Abdominal POCUS Essentials - Knobs & Probes
- Probes (Transducers):
- Curvilinear (Abdominal): 2-5 MHz; wide footprint, deep penetration. For general abdomen, FAST, aorta, RUQ, LUQ.
- Linear (Superficial): 5-12 MHz; high resolution, shallow penetration. For appendix, DVT, foreign bodies.
- Phased Array (Cardiac/FAST): 1-5 MHz; small footprint, good for intercostal views.
- Key Knobs (B-mode):
- Gain: Overall image brightness.
- Depth: Adjusts field of view (FOV).
- Frequency: 📌 High Freq = ↑Res (Superficial); Low Freq = ↑Penetration (Deep).
- Focus: Optimizes lateral resolution at specific depth.
- Freeze: Captures image.
- Measure: Calipers for dimensions.

⭐ The curvilinear probe is the workhorse for most abdominal POCUS applications due to its balance of penetration and resolution for visualizing deep abdominal structures effectively during exams like FAST scan (Focused Assessment with Sonography for Trauma).
FAST & eFAST - Trauma Truths
- FAST: Focused Assessment with Sonography for Trauma. Rapidly identifies free intraperitoneal fluid (hemoperitoneum) or pericardial effusion.
- Positive: Anechoic (black) collections in dependent areas.
- Key Views (📌 4 Ps):
- Perihepatic (RUQ, Morison's Pouch - most sensitive for hemoperitoneum)
- Perisplenic (LUQ)
- Pelvic (Suprapubic, Pouch of Douglas - most dependent)
- Pericardial (Subxiphoid - for tamponade)
- eFAST: Extended FAST. Adds bilateral anterior thoracic views (2nd-4th intercostal spaces).
- Detects: Pneumothorax, Hemothorax (pleural fluid).
- Goal: Guide immediate life-saving interventions in trauma resuscitation (ATLS algorithm).
- Key pneumothorax signs: Absent "lung sliding", absent B-lines ("comet-tails"), "stratosphere sign" (M-mode).
⭐ The "lung point" sign in eFAST, where normal lung sliding pattern meets an absent lung sliding pattern, is virtually 100% specific for pneumothorax.
Gastric Ultrasound - Full or Empty?
- Goal: Assess aspiration risk preoperatively.
- Technique:
- Probe: Curvilinear (2-5 MHz).
- Position: Supine, then Right Lateral Decubitus (RLD).
- View: Sagittal, antrum (between aorta & L-lobe liver).
- Qualitative Signs:
- Empty: "Bull's eye" sign (collapsed).
- Fluid: Anechoic (clear); hyperechoic (particulate/solid - "frosted glass").
- Perlas Grading (Antrum in RLD):
- Grade 0: Empty. Low risk.
- Grade 1: Fluid only in RLD. Low risk.
- Grade 2: Fluid in supine & RLD. High risk.
- Quantitative (RLD position):
- Gastric volume > 1.5 mL/kg → high risk.
- Antral CSA > 3.4 cm² → suggests high volume.
⭐ Solids or particulate matter visible in the antrum signify a "full" stomach, mandating aspiration precautions, regardless of calculated volume.

Key Organ Views - Beyond FAST
- Gallbladder & Biliary Tree:
- Acute Cholecystitis: Wall thickening >3mm, pericholecystic fluid, sonographic Murphy's sign.
- Cholelithiasis (gallstones), Choledocholithiasis (CBD stones, CBD diameter >6mm).
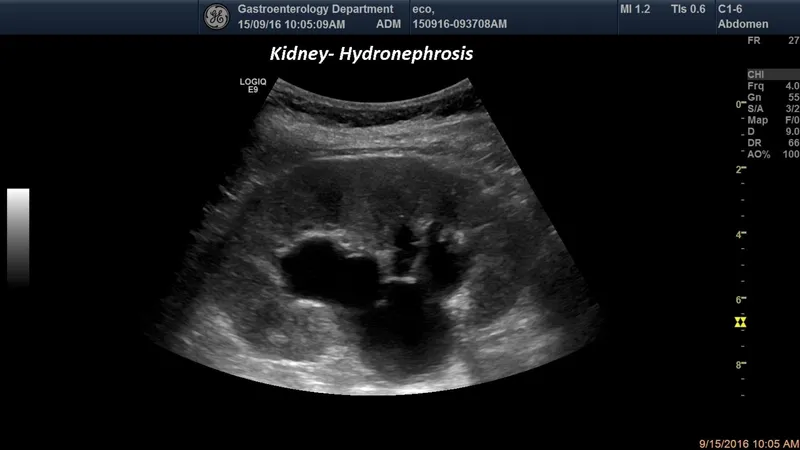
- Kidneys & Bladder:
- Hydronephrosis: Dilated renal pelvis/calyces, indicating obstruction.
- Renal calculi (stones).
- Bladder: Distension, volume assessment ( $V \approx 0.52 \times H \times W \times D$ ), Foley catheter placement.
- Aorta:
- Abdominal Aortic Aneurysm (AAA): Screen for dilation >3cm (outer-to-outer, infrarenal).
- Critical diameter >5.5cm often warrants intervention.
- Bowel:
- Ileus: Dilated, fluid-filled loops, ↓ or absent peristalsis.
- Small Bowel Obstruction (SBO): Dilated loops >2.5cm, wall edema, to-and-fro peristalsis.
⭐ Sonographic Murphy's sign (maximal tenderness over sonographically localized gallbladder) has higher specificity for acute cholecystitis than clinical Murphy's sign.
High‑Yield Points - ⚡ Biggest Takeaways
- FAST scan is crucial in trauma for free fluid detection (e.g., Morison's pouch).
- eFAST adds thoracic views for pneumothorax (no lung sliding) and hemothorax.
- Gastric ultrasound (antral CSA) assesses aspiration risk preoperatively.
- Lung US: A-lines (normal aeration), B-lines (pulmonary edema/interstitial syndrome).
- IVC collapsibility index aids in assessing fluid responsiveness.
- Guides vascular access (CVCs) and regional nerve blocks (e.g., TAP).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

