Pediatric Airway & Respiration - Tiny Passages, Big Impact
- Anatomical Differences (vs. Adult):
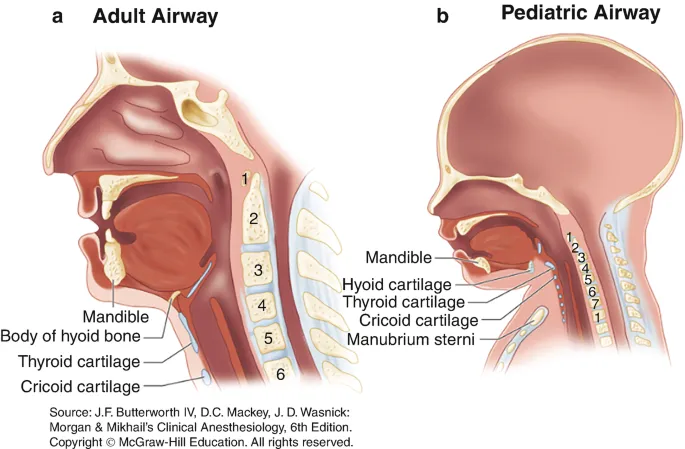
- Larynx: Higher (C3-C4), anterior, funnel-shaped.
- Epiglottis: Long, U/Ω-shaped, floppy.
- Tongue: Relatively larger, prone to obstruction.
- Cricoid Ring: Narrowest point < 5-8 yrs.
⭐ Cricoid cartilage is the narrowest part of the airway in children under 5-8 years.
- Trachea: Shorter (4-5 cm neonates), narrower, compliant.
- Nares: Small, easily obstructed.
- Physiological Differences:
- Obligate nose breathers (infants < 3-6 months). 📌 Mnemonic: "Infants Inhale Nasally."
- $VO_2$: ↑↑ ($6-8 \text{ mL/kg/min}$ vs $3-4$ adult).
- FRC: ↓ relative to $VO_2$; rapid desaturation.
- $V_T$: $6-8 \text{ mL/kg}$ (similar/kg to adults).
- RR: ↑ (Neonate: 30-60/min).
- Chest Wall: Compliant, ribs horizontal; diaphragmatic breathing, less efficient.
Pediatric Cardiovascular System - Little Hearts, Fast Rhythms
- Heart Rate (HR): Higher (Neonate: 120-160 bpm, Infant: 100-150 bpm), ↓ with age.
- Stroke Volume (SV): Relatively fixed in neonates; limited capacity to increase.
⭐ Neonatal cardiac output is primarily heart rate-dependent due to a fixed stroke volume.
- Cardiac Output (CO): Higher per kg body weight; $CO = HR \times SV$.
- Blood Pressure (BP): Lower (Neonate Systolic: 60-80 mmHg, Infant Systolic: 70-90 mmHg), ↑ with age.
- Myocardium:
- Less compliant (stiffer ventricles).
- Fewer contractile elements, more non-contractile tissue.
- Autonomic Control:
- Parasympathetic system (vagal tone) dominant at birth.
- Sympathetic innervation immature; blunted response to catecholamines.
- Blood Volume: Relatively larger (Neonate: 80-90 ml/kg; Infant: 75-80 ml/kg).
- Response to Hypoxia: Bradycardia (unlike adult tachycardia). 📌 Peds Brady Hypoxia.
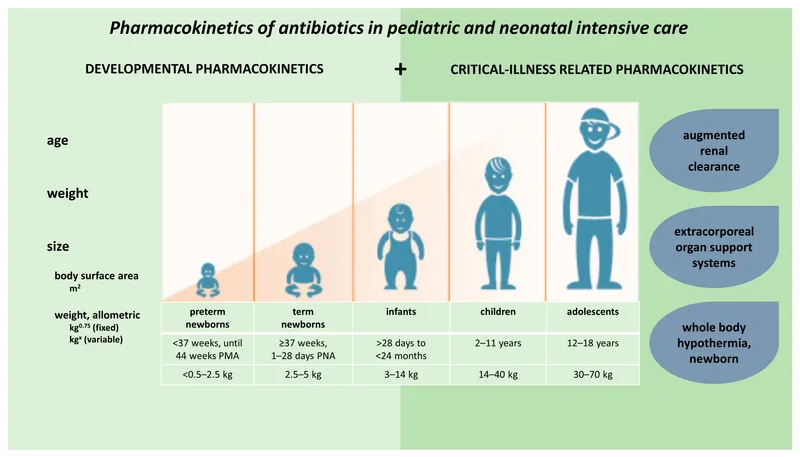
Pediatric Pharmacology - Small Bodies, Dose Adjustments
- Unique Pharmacokinetics (PK) & Pharmacodynamics (PD) in children.
- PK Differences:
- Body Composition: ↑ Total Body Water (TBW), ↓ fat → ↑ Volume of Distribution (Vd) for water-soluble drugs; ↓Vd for lipid-soluble drugs initially.
- Protein Binding: ↓ (e.g., albumin, alpha-1-acid glycoprotein) → ↑ free drug fraction.
- Hepatic Metabolism: Immature; enzyme activity (Phase I & II) varies with age. Glucuronidation ↓ in neonates.
- Renal Excretion: Immature (↓ Glomerular Filtration Rate (GFR), ↓ tubular function) → prolonged drug $t_{1/2}$ in neonates/infants.
- PD Differences:
- Altered receptor sensitivity and density (e.g., opioid receptors, neuromuscular junction).
⭐ Minimum Alveolar Concentration (MAC) for volatile anesthetics is highest in infants aged 1-6 months.
- Dosing Strategies:
- Primarily weight-based (mg/kg).
- Titrate to clinical effect; requires close monitoring.
- Age-specific adjustments are crucial due to organ maturation.
Key Systemic Differences - Warmth, Fluids & Nerves
- Thermoregulation (Warmth):
- Prone to rapid hypothermia: ↑ surface area/volume ratio, ↓ fat, ↓ shivering.
- Reliant on Non-Shivering Thermogenesis (NST) via brown fat.
- Hypothermia risks: ↑O2 consumption, acidosis, hypoglycemia.
⭐ Infants and neonates are prone to rapid hypothermia due to a large surface area-to-volume ratio and rely on non-shivering thermogenesis.

- Fluid & Renal Balance:
- ↑ Total Body Water (TBW) (70-80% neonates).
- Immature kidneys: GFR ~25% adult, matures by 1-2 yrs.
- Limited urine concentration/dilution; risk of dehydration/overload.
- Blood volume: Neonate 80-90 mL/kg.
- Nervous System:
- Immature CNS, permeable Blood-Brain Barrier (BBB).
- Incomplete myelination (until ~2 yrs).
- MAC peaks 1-6 months, then ↓.
- Spinal cord ends at L3 (neonates) vs L1 (adults).
High‑Yield Points - ⚡ Biggest Takeaways
- Airway: Larger tongue, anterior/cephalad larynx, omega-shaped epiglottis, cricoid narrowest point (subglottis).
- Respiratory: Higher O2 consumption, lower FRC, leading to rapid desaturation.
- Cardiovascular: HR-dependent cardiac output; bradycardia poorly tolerated; sensitive to vagal stimuli.
- Pharmacology: Larger Vd for water-soluble drugs; immature hepatic/renal function alters drug metabolism/excretion.
- Thermoregulation: Prone to hypothermia due to high surface area to volume ratio.
- Infants: Obligate nose breathers; higher closing volumes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

