Perioperative Ultrasound

On this page
🎯 Perioperative POCUS Mastery: Your Surgical Command Center
Perioperative ultrasound transforms you from a clinician who orders images into one who generates answers in real time at the bedside, the operating table, and during critical moments when decisions cannot wait. You'll master the physics that govern image quality, learn which probe and settings match each clinical question, and build systematic approaches for cardiac assessment, volume status, lung pathology, and vascular access. This isn't about becoming a radiologist-it's about integrating dynamic visual data into your surgical and anesthetic decision-making when seconds matter. By the end, you'll wield ultrasound as both diagnostic tool and procedural guide, elevating your clinical precision across the entire perioperative spectrum.
Understanding perioperative POCUS requires systematic mastery of multiple organ systems, each with specific imaging protocols and clinical applications. The integration spans from preoperative assessment through postoperative monitoring, creating a comprehensive diagnostic framework.
-
Cardiac Assessment Applications
- Preoperative ventricular function evaluation (ejection fraction >55% normal)
- Intraoperative volume status monitoring (IVC diameter <2.1cm suggests hypovolemia)
- Postoperative tamponade detection (pericardial effusion >2cm concerning)
- Hemodynamic instability correlation: >90% sensitivity
- Emergency intervention timing: <15 minutes critical window
- Survival impact: 3-fold improvement with early detection
-
Pulmonary POCUS Integration
- Pneumothorax identification (100% specificity with absent lung sliding)
- Pleural effusion quantification (>500ml detectable reliably)
- Lung recruitment assessment (B-line patterns indicate interstitial edema)
- Diagnostic accuracy: >95% vs chest X-ray 70%
- Time to diagnosis: <3 minutes vs 20-30 minutes for imaging
- Clinical impact: 50% reduction in unnecessary procedures
📌 Remember: FALLS mnemonic for perioperative POCUS applications - Fluid status, Airway assessment, Lung pathology, Left heart function, Shock evaluation. Each component provides quantitative data within 2-3 minutes of scanning.
| POCUS Application | Primary Indication | Diagnostic Accuracy | Time to Result | Clinical Impact | Complication Reduction |
|---|---|---|---|---|---|
| Cardiac Function | Hemodynamic instability | >95% | <5 minutes | Volume management | 45% |
| Lung Assessment | Respiratory distress | >90% | <3 minutes | Ventilator settings | 35% |
| Vascular Access | Central line placement | >98% | <2 minutes | First-pass success | 60% |
| Gastric Volume | Aspiration risk | >85% | <4 minutes | Anesthetic timing | 70% |
| Neuraxial Guidance | Spinal/epidural | >80% | <6 minutes | Success rate | 40% |
💡 Master This: Every perioperative POCUS examination follows the "Rule of 3s" - 3 views minimum per organ system, <3 minutes per assessment, 3-point clinical correlation (history, physical, imaging). This systematic approach ensures comprehensive evaluation while maintaining workflow efficiency.
Connect these foundational POCUS principles through systematic imaging protocols to understand how structured assessment transforms perioperative decision-making into evidence-based precision medicine.
🎯 Perioperative POCUS Mastery: Your Surgical Command Center
🔬 Ultrasound Physics Mastery: The Wave Engineering Blueprint
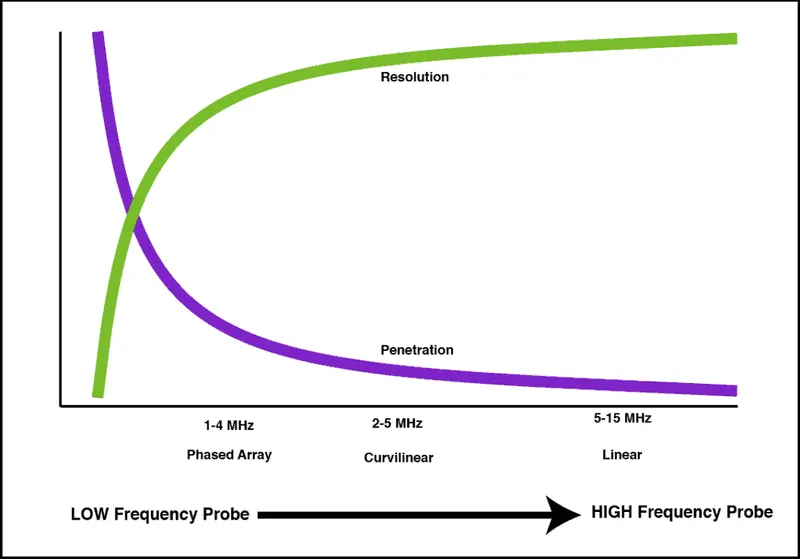
Understanding acoustic wave behavior predicts every imaging characteristic and optimization strategy. The relationship between frequency, wavelength, and penetration determines probe selection and image quality for specific clinical applications.
-
Frequency-Penetration Relationships
- High frequency (10-15 MHz): Penetration 2-4cm, resolution <0.5mm
- Medium frequency (5-10 MHz): Penetration 8-15cm, resolution 1-2mm
- Low frequency (2-5 MHz): Penetration >20cm, resolution 2-4mm
- Clinical correlation: Inverse relationship between frequency and penetration
- Resolution trade-off: Higher frequency = better resolution but less penetration
- Optimal selection: Match frequency to target depth and required detail
-
Acoustic Impedance Principles
- Tissue interfaces: Impedance mismatch creates reflection and refraction
- Air-tissue boundary: 99.9% reflection (complete acoustic barrier)
- Bone-soft tissue: >90% reflection (limited penetration)
- Gel coupling: Eliminates air interface for optimal transmission
- Angle optimization: Perpendicular incidence maximizes signal return
- Gain adjustment: Compensates for depth-related attenuation
📌 Remember: FLAW mnemonic for ultrasound physics optimization - Frequency selection, Lateral resolution, Axial resolution, Wavelength relationship. Frequency determines penetration (inversely), wavelength determines lateral resolution, pulse length determines axial resolution.
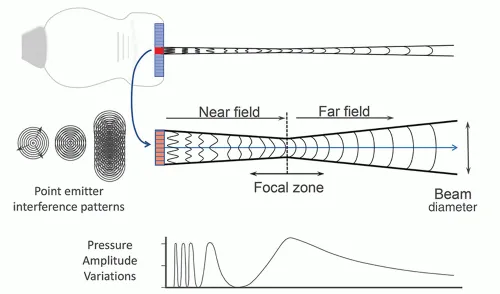
| Frequency (MHz) | Wavelength (mm) | Penetration (cm) | Axial Resolution (mm) | Lateral Resolution (mm) | Clinical Application |
|---|---|---|---|---|---|
| 2-3 | 0.8-1.2 | >20 | 2-4 | 3-5 | Abdominal, cardiac |
| 5-7 | 0.3-0.6 | 10-15 | 1-2 | 2-3 | General imaging |
| 10-12 | 0.15-0.25 | 4-6 | 0.5-1 | 1-2 | Vascular access |
| 15-18 | 0.1-0.15 | 2-4 | <0.5 | <1 | Superficial structures |
💡 Master This: Time-gain compensation (TGC) corrects for exponential attenuation following the relationship: $I = I_0 \times e^{-\alpha \times d}$ where α = attenuation coefficient (0.5-1 dB/cm/MHz in soft tissue), d = depth. Proper TGC maintains uniform brightness across imaging depth.
Connect these physics principles through probe selection strategies to understand how acoustic engineering enables optimal image quality for specific perioperative applications.
🔬 Ultrasound Physics Mastery: The Wave Engineering Blueprint
🎛️ Machine Mastery: The Control Center Architecture
Understanding control interactions enables systematic image optimization following logical sequences rather than random adjustments. Each control affects specific image characteristics with predictable relationships to acoustic physics.
-
Primary Image Controls
- Gain (overall): Amplifies all returning echoes uniformly (0-100% range)
- Time-gain compensation: Depth-specific amplification (exponential correction)
- Depth adjustment: Field of view (2-30cm typical range)
- Gain optimization: Just below noise threshold for maximum sensitivity
- TGC curve: Exponential increase compensating tissue attenuation
- Depth selection: Minimum depth containing target structure for optimal resolution
-
Advanced Optimization Controls
- Frequency selection: Penetration vs resolution trade-off
- Focus position: Beam narrowing at target depth
- Dynamic range: Contrast sensitivity (40-80dB typical)
- Frequency tuning: Higher frequency for superficial targets (<5cm)
- Focus placement: At or just below target structure depth
- Dynamic range: Lower values (40-50dB) increase contrast, higher values (60-80dB) show subtle differences
📌 Remember: DEPTH mnemonic for systematic optimization - Depth adjustment first, Examine gain settings, Position focus appropriately, Tune frequency selection, Harmonize TGC curve. Follow this sequence for consistent image quality across all applications.
| Control Parameter | Primary Effect | Adjustment Range | Clinical Impact | Optimization Goal | Common Errors |
|---|---|---|---|---|---|
| Overall Gain | Signal amplification | 0-100% | Image brightness | Just below noise | Over-amplification |
| TGC Curve | Depth compensation | Variable by depth | Uniform echogenicity | Exponential increase | Irregular curve |
| Frequency | Penetration/resolution | 2-15 MHz | Image quality | Match to depth | Wrong frequency |
| Focus Position | Beam concentration | Adjustable depth | Lateral resolution | At target level | Misplaced focus |
| Dynamic Range | Contrast sensitivity | 40-80 dB | Tissue differentiation | Clinical need | Extreme settings |
💡 Master This: Harmonic imaging uses fundamental frequency transmission with harmonic frequency reception (typically 2x fundamental). This technique reduces near-field artifacts by >80% and improves contrast resolution by 30-40%, particularly valuable for cardiac and abdominal imaging.
Connect these optimization principles through probe selection strategies to understand how systematic control manipulation enables consistent diagnostic quality across diverse perioperative applications.
🎛️ Machine Mastery: The Control Center Architecture
🔍 Probe Selection Mastery: The Precision Instrument Arsenal
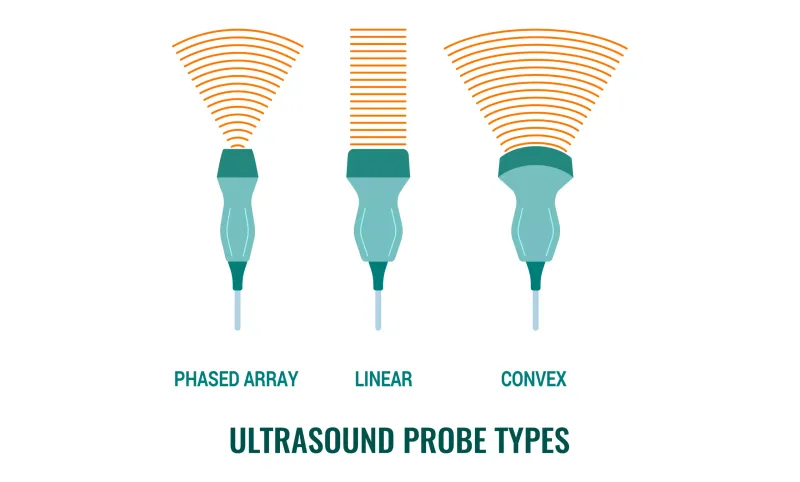
Understanding probe-anatomy relationships enables systematic selection based on target depth, field of view requirements, and resolution needs. Each transducer design optimizes specific acoustic characteristics for defined clinical applications.
-
Linear Array Transducers
- Frequency range: 5-15 MHz (high resolution applications)
- Field of view: Rectangular with parallel beam lines
- Optimal depth: 2-6cm (superficial structures)
- Vascular access: 10-15 MHz for vessel visualization <3cm depth
- Nerve blocks: 8-12 MHz for nerve identification and needle guidance
- Airway assessment: 5-10 MHz for tracheal and vocal cord imaging
- Footprint: 25-50mm length provides wide field for linear structures
-
Curved Array Transducers
- Frequency range: 2-8 MHz (penetration-optimized)
- Field of view: Sector with diverging beam pattern
- Optimal depth: 8-25cm (deep abdominal structures)
- Abdominal imaging: 2-5 MHz for organ visualization >10cm depth
- Gastric assessment: 3-6 MHz for antral cross-sectional area
- Renal evaluation: 2-5 MHz for kidney and bladder imaging
- Footprint: 40-60mm radius enables wide sector coverage
📌 Remember: FLAP mnemonic for probe selection - Frequency matches depth, Linear for superficial, Array type determines field, Phased for cardiac. Linear arrays for <6cm, curved arrays for >8cm, phased arrays for cardiac windows.
| Probe Type | Frequency Range | Optimal Depth | Field of View | Primary Applications | Resolution (mm) |
|---|---|---|---|---|---|
| High-freq Linear | 10-15 MHz | 1-4cm | Rectangular | Vascular access, superficial | <0.5 |
| Mid-freq Linear | 5-10 MHz | 3-8cm | Rectangular | Regional anesthesia, airway | 0.5-1.5 |
| Low-freq Linear | 3-7 MHz | 5-10cm | Rectangular | Neuraxial, deep vessels | 1-2 |
| Curved Array | 2-8 MHz | 8-25cm | Sector | Abdominal, cardiac (suboptimal) | 1-3 |
| Phased Array | 1-5 MHz | 10-20cm | Sector | Cardiac, thoracic | 2-4 |
- Phased array transducers: 1-5 MHz for cardiac imaging
- Small footprint: 15-25mm for intercostal access
- Sector scanning: 60-90 degree field enables cardiac windows
- Transthoracic echo: 2-4 MHz through intercostal spaces
- Lung assessment: 2-5 MHz for pleural and lung surface
- Hemodynamic evaluation: Doppler capability for flow assessment
⭐ Clinical Pearl: Probe-skin coupling requires >95% contact area for optimal transmission. Gel quantity should create thin, uniform layer without air bubbles. Pressure application should be firm but not compressive to avoid vessel collapse or tissue distortion.
💡 Master This: Probe orientation follows universal conventions - indicator dot corresponds to screen left for transverse views, screen top for longitudinal views. Consistent orientation prevents anatomical confusion and enables reproducible imaging across operators and institutions.
Connect these probe selection principles through systematic imaging protocols to understand how transducer optimization enables application-specific diagnostic excellence in perioperative settings.
🔍 Probe Selection Mastery: The Precision Instrument Arsenal
⚡ Clinical Integration Mastery: The Decision Algorithm Engine
Understanding protocol-driven integration enables systematic assessment that reduces diagnostic uncertainty while improving clinical outcomes. Each application follows evidence-based pathways with defined decision points and quantitative thresholds.
-
Hemodynamic Assessment Protocol
- Step 1: Left ventricular function (parasternal long axis)
- Step 2: Volume status (IVC diameter and collapsibility)
- Step 3: Right heart evaluation (RV size, TR velocity)
- EF estimation: >55% normal, 40-55% mild dysfunction, <40% significant
- IVC assessment: <2.1cm with >50% collapse suggests hypovolemia
- RV/LV ratio: >0.6 indicates RV dysfunction or pulmonary hypertension
- Decision timeline: Complete assessment within 5-8 minutes
-
Respiratory Assessment Integration
- Pneumothorax detection: Absent lung sliding with absent B-lines
- Pulmonary edema: ≥3 B-lines per intercostal space bilaterally
- Pleural effusion: Anechoic collection above diaphragm
- Sensitivity: >95% for pneumothorax vs <70% for chest X-ray
- Specificity: >90% for pulmonary edema with B-line quantification
- Clinical impact: 40-60% reduction in unnecessary procedures
📌 Remember: SHOCK mnemonic for hemodynamic POCUS - Systolic function (EF), Heart rate and rhythm, Obstruction (tamponade), Contractility assessment, Kinetic evaluation (wall motion). Systematic evaluation within <10 minutes guides immediate management.
| Clinical Scenario | POCUS Protocol | Key Measurements | Decision Threshold | Management Change | Outcome Improvement |
|---|---|---|---|---|---|
| Hypotension | Cardiac + IVC | EF, IVC diameter | EF <40% or IVC >2.5cm | Inotropes vs fluids | 35% faster resolution |
| Dyspnea | Lung + cardiac | B-lines, EF | ≥3 B-lines bilateral | Diuretics vs bronchodilators | 50% diagnostic accuracy |
| Chest Pain | Cardiac focused | Wall motion, EF | Regional WMA | Cardiology consult | 25% faster diagnosis |
| Shock | Comprehensive | Multiple parameters | Protocol-driven | Targeted therapy | 40% mortality reduction |
- Central venous access: Real-time needle visualization
- Arterial cannulation: Vessel identification and guidance
- Neuraxial procedures: Anatomical landmark identification
- Success rates: >95% first-pass with ultrasound guidance
- Complication reduction: 60-80% decrease in mechanical complications
- Time efficiency: 30-50% reduction in procedure time
⭐ Clinical Pearl: Multi-organ POCUS protocols demonstrate additive diagnostic value - cardiac + lung assessment provides >90% diagnostic accuracy for undifferentiated dyspnea compared to <70% for individual organ assessment.
💡 Master This: POCUS-guided fluid management using IVC assessment reduces fluid overload by >40% while maintaining hemodynamic stability. Dynamic parameters (IVC collapsibility >50% predicts fluid responsiveness with >85% accuracy in mechanically ventilated patients.
Connect these integration protocols through advanced applications to understand how systematic POCUS transforms perioperative decision-making into precision-guided patient care.
⚡ Clinical Integration Mastery: The Decision Algorithm Engine
🚀 Advanced Applications: The Cutting-Edge Integration Matrix
Understanding advanced integration enables predictive medicine where ultrasound data anticipates clinical deterioration before traditional monitoring detects changes. These applications represent the evolution from reactive to proactive perioperative care.
-
Artificial Intelligence Integration
- Automated EF calculation: ±5% accuracy compared to expert interpretation
- Real-time image optimization: Machine learning adjusts gain/TGC automatically
- Pattern recognition: AI algorithms detect subtle abnormalities missed by human observation
- Diagnostic speed: <30 seconds for comprehensive cardiac assessment
- Accuracy improvement: 15-20% increase in diagnostic precision
- Training acceleration: 50% reduction in competency development time
- Quality standardization: >95% consistency across operator skill levels
-
Multi-Parametric Monitoring
- Continuous cardiac output: Beat-to-beat hemodynamic tracking
- Respiratory mechanics: Real-time lung recruitment monitoring
- Fluid responsiveness: Dynamic prediction of volume requirements
- Stroke volume variation: >12% predicts fluid responsiveness (>90% accuracy)
- Lung ultrasound score: Quantitative B-line assessment for ARDS progression
- Integrated hemodynamics: Cardiac + vascular + pulmonary comprehensive evaluation
📌 Remember: SMART mnemonic for advanced POCUS - Synthetic intelligence integration, Multi-parametric monitoring, Automated analysis, Real-time optimization, Telemedicine connectivity. These technologies transform POCUS from diagnostic tool to intelligent monitoring system.

| Advanced Application | Technology Integration | Diagnostic Enhancement | Clinical Impact | Implementation Timeline | Cost-Benefit Ratio |
|---|---|---|---|---|---|
| AI-Assisted Imaging | Machine learning algorithms | 20% accuracy improvement | Standardized interpretation | 2-3 years | 3:1 ROI |
| Telemedicine POCUS | Remote expert consultation | >90% diagnostic concordance | Rural/resource-limited access | 1-2 years | 5:1 ROI |
| Wearable Integration | Continuous monitoring | Real-time trend analysis | Early deterioration detection | 3-5 years | 4:1 ROI |
| Robotic Guidance | Automated probe positioning | <1mm positioning accuracy | Procedure standardization | 5-7 years | 2:1 ROI |
- Expert consultation: Real-time specialist interpretation from remote locations
- Training support: Virtual mentorship for skill development
- Quality assurance: Centralized review of critical studies
- Diagnostic concordance: >90% agreement between on-site and remote interpretation
- Access expansion: Rural hospitals gain specialist expertise within <15 minutes
- Training efficiency: Virtual supervision reduces learning curve by 40%
- Predictive Analytics Integration
- Risk stratification: Machine learning models predict complications 24-48 hours in advance
- Outcome optimization: Algorithm-guided interventions improve patient outcomes
- Resource allocation: Predictive models optimize staffing and equipment utilization
- Complication prediction: >80% accuracy for major adverse events
- Length of stay: 15-25% reduction through optimized care pathways
- Cost reduction: >30% decrease in unnecessary interventions
⭐ Clinical Pearl: Blockchain integration enables secure, immutable POCUS data sharing across healthcare networks, facilitating longitudinal patient tracking and multi-institutional research while maintaining HIPAA compliance and data integrity.
💡 Master This: Augmented reality (AR) overlay systems project ultrasound images directly onto patient anatomy, enabling real-time needle guidance with <2mm accuracy for complex procedures. This technology reduces procedure time by >40% while improving first-pass success rates to >98%.
Connect these advanced applications through rapid mastery frameworks to understand how next-generation POCUS transforms perioperative medicine into predictive, personalized, precision healthcare.
🚀 Advanced Applications: The Cutting-Edge Integration Matrix
🎯 Rapid Mastery Arsenal: Your Clinical Excellence Toolkit
Understanding accelerated learning principles enables efficient skill acquisition through deliberate practice and systematic progression. These frameworks optimize training time while ensuring comprehensive competency across all perioperative applications.
- Essential Numbers Arsenal
- Normal EF: >55% (mild dysfunction 40-55%, severe <40%)
- IVC diameter: <2.1cm (hypovolemia), >2.5cm (hypervolemia)
- B-line threshold: ≥3 per space (pulmonary edema)
- Pneumothorax sensitivity: >95% (absent lung sliding)
- Cardiac output normal: 4-8 L/min (2.5-4.0 L/min/m² indexed)
- RV/LV ratio: <0.6 normal, >1.0 severe RV dysfunction
- TR velocity: <2.8 m/s normal, >3.4 m/s severe pulmonary hypertension
📌 Remember: MASTER mnemonic for rapid competency - Measurement accuracy, Anatomical recognition, Systematic protocols, Technical optimization, Error recognition, Rapid interpretation. 100 supervised scans minimum for basic competency, 300 scans for advanced proficiency.
| Competency Level | Scan Volume | Time to Proficiency | Accuracy Threshold | Clinical Applications | Supervision Required |
|---|---|---|---|---|---|
| Novice | 0-25 scans | 2-4 weeks | >70% accuracy | Basic views only | Direct supervision |
| Competent | 25-100 scans | 6-12 weeks | >85% accuracy | Standard protocols | Available supervision |
| Proficient | 100-300 scans | 3-6 months | >90% accuracy | Complex cases | Consultation available |
| Expert | >300 scans | 6-12 months | >95% accuracy | All applications | Independent practice |
- FALLS protocol: <5 minutes comprehensive assessment
- RUSH protocol: <8 minutes shock evaluation
- BLUE protocol: <3 minutes dyspnea assessment
- Time efficiency: Structured protocols reduce assessment time by >50%
- Diagnostic yield: Protocol adherence improves accuracy by >30%
- Error reduction: Systematic approach decreases missed findings by >60%
⭐ Clinical Pearl: Simulation-based training accelerates skill acquisition by 40-60% compared to traditional apprenticeship. High-fidelity simulators enable deliberate practice of rare complications and emergency scenarios without patient risk.
💡 Master This: Competency maintenance requires minimum 50 scans per quarter to preserve proficiency levels. Skills decay begins after >6 weeks without practice, with >20% accuracy decline after 3 months of non-use.
This comprehensive POCUS mastery framework transforms perioperative ultrasound from basic imaging to advanced diagnostic capability, enabling evidence-based decision-making that improves patient outcomes while optimizing healthcare delivery in modern surgical environments.
🎯 Rapid Mastery Arsenal: Your Clinical Excellence Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























