Kidneys: Gross Anatomy - Bean Scene Investigation
- Location: Retroperitoneal, T12-L3 (R lower). Size: ~11x6x3cm, ~150g.
- Coverings (In→Out): Capsule, Perinephric fat, Renal fascia, Paranephric fat. 📌 'Cats Prefer Real Prawns'.
- External: Poles (Sup/Inf), Borders (Med/Lat), Surfaces (Ant/Post). Hilum (medial).
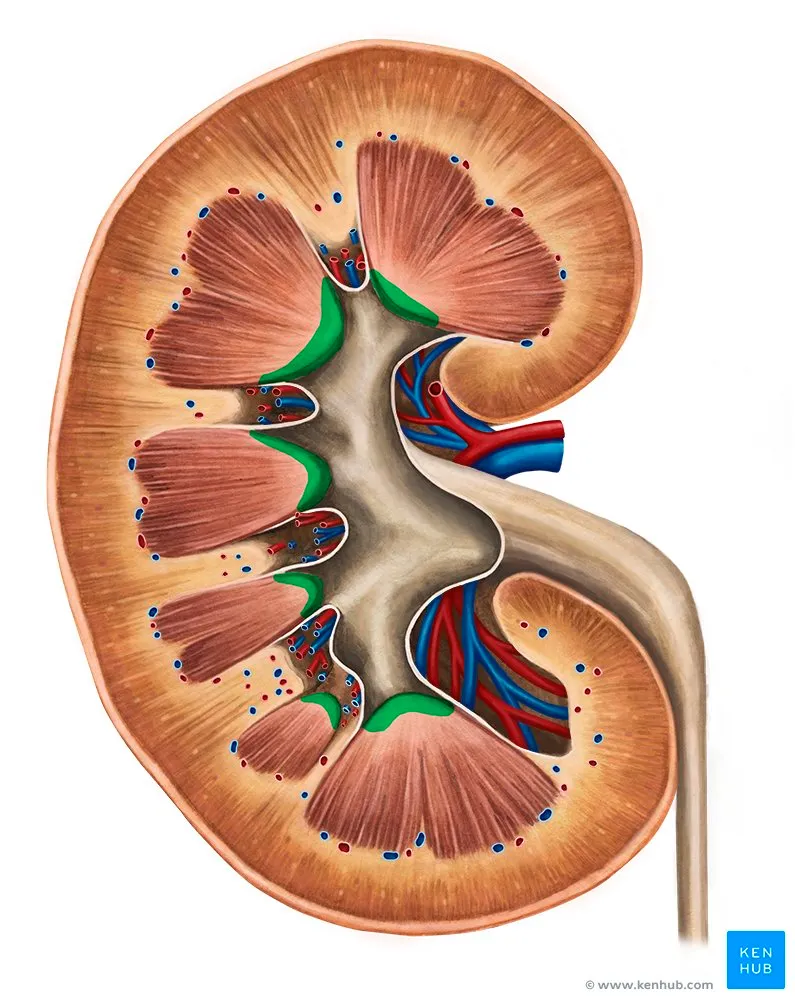
- Internal: Cortex; Medulla (Renal Pyramids 8-18); Columns of Bertin; Papilla → Minor Calyces (7-13) → Major Calyces (2-3) → Renal Pelvis.
- Hilum (Ant→Post): Vein, Artery, Pelvis (VAP).
⭐ The order of structures in the renal hilum from anterior to posterior is Vein, Artery, Pelvis (VAP).
- Arterial Supply: Renal → Segmental → Lobar → Interlobar → Arcuate → Interlobular. 📌 'Real Sexy Ladies Are Intelligent'.
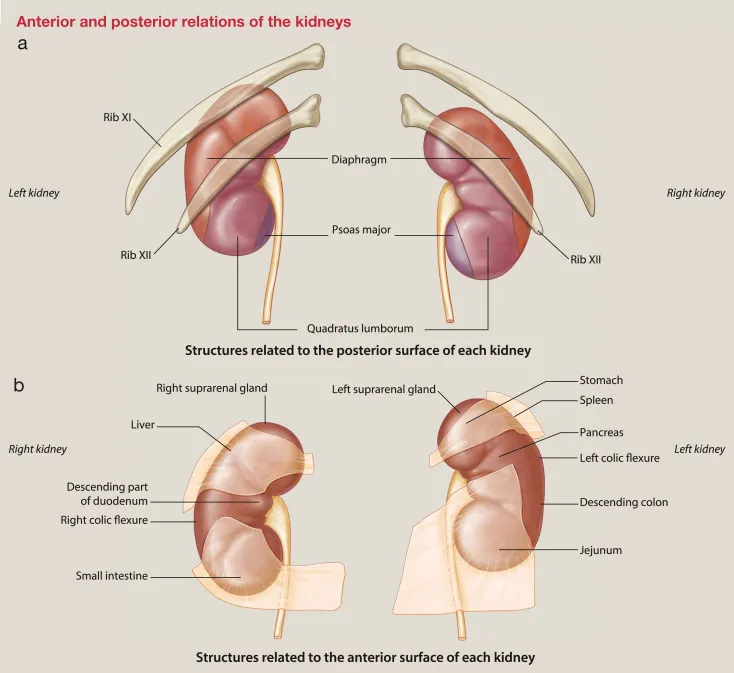
- Relations (Ant): R: Liver, Duodenum. L: Spleen, Pancreas, Stomach. (Post): Diaphragm, Ribs (R:12th, L:11th/12th).
Kidneys: Microscopic Anatomy - Nephron Ninjas
- Nephron Components: Functional unit of the kidney.
- Renal Corpuscle: Glomerulus (capillary tuft) + Bowman's Capsule (parietal: simple squamous; visceral: podocytes).
- Tubules:
- Proximal Convoluted Tubule (PCT): Simple cuboidal, prominent brush border (microvilli) for reabsorption.
- Loop of Henle (LoH): Thin segments (simple squamous), Thick ascending limb (simple cuboidal).
- Distal Convoluted Tubule (DCT): Simple cuboidal, fewer microvilli.
-
Nephron Types:
- Cortical (85%): Short LoH, mainly in cortex; peritubular capillaries.
- Juxtamedullary (15%): Long LoH deep into medulla; vasa recta; vital for urine concentration.
-
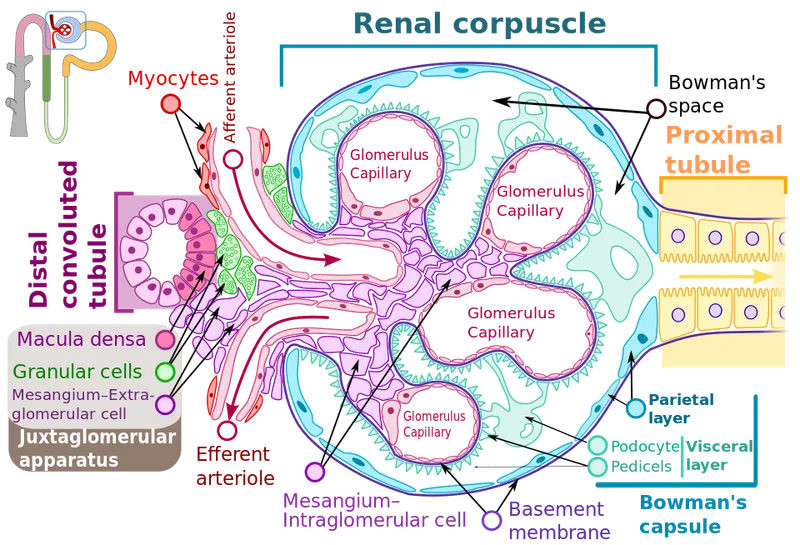
Juxtaglomerular Apparatus (JGA): Regulates GFR & blood pressure.
- Macula Densa: Specialized DCT cells; sense NaCl in tubular fluid.
- Juxtaglomerular (JG) Cells: Modified smooth muscle cells in afferent arteriole wall; secrete renin.
- Extraglomerular Mesangial Cells (Lacis cells).
-
Collecting System:
- Collecting Tubules & Ducts (Cortical/Medullary): Lined by:
- Principal Cells: Reabsorb Na+, secrete K+; ADH-sensitive H2O reabsorption.
- Intercalated Cells (Type A & B): Acid-base balance (H+/HCO3- transport).
- Collecting Tubules & Ducts (Cortical/Medullary): Lined by:
⭐ Juxtaglomerular cells, modified smooth muscle cells in the afferent arteriole wall, secrete renin in response to decreased renal perfusion or low NaCl at macula densa.
Ureters & Bladder - Passage & Pouch
- Ureters
- Course: Abdominal & pelvic; length ≈25-30 cm.
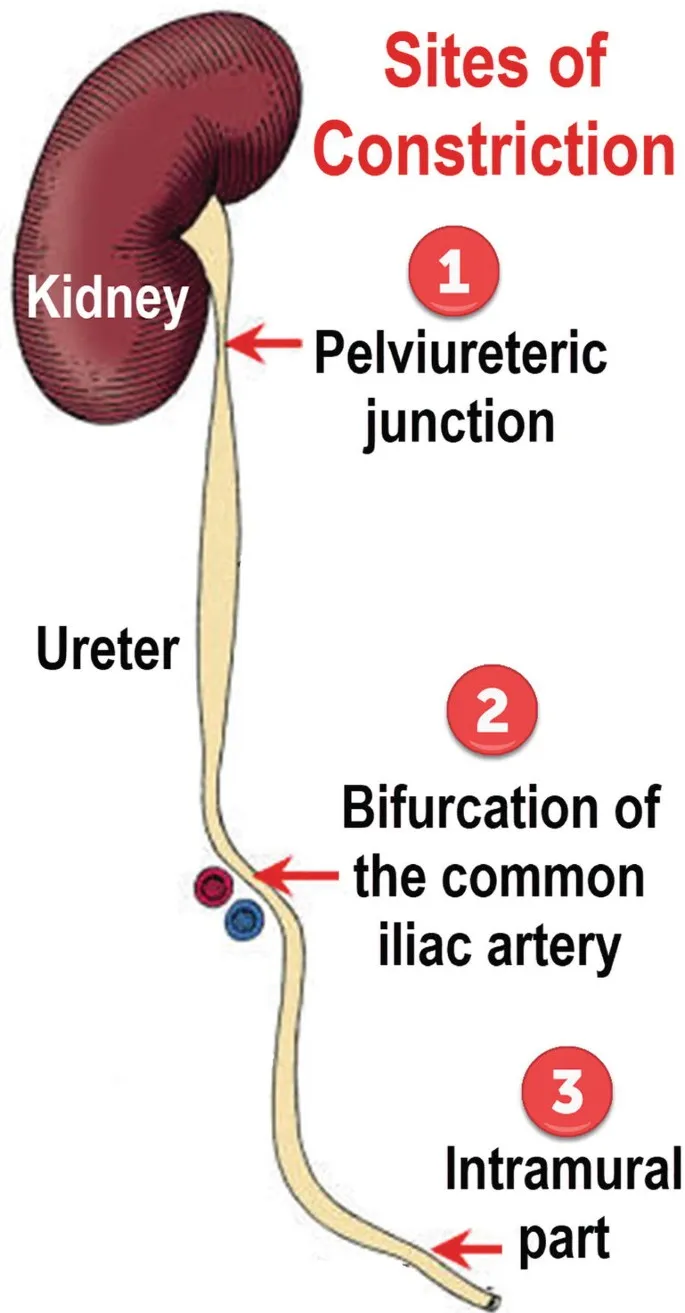
- Constrictions (3): Pelviureteric Junction (PUJ), crossing Pelvic brim/iliac vessels, Vesicoureteric Junction (VUJ). 📌 Mnemonic: 'UP on the Border of Vegas'.
- Blood Supply: Branches from renal, gonadal, aorta, common/internal iliac arteries.
- Histology: Transitional epithelium, 2-3 layers smooth muscle.
- Bladder
- Location: Retropubic; Shape: Tetrahedral (empty).
- Relations: Male (ant. to rectum, sup. to prostate); Female (ant. to uterus/vagina).
- Parts: Apex, body, fundus/base, neck.
- Trigone: Smooth area; boundaries: 2 ureteric orifices (superolateral), internal urethral meatus (inferior).
- Muscle: Detrusor (smooth); Internal urethral sphincter (smooth, involuntary at neck).
- Ligaments: Pubovesical (females), Puboprostatic (males).
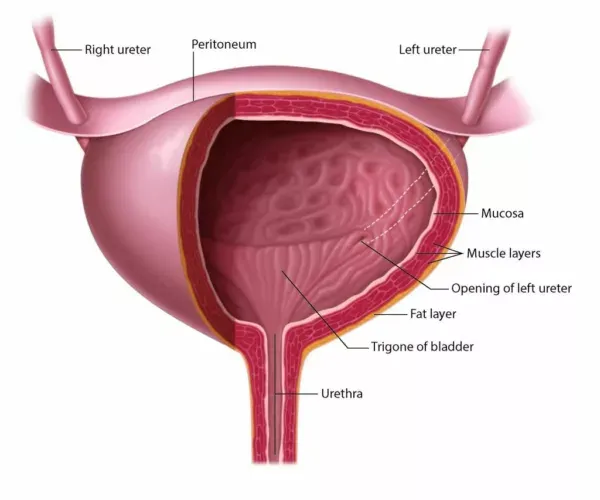
⭐ The three physiological constrictions of the ureter are common sites for calculus impaction: pelviureteric junction, crossing the pelvic brim/common iliac artery, and vesicoureteric junction.
Urethra & Clinical Snippets - Final Flush & Fixes
- Male Urethra:
- Prostatic: 3-4 cm; urethral crest, prostatic sinus.
- Membranous: 1-2 cm; urogenital diaphragm, narrowest, least dilatable.
- Spongy/Penile: 15 cm; corpus spongiosum.
- Sphincters: Internal (involuntary, bladder neck), External (voluntary, urogenital diaphragm).
- Female Urethra: ≈4 cm; anterior to vagina; ↑UTI susceptibility. Sphincters: Functional internal, external (voluntary).
- Histology: Epithelium transition (e.g., Male: Transitional → Pseudostratified/Columnar → Stratified Squamous; Female: Transitional → Stratified Squamous).
- Innervation (Micturition Control):
- Parasympathetic (S2-S4): Detrusor contraction, internal sphincter relaxation (Voiding).
- Sympathetic (T11-L2): Detrusor relaxation, internal sphincter contraction (Filling).
- Somatic (Pudendal n. S2-S4): External sphincter control.
- Applied Anatomy:
- Renal calculi sites: Calyces, Pelvi-Ureteric Junction (PUJ), Vesico-Ureteric Junction (VUJ).
- Benign Prostatic Hyperplasia (BPH) impacts prostatic urethra.
- Urethral rupture: Bulbous/membranous common.
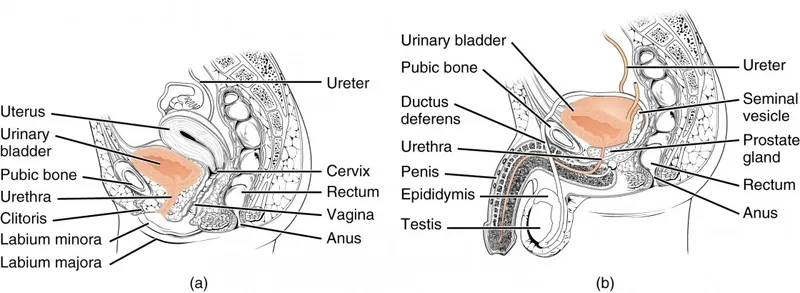
⭐ The membranous urethra in males is the shortest, least dilatable part, and is most susceptible to injury during pelvic fractures or instrumentation.
High-Yield Points - ⚡ Biggest Takeaways
- Kidneys: retroperitoneal; right lower. Hilum: VAP (Vein, Artery, Pelvis) anterior-posterior.
- JGA (macula densa, JG cells) regulates renin, BP, GFR.
- Ureter constrictions: PUJ, pelvic brim, VUJ (narrowest, common site for calculi).
- Bladder trigone: smooth; detrusor muscle (parasympathetic S2-S4) for voiding.
- Male urethra (≈20cm): prostatic, membranous (narrowest part), spongy. Female urethra (≈4cm): higher UTI risk.
- Horseshoe kidney: commonest fusion anomaly, ascent blocked by IMA (Inferior Mesenteric Artery).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

