ANS Thorax Overview - The Thoracic Conductors
- ANS: Controls involuntary thoracic visceral functions.
- Key Players:
- Sympathetic: Thoracolumbar (T1-L2) origin; ganglia in sympathetic chain. "Fight or flight."
- Parasympathetic: Craniosacral origin; Vagus (CN X) nerve dominates thorax. "Rest and digest."
- Plexuses: Cardiac, pulmonary, esophageal - nerve networks coordinating organ function.
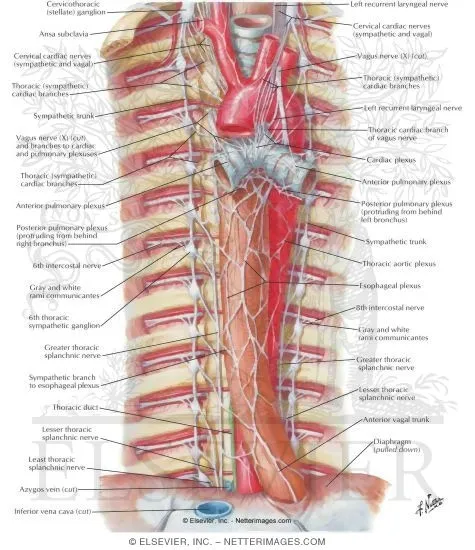
⭐ Thoracic organs typically have dual innervation: Sympathetic (mainly Norepinephrine, NE) and Parasympathetic (Acetylcholine, ACh), often with antagonistic actions to maintain homeostasis.
Sympathetic Thorax - Thoracic Turbocharge
- Origin: Lateral horns of T1-L2 spinal cord.
- Thoracic visceral outflow: T1-T5 segments; fibers synapse in paravertebral ganglia, forming cardiopulmonary nerves.
- Lower thoracic segments (T5-T12) form preganglionic splanchnic nerves (greater, lesser, least) passing to abdominal prevertebral ganglia.
- Ganglia: Paravertebral ganglia of the sympathetic trunk.
- Actions: ↑ Heart rate & contractility, bronchodilation, vasoconstriction (not coronaries), piloerection, sweating.
- 📌 Mnemonic: "T1-T5 for Thoracic Sympathy" (cardiopulmonary).

⭐ Cardiopulmonary splanchnic nerves are largely postganglionic sympathetic fibers, arising from cervical and upper thoracic paravertebral ganglia (T1-T5).
Parasympathetic Thorax - Vagal Serenity
- Primary Nerve: Vagus (CN X); originates from medulla oblongata.
- Thoracic Course & Key Trunks:
- Enters via superior thoracic aperture.
- Right Vagus: Forms posterior esophageal plexus & posterior vagal trunk.
- Left Vagus: Forms anterior esophageal plexus & anterior vagal trunk.
- Major Plexuses: Cardiac, pulmonary, esophageal.
- Actions (Acetylcholine on Muscarinic receptors):
- Heart: ↓ rate, ↓ contractility.
- Lungs: Bronchoconstriction, ↑ glandular secretions.
- Esophagus: ↑ peristalsis, ↑ secretions.
- 📌 Vagus nerve branches: Cardiac, Pulmonary, Esophageal.
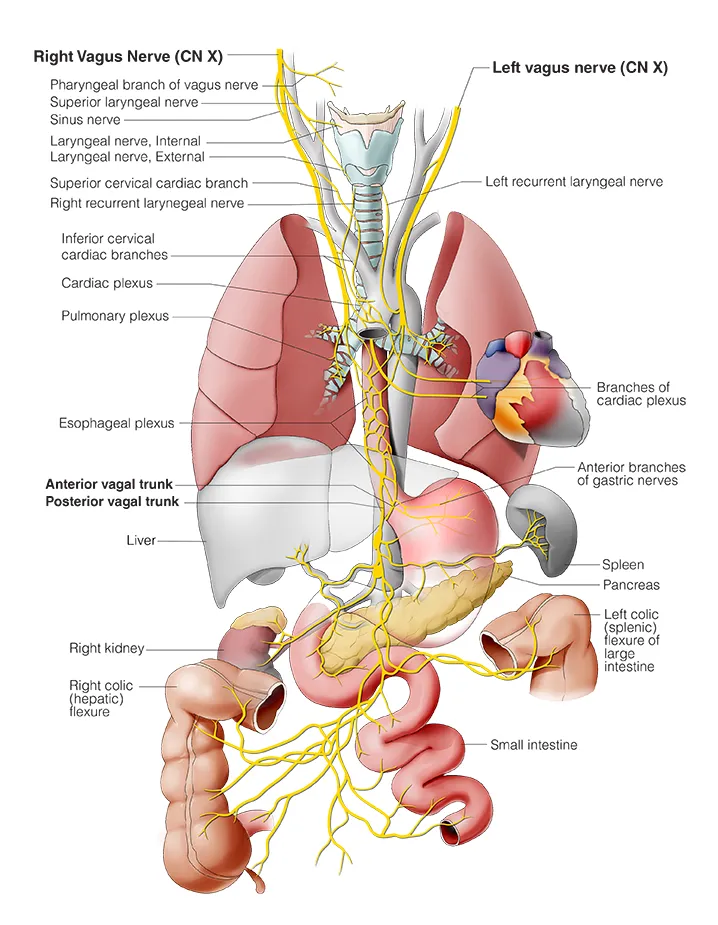
⭐ The left vagus nerve contributes to the anterior esophageal plexus and anterior vagal trunk.
Thoracic Autonomic Plexuses - Visceral Switchboards
These plexuses are networks of sympathetic and parasympathetic nerves that innervate thoracic viscera. They allow for integrated autonomic control.

| Plexus | Formation (S; P) | Location | Functions/Targets |
|---|---|---|---|
| Cardiac Plexus | S: Cervical & T1-T5 ganglia; P: Vagus n. (CN X) | Superficial: Inf. to aortic arch; Deep: Post. to aortic arch, Ant. to tracheal bifurcation | Heart (rate, contractility), coronary arteries |
| Pulmonary Plexus | S: T2-T5 ganglia; P: Vagus n. (CN X) | Ant. & Post. to lung roots | Lungs (bronchi, vessels), visceral pleura |
| Esophageal Plexus | S: T5-T6 ganglia; P: Vagus n. (CN X) → Vagal trunks | Surrounds esophagus | Esophagus (peristalsis, glands) |
These plexuses ensure coordinated responses of thoracic organs to autonomic signals.
Clinical Insights - Thoracic Nerve Dramas
- Horner's Syndrome: Classic triad (ptosis, miosis, anhydrosis). Caused by sympathetic trunk lesion (e.g., Pancoast tumor).
- Referred Pain:
- Cardiac (MI) → T1-T4 dermatomes (left arm, chest).
- Diaphragmatic irritation (phrenic nerve C3-C5) → shoulder tip pain.
- Achalasia Cardia: ↓ esophageal motility; loss of myenteric plexus ganglion cells.
- Raynaud's Disease: Peripheral vasospasm; thoracic sympathectomy for severe cases.

⭐ Referred pain from myocardial ischemia is often felt in T1-T4 dermatomes due to shared spinal segments with afferent sympathetic fibers.
High‑Yield Points - ⚡ Biggest Takeaways
- Sympathetic innervation to the thorax originates from T1-T5/T6 spinal cord segments.
- Preganglionic sympathetic fibers synapse in the sympathetic chain ganglia (paravertebral).
- Postganglionic sympathetic fibers form cardiopulmonary splanchnic nerves to supply viscera.
- Parasympathetic innervation is primarily via the vagus nerve (CN X).
- Vagus nerve carries preganglionic fibers synapsing in intramural ganglia within target organs.
- Key thoracic autonomic plexuses are the cardiac, pulmonary, and esophageal plexuses.
- Visceral pain afferents often travel with sympathetic fibers, explaining referred pain patterns (e.g., cardiac pain).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

