Classification & Initial Signs - Red Alert Signals
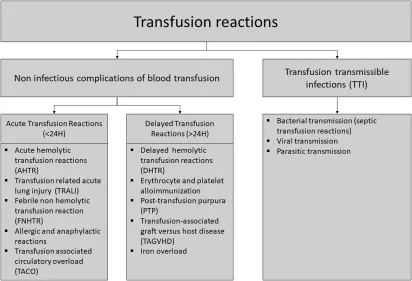
Classification:
Initial Signs (Red Alert Signals):
- Fever (Temp ↑ >1°C or >38°C), chills/rigors (Most common)
- Hypotension (SBP ↓ >30mmHg), tachycardia (HR ↑ >20bpm)
- Respiratory distress: dyspnea, tachypnea, hypoxia
- Hemoglobinuria (red/dark urine), oliguria
- Skin: Urticaria, rash, pruritus, flushing
- Pain: Chest, back, flank, infusion site
- Nausea/Vomiting
- Anxiety, sense of impending doom
- Under Anesthesia: Unexplained hypotension, hemoglobinuria, diffuse oozing.
⭐ Fever is the most common sign of a transfusion reaction. In anesthetized patients, unexplained hypotension or hemoglobinuria may be the first sign of Acute Hemolytic Transfusion Reaction (AHTR).
Acute Immune Reactions - Rapid Response Havoc
Immediate, antibody-mediated responses to transfused blood components. Require prompt recognition and intervention.
- Acute Hemolytic Transfusion Reaction (AHTR)
- Cause: ABO incompatibility (IgM); intravascular hemolysis.
- Sx: Fever, chills, hypotension, hemoglobinuria, flank pain, DIC. Under GA: unexplained hypotension, oozing.
- 📌 Mnemonic: Hemolysis Alters Vitals Output Clotting (HAVOC)
- Febrile Non-Hemolytic (FNHTR)
- Cause: Anti-leukocyte Abs or cytokines.
- Sx: Temp ↑ ≥ 1°C, chills.
- Tx: Stop, antipyretics. Prevent: Leukoreduction.
- Allergic & Anaphylactic Reactions
- Urticarial: Hives, pruritus. Tx: Antihistamines.
- Anaphylaxis: Severe hypotension, bronchospasm. IgA deficiency risk. Tx: Epinephrine, steroids.
⭐ AHTR is the most feared acute reaction, often due to clerical error leading to ABO incompatibility.
Delayed & Non-Immune Issues - Slow Burn & Sneaky Foes
- Delayed Hemolytic Transfusion Reaction (DHTR)
- Onset: >24h (typ. 3-30d)
- Cause: Anamnestic Ab (Kidd, Duffy, Kell) to RBCs
- Sx: Mild jaundice, fever, unexpected ↓Hb, +DAT
- Transfusion-Associated Graft-vs-Host Disease (TA-GVHD)
- Onset: 1-2w; highly fatal (mortality >90%)
- Cause: Donor T-lymphocytes attack recipient tissues
- Sx: Rash, fever, diarrhea, pancytopenia, ↑LFTs
⭐ TA-GVHD: Prevent with irradiated blood for at-risk (immunocompromised, relative donors, HLA-matched).
- Post-Transfusion Purpura (PTP)
- Onset: 5-10d post-transfusion
- Cause: Alloantibodies to platelet antigens (usu. HPA-1a)
- Sx: Severe thrombocytopenia (plt <10,000/µL), bleeding
- Iron Overload (Transfusional Hemosiderosis)
- Cause: Chronic transfusions (1 unit ≈ 200-250mg Fe)
- Effects: Cardiac, hepatic, endocrine dysfunction
- Tx: Iron chelation
- Transfusion-Transmitted Infections (TTIs)
- Viral: HBV, HCV, HIV (window period risk; screening ↓ risk)
- Parasitic: Malaria, Babesiosis (region-dependent)
Massive Transfusion & Prevention - The Big Pour Fixes
Definition: >10U pRBCs/24h, or >1 blood vol/24h, or >50% blood vol/4h. 📌 Risk: "Lethal Triad" (Hypothermia, Acidosis, Coagulopathy).
- Key Complications & Management:
- Hypothermia: ↓Coagulation. Warm fluids/blood.
- Acidosis: ↓Myocardial function. Correct cause.
- Coagulopathy: Dilutional. Use 1:1:1 (pRBC:FFP:PLT).
- Hypocalcemia (Citrate): Arrhythmias. Give $Ca^{2+}$ (e.g., 1g CaCl2 / 4-6U pRBCs).
- Hyperkalemia (Stored blood): Arrhythmias. Monitor, Rx for $K^{+}$.
- ↓2,3-DPG: Left shift ODC.
- Damage Control Resuscitation (DCR) Principles:
- Permissive hypotension (SBP 80-90 mmHg, no TBI).
- Monitor: Temp, ABG, $Ca^{2+}$, $K^{+}$, Coags (TEG/ROTEM).
- TXA: 1g load, then 1g/8h.
⭐ A target ratio of platelets:FFP:RBCs of 1:1:1 in massive transfusion is associated with improved 6-hour and 24-hour survival in trauma patients.
High‑Yield Points - ⚡ Biggest Takeaways
- AHTR: ABO incompatibility causes fever, chills, hemoglobinuria, DIC. Stop transfusion immediately.
- FNHTR: Most common reaction; cytokines from donor WBCs. Prevent with leukoreduction.
- TRALI: Non-cardiogenic pulmonary edema within 6 hours; donor antibodies. Leading transfusion mortality.
- TACO: Cardiogenic pulmonary edema from volume overload. Manage with diuretics, slow transfusion.
- Massive Transfusion: Risks: hypothermia, dilutional coagulopathy, hypocalcemia (citrate toxicity), hyperkalemia.
- Allergic Reactions: Urticaria common (antihistamines); anaphylaxis rare (epinephrine), potentially fatal.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

