Fast-Track Cardiac Anesthesia - Speedy Recovery Kickstart
- Definition: A coordinated perioperative approach to accelerate physiological recovery and reduce hospital stay after cardiac surgery.
- Primary Goals:
- Early tracheal extubation (target <6 hours).
- ↓ ICU and overall hospital stay.
- ↓ Costs, ↑ resource utilization.
- Enhanced patient satisfaction and comfort.
- Key Program Components:
- Careful patient selection.
- Opioid-sparing anesthetic techniques (e.g., regional, short-acting IV agents).
- Multimodal analgesia.
- Proactive nausea/vomiting control.
- Early mobilization and nutrition.
⭐ The primary goal of fast-track cardiac anesthesia is tracheal extubation within 6 hours post-surgery.
Fast-Track Cardiac Anesthesia - The Right Fit Fast
Aims for early extubation & ICU discharge. Key: meticulous patient selection.
Selection Criteria:
| Aspect | Favorable (Inclusion) | Unfavorable (Exclusion) |
|---|---|---|
| Surgery | Elective | Emergency, Redo-surgery |
| LV Function | LVEF > 40% | LVEF < 30% |
| Age | < 75 yrs | Significant frailty |
| BMI | < 35 kg/m² | Morbid obesity |
| Coagulopathy | None severe | Severe coagulopathy |
| Comorbidities | Well-controlled | Severe pulm HTN, unstable comorbidities |
- Fit patient
- Adequate LVF (LVEF > 40%)
- Stable
- Team approach
- Contraindications: Acute MI, Re-op difficult
Preoperative Optimization:
- Optimize comorbidities (DM, HTN).
- Enhance cardiac status.
- Patient education.
⭐ Patients with preoperative LVEF <30% are generally poor candidates for fast-track protocols.
Fast-Track Cardiac Anesthesia - Speedy & Smooth Sailing
Aims for early extubation (<6 hrs) & reduced ICU stay.
-
Anesthetic Agents:
- Opioids: Remifentanil, Sufentanil (short-acting).
- Volatiles: Sevoflurane, Desflurane (rapid offset).
- NMBs: Rocuronium + Sugammadex (rapid reversal).
- Target BIS: 40-60.
Agent Type Fast-Track Edge Remifentanil Opioid Ultra-short context-sensitive HT Sufentanil Opioid Potent, short duration Sevoflurane Volatile Low solubility, smooth recovery Desflurane Volatile Very low solubility, rapid offset Rocuronium NMB Rapid onset Sugammadex Reversal Rapid Rocuronium reversal -
Techniques:
- Opioid-sparing: Multimodal analgesia.
- Balanced anesthesia: Synergistic agent use.
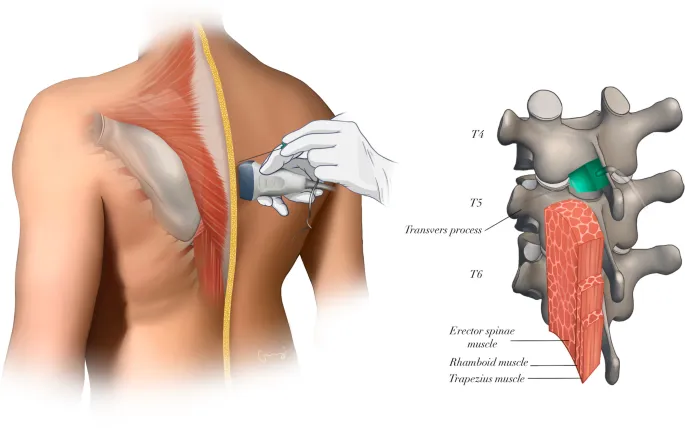
- Regional blocks: Paravertebral (PVB), Erector Spinae Plane (ESP).
-
Intraoperative Care:
- Goal-Directed Fluid Therapy (GDFT).
- Normothermia: Target 36-37°C.
- TEE for hemodynamic monitoring.
⭐ Remifentanil infusion is common due to its ultra-short context-sensitive half-time, aiding rapid awakening.
Fast-Track Cardiac Anesthesia - Quick Exit Strategy
- Goal: Rapid extubation & ICU discharge.
- Extubation Criteria (Key):
- Hemodynamic stability (e.g., MAP >65 mmHg, low inotropes)
- Normothermia (>36°C)
- Minimal bleeding: <1.5 ml/kg/hr
- PaO2/FiO2 ratio: >200
- Adequate consciousness: GCS >13
- Effective pain control
- 📌 Mnemonic: AWAKE & READY (Airway clear, Warm, Adequate Vitals, K+ normal, Extubation criteria met/Resp mechanics good, Analgesia effective, Drains minimal, You cooperative)
- Multimodal Analgesia: Key to ↓opioids. Includes paracetamol, NSAIDs (cautious), gabapentinoids, regional blocks.
- Early Mobilization: Crucial for recovery; implement protocols.
- Barriers to Fast-Tracking: Bleeding, arrhythmias, respiratory insufficiency, delirium.
⭐ Effective multimodal analgesia is paramount to minimize opioid consumption and facilitate early extubation and ambulation.
High‑Yield Points - ⚡ Biggest Takeaways
- Primary goal: Early extubation (typically <6 hours post-op) and reduced ICU/hospital stay.
- Utilizes short-acting opioids (e.g., remifentanil), volatile agents (e.g., desflurane), and regional anesthesia.
- Strict patient selection is crucial; avoids complex cases or severe comorbidities.
- Multimodal analgesia (e.g., NSAIDs, paracetamol, nerve blocks) is key for opioid-sparing.
- Benefits include lower costs, reduced ventilator-associated pneumonia (VAP), and faster recovery.
- Requires normothermia maintenance and minimal fluid overload for optimal outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more