Intro & Benefits - Tiny Patients, Big Relief
- Pediatric Regional Anesthesia (RA): Precise local anesthetic placement near nerves for targeted analgesia/anesthesia in children, enhancing perioperative care.
- Key Benefits:
- Reduced General Anesthesia (GA) requirement.
- Superior postoperative analgesia.
- ↓ Opioid consumption & related side effects (e.g., PONV, respiratory depression).
- Faster recovery & earlier hospital discharge.
- Attenuates surgical stress response.
- Versatile: sole anesthetic or GA adjunct.
⭐ Regional anesthesia significantly reduces postoperative apnea risk in former preterm infants < 60 weeks post-conceptual age undergoing surgery (a critical exam point).
Anatomy & Physiology - Little Bodies, Different Blocks
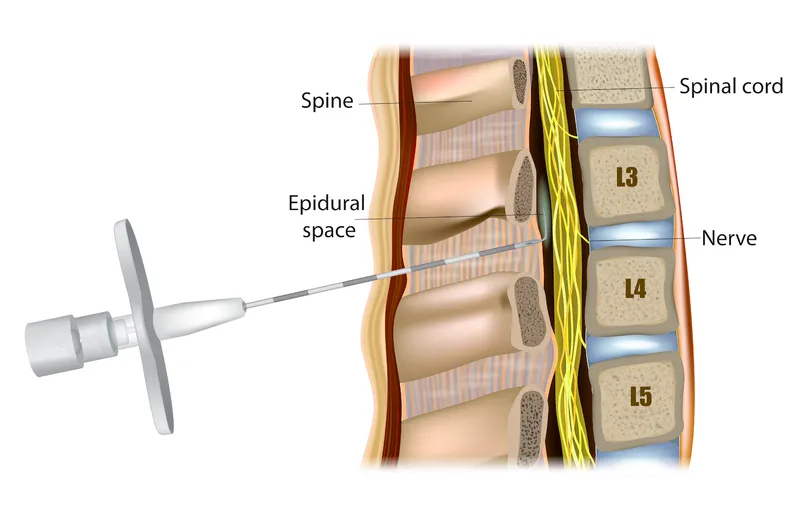
- Spinal Cord: Ends L3 (neonates), L1 (adults).
- Dura Mater: Thinner, ↑permeable → faster LA onset.
- Epidural Space: ↓fat, ↑vascularity → ↑systemic absorption.
- CSF Volume: Larger (neonate 4 ml/kg vs adult 2 ml/kg) → may need ↑spinal dose/kg.
- Nerves: Myelination incomplete → faster onset, shorter duration.
- Drug Handling: Immature liver, ↓protein binding → ↑free drug.
⭐ Neonatal spinal cord ends at L3; adult at L1. Crucial for safe needle placement.
 oka
oka
Common Blocks - Numbing Nuggets for Neonates

- Caudal Block: Most common. Simple, effective.
- Landmark: Sacral hiatus.
- Drugs: Bupivacaine 0.125-0.25%; Ropivacaine 0.2%.
- Volume: 0.5-1.0 mL/kg (sacro-lumbar), 1.0-1.25 mL/kg (lower thoracic).
- Uses: Sub-umbilical surgeries (hernia, circumcision).
- ⚠️ Risks: Intravascular injection, dural puncture.
- Epidural Anesthesia (Lumbar/Thoracic):
- Single shot or continuous catheter.
- Test dose (with epinephrine) vital.
- ↑ dural puncture risk in neonates.
- Major Peripheral Nerve Blocks (PNBs):
- Femoral, sciatic, axillary brachial plexus.
- Ultrasound guidance (USG) standard for safety & efficacy.
- ↓ drug volumes vs central blocks.
⭐ Caudal block is the most frequently performed regional anesthetic technique in children.
Pharmacology & Toxicity - Safe Sips, Serious Risks
- LAs (Max Doses): Crucial: accurate weight-based dosing.
- Bupivacaine: 2-2.5 $mg/kg$
- Ropivacaine: 2-3 $mg/kg$ (often preferred due to ↓ cardiotoxicity)
- Lidocaine (c̄ epi): 5-7 $mg/kg$
- Adjuvants: Enhance block quality/duration.
- Clonidine: 1-2 $mcg/kg$
- Dexmedetomidine: 0.5-1 $mcg/kg$
- LAST (Local Anesthetic Systemic Toxicity):
- ⚠️ Early: Tinnitus, metallic taste, perioral numbness. Late: Seizures, arrhythmias, cardiac arrest.
- Management Protocol:
> ⭐ In LAST, 20% Lipid Emulsion: Bolus **1.5** $mL/kg$ (repeat if needed), then infuse **0.25** $mL/kg/min$ (max total **10-12** $mL/kg$).
Techniques & Tech - Precision Pointers for Peds
- Ultrasound Guidance (USG): Gold standard for real-time visualization. Improves success, ↓ complications.
- Nerve Stimulators: Adjunct to USG or for specific blocks. Elicit motor response at <0.5 mA.
- Needles: Short-bevel, echogenic tips for better US visibility. Size appropriate for age/block.
- Catheters: For continuous infusions, prolonging analgesia.
- Safety First: Test dose, incremental injection, frequent aspiration.

⭐ USG significantly reduces local anesthetic systemic toxicity (LAST) risk in children compared to landmark techniques.
Complications & Fixes - Oopsies & Ounces of Prevention
- LAST (Local Anesthetic Systemic Toxicity):
- Prevent: Max dose (Bupivacaine 2-2.5 mg/kg), ultrasound, test dose.
- Treat: Lipid emulsion (Intralipid 20%: 1.5 mL/kg bolus).
- Nerve Injury: Ultrasound guidance, avoid paresthesia/high pressure.
- Hematoma: Assess coagulation status.
- Infection: Strict aseptic technique.
- Block Failure: Ultrasound confirmation, have backup plan.
⭐ In children, LAST often presents with agitation/seizures, potentially lacking classic adult prodromal symptoms (e.g., tinnitus, metallic taste).
High‑Yield Points - ⚡ Biggest Takeaways
- Caudal block is the most common pediatric regional technique, ideal for infraumbilical procedures.
- Higher risk of Local Anesthetic Systemic Toxicity (LAST) due to immature hepatic metabolism and ↓ plasma protein binding.
- Epinephrine (1:200,000) addition prolongs analgesia and reduces systemic absorption of local anesthetics.
- Accurate dose calculation (mg/kg) is critical; strictly adhere to maximum recommended doses.
- Ultrasound guidance is standard, enhancing success and safety by visualizing neural structures and spread.
- Key contraindications include coagulopathy, local infection, parental refusal, and known allergy to agents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

