Probe Selection and Manipulation - Probe Profile Party
| Probe | Freq. (MHz) | Image | Key Features | Common Anesthetic Uses |
|---|---|---|---|---|
| Linear | High (5-15) | Rectangular | ↑Resolution, ↓Depth | Vascular access, superficial nerves, pleura, ocular |
| Curvilinear | Low (2-5) | Curved Sector | ↓Resolution, ↑Depth | FAST, abdomen, deep lung, difficult airway (subglottic) |
| Phased Array | Low (1-5) | Pointed Sector | Small footprint, steerable | Cardiac (TTE), deep lung, FAST, transcranial |
Probe Manipulations (📌 Mnemonic: PARTS):
- Pressure: Optimal acoustic coupling.
- Alignment: Long/short axis to target.
- Rotation: Twisting on central axis.
- Tilting (Rocking): Angling beam, footprint static.
- Sliding (Sweeping): Moving footprint across skin.
⭐ Higher frequency probes offer better resolution but less penetration; lower frequency probes provide greater penetration but with lower resolution. This is a fundamental trade-off in probe selection for optimal imaging based on target depth and required detail.
Probe Selection and Manipulation - Wave Wisdom Wonders
- Probe Choice & Frequency:
- Linear (5-15 MHz): High resolution, superficial (vascular access, nerve blocks).
- Curvilinear (Convex, 2-5 MHz): Lower resolution, deeper (abdomen, FAST).
- Phased Array (1-5 MHz): Small footprint, deep, steerable beam (cardiac, TCD).
- Core Physics:
- $Resolution \propto Frequency$ (↑Freq = ↑Res)
- $Penetration \propto 1/Frequency$ (↑Freq = ↓Depth)
- 📌 LUF: Low Frequency = Deeper Penetration, Lower Resolution.
- 📌 HUH: High Frequency = Superficial, Higher Resolution.
- Basic Manipulations:
- Sliding: Moving probe.
- Tilting: Angling beam.
- Rotation: Twisting probe.
- Compression: Assessing tissue.
- Rocking: Heel-toe motion.
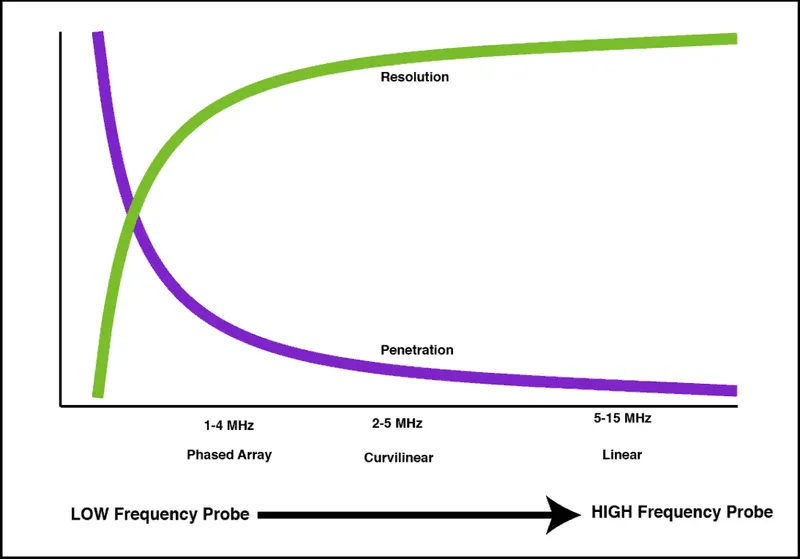
⭐ Optimal image acquisition requires selecting the highest frequency probe that can penetrate to the target depth.
Probe Selection and Manipulation - Scan Smart Steps
-
Probe Choice: Match Frequency to Depth
- High Frequency (e.g., 7-15 MHz, Linear): Superficial structures (nerves, vessels, pleura). Detail > Penetration.
- Low Frequency (e.g., 2-5 MHz, Curvilinear/Phased Array): Deeper structures (cardiac, abdominal, lung). Penetration > Detail.
- Specialized: Endocavitary (transvaginal, transrectal), TEE (transesophageal).
-
Basic Probe Maneuvers: 📌 PARTS
- Pressure: Apply to improve contact, displace air/fat.
- Alignment: Align probe with long/short axis of target.
- Rotation: Turn probe around its central axis.
- Tilt (Angulation): Sweep beam side-to-side/up-down without moving footprint.
- Sweep/Sliding: Move probe across skin surface.

-
Optimize Image: Adjust Depth (target in middle 2/3), Gain (overall brightness), TGC (Time Gain Compensation for depth-specific gain), Focus (at/below target).
⭐ Anisotropy: Tendons or nerves may appear falsely hypoechoic if the US beam is not perpendicular to their fibers. Correct by slightly angling or rocking the probe (heel-toe maneuver) to achieve perpendicularity.
Probe Selection and Manipulation - View Virtues & Vexations
-
Probe Manipulation (📌 PARTS):
- Pressure: Optimizes acoustic coupling, displaces bowel gas.
- Angulation (Tilting/Rocking): Sweeps beam across a plane; footprint stationary.
- Rotation: Turns probe on its central axis (e.g., transverse to longitudinal).
- Translation (Sliding): Moves probe across skin surface to new window.
- Screen Orientation: Probe marker (notch/dot) corresponds to screen indicator (left for transverse, cephalad for sagittal).
-
Common Artifacts:
Artifact Appearance Cause Remedy Shadowing Hypoechoic area deep to object High attenuation (bone, stone, air) Change angle, ↓frequency, harmonics Reverberation Multiple, parallel bright lines Sound 'bounces' between reflectors ↓Gain, change angle, harmonics, pressure Mirror Image Duplicated structure across line Strong, smooth reflector (diaphragm) ↓Gain, change angle, identify reflector Edge Shadow Hypoechoic bands at curved edge Beam refraction/reflection Compound imaging, change angle, steer
⭐ Anisotropy: Tendon/nerve echogenicity changes with insonation angle; perpendicular (90°) imaging is key for optimal visualization.
High‑Yield Points - ⚡ Biggest Takeaways
- Probe choice: High-frequency (>7 MHz linear) for superficial, high-resolution (vessels, nerves); Low-frequency (2-5 MHz curvilinear/phased array) for deep penetration (cardiac, abdomen).
- Master basic movements: Sliding, Tilting (Rocking), Rotating, Compression.
- Anisotropy: Minimize by keeping beam perpendicular to nerves for best visualization.
- Orientation marker (probe & screen) is crucial for correct anatomical interpretation.
- Use ultrasound gel for essential acoustic coupling and optimal image quality.
- Depth and gain settings must be optimized for clear imaging of the target structure; adjust frequently during scanning.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

