PPTL Basics & Timing - Snip Snip Soon!
- PPTL: Permanent contraception post-childbirth.
- Optimal Timing:
- Post-vaginal: <48h (ideal 24h), up to 7 days if stable.
- During Cesarean section.
- Rationale for Early PPTL:
- High uterine fundus (umbilical level) → easy tubal access.
- Patient already in hospital.
- Ensures non-pregnant status.
- Essentials:
- Pre-labor informed consent crucial.
- Anesthesia: Regional (epidural/spinal) common.
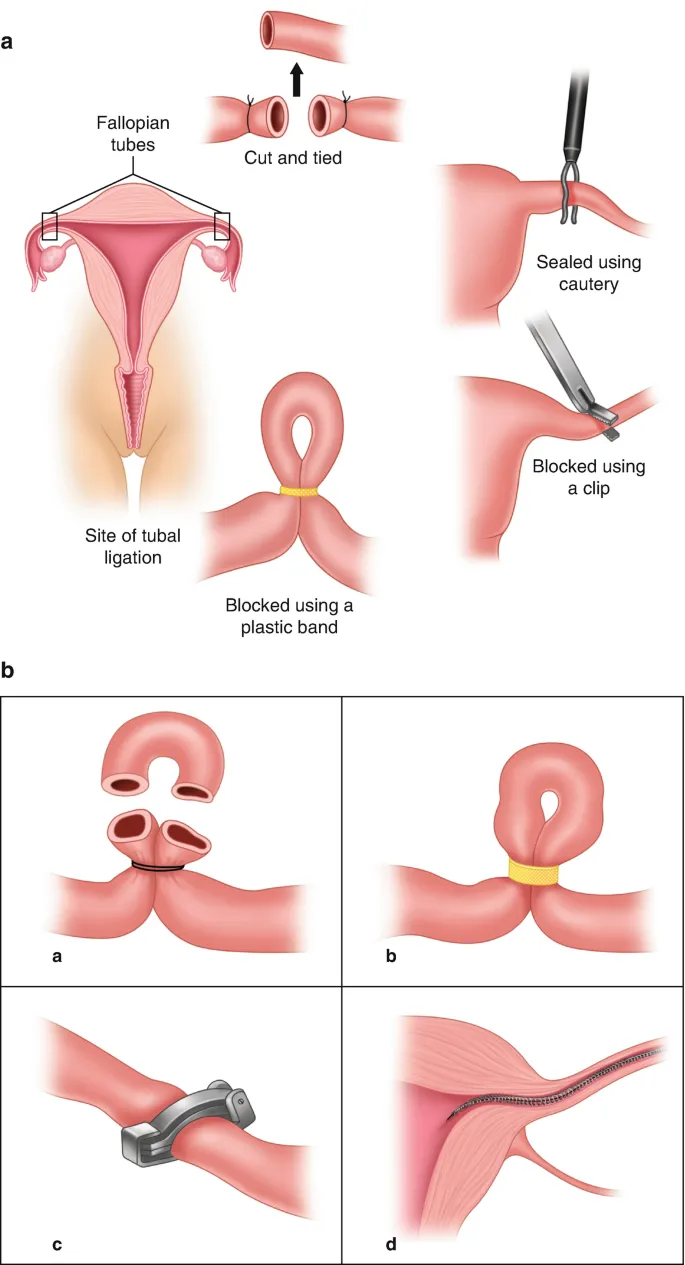
⭐ The ideal timing for postpartum tubal ligation is within 24-48 hours after vaginal delivery or at the time of Cesarean section, balancing patient recovery, uterine anatomy, and informed consent.
Postpartum Physiology - Mom's Body Quirks
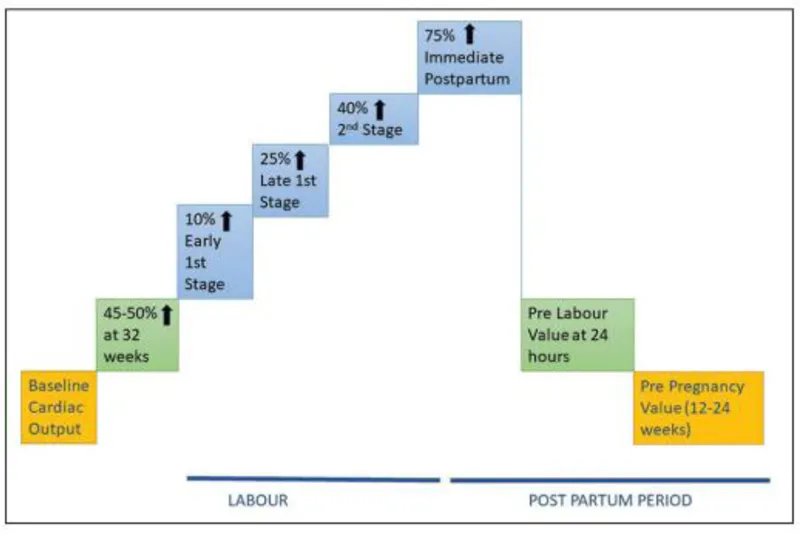
- Cardiovascular System:
- Initially ↑ Cardiac Output (CO); normalizes by ~2 weeks.
- Blood volume normalizes.
- Hypercoagulable state persists (↑ DVT/PE risk).
- Respiratory System:
- Functional Residual Capacity (FRC) normalizes.
- Airway edema may persist for 24-48 hours.
- Gastrointestinal System:
- Delayed gastric emptying.
- ↓ Lower Esophageal Sphincter (LES) tone.
⭐ Postpartum patients have an increased risk of aspiration due to delayed gastric emptying and decreased lower esophageal sphincter tone, mandating careful airway management.
- Nervous System:
- ↓ MAC for volatile anesthetics (persists 1-2 days).
- Neuraxial sensitivity normalizes.
 oka
oka
Preoperative Assessment - Safety Check Time!
- Consent: Verify informed, non-coerced consent; discuss permanence.
- Timing: Optimal <48h postpartum; ensure maternal stability.
- NPO: Adhere to 6-8h (solids), 2h (clear fluids) guidelines.
- Airway: Re-assess for edema, Mallampati score.
- Labs: Check Hb, platelets; coagulation status (especially post-neuraxial).
- Review: Recent labor, delivery, anesthesia records; estimated blood loss.
- Aspiration Prophylaxis: Consider (e.g., sodium citrate, ranitidine).
⭐ Thorough informed consent for PPTL is critical, ensuring the patient understands the permanence of the procedure and is not under duress, especially in the emotional postpartum period.
Anesthetic Techniques - Numb or Snooze?
Choice depends on maternal status, urgency, and patient/surgeon preference.
- Neuraxial Anesthesia (Preferred)
- Spinal (SAB):
- Rapid, dense block. Hyperbaric Bupivacaine 0.5% (7.5-12 mg) + Fentanyl 10-25 mcg.
- Risk: Hypotension.
- Epidural:
- Titratable, can use existing labor epidural. Lidocaine 2% or Bupivacaine 0.5%.
- Slower onset.
- CSE: Combines SAB speed with epidural flexibility.
- Spinal (SAB):
- General Anesthesia (GA)
- Indications: Contraindication/refusal of neuraxial, failed block, emergency.
- Technique: RSI mandatory (⚠️ ↑ aspiration risk).
- Consider: Difficult airway, neonatal effects (minimal if >1 hr post-delivery).
- Avoid uterine atony: use low concentration of volatile agents.
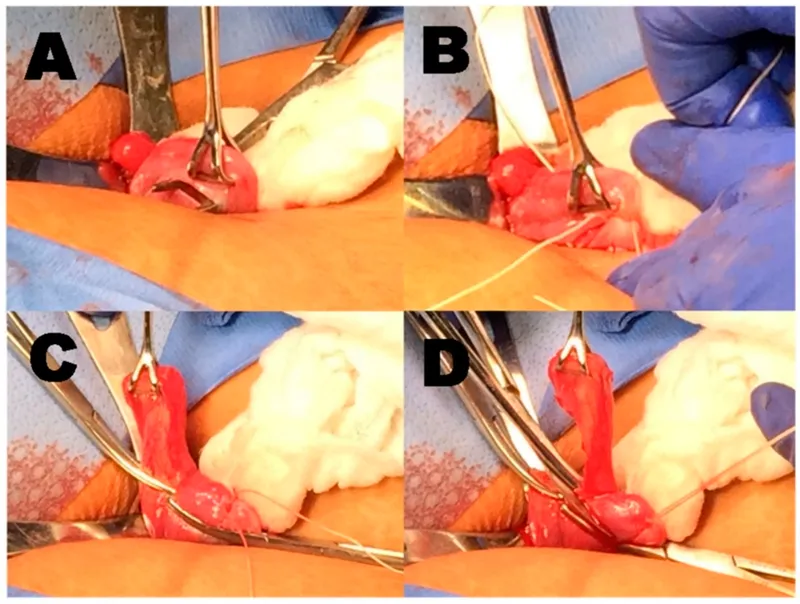
⭐ Neuraxial anesthesia (spinal or epidural) is the preferred technique for PPTL as it avoids airway manipulation, provides excellent analgesia, and allows the mother to be awake.
Complications & Management - Trouble Shooters' Guide
⭐ Factors associated with increased regret after tubal ligation include young maternal age (<25 years), unstable marital status, and making the decision during a stressful period like labor.
High‑Yield Points - ⚡ Biggest Takeaways
- Optimal timing: Best within 24-48 hours postpartum; fundus at umbilicus aids surgical access.
- Anesthetic choice: Neuraxial techniques (spinal/epidural) are strongly preferred over General Anesthesia (GA).
- Aspiration risk: Remains elevated; administer non-particulate antacids, H2 blockers, or PPIs.
- GA considerations: If GA is necessary, Rapid Sequence Intubation (RSI) is mandatory.
- Physiological state: Account for persistent peripartum changes (e.g., ↑CO, ↓FRC, ↑VTE risk).
- Neuraxial block level: Ensure sensory block to T4-T6 dermatome for adequate surgical anesthesia.
- Postoperative management: Focus on effective multimodal analgesia and VTE prophylaxis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

