ERAS & RA Fundamentals - Synergistic Duo
- ERAS (Enhanced Recovery After Surgery):
- A multimodal, multidisciplinary, evidence-based pathway.
- Core Goals: Minimize surgical stress, accelerate physiological recovery, reduce LOS & complications.
- RA (Regional Anesthesia) in ERAS:
- A cornerstone for achieving ERAS objectives.
- Provides: Superior, targeted analgesia; blunts neuroendocrine stress response.
- Key Benefits:
- Significant opioid-sparing effect (↓ PONV, sedation, ileus, respiratory depression).
- Facilitates early mobilization and return of gut function.
- Synergy: RA is pivotal, enabling multiple ERAS elements for improved patient outcomes.
⭐ Thoracic epidural analgesia (TEA) is a cornerstone RA technique in ERAS for major abdominal/thoracic surgery, significantly improving pain control and hastening gut recovery.

RA Modalities in ERAS - The Anesthetist's Toolkit
- Neuraxial Anesthesia: Cornerstone for major surgeries.
- Epidural (Thoracic/Lumbar): Catheters for continuous analgesia. ↓opioids, ↓ileus.
- Spinal: Single-shot or continuous. Rapid, dense block.
- Peripheral Nerve Blocks (PNBs): Targeted, opioid-sparing; Ultrasound-Guided (USG) standard.
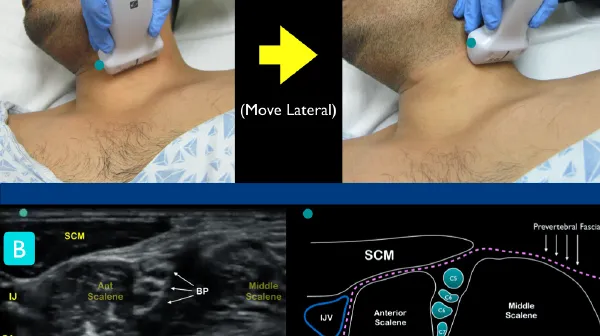
- Upper Limb: Interscalene, Supraclavicular.
- Lower Limb: Femoral, Sciatic, Adductor Canal Block (ACB).
- Truncal: Paravertebral, Intercostal.
- Fascial Plane Blocks (FPBs): USG-guided, volume-dependent spread.
- TAP: Anterior abdominal wall.
- QL (Quadratus Lumborum): Abdominal analgesia (somatic/visceral).
- ESP (Erector Spinae Plane): Thoracic/abdominal wall.
- PECS/Serratus Anterior: Chest wall.
- Local Infiltration Analgesia (LIA): Surgeon-administered; common in arthroplasty.
⭐ Adductor canal block post-Total Knee Arthroplasty (TKA) offers analgesia comparable to femoral nerve block but with significantly better quadriceps strength preservation, crucial for early mobilization in ERAS.
RA Benefits & Pathways - Speedy Recovery Catalysts
- Core RA Benefits for ERAS:
- Opioid Sparing: ↓ opioid-related side effects (e.g., sedation, respiratory depression, PONV, pruritus).
- Superior Postoperative Analgesia: Lower pain scores, ↑ patient comfort & satisfaction.
- Facilitates Early Mobilization: Key for VTE prevention, faster overall recovery.
- Reduced Postoperative Nausea & Vomiting (PONV): Both direct effect & secondary to opioid reduction.
- Accelerated Return of Bowel Function: ↓ incidence/duration of postoperative ileus.
- Attenuation of Surgical Stress Response: Modulates neuroendocrine changes.
- Potential for ↓ hospital Length Of Stay (LOS) & costs.
- RA in Specific ERAS Pathways:
- Colorectal Surgery: Thoracic Epidural Analgesia (TEA) (e.g., T6-T10), Transversus Abdominis Plane (TAP) blocks, Quadratus Lumborum (QL) blocks.
- Orthopedic Surgery (TKR/THR): Spinal anesthesia, Epidural, Peripheral Nerve Blocks (PNBs) like femoral, adductor canal, sciatic, iPACK (infiltration between popliteal artery and capsule of knee).
- Thoracic/Cardiac Surgery: Paravertebral Blocks (PVB), Erector Spinae Plane (ESP) blocks, intercostal nerve blocks.
⭐ Thoracic epidural analgesia (TEA) is a cornerstone in many major abdominal surgery ERAS protocols, offering profound analgesia and sympathetic blockade, which aids early gut recovery and mobilization.
RA Selection & Safety - Prudent Pain Protocol
- Goal: Optimize analgesia, ↓opioids, facilitate recovery.
- Selection Criteria:
- Patient: Co-morbidities (esp. coagulopathy), consent.
- Surgery: Type, duration, anticipated pain level.
- Technique: Epidural, PNBs (e.g., TAP, ESP, QLB), spinal.
- Safety First:
- Strict asepsis.
- Ultrasound guidance preferred for PNBs.
- Monitor for LAST, nerve injury, hematoma.
- ⚠️ Adherence to anticoagulation guidelines (ASRA) is paramount.
⭐ For neuraxial techniques, specific timing for anticoagulant interruption & resumption is crucial. E.g., LMWH prophylactic dose: wait 10-12 hours before block, restart 4 hours post-catheter removal.
High‑Yield Points - ⚡ Biggest Takeaways
- Reduces opioid consumption and related side effects (nausea, vomiting, ileus).
- Improves postoperative pain control, facilitating early mobilization.
- Common techniques: epidural analgesia, spinal anesthesia, peripheral nerve blocks (PNBs).
- Thoracic epidural analgesia (TEA) is gold standard for major abdominal/thoracic surgery.
- PNBs (e.g., TAP blocks, femoral nerve blocks) are crucial for orthopedic and abdominal surgeries.
- Catheter-based techniques allow prolonged analgesia.
- Contributes to reduced hospital stay and improved patient satisfaction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

