Obstetric Anesthesia

On this page
🎯 Obstetric Anesthesia Mastery: The High-Stakes Precision Game
Obstetric anesthesia demands split-second decisions that protect two lives simultaneously while navigating dramatic physiologic changes, unpredictable complications, and time-critical emergencies. You'll master neuraxial techniques that eliminate pain while preserving maternal stability, build pattern recognition algorithms that distinguish benign adaptation from life-threatening crisis, and deploy evidence-based protocols for hemorrhage, failed airways, and cardiovascular collapse. This lesson transforms theoretical knowledge into clinical reflexes, equipping you to deliver safe, effective anesthesia across routine deliveries and obstetric catastrophes alike.
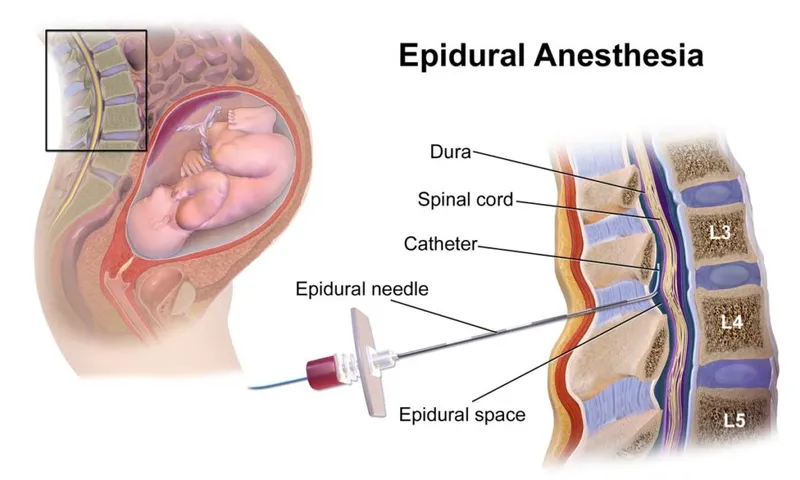
Physiological Foundation Architecture
The pregnant patient presents unique anesthetic challenges through systematic physiological adaptations that peak at 36-40 weeks gestation:
-
Cardiovascular Adaptations
- Cardiac output increases 30-50% by third trimester
- Blood volume expands 45% (plasma 55%, RBC 25%)
- Heart rate increases 15-20 bpm above baseline
- Stroke volume peaks at 28-32 weeks (+30%)
- Systemic vascular resistance decreases 20%
- Central venous pressure remains unchanged (6-8 mmHg)
-
Respiratory System Changes
- Functional residual capacity decreases 20%
- Oxygen consumption increases 20-30%
- Minute ventilation increases 50% (tidal volume +40%, rate +15%)
- Rapid desaturation during apnea (<3 minutes vs 8-10 minutes)
- PaCO2 decreases to 28-32 mmHg (respiratory alkalosis)
📌 Remember: CARDIAC - Cardiac output up, Aortocaval compression risk, Respiratory changes, Decreased FRC, Increased O2 consumption, Airway edema, Coagulation enhanced
Neuraxial Anesthesia Considerations
| Parameter | Non-Pregnant | Term Pregnancy | Clinical Significance | Anesthetic Implication |
|---|---|---|---|---|
| CSF Volume | 150 mL | 100 mL (-33%) | Reduced buffering capacity | Lower LA doses required |
| Epidural Space | Normal | Compressed | Venous engorgement | Increased block height |
| MAC Requirements | Baseline | Reduced 25-40% | Progesterone sensitivity | Lower volatile agent needs |
| Protein Binding | Normal | Decreased 10-20% | Increased free drug | Enhanced drug effects |
| Gastric Emptying | 2-4 hours | >8 hours | Aspiration risk | RSI considerations |
Placental Physiology and Drug Transfer
Understanding placental barrier function determines safe anesthetic choices:
-
Molecular Weight Thresholds
- <500 Da: Rapid transfer (most anesthetics)
- 500-1000 Da: Variable transfer (depends on lipophilicity)
-
1000 Da: Minimal transfer (muscle relaxants, heparin)
-
Drug Characteristics Favoring Transfer
- High lipid solubility (propofol, thiopental)
- Low protein binding (lidocaine 70% vs bupivacaine 95%)
- Non-ionized at physiological pH (volatile agents)
💡 Master This: Fetal/maternal drug ratio predicts neonatal effects. Ratios >0.5 (propofol, thiopental) require neonatal monitoring, while ratios <0.3 (bupivacaine, rocuronium) provide maternal safety margins.
Connect these foundational principles through regional anesthesia techniques to understand optimal labor analgesia protocols.
🎯 Obstetric Anesthesia Mastery: The High-Stakes Precision Game
🧩 Neuraxial Blockade: The Precision Pain Control System
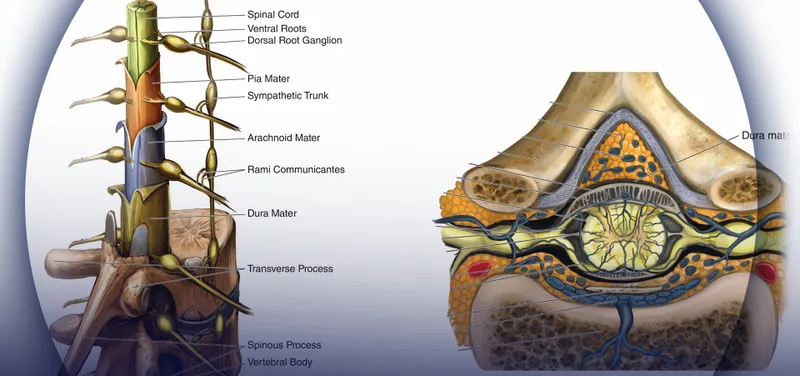
Spinal vs Epidural: Technical Precision Matrix
Comparative Technique Analysis
| Technique | Onset Time | Duration | LA Volume | Block Quality | Maternal Mobility |
|---|---|---|---|---|---|
| Spinal | 2-5 minutes | 2-4 hours | 1-3 mL | Dense, reliable | Limited initially |
| Epidural | 10-20 minutes | Variable | 10-20 mL | Variable density | Maintained |
| CSE | 2-5 minutes | Variable | 1-3 + 10-20 mL | Dense + flexible | Early mobility |
| DPE | 10-20 minutes | Extended | 15-25 mL | Bilateral reliable | Good throughout |
| PCEA | 15-30 minutes | Continuous | Patient-controlled | Consistent | Excellent |
Local Anesthetic Pharmacodynamics
-
Bupivacaine Characteristics
- Onset: 15-20 minutes (epidural), 5-10 minutes (spinal)
- Duration: 2-4 hours (motor), 4-8 hours (sensory)
- Concentration: 0.125-0.25% (epidural), 0.5% (spinal)
- Motor-sparing: 0.0625-0.125% with opioids
- Cesarean section: 0.5-0.75% (epidural), 0.75% (spinal)
-
Ropivacaine Advantages
- Reduced motor block at equivalent sensory levels
- Lower cardiotoxicity (safer if intravascular injection)
- Differential blockade: sensory > motor > sympathetic
- Labor analgesia: 0.1-0.2% concentration
- Cesarean section: 0.75-1.0% concentration
⭐ Clinical Pearl: Ropivacaine 0.1% with fentanyl 2 mcg/mL provides equivalent analgesia to bupivacaine 0.125% with 50% less motor block, enabling ambulatory labor in 85% of patients.
Opioid Adjuvant Integration
- Fentanyl Neuraxial Dosing
- Epidural: 50-100 mcg bolus, 2-4 mcg/mL infusion
- Spinal: 10-25 mcg (labor), 10-15 mcg (cesarean)
- Duration: 2-4 hours epidural, 3-6 hours spinal
- Onset enhancement: 50% faster with opioids
- Pruritus incidence: 30-100% (dose-dependent)
💡 Master This: Lipophilic opioids (fentanyl, sufentanil) provide segmental analgesia with minimal rostral spread, while hydrophilic opioids (morphine) cause delayed respiratory depression up to 24 hours post-injection.
Connect these technical foundations through complication management protocols to understand comprehensive safety frameworks.
🧩 Neuraxial Blockade: The Precision Pain Control System
🔧 Clinical Decision Algorithms: The Pattern Recognition Framework
Labor Analgesia Decision Matrix
"See This, Think That" Recognition Patterns
-
Hypotension After Neuraxial Block
- See: SBP drop >20% or <100 mmHg
- Think: Aortocaval compression + sympathetic blockade
- Act: Left uterine displacement + ephedrine 5-10 mg IV
- Phenylephrine 50-100 mcg if maternal tachycardia
- Fluid preload 500-1000 mL crystalloid
-
Inadequate Epidural Block
- See: Unilateral block or missed segments
- Think: Catheter malposition or anatomical variants
- Act: Patient positioning + 5-10 mL top-up
- Catheter withdrawal 1-2 cm if >15 cm insertion
- Replace catheter if persistent after 2 attempts
Emergency Conversion Protocols
| Scenario | Time Constraint | Primary Technique | Backup Plan | Success Rate |
|---|---|---|---|---|
| Category 1 C-Section | <30 minutes | Spinal anesthesia | General anesthesia | 95% |
| Failed Epidural | <15 minutes | Epidural top-up | Spinal/General | 80% |
| Instrumental Delivery | <10 minutes | Pudendal block | Epidural boost | 90% |
| Retained Placenta | <20 minutes | Epidural extension | Spinal/General | 85% |
| Postpartum Hemorrhage | Immediate | Existing neuraxial | General anesthesia | Variable |
Contraindication Assessment Framework
-
Absolute Contraindications
- Patient refusal (document thoroughly)
- Coagulopathy: INR >1.5, platelets <70,000
- Local infection at insertion site
- Systemic sepsis with hemodynamic instability
- Increased intracranial pressure (space-occupying lesion)
-
Relative Contraindications
- Hypovolemia (correct before neuraxial)
- Cardiac disease with fixed output (severe AS, MS)
- Neurological disease (document baseline deficits)
- Previous spinal surgery (anatomical distortion)
- Anticoagulation (timing-dependent)
⭐ Clinical Pearl: Platelet count >100,000 with normal function allows safe neuraxial anesthesia. Aspirin use requires 7-day discontinuation, while LMWH needs 12-hour interval before neuraxial procedures.
💡 Master This: Risk-benefit analysis guides every neuraxial decision. Category 1 cesarean sections may require general anesthesia despite functioning epidural if surgical urgency exceeds neuraxial conversion time.
Connect these decision algorithms through complication management strategies to understand comprehensive crisis response protocols.
🔧 Clinical Decision Algorithms: The Pattern Recognition Framework
🔍 Complication Recognition: The Differential Diagnosis Matrix
Hypotension Differential Analysis
| Etiology | Onset Pattern | Associated Signs | BP Response | Treatment Priority |
|---|---|---|---|---|
| Aortocaval Compression | Gradual, positional | Nausea, fetal bradycardia | Improves with positioning | Left displacement |
| Sympathetic Blockade | Rapid post-injection | High sensory level | Responds to vasopressors | Ephedrine/phenylephrine |
| Local Anesthetic Toxicity | Immediate | CNS symptoms, arrhythmias | Refractory hypotension | Lipid emulsion therapy |
| Anaphylaxis | Minutes post-exposure | Bronchospasm, rash | Severe, persistent | Epinephrine, steroids |
| High Spinal | 5-15 minutes | Dyspnea, upper limb weakness | Progressive decline | Airway management |
Respiratory Compromise Assessment
Neurological Complication Matrix
-
Postdural Puncture Headache (PDPH)
- Incidence: 1-5% (epidural), <1% (spinal with pencil-point needles)
- Characteristics: Postural, frontal-occipital, photophobia
- Treatment: Conservative 48-72 hours, then epidural blood patch
- Success rate: 85-95% with 20 mL autologous blood
- Contraindications: Fever, bacteremia, coagulopathy
-
Epidural Hematoma Risk Factors
- Anticoagulation: Warfarin, LMWH, novel anticoagulants
- Coagulopathy: Platelets <70,000, INR >1.5
- Multiple attempts: >3 needle passes
- Incidence: 1:150,000 epidurals, 1:220,000 spinals
- Presentation: Progressive neurological deficit over hours
Local Anesthetic Systemic Toxicity (LAST)
| Phase | CNS Symptoms | Cardiovascular Signs | Plasma Level | Management |
|---|---|---|---|---|
| Early | Tinnitus, metallic taste | Hypertension, tachycardia | 4-8 mcg/mL | Stop injection, O2 |
| Moderate | Confusion, seizures | Arrhythmias, hypotension | 8-12 mcg/mL | Lipid emulsion 20% |
| Severe | Coma, respiratory arrest | Cardiac arrest, asystole | >12 mcg/mL | ACLS + lipid therapy |
Fetal Bradycardia Response Protocol
- Immediate Assessment (<3 minutes)
- Maternal positioning: Left lateral, knee-chest
- Oxygen administration: 15 L/min non-rebreather mask
- IV fluid bolus: 500-1000 mL crystalloid
- Ephedrine 5-10 mg if maternal hypotension
- Terbutaline 0.25 mg SQ if uterine hypertonus
💡 Master This: Category 1 fetal bradycardia (<110 bpm for >10 minutes) requires delivery within 30 minutes. Failed intrauterine resuscitation mandates immediate cesarean section with general anesthesia if neuraxial conversion unsuccessful.

Connect these complication frameworks through advanced management protocols to understand evidence-based treatment algorithms.
🔍 Complication Recognition: The Differential Diagnosis Matrix
⚖️ Advanced Management Protocols: The Evidence-Based Treatment Matrix
Cesarean Section Anesthesia Algorithm
Spinal Anesthesia Optimization Protocol
| Component | Standard Dose | High-Risk Modification | Success Rate | Duration |
|---|---|---|---|---|
| Hyperbaric Bupivacaine | 10-12.5 mg | 8-10 mg (short stature) | 95-98% | 2-3 hours |
| Fentanyl | 10-15 mcg | 10 mcg (respiratory disease) | Enhanced quality | +30-60 min |
| Morphine | 100-200 mcg | 100 mcg (elderly) | 18-24 hr analgesia | Extended |
| Phenylephrine Infusion | 25-50 mcg/min | 50-100 mcg/min (obesity) | Maintains BP | Titrated |
| Ondansetron | 4-8 mg | 8 mg (high-risk PONV) | 60-80% reduction | 4-6 hours |
Failed Spinal Management
-
Inadequate Block Assessment (10-15 minutes post-injection)
- Sensory level: Pinprick to T4 bilaterally required
- Motor assessment: Modified Bromage scale 2-3
- Sympathetic block: 20% BP reduction expected
- Supplementation options: Epidural catheter, repeat spinal
- Conversion threshold: >50% inadequate block
-
Rescue Techniques Success Rates
- Epidural top-up: 70-80% success if partial block
- Repeat spinal: 85-90% success if complete failure
- General anesthesia: 100% reliable but increased risks
- Time constraints: Category 1 = GA preferred if >15 minutes
Postoperative Pain Management Evidence
-
Multimodal Analgesia Protocol
- Intrathecal morphine: 100-200 mcg (18-24 hour duration)
- Acetaminophen: 1000 mg q6h (hepatic metabolism)
- NSAIDs: Ibuprofen 600 mg q6h (avoid if renal/cardiac disease)
- Gabapentin: 300-600 mg preoperatively (30% opioid reduction)
- Dexamethasone: 8 mg IV (anti-inflammatory, antiemetic)
-
Breakthrough Pain Management
- PCA morphine: 1-2 mg bolus, 5-10 minute lockout
- Tramadol: 50-100 mg q6h (ceiling effect at 400 mg/day)
- Oxycodone: 5-10 mg q4-6h (oral bioavailability 60-80%)
⭐ Clinical Pearl: Intrathecal morphine 150 mcg provides equivalent analgesia to PCA morphine for 24 hours with 60% reduction in total opioid consumption and improved patient satisfaction scores.
High-Risk Patient Modifications
-
Obesity (BMI >35) Adjustments
- Spinal dose: Reduce 10-20% (enhanced spread)
- Positioning: Sitting position for landmark identification
- Monitoring: Continuous pulse oximetry, ETCO2 if sedation
- Ultrasound guidance: Improves success in >80% of difficult cases
- Airway assessment: Mallampati, neck circumference >43 cm
-
Preeclampsia Protocol Modifications
- Platelet threshold: >70,000 for neuraxial anesthesia
- Magnesium interactions: Enhanced neuromuscular blockade
- Antihypertensive timing: Avoid ACE inhibitors perioperatively
- Target BP: <160/110 mmHg but >140/90 mmHg
- Fluid restriction: 80-100 mL/hr maintenance
💡 Master This: Evidence-based protocols reduce anesthetic complications by 40-60% through standardized approaches. Checklist utilization improves safety outcomes and reduces variability in high-risk scenarios.
Connect these advanced protocols through system integration strategies to understand comprehensive perioperative care frameworks.
⚖️ Advanced Management Protocols: The Evidence-Based Treatment Matrix
🔗 Multisystem Integration: The Comprehensive Care Architecture
Maternal-Fetal Physiological Integration
-
Uteroplacental Blood Flow Optimization
- Baseline flow: 500-800 mL/min at term (10-15% cardiac output)
- Anesthetic effects: Sympathetic blockade improves uterine perfusion
- Positioning impact: 15-degree left tilt increases flow 25-30%
- Hypotension threshold: <80% baseline reduces fetal oxygen delivery
- Vasopressor choice: Phenylephrine maintains placental perfusion
-
Fetal Drug Exposure Minimization
- Neuraxial advantages: Minimal systemic absorption (<5% maternal dose)
- Protein binding: Bupivacaine 95% vs lidocaine 70% bound
- Fetal metabolism: Immature enzyme systems prolong drug half-life
- Umbilical cord pH: Maintain >7.25 (arterial), >7.30 (venous)
- Base excess: Target >-8 mEq/L for optimal outcomes

Cardiovascular-Respiratory Synchronization
Advanced Monitoring Integration Matrix
| System | Parameter | Normal Range | Critical Threshold | Intervention Trigger |
|---|---|---|---|---|
| Cardiovascular | MAP | 80-100 mmHg | <65 mmHg | Vasopressor therapy |
| Respiratory | SpO2 | >95% | <92% | Supplemental O2 |
| Neurological | Sensory Level | T6-T4 | >T2 | Respiratory support |
| Fetal | FHR | 110-160 bpm | <110 or >180 | Intrauterine resuscitation |
| Uterine | Contraction | <5 in 10 min | Tetanic | Tocolytic therapy |
Cutting-Edge Research Applications
-
Enhanced Recovery After Surgery (ERAS) Protocols
- Preoperative optimization: Carbohydrate loading, anxiety reduction
- Intraoperative management: Goal-directed fluid therapy, multimodal analgesia
- Postoperative acceleration: Early mobilization, optimized nutrition
- Length of stay reduction: 20-30% with ERAS implementation
- Complication rates: Decreased 40% with protocol adherence
-
Personalized Medicine Integration
- Pharmacogenomic testing: CYP2D6 variants affect opioid metabolism
- Genetic polymorphisms: COMT variants influence pain sensitivity
- Precision dosing: Weight-based algorithms improve drug efficacy
- Biomarker utilization: Inflammatory markers guide analgesic choices
- Predictive modeling: AI algorithms optimize anesthetic plans
Quality Metrics and Outcome Optimization
-
Maternal Outcome Measures
- Anesthetic satisfaction: >90% with optimal protocols
- Conversion to GA rate: <5% for elective procedures
- PDPH incidence: <2% with pencil-point needles
- Hypotension episodes: <20% with prophylactic measures
- Nausea/vomiting: <30% with multimodal prevention
-
Neonatal Outcome Correlations
- Apgar scores: >7 at 5 minutes in >95% with neuraxial anesthesia
- NICU admission rates: <10% for term deliveries
- Umbilical cord gases: pH >7.25 in >90% of cases
⭐ Clinical Pearl: Integrated care protocols combining evidence-based anesthesia, fetal monitoring, and team communication reduce composite maternal morbidity by 35% and improve neonatal outcomes by 25%.
💡 Master This: Systems-based practice requires understanding interdependencies between anesthetic interventions and physiological responses. Anticipatory management prevents complications more effectively than reactive treatment.
Connect these integration strategies through rapid mastery frameworks to understand clinical excellence tools.
🔗 Multisystem Integration: The Comprehensive Care Architecture
🎯 Clinical Mastery Arsenal: The Rapid Excellence Framework
Essential Numbers Arsenal
| Critical Threshold | Value | Clinical Significance | Action Required |
|---|---|---|---|
| Spinal Sensory Level | T4 | Adequate for cesarean | Proceed with surgery |
| Maternal Hypotension | <80% baseline | Uteroplacental compromise | Immediate vasopressor |
| Fetal Bradycardia | <110 bpm >10 min | Category 1 emergency | Delivery within 30 min |
| Platelet Count | <70,000 | Neuraxial contraindication | Alternative anesthesia |
| PDPH Incidence | 1-5% | Expected complication | Conservative then EBP |
Rapid Assessment Framework
Clinical Commandments for Excellence
- The Five Pillars of Obstetric Anesthesia
- Maternal Safety First: Every decision prioritizes maternal wellbeing
- Fetal Consideration Always: Minimize drug exposure, optimize perfusion
- Communication Excellence: Clear, timely, documented interactions
- Evidence-Based Practice: Guidelines, protocols, best practices
- Team Coordination: Multidisciplinary, collaborative, efficient
⭐ Clinical Pearl: The 30-Second Rule - Every obstetric emergency requires initial assessment and intervention initiation within 30 seconds of recognition. Delayed response exponentially increases morbidity risk.
Master Clinician Checklist
-
Pre-Procedure Verification
- Informed consent obtained and documented
- Coagulation status assessed (platelets >70,000)
- IV access established (16-18 gauge minimum)
- Monitoring applied (NIBP, pulse oximetry, ECG)
- Emergency drugs prepared (ephedrine, phenylephrine)
- Airway assessment completed (backup plan ready)
-
Post-Procedure Excellence
- Sensory level documented (bilateral T4 for cesarean)
- Motor function assessed (modified Bromage scale)
- Hemodynamic stability confirmed (BP within 20% baseline)
- Pain scores evaluated (VAS <3 for labor, <4 post-cesarean)
- Complications monitored (PDPH, neurological deficits)
Pattern Recognition Mastery
💡 Master This: Expert pattern recognition develops through deliberate practice with systematic case review. Monthly case discussions focusing on decision points and alternative approaches accelerate clinical expertise development.
The Expert's Mental Model: Every obstetric anesthetic follows predictable phases - Assessment → Planning → Execution → Monitoring → Adjustment → Completion. Mastery means seamless transitions between phases with anticipatory management of potential complications.
🎯 Clinical Mastery Arsenal: The Rapid Excellence Framework
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























