Pediatric Fluid Physiology - Tiny Tot Hydration
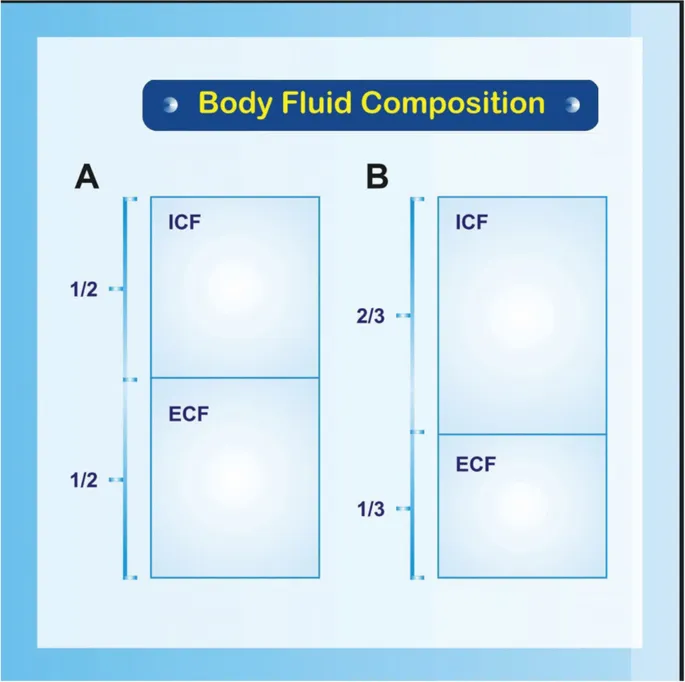
- Body Water: Higher Total Body Water (TBW) in pediatrics (Neonate 75-80%, Preterm up to 85%). Extracellular Fluid (ECF) is ~45% of body weight (Adult ~20%), contracts rapidly postnatally.
- Physiological Factors:
- ↑ Basal Metabolic Rate (BMR).
- ↑ Surface Area to Volume ratio → ↑ Insensible water losses (skin, respiratory).
- Renal Immaturity:
- ↓ Glomerular Filtration Rate (GFR) at birth; reaches adult levels by 1-2 years.
- Limited urine concentrating and diluting capacity.
- Potential for Na⁺ wasting, especially in preterm infants.
- Maintenance Fluid Calculation (📌 4-2-1 Rule):
- $0-10 \text{ kg: } 4 \text{ mL/kg/hr}$
- $10-20 \text{ kg: } +2 \text{ mL/kg/hr for this portion}$
- $>20 \text{ kg: } +1 \text{ mL/kg/hr for this portion}$
⭐ Neonates are obligate glucose consumers; hypoglycemia can occur quickly with inadequate intake, often coexisting with dehydration.
 )
)
Preoperative Fasting & Deficits - Empty Tummy Rules
- NPO Guidelines (📌 "2-4-6-8" Rule):
- Clear liquids (water, clear juice): 2 hrs
- Breast milk: 4 hrs
- Infant formula: 6 hrs
- Light meal (toast, milk): 6 hrs
- Heavy/Fried meal: 8 hrs
- Fluid Deficit Calculation:
- Maintenance (4-2-1 Rule):
- First 0-10 kg: $4$ ml/kg/hr
- Next 10-20 kg: $2$ ml/kg/hr
- Above 20 kg: $1$ ml/kg/hr
- Deficit = Total Hourly Maintenance × Fasting Hours
- Replace: 50% in 1st hr, 25% in 2nd hr, 25% in 3rd hr.
- Maintenance (4-2-1 Rule):
⭐ Prolonged fasting beyond guidelines offers no added safety, risking hypoglycemia and dehydration, especially in neonates and infants.
Intraoperative Fluid Management - In-Op Juice Juggling
- Goal: Maintain euvolemia, electrolyte & glucose balance.
- Maintenance (📌 4-2-1 Rule):
- $0-10 \text{ kg}$: 4 mL/kg/hr
- $11-20 \text{ kg}$: 2 mL/kg/hr
- $>20 \text{ kg}$: 1 mL/kg/hr
- Use isotonic crystalloids (RL, Plasmalyte).
- Deficit Replacement (NPO): (Maintenance rate × NPO hours). Give 50% in 1st hr, 25% in 2nd, 25% in 3rd.
- Ongoing Losses:
- Third space: 1-10 mL/kg/hr (surgery-dependent).
- Minimal trauma: 1-3 mL/kg/hr
- Moderate trauma: 3-7 mL/kg/hr
- Major trauma: 7-10 mL/kg/hr
- Blood loss: Replace 3:1 with crystalloid, 1:1 with colloid/blood.
- Third space: 1-10 mL/kg/hr (surgery-dependent).
- Monitoring: Urine output (1-2 mL/kg/hr), vitals.
- Glucose: Neonates/infants may need dextrose in IVF (Target GIR 4-6 mg/kg/min).
⭐ Neonates have limited renal concentrating ability; careful to avoid fluid overload.
Fluid Choices & Monitoring - Potion Selection & Watchful Eyes
Fluid Selection:
- Crystalloids (Go-to):
- Isotonic (Bolus/Deficit): Ringer's Lactate (RL), Normal Saline (NS, 0.9% NaCl). Bolus: 10-20 ml/kg.
- Maintenance (Holliday-Segar formula based):
- Neonates: D5 0.2% NaCl + 20 mEq/L KCl.
- Children: D5 0.45% NaCl + 20 mEq/L KCl.
- Limit intraop dextrose unless specific risk (e.g., neonates, prolonged fasting, <6 months old).
- Colloids (e.g., Albumin 5%): For significant protein loss or large volume resuscitation if crystalloids are insufficient.
Watchful Eyes (Monitoring):
- Key Vitals: Heart Rate (HR), Blood Pressure (BP) (age-appropriate cuff), Capillary Refill Time (CRT) (<2 sec).
- Urine Output (UOP): Target >1-2 ml/kg/hr.
- Labs: Hematocrit (Hct), glucose, electrolytes as clinically indicated.
⭐ Neonates are particularly susceptible to hypoglycemia and hyponatremia. Maintenance fluids should typically contain glucose (e.g., D5 or D10) and appropriate sodium (e.g., 0.2% NaCl).
High‑Yield Points - ⚡ Biggest Takeaways
- Maintenance fluids calculated by Holliday-Segar (4/2/1 rule).
- Neonates: limited renal concentration, ↑ insensible losses.
- Hypoglycemia risk is high; monitor glucose, consider dextrose-containing fluids for maintenance in neonates/infants.
- Prefer isotonic crystalloids (NS, RL) intraoperatively; avoid hypotonic solutions.
- Blood volume: Neonates 85-90 mL/kg, Infants 80 mL/kg, Children 70-75 mL/kg.
- Replace third-space losses judiciously.
- Monitor closely for fluid overload due to small circulatory volume and immature kidneys.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

