Airway US Basics - Scan & See
- Why Airway US?
- Non-invasive, real-time, dynamic assessment.
- Complements static predictors (e.g., Mallampati).
⭐ Ultrasound offers a dynamic, real-time assessment of the airway, complementing traditional static predictors like Mallampati score.
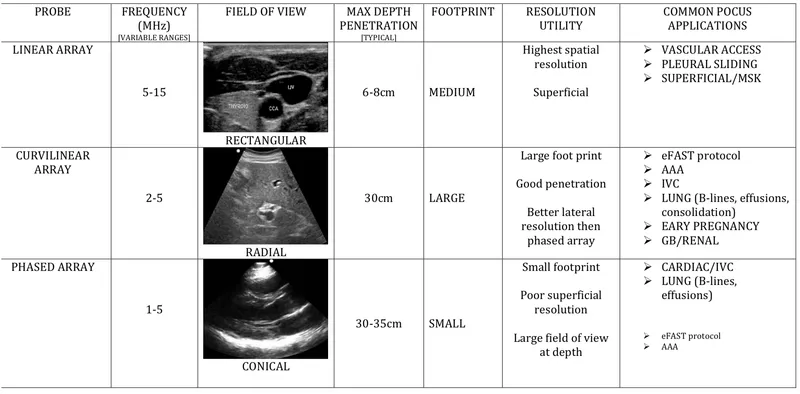
- Probe Selection:
- High-frequency linear (5-12 MHz): Superior resolution for superficial structures (e.g., vocal cords, cricothyroid membrane).
- Low-frequency curvilinear (2-5 MHz): Better penetration for deeper structures, wider field (e.g., epiglottis, subglottic view).
- Basic Views & Structures:
- Scan in transverse & sagittal planes.
- Identify: Hyoid bone, epiglottis, thyroid cartilage, vocal cords (true/false), cricoid cartilage, tracheal rings.
Sonoanatomy - Airway Atlas
- Tongue & Floor of Mouth:
- Genioglossus muscle: Hypoechoic, bulky, forms tongue base.
- Mylohyoid muscle: Thin, hypoechoic band inferiorly.
- Hyoid Bone: Key landmark.
⭐ The hyoid bone, appearing as a hyperechoic curved line with posterior acoustic shadowing, is a primary landmark for orienting airway ultrasound.
- Laryngeal Structures (Superior to Inferior):
- Epiglottis: Hypoechoic, leaf-like; anterior pre-epiglottic space (hypoechoic fat).
- Thyroid Cartilage: Hyperechoic; inverted V-shape (transverse), linear (sagittal). Vocal cord attachment.
- Vocal Cords: True (hypoechoic, medial) & False (hyperechoic, lateral) - "sandwich sign" at glottis.
- Arytenoid Cartilages: Hypoechoic, pyramidal, atop posterior cricoid.
- Cricoid Cartilage: Hyperechoic complete ring; "signet ring" appearance.
- Trachea & Esophagus:
- Tracheal Rings: Anterior, hyperechoic, C-shaped/inverted U-shapes ("string of beads" sign). Air-mucosa interface (A-line).
- Esophagus: Typically collapsed, posterior/postero-lateral to trachea; multilayered "target sign".

Prediction Parameters - Crystal Ball Scan
- PTST (Pre-tracheal Soft Tissue):
- ↑ PTST-VC (Vocal Cords): >2.8 mm predicts difficult laryngoscopy (DL).
- ↑ PTST-H (Hyoid).
- SED (Skin-to-Epiglottis Distance):
- ↓ SED is a key predictor of difficult intubation.
- Tongue Dimensions:
- ↑ Thickness/volume linked to difficult airway.
- Other Distances:
- ↓ sHMD (Sonographic Hyomental Distance).
- ↓ Skin-to-Anterior Commissure distance.
- Visibility:
- Impaired view of hyoid, epiglottis, vocal cords.
⭐ Key predictors of difficult intubation include increased pre-tracheal soft tissue thickness at the vocal cord level and a reduced skin-to-epiglottis distance.
)
Clinical Uses - Guided Moves
- ETT Confirmation:
- Transtracheal: Direct ETT view, cuff inflation, "double tract sign" (trachea anterior, esophagus posterior).
- Transthoracic: Bilateral lung sliding ("ants marching"), diaphragm movement.
- LMA Confirmation:
- Verify correct tip placement in hypopharynx.
- Procedure Guidance:
- Percutaneous Dilatational Tracheostomy (PDT): Midline, vessels (e.g., AJV, ITA), pre-tracheal structures, best puncture site.
- Cricothyroidotomy: Rapid cricothyroid membrane identification.
- Nerve Blocks (e.g., SLN, transtracheal): Precise needle guidance, local anesthetic spread.
⭐ Transtracheal ultrasound reliably confirms endotracheal tube placement by visualizing the tube within the trachea, often with a 'double tract' sign if the esophagus is also seen.
High‑Yield Points - ⚡ Biggest Takeaways
- Airway ultrasound rapidly identifies key landmarks: hyoid, epiglottis, vocal cords, trachea, cricothyroid membrane.
- Vocal cord mobility: Assessed by "bilateral shimmering" or symmetrical adduction/abduction.
- ETT confirmation: Direct tracheal visualization (e.g., "bullet sign", tracheal rings) and bilateral lung sliding are crucial.
- Cricothyroid membrane (CTM): Accurately located between thyroid and cricoid for emergency front-of-neck access (FONA).
- Subglottic diameter measurement: Aids in pediatric ETT sizing and detecting potential stenosis.
- Predicts difficult intubation: By assessing anterior neck soft tissue thickness or hyomental distance extended (HMDE).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

