Pelvic Ring Stability & Trauma - Crash Course Pelvis
- Pelvic Ring: Composed of sacrum & two innominate bones. Posterior arch (sacroiliac joints & strong posterior ligaments) is crucial for stability.
- Key Stabilizing Ligaments:
- Posterior Sacroiliac Ligaments (strongest, resist vertical shear)
- Sacrospinous & Sacrotuberous Ligaments (resist external rotation)
- Symphysis Pubis & ligaments (anterior support)
- Classification (Examples):
- Young-Burgess: Based on mechanism of injury (e.g., APC - Anteroposterior Compression, LC - Lateral Compression, VS - Vertical Shear).
- Tile: Based on stability (A: Stable; B: Rotationally unstable, vertically stable; C: Rotationally & vertically unstable).
- Clinical Concerns: Massive hemorrhage (venous > arterial), urogenital injuries, lumbosacral plexus injuries (L5, S1 roots).
- Management: ATLS protocol, pelvic binder/sheet for temporary stabilization, angiography for arterial bleeding.
⭐ Anteroposterior compression (APC) Type III injuries ("open book" pelvis) involve complete posterior ligament disruption and pubic symphysis diastasis > 2.5 cm.

Perineal Tears & Pudendal Block - Ouch & Order Downstairs
- Perineal Tears: Childbirth injury.
- 1st degree: Skin, vaginal mucosa.
- 2nd degree: Muscles.
- 3rd degree: Anal sphincter.
- 3a: <50% External Anal Sphincter (EAS) thickness.
- 3b: >50% EAS thickness.
- 3c: Internal Anal Sphincter (IAS) also torn.
- 4th degree: Rectal mucosa.
- 3rd/4th degree repair prevents incontinence.
- Pudendal Nerve Block: Perineal anesthesia.
- Targets Pudendal nerve (S2-S4). 📌 S2,S3,S4 keep perineum off floor.
- Landmark: Ischial spine.
- Uses: Episiotomy, operative delivery, repair.
- Anesthetizes: Vulva, lower vagina, perineum.
⭐ Pudendal block spares uterine contraction pain (T10-L1).

Pelvic Support Defects & Prolapse - Droops & Dynamics
- Weakening of pelvic floor structures (muscles, ligaments, fascia) causing pelvic organ descent.
- Types:
- Cystocele (bladder), Rectocele (rectum), Enterocele (bowel)
- Uterine prolapse, Vaginal vault prolapse (post-hysterectomy)
- Risk Factors: Childbirth, aging, ↑ intra-abdominal pressure (obesity, chronic cough), genetics.
- DeLancey's Levels of Support:
- Level I (Apical): Uterosacral/cardinal lig. Defect → uterine/apical prolapse.
- Level II (Lateral): Arcus tendineus fasciae pelvis. Defect → cystocele/rectocele.
- Level III (Distal): Perineal body. Defect → perineal descent.
- Symptoms: Pelvic pressure, bulge, "dragging", urinary/fecal/sexual dysfunction.
- Diagnosis: POP-Q system.
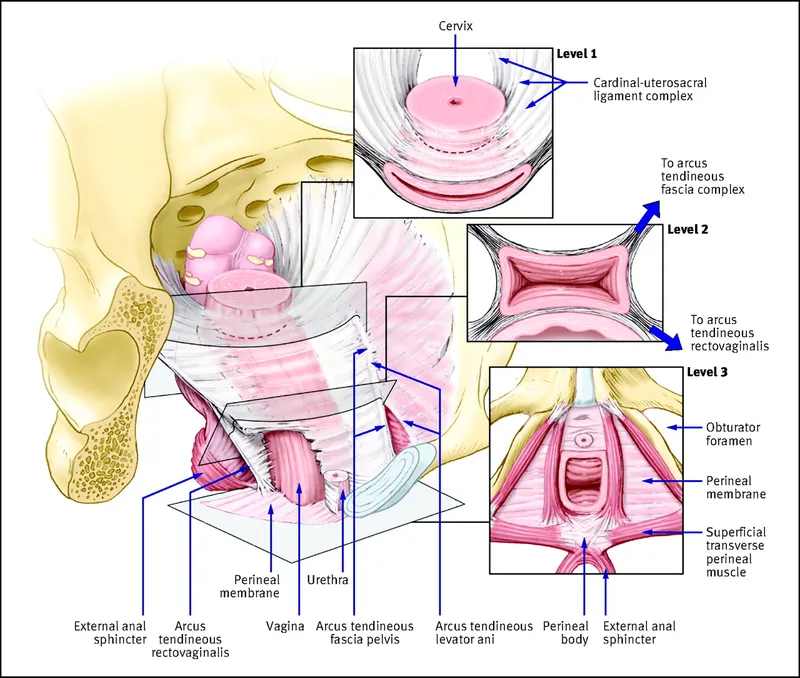
⭐ The uterosacral ligaments are key for Level I (apical) support; their damage is a primary cause of uterine and vaginal vault prolapse.
Pelvic Neurovasculature Clinical Hits - Pelvic Power Lines
- Arteries:
- Internal Iliac A.: Ant. div (viscera, PPH ligation); Post. div (pelvic wall).
- Uterine A.: Crosses ureter anteriorly (📌 "Water under bridge"); hysterectomy risk.
- Ovarian A.: From abdominal aorta; ovarian torsion risk.
- Pudendal A.: Main perineum supply; accompanies pudendal N.
- Veins:
- Pelvic Venous Plexuses (e.g., prostatic, uterine): Valveless; Batson's plexus → vertebral mets.
- Ovarian V.: Right → IVC; Left → Left Renal V. (↑ L-sided varicocele risk).
- Nerves:
- Pudendal N. (S2,S3,S4): Perineal sensation/motor; nerve block for childbirth; Alcock's canal entrapment.
- Obturator N. (L2,L3,L4): Adductor muscles; injury in pelvic surgery (e.g., lymphadenectomy) → adductor weakness, medial thigh sensory loss.
- Sciatic N. (L4-S3): Vulnerable: misplaced IM gluteal injection, posterior hip dislocation.
- Pelvic Splanchnic Ns. (S2-S4): Parasympathetic innervation; "Nervi Erigentes" for erection.
⭐ Obturator nerve injury during pelvic lymphadenectomy is a known complication, potentially causing adductor muscle weakness and sensory loss over the medial thigh.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Pudendal nerve block: Ischial spine is the crucial palpable landmark for anaesthesia.
- Episiotomy: Posterolateral incision preferred to avoid anal sphincter and Bartholin's duct injury.
- Pelvic fractures: High risk of bladder and urethral injuries, especially with anterior arch disruption.
- Uterine prolapse: Caused by weakened pelvic diaphragm (levator ani) and supporting ligaments.
- Benign Prostatic Hyperplasia (BPH): Common cause of urinary outflow obstruction in elderly males.
- Ischioanal abscess: Common infection in the ischioanal fossa, potentially leading to fistula-in-ano.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

