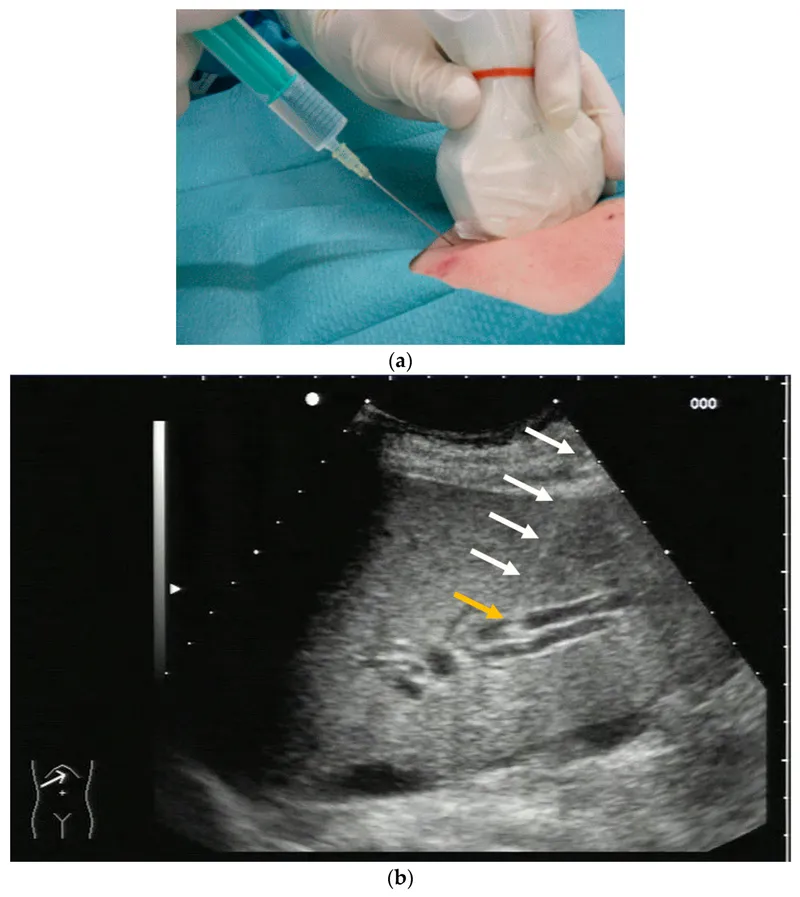
⭐ This technique, also known as the "walk-down" or "chase" technique, requires frequent probe manipulation to track the needle tip, which is seen intermittently as a dot, demanding significant hand-eye coordination and spatial awareness for safety and accuracy near critical structures.
High‑Yield Points - ⚡ Biggest Takeaways
- Ultrasound guidance boosts block success and cuts complications (e.g., vascular puncture).
- High-frequency linear probes (e.g., 6-13 MHz) are best for PNBs due to high superficial resolution.
- Key views: Short-axis (SAX) shows "honeycomb" nerve; Long-axis (LAX) for in-plane needle path.
- Nerves are typically hyperechoic with a distinct fascicular pattern.
- Anisotropy: nerve brightness changes with probe tilt; perpendicular alignment is key.
- "Donut sign" (SAX) confirms circumferential local anesthetic spread around the nerve.
- In-plane technique allows full needle visualization, improving safety during insertion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

