ICP Fundamentals - Skull's Tight Squeeze
- Monro-Kellie Doctrine: Skull is a rigid box. Intracranial volume ($V_{brain} + V_{blood} + V_{CSF}$) is constant.
- Components: Brain (~80%), Blood (~12%), CSF (~8%).
- Normal ICP: 5-15 mmHg. Pathological if sustained > 20 mmHg.
- Cerebral Perfusion Pressure (CPP): $CPP = MAP - ICP$.
- Normal/Target CPP: 60-70 mmHg.
- Minimum CPP to prevent ischemia: 50 mmHg.
- Compliance: Brain's ability to accommodate volume changes. Initially high, then rapidly decreases with ↑ volume.

⭐ Cushing's triad (hypertension, bradycardia, irregular respirations) is a late and ominous sign of severely elevated ICP indicating brainstem compression.
Raised ICP: Etiology & Clinical Features - Pressure's Nasty News
- Etiology (Monro-Kellie Doctrine Imbalance):
- ↑ Brain Parenchyma: Tumor, edema, hematoma.
- ↑ CSF: Hydrocephalus, ↓ absorption.
- ↑ Blood Volume: Hyperemia, venous obstruction.
- Clinical Features:
- Early: Headache (worse AM), vomiting (projectile), papilledema, CN VI palsy (diplopia), altered sensorium.
- Late/Ominous:
- 📌 Cushing's Triad: ↑ SBP (wide pulse pressure), ↓ HR, irregular respirations.
- Pupillary changes (e.g., unilateral fixed dilated pupil → uncal herniation).
- Posturing, coma.
⭐ Uncal herniation classically causes ipsilateral CN III palsy (fixed dilated pupil) and contralateral hemiparesis.

ICP Monitoring - Window to Brain
- Indications: Severe TBI (GCS 3-8) + abnormal CT; or normal CT if age >40 yrs, motor posturing, or SBP <90 mmHg.
- Types:
- Invasive (Gold Standard): EVD (External Ventricular Drain - also therapeutic), intraparenchymal, subdural, epidural.
- Non-invasive: Transcranial Doppler (TCD), Optic Nerve Sheath Diameter (ONSD), pupillometry.
- Waveform Components:
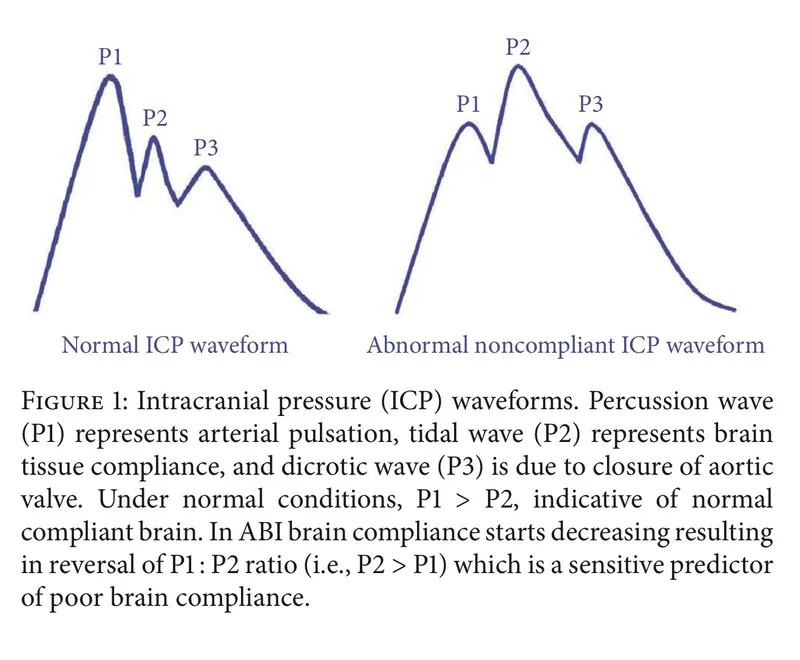
- P1 (Percussion wave): Arterial pulsation.
- P2 (Tidal wave): Brain compliance. ↑P2 indicates ↓compliance.
- P3 (Dicrotic wave): Aortic valve closure.
- Normal: P1 > P2. Pathological: P2 > P1.
⭐ EVD is the gold standard for ICP monitoring as it allows simultaneous therapeutic CSF drainage for ICP management.
ICP Management: Tier 1 - First-Line Fixes
Initial, non-invasive measures to manage elevated ICP (target < 20-22 mmHg).
- Positioning: Head up 30°, midline neck. Avoid constrictions, extreme rotation/flexion. Promotes venous outflow.
- Sedation & Analgesia: Propofol, opioids (e.g., fentanyl) to ↓CMRO2, control pain/agitation.
- Ventilation: Maintain PaCO2 35-40 mmHg (normocapnia). Ensure PaO2 > 100 mmHg (avoid hypoxia).
- Physiological Homeostasis: Target CPP 50-70 mmHg. Maintain normothermia, normoglycemia. Treat seizures.
⭐ If an External Ventricular Drain (EVD) is present, CSF drainage is a rapid Tier 0/1 intervention to decrease ICP immediately.
ICP Management: Advanced - Brain Rescue Ops
For refractory Intracranial Pressure (ICP > 20-25 mmHg) when Tier 1 fails. Goal: Maintain Cerebral Perfusion Pressure (CPP) 60-70 mmHg.
- Tier 2 Medical Management:
- Hyperosmolar Therapy:
- Mannitol 0.5-1 g/kg (Serum Osmolality < 320 mOsm/L).
- Hypertonic Saline (e.g., 3%): Target $Na^+$ 145-155 mEq/L.
- Controlled Hyperventilation: Target $P_{aCO_2}$ 30-35 mmHg (short-term). ⚠️ Avoid $P_{aCO_2}$ < 25 mmHg.
- Barbiturate Coma (Thiopental): EEG burst suppression. Reduces ↓$CMRO_2$, ↓$CBF$, ↓ICP.
- Hyperosmolar Therapy:
- Surgical Intervention:
- Decompressive Craniectomy: For malignant, refractory ICP.

⭐ Decompressive craniectomy can be life-saving in malignant MCA infarction with refractory ICP.
High‑Yield Points - ⚡ Biggest Takeaways
- Normal Intracranial Pressure (ICP) is 5-15 mmHg; sustained ICP >20 mmHg requires intervention.
- Cerebral Perfusion Pressure (CPP) = Mean Arterial Pressure (MAP) - ICP (or CVP if higher); target 60-70 mmHg.
- Cushing's Triad (hypertension, bradycardia, irregular respirations) is a late sign of severely ↑ICP.
- Management includes head elevation (30°), controlled hyperventilation (PaCO2 30-35 mmHg), and osmotic agents like mannitol or hypertonic saline.
- Avoid hypoxia, hypercapnia, hypotension, and high concentrations of volatile anesthetics which can ↑ICP.
- Barbiturates (e.g., thiopental) or propofol can ↓ICP by reducing cerebral metabolic rate (CMRO2).
- Maintain normothermia; fever can significantly ↑ICP by increasing CMRO2.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

