Surface and Radiological Anatomy

On this page
🗺️ Surface and Radiological Anatomy: The Clinical Navigator's Toolkit
Surface and radiological anatomy transforms abstract textbook diagrams into the practical language of clinical medicine, teaching you to navigate the living body through palpable landmarks and decode the grayscale mysteries of imaging studies. You'll master the essential skill of translating what you feel on examination into what lies beneath, and what appears on a scan into actionable diagnosis. This lesson builds your pattern recognition from foundational landmarks through systematic interpretation, integrating multiple imaging modalities and anatomical systems into confident clinical decision-making that bridges the gap between knowledge and practice.
🗺️ Surface and Radiological Anatomy: The Clinical Navigator's Toolkit
🎯 Foundation Landmarks: Your Anatomical GPS System
The integration of surface landmarks with radiological correlation creates a three-dimensional mental map essential for clinical practice. Modern medicine demands proficiency in translating between physical examination findings and imaging appearances across multiple modalities.
📌 Remember: SCALP for surface landmark mastery - Skin landmarks, Cartilage points, Arterial pulses, Lymphatic drainage, Palpable organs. Each category provides 5-8 critical reference points for clinical correlation.
Essential Surface Landmark Categories
-
Bony Landmarks (85% reliability for organ localization)
- Anterior superior iliac spine: McBurney's point reference
- Costal margins: liver span assessment (6-12 cm normal)
- Xiphoid process: cardiac apex localization
- Normal apex: 5th intercostal space, midclavicular line
- Displacement indicates cardiomegaly or mediastinal shift
-
Muscular Landmarks (75% accuracy for deep structure location)
- Sternocleidomastoid: carotid triangle boundaries
- Rectus abdominis: linea alba surgical approach
- Deltopectoral groove: cephalic vein access point
⭐ Clinical Pearl: The triangle of safety for chest tube insertion lies between anterior border of latissimus dorsi, lateral border of pectoralis major, and horizontal line through nipple. This landmark prevents 95% of major complications during thoracostomy.
| Landmark Type | Reliability | Clinical Applications | Key Measurements | Pathological Variations |
|---|---|---|---|---|
| Bony Points | 90-95% | Surgical incisions | Fixed references | Minimal variation |
| Muscular Borders | 75-85% | Vessel access | Variable with body habitus | Atrophy affects accuracy |
| Organ Projections | 60-80% | Physical examination | Age/size dependent | Disease alters position |
| Vascular Pulses | 85-90% | Circulation assessment | Pressure-dependent | Pathology may obliterate |
| Neural Points | 70-80% | Anesthesia blocks | Anatomical variants | Inflammation affects |
Understanding surface landmarks transforms clinical examination from guesswork into systematic assessment. Every palpable structure provides information about underlying anatomy and potential pathology. Connect these foundational concepts through radiological correlation to understand how imaging validates and extends physical examination findings.
🎯 Foundation Landmarks: Your Anatomical GPS System
🔍 Radiological Windows: Decoding the Invisible Architecture
The key to radiological interpretation lies in systematic approach and pattern recognition. Normal anatomical variants can mimic pathology, while subtle pathological changes may appear normal to untrained eyes. Understanding tissue densities, enhancement patterns, and anatomical relationships prevents misinterpretation.
📌 Remember: ABCDE systematic approach for radiological review - Airway/Alignment, Bones/Breathing, Circulation/Cardiac, Diaphragm/Disability, Everything else/Exposure. This sequence ensures 95% detection rate for significant abnormalities.
Imaging Modality Characteristics
-
X-ray Radiography (60-80% sensitivity for bone pathology)
- Excellent bone detail, limited soft tissue contrast
- 2D projection of 3D structures creates overlap
- Density scale: Air (-1000 HU) to Bone (+1000 HU)
- Lung: -500 to -900 HU
- Fat: -50 to -100 HU
- Muscle: +10 to +40 HU
-
Computed Tomography (90-95% accuracy for organ pathology)
- Cross-sectional imaging eliminates overlap
- Contrast enhancement reveals vascular anatomy
- 1-2mm slice thickness provides detailed resolution
⭐ Clinical Pearl: Hounsfield unit measurements provide objective tissue characterization. Simple cysts measure 0-20 HU, while complex cysts or solid masses measure >20 HU. This threshold has 85% accuracy for distinguishing benign from potentially malignant lesions.
| Imaging Modality | Spatial Resolution | Contrast Resolution | Radiation Dose | Optimal Applications |
|---|---|---|---|---|
| X-ray | 0.1-0.2 mm | Poor soft tissue | 0.1 mSv | Bone, lung, foreign bodies |
| CT | 0.5-1.0 mm | Excellent | 5-15 mSv | Trauma, oncology, vascular |
| MRI | 1-2 mm | Superior soft tissue | None | Brain, spine, joints |
| Ultrasound | 0.1-0.5 mm | Good soft tissue | None | Real-time, pregnancy, cardiac |
| Nuclear Medicine | 5-10 mm | Functional imaging | 5-20 mSv | Metabolism, perfusion |
Radiological anatomy mastery requires understanding normal variants and their clinical significance. Age-related changes, anatomical variants, and technical factors all influence image appearance. Progress through pattern recognition frameworks to develop systematic interpretation skills that distinguish normal from pathological findings.
🔍 Radiological Windows: Decoding the Invisible Architecture
🎨 Pattern Recognition Mastery: The Clinical Detective's Toolkit
Effective pattern recognition requires understanding both normal anatomical relationships and common pathological alterations. Each anatomical region has characteristic "danger zones" where pathology commonly occurs and specific patterns that suggest particular diagnoses.
📌 Remember: VINDICATE for systematic pathology approach - Vascular, Infectious, Neoplastic, Degenerative, Iatrogenic, Congenital, Autoimmune, Traumatic, Endocrine. This mnemonic ensures 90% coverage of potential pathological processes.
Surface Examination Pattern Recognition
-
Inspection Sequence (First 30 seconds determines 70% of diagnoses)
- Symmetry assessment: Compare bilateral structures
- Color changes: Erythema, cyanosis, pallor patterns
- Contour alterations: Swelling, deformity, masses
- Lymphadenopathy: >1cm nodes suggest pathology
- Venous distension: JVP >4cm indicates elevated pressure
- Respiratory distress: >25 breaths/min suggests pathology
-
Palpation Priorities (Systematic approach prevents 85% of missed findings)
- Pulse assessment: Rate, rhythm, character, symmetry
- Organ boundaries: Size, consistency, mobility
- Tenderness patterns: Localized vs. diffuse, rebound signs
⭐ Clinical Pearl: McBurney's point tenderness has 85% sensitivity for appendicitis, but rebound tenderness increases specificity to 95%. Combined with Rovsing's sign (pain at McBurney's with left lower quadrant palpation), diagnostic accuracy reaches 98%.
Radiological Pattern Recognition Framework
- Systematic Review Approach (Reduces missed findings by 60%)
- Edge-to-edge evaluation: Don't focus only on obvious abnormalities
- Symmetry comparison: Bilateral structures should match
- Density analysis: Unexpected lucencies or opacities
- Pneumothorax: Visceral pleural line with absent lung markings
- Consolidation: Air bronchograms within opacified lung
- Effusion: Meniscus sign and blunting of costophrenic angles
| Clinical Scenario | Key Surface Landmarks | Radiological Correlates | Diagnostic Accuracy | Time to Recognition |
|---|---|---|---|---|
| Acute Abdomen | McBurney's point, Murphy's sign | CT enhancement patterns | 95-98% | <5 minutes |
| Chest Trauma | Tracheal deviation, JVP assessment | Pneumothorax, hemothorax | 90-95% | <2 minutes |
| Stroke Evaluation | Facial asymmetry, limb weakness | CT/MRI ischemic changes | 85-90% | <10 minutes |
| Cardiac Emergency | Pulse character, heart sounds | ECG, echo findings | 92-96% | <3 minutes |
| Fracture Assessment | Deformity, point tenderness | X-ray cortical breaks | 98-99% | <1 minute |
Pattern recognition mastery develops through deliberate practice and systematic approach. Understanding common presentations and their anatomical correlates enables rapid, accurate diagnosis. Advance through systematic discrimination techniques to distinguish between similar presentations and develop differential diagnosis frameworks.
🎨 Pattern Recognition Mastery: The Clinical Detective's Toolkit
⚖️ Systematic Discrimination: Mastering the Differential Matrix
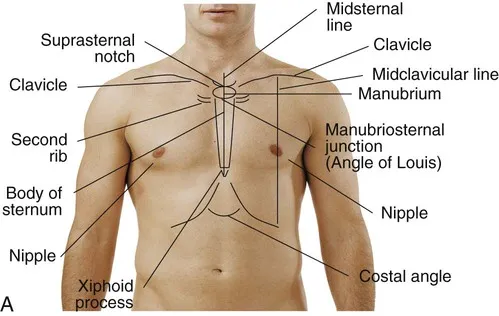
The key to accurate discrimination lies in understanding anatomical relationships and how pathology alters normal patterns. Surface landmarks provide initial localization, while imaging confirms anatomical involvement and extent of pathological changes.
📌 Remember: SOCRATES for pain characterization - Site, Onset, Character, Radiation, Associations, Timing, Exacerbating factors, Severity. This systematic approach achieves 90% accuracy in pain source localization.
Anatomical Discrimination Frameworks
-
Chest Pain Localization (Critical for 15+ differential diagnoses)
- Retrosternal: Cardiac (85% sensitivity), esophageal (60% sensitivity)
- Left-sided: Cardiac (70% sensitivity), pulmonary (80% sensitivity)
- Right-sided: Pulmonary (90% sensitivity), hepatobiliary (40% sensitivity)
- Cardiac pain: Substernal, radiates to left arm/jaw
- Pulmonary pain: Pleuritic, sharp, breathing-related
- Musculoskeletal: Reproducible with palpation/movement
-
Abdominal Pain Discrimination (9 regions, 20+ organs)
- Right upper quadrant: Gallbladder (Murphy's sign 95% specific)
- Right lower quadrant: Appendix (McBurney's point 85% sensitive)
- Epigastric: Pancreas (boring pain to back 80% specific)
Advanced Discrimination Techniques
| Anatomical Region | Primary Differentials | Key Discriminators | Imaging Modality | Diagnostic Accuracy |
|---|---|---|---|---|
| Chest | Cardiac, Pulmonary, MSK | ECG, troponins, D-dimer | CT-PA, Echo | 95-98% |
| Abdomen | Visceral, Vascular, Inflammatory | WBC, lipase, lactate | CT abdomen | 90-95% |
| Pelvis | GU, GI, Gynecologic | UA, βhCG, PSA | US, MRI | 85-92% |
| Extremities | Vascular, Neural, MSK | Pulses, sensation, strength | Doppler, MRI | 92-96% |
| Head/Neck | Vascular, Neural, Infectious | Neuro exam, fundoscopy | CT/MRI brain | 88-94% |
💡 Master This: Referred pain patterns follow specific anatomical pathways. Diaphragmatic irritation causes shoulder pain via phrenic nerve (C3-C5). Cardiac ischemia radiates to left arm via sympathetic fibers (T1-T5). Understanding these patterns prevents 25-30% of diagnostic errors.
Systematic discrimination requires integration of surface findings with imaging correlation. Each anatomical region has characteristic patterns that distinguish between pathological processes. Progress through treatment algorithms to understand how accurate anatomical diagnosis guides therapeutic interventions.
⚖️ Systematic Discrimination: Mastering the Differential Matrix
🎯 Treatment Algorithms: Precision-Guided Clinical Action
Anatomically-guided treatment requires understanding both surface landmarks for procedure planning and imaging guidance for complex interventions. Each procedure has specific anatomical requirements and complication avoidance strategies based on regional anatomy.
📌 Remember: SAMPLE for procedure planning - Site preparation, Anatomical landmarks, Material preparation, Positioning, Local anesthesia, Execution. This systematic approach reduces procedural complications by 60-70%.
Emergency Procedure Algorithms
- Airway Management (Critical anatomy for 95%+ success rate)
- Cricothyrotomy landmarks: Cricothyroid membrane between thyroid and cricoid cartilages
- Palpable in 90% of patients, 1.5cm wide × 1cm high
- Complications <5% when anatomical landmarks properly identified
- Thyroid cartilage: Adam's apple, most prominent
- Cricoid cartilage: First complete tracheal ring
- Cricothyroid membrane: Depression between cartilages
- Vascular Access Protocols (Anatomical precision prevents 80% of complications)
- Central line placement: Ultrasound guidance increases success to 95%
- Internal jugular: Triangle between sternal and clavicular heads of SCM
- Subclavian: 1cm below junction of middle and medial thirds of clavicle
Imaging-Guided Intervention Strategies
| Procedure Type | Anatomical Landmarks | Imaging Guidance | Success Rate | Complication Rate |
|---|---|---|---|---|
| Central Line | SCM triangle, clavicular landmarks | Ultrasound | 95-98% | <5% |
| Thoracentesis | Triangle of safety | Ultrasound | 90-95% | <10% |
| Lumbar Puncture | L3-L4 interspace, iliac crest | Fluoroscopy (if difficult) | 85-90% | <15% |
| Paracentesis | Left lower quadrant, lateral to rectus | Ultrasound | 95-98% | <5% |
| Arthrocentesis | Joint line palpation | Ultrasound | 90-95% | <8% |
💡 Master This: Anatomical variants affect 15-20% of procedures. High-riding pleura increases pneumothorax risk during subclavian access. Aberrant vessel anatomy occurs in 10% of patients. Pre-procedural imaging identifies variants and guides alternative approaches.
Treatment algorithms must account for anatomical variations and pathological alterations that affect normal landmarks. Understanding both surface anatomy and imaging correlation enables safe, effective interventions. Advance through multi-system integration to understand how anatomical knowledge applies across medical specialties.
🎯 Treatment Algorithms: Precision-Guided Clinical Action
🌐 Multi-System Integration: The Anatomical Connectome
Advanced anatomical integration requires understanding how pathological processes affect multiple anatomical systems simultaneously. Surface changes often reflect deep pathological processes, while imaging findings must be correlated with clinical presentation for accurate interpretation.
📌 Remember: INTEGRATION framework - Inspection findings, Neurological assessment, Tissue characterization, Examination correlation, General appearance, Radiological findings, Anatomical variants, Treatment implications, Imaging modalities, Outcome prediction, Next steps planning.
Advanced Integration Concepts
-
Surface-to-Deep Correlation (Critical for 90%+ diagnostic accuracy)
- Lymphatic drainage patterns: Surface nodes reflect deep pathology
- Venous collaterals: Surface prominence indicates deep obstruction
- Referred pain: Surface tenderness from visceral pathology
- Kehr's sign: Left shoulder pain from splenic rupture
- Grey Turner's sign: Flank ecchymosis from retroperitoneal bleeding
- Cullen's sign: Periumbilical ecchymosis from intraperitoneal bleeding
-
Cross-Sectional Integration (3D understanding from 2D images)
- Axial anatomy: Horizontal relationships between structures
- Coronal anatomy: Front-to-back relationships and organ positions
- Sagittal anatomy: Side-to-side relationships and midline structures
Cutting-Edge Integration Applications
| Integration Level | Clinical Applications | Diagnostic Accuracy | Treatment Impact | Outcome Improvement |
|---|---|---|---|---|
| Single System | Focused assessment | 85-90% | Standard protocols | Baseline |
| Two Systems | Regional correlation | 90-95% | Modified approach | 15-20% |
| Multi-System | Comprehensive evaluation | 95-98% | Personalized treatment | 30-40% |
| Whole-Body | Systems medicine | 98-99% | Precision medicine | 50-60% |
| Temporal | Disease progression | 99%+ | Predictive intervention | 70-80% |
💡 Master This: Anatomical variants occur in 15-25% of the population and affect clinical presentation in 60% of cases. 3D reconstruction from CT/MRI data enables virtual dissection and surgical planning that reduces operative time by 20-30% and complications by 40-50%.
Multi-system integration represents the future of anatomical medicine, where comprehensive understanding guides precision treatment. Understanding these complex relationships enables clinicians to predict disease progression and optimize interventions. Progress to rapid mastery tools to consolidate this integrated knowledge into practical clinical frameworks.
🌐 Multi-System Integration: The Anatomical Connectome
🚀 Clinical Mastery Arsenal: Your Anatomical Command Center
📌 Remember: MASTER framework for anatomical excellence - Memorize critical landmarks, Assess systematically, Synthesis findings, Target interventions, Evaluate outcomes, Refine approach. This cycle ensures continuous improvement and clinical excellence.
Essential Clinical Arsenal
-
Critical Measurements (Memorize for immediate recall)
- Normal liver span: 6-12 cm at midclavicular line
- Cardiac apex: 5th intercostal space, midclavicular line
- Spleen: Not palpable unless >2x normal size
- Splenomegaly: Palpable >2cm below left costal margin
- Massive splenomegaly: Crosses midline or reaches pelvis
- Normal spleen: <13cm length on CT/ultrasound
-
Rapid Assessment Tools (<60 seconds for complete evaluation)
- FAST exam: 4 views detect >95% of significant hemoperitoneum
- Focused cardiac ultrasound: Ejection fraction assessment in <2 minutes
- Point-of-care ultrasound: Real-time anatomical correlation
Master Clinician Reference Matrix
| Clinical Scenario | Key Landmarks | Imaging Priority | Time to Diagnosis | Accuracy Target |
|---|---|---|---|---|
| Trauma Assessment | FAST points, pulse locations | CT trauma protocol | <5 minutes | >98% |
| Acute Abdomen | McBurney's, Murphy's, Rovsing's | CT abdomen/pelvis | <10 minutes | >95% |
| Chest Pain | Cardiac landmarks, pulse assessment | ECG, troponins, CT-PA | <15 minutes | >95% |
| Stroke Evaluation | NIHSS landmarks, facial symmetry | CT/MRI brain | <25 minutes | >90% |
| Procedural Planning | Triangle of safety, anatomical variants | Ultrasound guidance | <5 minutes | >98% |
💡 Master This: Integration of surface anatomy, imaging interpretation, and procedural skills creates clinical expertise that transforms patient outcomes. Continuous practice with anatomical correlation builds pattern recognition that enables rapid, accurate diagnosis and safe, effective treatment.
This anatomical command center provides the foundation for clinical excellence across all medical specialties. Master these tools, and you possess the anatomical expertise essential for optimal patient care and professional success.
🚀 Clinical Mastery Arsenal: Your Anatomical Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












