Local Anesthetics

On this page
🧬 The Molecular Gatekeepers: Local Anesthetic Architecture
Local anesthetics are molecular precision tools that silence pain by blocking sodium channels, yet their clinical mastery demands far more than memorizing names and maximum doses. You'll discover how chemical structure predicts onset and duration, why toxicity strikes the brain before the heart, and how to select the right agent for each clinical scenario from dental blocks to epidurals. We'll build your pattern recognition for adverse events, equip you with evidence-based rescue protocols, and integrate these concepts across surgery, emergency medicine, and obstetrics so you can wield these drugs with both confidence and caution.

📌 Remember: LAB - Lipophilic aromatic ring, Amide/ester linkage, Basic amine group - the three essential components that define every local anesthetic molecule
The fundamental architecture consists of three critical domains connected in precise sequence. The lipophilic aromatic ring provides membrane penetration capability, typically a benzene derivative that determines potency through hydrophobic interactions. The intermediate chain contains either an ester or amide linkage, dictating metabolic pathway and allergenic potential. The hydrophilic amine group enables water solubility and pH-dependent ionization crucial for clinical activity.
-
Aromatic Ring Domain
- Benzene-based structure with 70-90% lipophilicity contribution
- Para-aminobenzoic acid (PABA) derivatives in esters
- Procaine: single PABA structure
- Chloroprocaine: chlorinated PABA for enhanced potency
- Non-PABA structures in amides
- Lidocaine: xylidine-based aromatic system
- Bupivacaine: butyl-substituted aniline ring
-
Intermediate Linkage Chain
- Ester bonds: hydrolyzed by plasma pseudocholinesterases
- Half-life: 1-8 minutes in plasma
- Metabolism rate: 4000-fold faster than amides
- Amide bonds: metabolized by hepatic microsomal enzymes
- Half-life: 90-200 minutes in plasma
- CYP1A2 and CYP3A4 primary pathways
- Ester bonds: hydrolyzed by plasma pseudocholinesterases
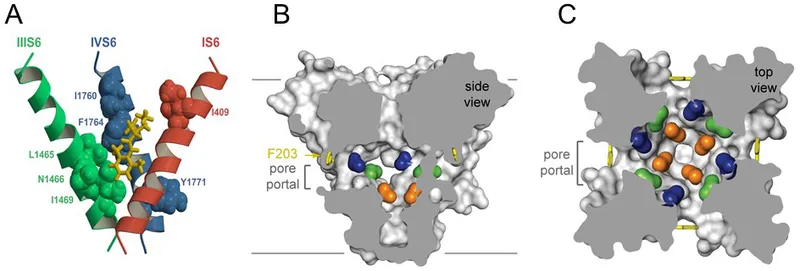
| Property | Ester LAs | Amide LAs | Clinical Significance | Potency Factor | Duration Range |
|---|---|---|---|---|---|
| Linkage Stability | Hydrolyzed rapidly | Metabolized slowly | Systemic toxicity risk | 1-4x procaine | 30min-8hrs |
| Allergic Potential | High (PABA metabolites) | Minimal (<1%) | Cross-reactivity patterns | Lipophilicity dependent | Onset: 1-30min |
| Plasma Protein Binding | 5-15% | 55-95% | Duration correlation | pKa determines onset | Recovery: 2-24hrs |
| Volume Distribution | 0.7-1.2 L/kg | 1.1-2.7 L/kg | Dosing calculations | Protein binding = duration | Half-life: 1-200min |
| Hepatic Dependence | Minimal | Complete | Liver disease impact | Molecular weight varies | Toxic threshold variable |
The pKa value determines onset speed through Henderson-Hasselbalch equilibrium. Most local anesthetics have pKa values between 7.6-9.1, creating pH-dependent ionization that affects membrane penetration. At physiological pH 7.4, agents with lower pKa values like lidocaine (7.9) achieve 65% unionized fraction, enabling rapid onset within 2-5 minutes. Higher pKa agents like procaine (8.9) show only 25% unionized fraction, resulting in 10-20 minute onset delays.
💡 Master This: The unionized fraction penetrates nerve membranes, while the ionized fraction blocks sodium channels - both forms are essential for complete anesthetic action, explaining why alkalinization speeds onset but doesn't eliminate the need for ionized drug

Protein binding correlates directly with duration of action through tissue reservoir effects. Bupivacaine demonstrates 95% protein binding with 4-8 hour duration, while procaine shows 6% binding with 30-60 minute duration. This relationship enables predictable clinical planning for surgical procedures requiring specific anesthetic windows.
📌 Remember: POLD - Protein binding determines duration, Onset depends on pKa, Lipophilicity controls potency, Degradation pathway affects toxicity risk
Understanding molecular architecture transforms clinical decision-making from empirical guessing to scientific precision, enabling optimal agent selection based on procedure requirements and patient physiology.
🧬 The Molecular Gatekeepers: Local Anesthetic Architecture
⚡ The Sodium Channel Siege: Mechanism Mastery
Voltage-gated sodium channels exist in three distinct conformational states that determine local anesthetic binding affinity. The resting state (closed but activatable) shows minimal drug binding, while the activated state (open during depolarization) demonstrates moderate affinity. The inactivated state (refractory period) exhibits highest binding affinity, explaining use-dependent blockade where repeated nerve stimulation enhances anesthetic effect.
📌 Remember: ROI - Resting (low affinity), Open (moderate affinity), Inactivated (high affinity) - the three states that determine local anesthetic binding strength
The use-dependent block phenomenon explains why local anesthetics preferentially affect high-frequency firing nerves. Pain fibers (C-fibers) firing at 2-20 Hz experience progressive block intensification with each action potential, while motor fibers firing at 0.1-1 Hz maintain relative function. This selectivity enables differential nerve blockade where sensory loss precedes motor paralysis.
- Channel State Transitions
- Resting potential: -70mV with channels closed
- Sodium permeability: <1% of peak
- LA binding affinity: minimal
- Activation threshold: -55mV triggers opening
- Sodium influx: 500-fold increase
- Channel open time: 0.5-1 millisecond
- Inactivation phase: +30mV peak depolarization
- Fast inactivation: 1-2 milliseconds
- LA binding affinity: 10-100x higher
- Resting potential: -70mV with channels closed

| Nerve Fiber Type | Diameter (μm) | Myelination | Firing Frequency | Block Sensitivity | Clinical Function |
|---|---|---|---|---|---|
| C-fibers (pain) | 0.2-1.5 | Unmyelinated | 2-20 Hz | Highest | Temperature, dull pain |
| Aδ-fibers (pain) | 2-5 | Lightly myelinated | 5-50 Hz | High | Sharp pain, cold |
| Aβ-fibers (touch) | 5-12 | Myelinated | 1-10 Hz | Moderate | Light touch, pressure |
| Aγ-fibers (motor) | 3-6 | Myelinated | 0.5-2 Hz | Low | Muscle spindle control |
| Aα-fibers (motor) | 12-20 | Heavily myelinated | 0.1-1 Hz | Lowest | Motor function, proprioception |
⭐ Clinical Pearl: Differential nerve block follows predictable sequence - pain → temperature → touch → proprioception → motor - with recovery occurring in reverse order, enabling assessment of block regression
Local anesthetics demonstrate stereoselective binding with significant clinical implications. S-bupivacaine (levobupivacaine) shows 60% less cardiac toxicity than racemic bupivacaine while maintaining equivalent analgesic potency. This stereoselectivity results from different binding orientations within the sodium channel pore, affecting both therapeutic efficacy and toxic potential.
💡 Master This: The hydrophobic pathway theory explains how local anesthetics reach their binding site - unionized molecules penetrate the lipid membrane directly to access intracellular channel domains, while ionized forms enter through the open channel pore during depolarization
Frequency-dependent blockade intensifies with repetitive nerve stimulation, creating cumulative channel inactivation. Each action potential increases the proportion of channels in the high-affinity inactivated state, progressively deepening the block. This mechanism explains why nerve stimulator testing during regional anesthesia may actually enhance block density through repeated stimulation.
The critical length concept determines minimum nerve segment requiring blockade for complete conduction failure. Myelinated nerves need 2-3 nodes of Ranvier blocked simultaneously, spanning 6-9mm of nerve length. Unmyelinated fibers require 8-10mm of continuous blockade. Understanding critical length explains why inadequate local anesthetic spread results in patchy or incomplete blocks.
📌 Remember: CLIMB - Critical length varies by fiber type, Length determines block success, Inactivated state has highest affinity, Myelinated needs nodal blockade, Blockade intensifies with use
This mechanistic understanding transforms regional anesthesia from empirical technique to precision medicine, enabling predictable nerve blockade tailored to specific surgical and analgesic requirements.
⚡ The Sodium Channel Siege: Mechanism Mastery
🎯 Clinical Command Center: Pattern Recognition Mastery
Onset Pattern Recognition follows predictable timelines that signal block success or failure. Lidocaine demonstrates 2-5 minute sensory onset with complete block by 15 minutes, while bupivacaine shows 10-20 minute onset with peak effect at 30-45 minutes. Deviations from these patterns indicate technical issues, anatomical variants, or pharmacological problems requiring immediate intervention.
📌 Remember: FAST onset patterns - Five minutes for lidocaine sensation, Always check at 15 minutes, Slow bupivacaine needs 20 minutes, Thirty minutes for peak effect assessment
-
Rapid Onset Indicators (2-5 minutes)
- Lidocaine 1-2%: immediate tingling sensation
- Sensory loss: 3-5 minutes
- Motor block: 5-10 minutes
- Mepivacaine 1-2%: similar onset profile
- Duration advantage: 50% longer than lidocaine
- Less vasodilation: reduced systemic absorption
- Chloroprocaine 2-3%: fastest onset available
- Sensory block: 1-3 minutes
- Complete recovery: 30-60 minutes
- Lidocaine 1-2%: immediate tingling sensation
-
Delayed Onset Patterns (10-30 minutes)
- Bupivacaine 0.25-0.75%: gradual progressive block
- Initial tingling: 5-10 minutes
- Complete sensory loss: 15-30 minutes
- Motor blockade: 20-45 minutes
- Ropivacaine 0.2-1%: motor-sparing characteristics
- Sensory-motor dissociation: 2:1 ratio
- Cardiovascular safety: 4x less toxic
- Bupivacaine 0.25-0.75%: gradual progressive block

| Agent | Onset Time | Peak Effect | Duration | Motor Block | Cardiovascular Safety |
|---|---|---|---|---|---|
| Chloroprocaine 3% | 1-3 min | 5-10 min | 30-60 min | Minimal | Excellent |
| Lidocaine 2% | 2-5 min | 10-15 min | 90-180 min | Moderate | Good |
| Mepivacaine 2% | 3-8 min | 15-20 min | 120-240 min | Moderate | Good |
| Bupivacaine 0.5% | 10-20 min | 30-45 min | 240-480 min | Dense | Poor |
| Ropivacaine 0.75% | 10-25 min | 30-60 min | 240-420 min | Selective | Excellent |
⭐ Clinical Pearl: Pinprick sensation remaining at 30 minutes indicates <50% probability of adequate surgical anesthesia, requiring supplementation or alternative technique regardless of patient comfort level
Troubleshooting Failed Blocks follows systematic diagnostic patterns. Patchy or incomplete blocks suggest inadequate volume or concentration, anatomical variants, or technical placement errors. Complete absence of effect indicates wrong injection site, intravascular injection, or drug preparation errors.
Duration Prediction Patterns enable surgical planning and postoperative management. Ester local anesthetics provide 30-90 minute duration suitable for minor procedures, while amide agents offer 2-8 hour duration for major surgery. Epinephrine addition extends duration by 50-100% through vasoconstriction and reduced systemic absorption.
💡 Master This: Block regression follows reverse order - motor function returns before sensory, and pain sensation returns last, creating a 2-4 hour window of continued analgesia after motor recovery with long-acting agents
Complication Recognition Patterns require immediate identification and management. Systemic toxicity presents with CNS excitation followed by depression, while cardiovascular toxicity shows progressive conduction delays and myocardial depression. Allergic reactions demonstrate rapid onset with skin manifestations and respiratory symptoms.
-
Early Warning Signs
- Metallic taste or perioral numbness: plasma levels >2-3 μg/mL
- Tinnitus or visual disturbances: approaching toxic threshold
- Muscle twitching or agitation: CNS excitation phase
- Bradycardia or hypotension: cardiovascular depression
-
Emergency Response Triggers
- Seizure activity: immediate lipid emulsion therapy
- Cardiac arrhythmias: ACLS with lipid rescue
- Respiratory depression: airway management priority
- Anaphylaxis: epinephrine and supportive care
Patient-Specific Modification Patterns account for physiological variables affecting drug response. Elderly patients require 25-30% dose reduction due to decreased clearance and increased sensitivity. Pregnant patients show enhanced neural sensitivity requiring reduced concentrations while avoiding bupivacaine due to cardiac toxicity risk.
📌 Remember: AGES - Adjust doses for elderly, Gestational changes increase sensitivity, Enhanced toxicity in pregnancy, Special populations need modifications
This pattern recognition framework transforms clinical decision-making from reactive troubleshooting to proactive management, enabling consistent success in regional anesthesia practice.
🎯 Clinical Command Center: Pattern Recognition Mastery
🔬 The Differential Diagnosis Matrix: Agent Selection Science

Potency Relationships follow predictable patterns based on lipophilicity and protein binding characteristics. Bupivacaine demonstrates 4x greater potency than lidocaine, enabling lower concentrations for equivalent effect while extending duration 3-4 fold. Chloroprocaine requires higher concentrations but provides fastest onset with minimal systemic toxicity.
📌 Remember: POWER - Potency correlates with lipophilicity, Onset speed varies inversely with pKa, Wider therapeutic index means safer, Ester metabolism faster than amide, Recovery follows reverse block sequence
| Agent | Relative Potency | Onset (min) | Duration (hrs) | Protein Binding | Toxic Dose (mg/kg) |
|---|---|---|---|---|---|
| Procaine | 1 | 15-30 | 0.5-1 | 6% | 8-10 |
| Chloroprocaine | 1 | 2-5 | 0.5-1 | 9% | 15-20 |
| Lidocaine | 2 | 2-5 | 1-3 | 65% | 4-7 |
| Mepivacaine | 2 | 3-8 | 2-4 | 75% | 4-7 |
| Prilocaine | 2 | 2-8 | 1-3 | 55% | 6-8 |
| Bupivacaine | 4 | 10-20 | 4-8 | 95% | 2-3 |
| Levobupivacaine | 4 | 10-25 | 4-8 | 97% | 3-4 |
| Ropivacaine | 3 | 10-25 | 4-6 | 94% | 3-4 |
⭐ Clinical Pearl: Cardiac safety ranking from safest to most dangerous: Chloroprocaine > Ropivacaine > Levobupivacaine > Lidocaine > Mepivacaine > Bupivacaine, with 10-fold safety difference between extremes
Onset Speed Determinants depend primarily on pKa values and concentration gradients. Agents with pKa closest to physiological pH achieve fastest onset through higher unionized fractions. Lidocaine (pKa 7.9) reaches 65% unionized at pH 7.4, while procaine (pKa 8.9) achieves only 25% unionized, explaining 5-fold onset difference.
Duration Matching Strategies require precise correlation between surgical time requirements and pharmacological profiles. Outpatient procedures benefit from intermediate-duration agents (2-4 hours) that provide adequate anesthesia without prolonged motor blockade. Inpatient surgery can utilize long-acting agents for extended postoperative analgesia.
-
Short-Duration Applications (30-90 minutes)
- Chloroprocaine 2-3%: fastest onset, minimal toxicity
- Ideal for: outpatient procedures, cardiac patients
- Limitations: brief duration, requires frequent redosing
- Lidocaine 1-2%: reliable onset, moderate duration
- Ideal for: minor surgery, diagnostic procedures
- Advantages: familiar pharmacology, wide availability
- Chloroprocaine 2-3%: fastest onset, minimal toxicity
-
Intermediate-Duration Applications (2-4 hours)
- Mepivacaine 1-2%: balanced profile, less vasodilation
- Ideal for: ambulatory surgery, regional blocks
- Benefits: reduced bleeding, stable hemodynamics
- Prilocaine 1-2%: low systemic toxicity, good penetration
- Ideal for: IVRA, large volume blocks
- Caution: methemoglobinemia with doses >8 mg/kg
- Mepivacaine 1-2%: balanced profile, less vasodilation
Special Population Considerations require agent-specific modifications based on physiological alterations and safety profiles. Pregnant patients should avoid bupivacaine due to enhanced cardiotoxicity and difficult resuscitation. Elderly patients demonstrate increased sensitivity requiring 25-30% dose reduction across all agents.
💡 Master This: Ropivacaine provides optimal safety profile for high-risk patients with equivalent analgesia to bupivacaine but superior cardiovascular safety and reduced motor blockade enabling early mobilization
Concentration-Volume Relationships determine block characteristics and safety margins. Higher concentrations provide denser motor blockade but increased toxicity risk, while larger volumes improve block spread with lower peak plasma levels. Dilute solutions (0.125-0.25%) enable sensory-selective blockade for labor analgesia and postoperative pain management.
| Clinical Goal | Optimal Agent | Concentration | Volume | Expected Outcome |
|---|---|---|---|---|
| Dense surgical block | Bupivacaine | 0.5-0.75% | 15-25 mL | Complete anesthesia 4-8 hrs |
| Motor-sparing analgesia | Ropivacaine | 0.2-0.375% | 20-30 mL | Sensory block 4-6 hrs |
| Rapid onset block | Lidocaine | 1.5-2% | 15-25 mL | Fast onset 2-3 hrs |
| Outpatient procedure | Mepivacaine | 1-1.5% | 15-20 mL | Balanced profile 2-4 hrs |
| High-risk cardiac | Chloroprocaine | 2-3% | 15-25 mL | Minimal toxicity 1 hr |
📌 Remember: MATCH - Match duration to procedure, Assess cardiac risk, Tailor concentration to needs, Consider patient factors, Handle adjuvants appropriately
This systematic selection framework transforms agent choice from empirical preference to evidence-based precision, optimizing outcomes while minimizing complications across diverse clinical scenarios.
🔬 The Differential Diagnosis Matrix: Agent Selection Science
⚖️ Treatment Algorithms: Evidence-Based Management Protocols
Pre-procedure Assessment Algorithm systematically evaluates patient factors, procedural requirements, and safety considerations to guide optimal agent selection and dosing strategies. Cardiac risk stratification determines agent safety profiles, while procedure duration guides pharmacological matching for optimal outcomes.
Maximum Dose Calculation Protocol prevents systemic toxicity through weight-based dosing with safety margins. Lidocaine maximum: 4.5 mg/kg without epinephrine, 7 mg/kg with epinephrine. Bupivacaine maximum: 2.5 mg/kg regardless of epinephrine due to prolonged elimination and enhanced cardiotoxicity.
📌 Remember: DOSE - Determine weight accurately, Optimize with epinephrine, Safety margins essential, Extra caution with bupivacaine
- Standard Maximum Doses (mg/kg)
- Lidocaine: 4.5 mg/kg plain, 7 mg/kg with epinephrine
- 70kg patient: 315mg plain, 490mg with epi
- Clinical volumes: 15-25mL of 1.5-2% solution
- Bupivacaine: 2.5 mg/kg (epinephrine doesn't increase limit)
- 70kg patient: 175mg maximum dose
- Clinical volumes: 35mL of 0.5% or 70mL of 0.25%
- Ropivacaine: 3 mg/kg maximum recommended dose
- 70kg patient: 210mg maximum dose
- Clinical volumes: 28mL of 0.75% or 42mL of 0.5%
- Lidocaine: 4.5 mg/kg plain, 7 mg/kg with epinephrine
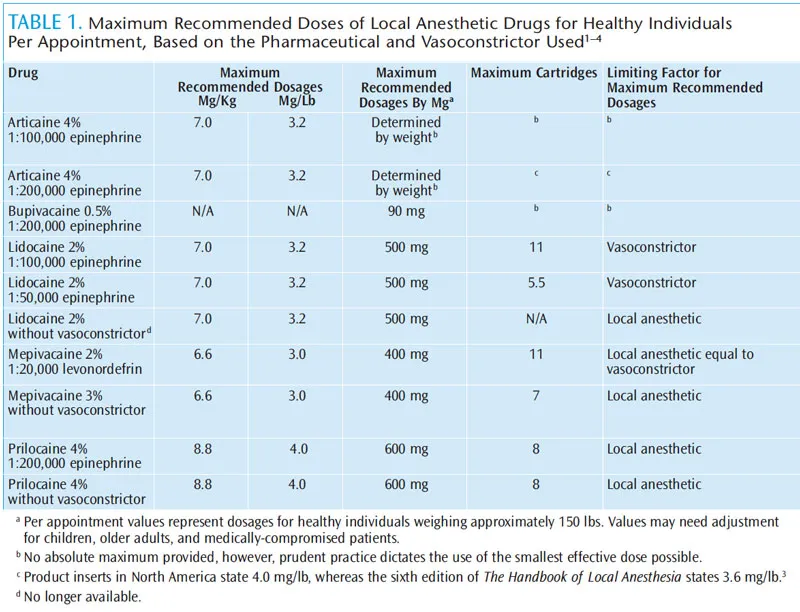
Block Assessment Protocol provides systematic evaluation at predetermined intervals to ensure adequate anesthesia and identify complications early. 15-minute assessment determines block progression, while 30-minute evaluation confirms surgical readiness or need for supplementation.
| Time Point | Assessment Parameters | Success Criteria | Failure Actions |
|---|---|---|---|
| 5 minutes | Sensory onset, patient comfort | Tingling/numbness present | Continue monitoring |
| 15 minutes | Sensory level, motor function | Loss of sharp sensation | Consider supplementation |
| 30 minutes | Complete block assessment | Surgical anesthesia achieved | Supplement or convert |
| 60 minutes | Block stability, complications | Maintained anesthesia | Monitor for regression |
| Post-op | Recovery progression, complications | Appropriate regression | Manage complications |
⭐ Clinical Pearl: Lipid emulsion therapy should be immediately available for any procedure using >100mg bupivacaine or >300mg lidocaine, with 1.5 mL/kg bolus followed by 0.25 mL/kg/min infusion for systemic toxicity
Supplementation Strategy Protocol addresses inadequate blocks through systematic approaches that maximize success while minimizing additional risk. Volume supplementation improves spread, while concentration adjustment enhances block density for surgical requirements.
- Supplementation Decision Matrix
- Patchy sensory block: Add 5-10mL of same concentration
- Success rate: 70-80% with additional volume
- Time to effect: 10-15 minutes for improvement
- Inadequate motor block: Increase concentration by 0.25-0.5%
- Bupivacaine 0.25% → 0.5% for surgical anesthesia
- Lidocaine 1% → 1.5-2% for dense blockade
- Complete block failure: Consider alternative technique
- Success rate: <30% with repeat same approach
- Time factor: surgical delay vs general anesthesia
- Patchy sensory block: Add 5-10mL of same concentration
Recovery Monitoring Protocol ensures safe emergence from regional anesthesia through systematic assessment of motor function, sensory recovery, and complication surveillance. Standardized discharge criteria prevent premature mobilization and associated injuries.
💡 Master This: Block regression assessment requires hourly evaluation until protective sensation returns, with specific attention to motor function recovery before patient mobilization to prevent falls and injuries
Quality Improvement Integration incorporates outcome tracking and complication analysis to refine protocols and improve performance. Success rates >95%, complication rates <2%, and patient satisfaction scores >90% represent benchmark targets for regional anesthesia programs.
- Key Performance Indicators
- Block success rate: >95% for experienced practitioners
- Supplementation rate: <10% with proper technique
- Systemic toxicity: <0.1% with dose adherence
- Patient satisfaction: >90% with adequate counseling
- Complication rate: <2% overall adverse events
📌 Remember: TRACK - Time intervals for assessment, Recognize complications early, Algorithmic responses, Continuous monitoring, Keep detailed records
These evidence-based protocols transform local anesthetic practice from intuitive art to systematic science, ensuring consistent outcomes while maintaining the highest safety standards across all clinical applications.
⚖️ Treatment Algorithms: Evidence-Based Management Protocols
🔗 Advanced Integration: Multi-System Mastery
Cardiovascular Integration Patterns reveal how regional anesthesia modulates hemodynamic responses through sympathetic blockade and direct myocardial effects. Neuraxial blocks above T4 level produce significant hypotension through sympathetic denervation, while peripheral blocks provide cardiovascular stability with minimal systemic effects.
📌 Remember: HEART - Hypotension with high blocks, Epinephrine effects, Arrhythmia risk with bupivacaine, Reduced stress response, Toxicity varies by agent
- Sympathetic Blockade Levels
- T1-T4 blockade: Cardiac sympathetics affected
- Heart rate reduction: 20-30% from baseline
- Contractility decrease: 15-25% reduction
- Coronary vasodilation: improved perfusion
- T5-T10 blockade: Splanchnic sympathetics blocked
- Venous pooling: 30-40% capacity increase
- Preload reduction: significant hypotension risk
- GI motility: enhanced peristalsis
- T11-L2 blockade: Lower extremity sympathetics
- Vasodilation: increased limb blood flow
- Temperature elevation: 2-3°C in blocked region
- Minimal hemodynamic impact
- T1-T4 blockade: Cardiac sympathetics affected
Respiratory System Integration demonstrates how regional techniques preserve pulmonary function while reducing opioid requirements and associated respiratory depression. Intercostal blocks may reduce vital capacity by 5-10%, while epidural anesthesia above T6 can impair accessory muscle function and cough effectiveness.
| Block Level | Respiratory Impact | Vital Capacity | Cough Function | Clinical Significance |
|---|---|---|---|---|
| C3-C5 (Phrenic) | Diaphragm paralysis | 50-75% reduction | Severely impaired | Avoid bilateral blocks |
| T1-T6 (Upper thoracic) | Accessory muscle loss | 15-25% reduction | Moderately impaired | Monitor high-risk patients |
| T6-T12 (Lower thoracic) | Intercostal weakness | 5-15% reduction | Mildly impaired | Generally well tolerated |
| Below T12 | Minimal impact | <5% change | Normal | No respiratory concerns |
⭐ Clinical Pearl: Regional anesthesia reduces perioperative insulin requirements in diabetic patients by 25-40% through decreased stress hormone release and improved glucose homeostasis, enabling better glycemic control
Pharmacokinetic Integration reveals how patient factors and co-administered drugs modify local anesthetic behavior. Alpha-1 acid glycoprotein levels increase protein binding during acute illness, potentially reducing free drug concentrations and requiring dose adjustments for optimal effect.
Synergistic Drug Interactions enable enhanced efficacy while reducing individual drug requirements and associated side effects. Dexamethasone 4-8mg prolongs local anesthetic duration by 6-12 hours through anti-inflammatory effects and sodium channel modulation.
- Proven Adjuvant Synergies
- Epinephrine 1:200,000: Duration extension 50-100%
- Mechanism: vasoconstriction reduces systemic absorption
- Contraindications: end-artery locations, severe CAD
- Dexamethasone 4-8mg: Analgesia prolongation 6-12 hours
- Mechanism: anti-inflammatory and direct neural effects
- Benefits: no motor block extension, reduced PONV
- Clonidine 1-2 μg/kg: Duration increase 2-4 hours
- Mechanism: alpha-2 agonism and hyperpolarization
- Side effects: sedation, hypotension, bradycardia
- Epinephrine 1:200,000: Duration extension 50-100%
Cutting-Edge Integration Concepts incorporate recent research findings that revolutionize clinical practice. Liposomal bupivacaine provides 72-hour analgesia through sustained release technology, while perineural dexmedetomidine offers opioid-sparing analgesia with minimal systemic effects.
💡 Master This: Multimodal analgesia integration combining regional blocks, systemic adjuvants, and topical agents reduces opioid consumption by 70-90% while improving pain scores and accelerating recovery
Patient-Specific Integration Strategies customize anesthetic approaches based on individual physiology, comorbidities, and genetic factors. CYP2D6 poor metabolizers show prolonged local anesthetic effects, while patients with sodium channelopathies demonstrate enhanced sensitivity requiring dose modifications.
- Personalized Medicine Factors
- Genetic polymorphisms: CYP enzyme variants affect metabolism
- CYP2D6 poor metabolizers: 25% of population
- Prolonged effect: 2-3x normal duration
- Age-related changes: Decreased clearance in elderly
- Dose reduction: 25-30% for patients >70 years
- Increased sensitivity: enhanced neural uptake
- Disease-specific modifications: Organ dysfunction impacts
- Liver disease: amide metabolism impaired
- Kidney disease: metabolite accumulation possible
- Genetic polymorphisms: CYP enzyme variants affect metabolism
Outcome Optimization Integration combines evidence-based protocols with real-time monitoring to maximize benefits while minimizing risks. Enhanced recovery protocols incorporating regional anesthesia reduce hospital length of stay by 1-2 days and improve patient satisfaction scores by 15-25%.
📌 Remember: INTEGRATE - Individualize approaches, Neuraxial vs peripheral, Timing optimization, Endocrine benefits, Genetic factors, Respiratory preservation, Adjuvant synergies, Toxicity prevention, Enhanced recovery
This advanced integration framework transforms local anesthetic practice from single-system focus to holistic patient care, enabling precision medicine approaches that optimize outcomes across multiple physiological domains while maintaining safety and improving patient experience.
🔗 Advanced Integration: Multi-System Mastery
🎯 Clinical Mastery Arsenal: Rapid Reference Framework

Essential Numbers Arsenal provides critical thresholds and safety limits that prevent complications and optimize outcomes. Master practitioners instantly recall these quantitative benchmarks that guide dosing decisions, timing assessments, and safety monitoring.
📌 Remember: NUMBERS - Never exceed max doses, Unionized fraction determines onset, Minutes to peak effect, Binding affects duration, Elimination varies by class, Recovery follows sequence, Safety margins essential
-
Critical Dose Thresholds (mg/kg)
- Lidocaine: 4.5 plain, 7 with epi
- Bupivacaine: 2.5 (no epi benefit)
- Ropivacaine: 3 maximum safe dose
- Chloroprocaine: 15-20 (highest safety margin)
-
Timing Benchmarks (minutes)
- Onset assessment: 15 minutes for all agents
- Peak effect: 30 minutes for long-acting
- Failure threshold: 45 minutes without effect
- Supplementation window: 30-60 minutes optimal
Rapid Assessment Protocol enables systematic evaluation in <2 minutes to determine block adequacy, complication presence, and intervention needs. This streamlined approach prevents delays while ensuring comprehensive safety assessment.
| Assessment Domain | Quick Test | Normal Response | Abnormal Findings | Immediate Action |
|---|---|---|---|---|
| Sensory Block | Pinprick test | No sharp sensation | Partial/absent loss | Supplement or convert |
| Motor Function | Hand grip/foot flex | Appropriate weakness | Unexpected strength | Reassess technique |
| Sympathetic Block | Temperature change | Warm, dry skin | Cool, normal color | Check block level |
| Systemic Effects | Mental status | Alert, oriented | Confusion, agitation | LAST protocol |
| Cardiovascular | BP, HR monitoring | Stable vitals | Hypotension, arrhythmia | Hemodynamic support |
⭐ Clinical Pearl: "20-20-20 Rule" for LAST management - 20mL lipid bolus, 20mL/min infusion, 20 minutes of aggressive resuscitation before considering extracorporeal support
Agent Selection Matrix enables instant matching of patient factors with optimal agents through systematic decision trees. This rapid-fire approach eliminates analysis paralysis while ensuring evidence-based choices.
- High-Speed Selection Criteria
- Cardiac risk present: Ropivacaine or Chloroprocaine
- Pregnancy: Lidocaine, avoid Bupivacaine
- Outpatient surgery: Mepivacaine or Lidocaine
- Long procedure: Bupivacaine or Ropivacaine
- Rapid onset needed: Lidocaine or Chloroprocaine
Troubleshooting Rapid Response addresses common problems with immediate solutions that salvage procedures and maintain patient safety. These proven interventions represent collective wisdom from expert practitioners.
💡 Master This: "Rule of 15s" - Assess at 15 minutes, supplement by 30 minutes, convert by 45 minutes if inadequate - this timeline prevents delays while maximizing success rates
Quality Metrics Dashboard provides performance benchmarks that define excellence in regional anesthesia practice. These quantitative targets enable continuous improvement and outcome optimization.
- Excellence Benchmarks
- Success rate: >95% first-attempt blocks
- Complication rate: <2% overall adverse events
- Supplementation rate: <10% additional interventions
- Patient satisfaction: >90% positive feedback
- Block duration: Within 20% of predicted time
Emergency Drug Calculations provide instant dosing for critical situations without mathematical delays. These pre-calculated values enable immediate intervention during life-threatening complications.
| Patient Weight | Lipid 20% Bolus | Lipid Infusion | Epinephrine 1:10,000 | Atropine |
|---|---|---|---|---|
| 50 kg | 75 mL | 75 mL/hr | 0.5 mL (50 μg) | 0.5 mg |
| 70 kg | 105 mL | 105 mL/hr | 0.7 mL (70 μg) | 0.5 mg |
| 90 kg | 135 mL | 135 mL/hr | 0.9 mL (90 μg) | 0.5 mg |
| 110 kg | 165 mL | 165 mL/hr | 1.1 mL (110 μg) | 0.5 mg |
📌 Remember: PEARLS - Patient factors modify response, Epinephrine extends duration, Assess systematically, Recognize complications early, Lipid rescue for toxicity, Supplementation has time limits
- Master Practitioner Insights
- Alkalinization speeds onset but doesn't improve quality
- Epinephrine contraindicated in digital blocks
- Test dose unreliable for detecting intravascular injection
- Motor block regression precedes sensory recovery
- Lipid emulsion effective for all LA toxicity
This clinical mastery arsenal transforms complex decision-making into systematic excellence, enabling confident practice under any clinical circumstances while maintaining optimal patient outcomes and safety standards.
🎯 Clinical Mastery Arsenal: Rapid Reference Framework
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























