Temperature Regulation in Children - Why Kids Chill Fast
Children are prone to hypothermia under anesthesia due to:
- ↑ Body Surface Area to Mass Ratio: Larger than adults, promoting rapid heat loss to the environment.
- ↓ Thermal Insulation:
- Thinner skin.
- Less subcutaneous fat, especially premature infants.
- Immature Thermoregulatory System:
- Shivering is poorly developed/absent in neonates.
- Neonates rely on non-shivering thermogenesis (NST) in brown fat.
- Anesthetic-Induced Impairment:
- Vasodilation: Redistributes core heat peripherally.
- Inhibition of shivering.
- Hypothalamic thermoregulatory depression.
- Higher Basal Metabolic Rate: Generates more heat/kg, but losses often exceed production.
⭐ Neonates lose heat approximately 4 times faster than adults; vigilant temperature monitoring is essential.
Temperature Regulation in Children - The Heat Thieves
- Children lose heat rapidly via four main "thieves":
- Radiation (40-60%): To cooler objects not in direct contact (e.g., OR walls). Largest source.
- Convection (15-30%): To air currents (e.g., OR ventilation, drafts).
- Evaporation (20-25%): From skin, respiratory tract, open wounds. ↑ with ↓ humidity.
- Conduction (3-5%): Via direct contact with cooler surfaces (e.g., OR table, cold fluids).
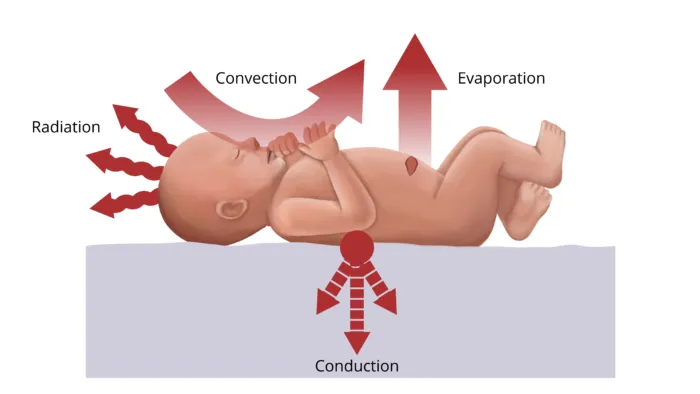
⭐ Radiation is the predominant mechanism of heat loss in infants and children in the operating room.
Temperature Regulation in Children - The Icy Impact
- Children, especially neonates, are highly susceptible to hypothermia (core temp < 36°C).
- Reasons: Large surface area to mass ratio, thin subcutaneous fat, immature thermoregulation, limited shivering.
- Neonates: Rely on Non-Shivering Thermogenesis (NST) in Brown Adipose Tissue (BAT) for heat.
- Major Heat Loss Mechanisms (📌 CCRE):
- Radiation: To cooler OR environment (largest, ~40-60%).
- Convection: Air currents over skin (~15-30%).
- Evaporation: From skin, respiratory tract (~20%).
- Conduction: Direct contact with cold surfaces (~5%).
- Consequences of Hypothermia:
- Delayed emergence, ↑ O₂ demand (shivering).
- Coagulopathy, ↑ surgical site infections.
- Cardiac irritability, metabolic acidosis.
- Prevention Strategies:
- Ambient OR temp: 23-25°C for infants, 21°C for children.
- Forced-air warming devices.
- Warmed IV fluids & inspired gases.
- Minimize exposure; use head coverings.
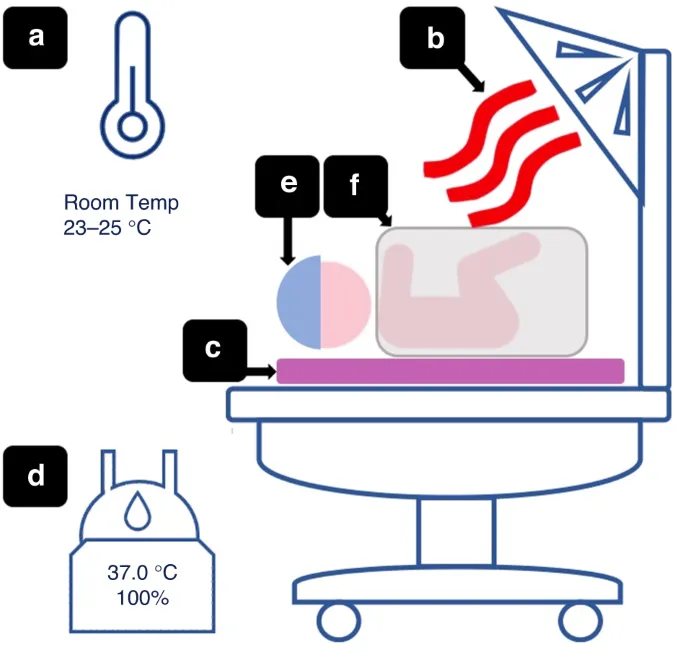
⭐ Volatile anesthetics and opioids can significantly impair non-shivering thermogenesis (NST) in neonates by inhibiting brown adipose tissue (BAT) function, making active warming crucial.
Temperature Regulation in Children - Stay Warm, Stay Safe
- Infants & children: prone to hypothermia (core temp < 36°C) due to:
- Large surface area to volume ratio.
- Less subcutaneous fat; limited shivering.
- Immature thermoregulatory center.
- Heat Loss Mechanisms: Radiation (major), Convection, Evaporation, Conduction. (📌 RCEC)
- Adverse Effects: ↑O₂ consumption, delayed emergence, coagulopathy, wound infection, cardiac events.
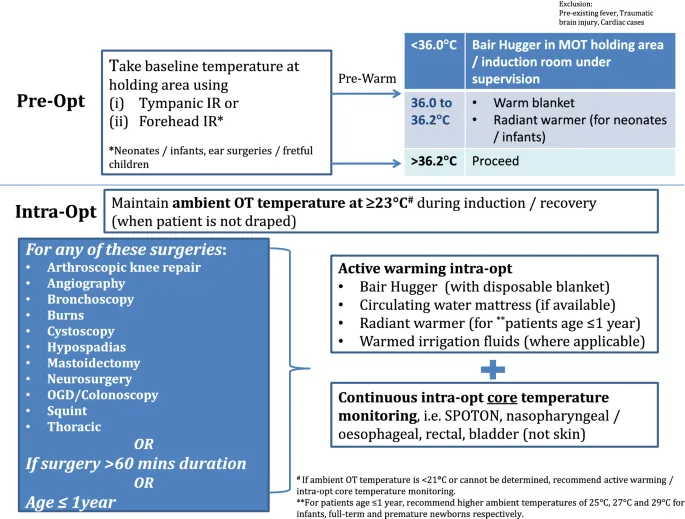
- Prevention & Management:
- Ambient OR temp: 23-25°C (infants), 21°C (children).
- Forced-air warmers, warmed IV fluids (37°C), radiant warmers.
- Active airway heating & humidification.
- Continuous core temperature monitoring (esophageal, rectal).
⭐ Non-shivering thermogenesis in neonates occurs in brown adipose tissue (BAT) but is rapidly depleted.
High‑Yield Points - ⚡ Biggest Takeaways
- Infants are prone to hypothermia: large surface area/volume ratio, ↓ fat, immature thermoregulation.
- Non-shivering thermogenesis (NST) in brown fat is primary neonatal heat source, blunted by anesthesia.
- Anesthetics impair thermoregulation, causing vasodilation & ↓ metabolic rate, promoting heat loss.
- Hypothermia complications: delayed recovery, ↑O₂ consumption, coagulopathy, cardiac events, ↑infection risk.
- Prevention: pre-warming, forced-air warmers, warmed IV fluids, ↑ambient temperature, minimize exposure.
- Malignant Hyperthermia (MH): rare, critical hyperthermic emergency triggered by specific anesthetic agents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

