Anesthesia for Common Pediatric Surgeries: Pre-op - Tiny Patient Prep
- Preoperative Assessment:
- Hx: Birth (prematurity, IUGR), congenital anomalies (cardiac/airway), prev. anesthesia Hx, allergies, meds, recent URI (symptoms, duration, severity).
- Exam: Airway (Mallampati, tonsils, loose teeth, neck), CVS (murmurs), RS (wheeze, SpO2), hydration.
- Labs: Hb baseline; Type & screen for major surgery. Specific tests if co-morbidities.
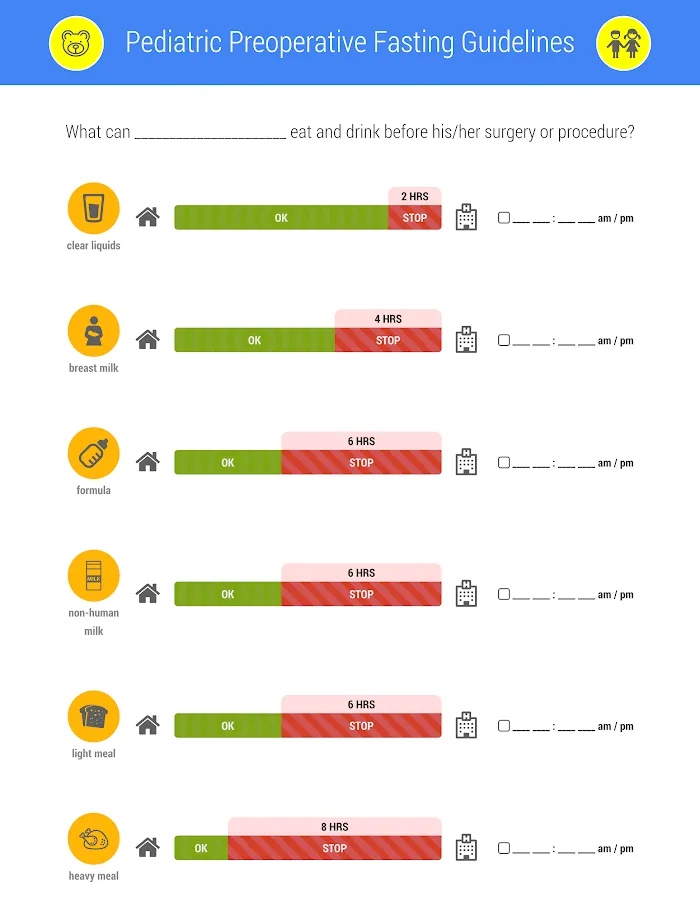
- Fasting (NPO) Guidelines: (📌 "2-4-6 Clear Breast Formula")
- Clear fluids (water, pulp-free juice): 2h
- Breast milk: 4h
- Infant formula, non-human milk, light meal: 6h
- Premedication:
- Goals: ↓Anxiety, smooth separation/induction, antisialagogue.
- Common: Oral Midazolam 0.25-0.5 mg/kg (max 15-20 mg); IN Dexmedetomidine 1-2 mcg/kg.
- Parental Presence at Induction (PPAI) can ↓anxiety.
⭐ Children with an active or recent URI (within 2-4 weeks) have a 2-7 fold ↑ risk of respiratory adverse events like laryngospasm or bronchospasm.
Anesthesia for Common Pediatric Surgeries: Intraoperative - Airway Adventures Tiny Tactics
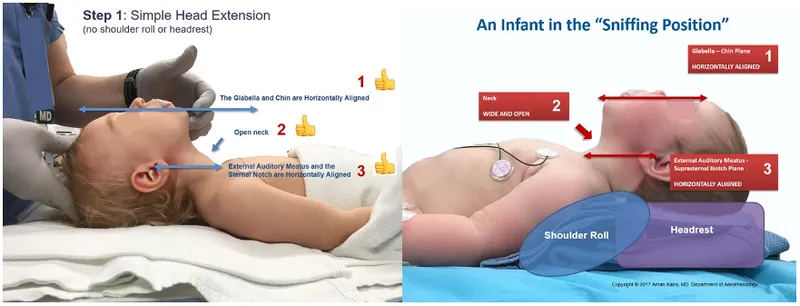
- Airway Arsenal:
- Masks: Anatomical, transparent (e.g., Rendell-Baker Soucek).
- Blades: Miller (0-1 for neonate/infant, 2 for child), Macintosh (2-3 for child), Wis-Hipple.
- ETT: Uncuffed (traditionally <8 yrs) size $ (Age/4) + 4 $; Depth $ ETT \text{ size (ID mm)} \times 3 $ or $ (Age/2) + 12 $ cm. Cuffed: size $ (Age/4) + 3.5 $.
- SGA: LMA (size by weight, e.g., Size 1 <5kg, 1.5 5-10kg, 2 10-20kg), i-gel.
- Induction & RSI:
- Inhalational: Sevoflurane (smooth, rapid, preferred).
- IV: Propofol (2.5-3.5 mg/kg), Ketamine (1-2 mg/kg IV, 4-6 mg/kg IM).
- RSI: For aspiration risk. Pre-O2, cricoid pressure (Sellick's), rapid induction agent + NMB (Suxamethonium 1-2 mg/kg IV or Rocuronium 1.2 mg/kg IV).
- Maintenance:
- Volatiles (Sevoflurane, Isoflurane) or TIVA.
- Opioids (Fentanyl 1-2 mcg/kg). NMBs (Atracurium, Rocuronium) - dose adjust for age.
- Laryngospasm Management:
- Identify: Inspiratory stridor, "ball-valve" obstruction, ↓SaO2, absent EtCO2.
- Treat: 100% O2, CPAP, deepen anesthesia, Larson's maneuver, Suxamethonium (0.1-1 mg/kg IV or 4 mg/kg IM).
- 📌 LPS (Laryngospasm Point Stimulation) for Larson's maneuver.
- Monitoring:
- Standard ASA: ECG, NIBP, SpO2, Temperature (core & peripheral).
- Precordial/esophageal stethoscope.
- Capnography (EtCO2): Gold standard for ETT placement & continuous ventilation monitoring.
⭐ For cuffed ETTs in children, ensure cuff pressure is maintained <20-25 cm H2O to prevent tracheal mucosal ischemia and post-extubation stridor. Microcuff ETTs are increasingly preferred.
Anesthesia for Common Pediatric Surgeries: Specific Cases & Post-Op - Surgical Spotlights Ouchless Outcomes
- Tonsillectomy & Adenoidectomy (T&A):
- Airway: Shared; risk of obstruction, bleeding. Consider oral RAE tube.
- Extubation: Fully awake, lateral position to prevent aspiration.
- Pain: Severe; multimodal (opioids e.g., fentanyl, NSAIDs e.g., ketorolac).
- Bleeding: Primary (<24h), Secondary (5-10d).
- Pyloromyotomy:
- Pre-op: Correct dehydration, hypokalemic hypochloremic metabolic alkalosis. 📌 Vomit K+Cl-
- Anesthesia: RSI (often with cricoid), avoid N₂O. Atropine for bradycardia.
- Post-op: Apnea/hypoglycemia watch. Test feed post-op.
- Inguinal Hernia Repair:
- Day-case common. LMA or ETT.
- Anesthesia: GA + regional (caudal, ilioinguinal/iliohypogastric block highly effective).
- Ex-premies (<60 wks PCA): ↑ Apnea risk, may need admission.

- Post-Op Care:
- Pain: Multimodal; age-specific scales (e.g., FLACC). Paracetamol, NSAIDs, opioids, regional.
- PONV: High risk. Prophylaxis: Ondansetron (0.1-0.15 mg/kg), Dexamethasone (0.15-0.5 mg/kg). Consider aprepitant.
- Emergence Delirium (ED): Common (sevoflurane). Prevent/treat: Dexmedetomidine, midazolam, propofol bolus.
⭐ In pyloric stenosis, surgery is deferred until fluid/electrolyte resuscitation is adequate, typically when serum chloride is >85 mEq/L and bicarbonate <30 mEq/L.
High‑Yield Points - ⚡ Biggest Takeaways
- Post-tonsillectomy hemorrhage: High risk within 24 hrs (primary) or 5-10 days (secondary); full stomach, difficult airway.
- Pyloric stenosis: Correct hypochloremic metabolic alkalosis pre-op; RSI with cricoid.
- TEF: Avoid PPV before fistula ligation; gastrostomy open to air.
- CDH: Gentle ventilation, avoid high PIP; preductal SpO2; delayed repair.
- Omphalocele/Gastroschisis: Cover defect (heat/fluid loss); RSI; monitor intra-abdominal pressure.
- Cleft lip/palate: Airway management crucial; RAE tube; post-op obstruction risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

