Spinal Cord 101 - The Grand Design
- Location: CNS, vertebral canal. Extends from foramen magnum to Conus Medullaris (L1-L2 adult). Filum terminale to coccyx.
- Segments: 31 pairs: 8C, 12T, 5L, 5S, 1Co.
- 📌 Mnemonic: Breakfast at 8, Lunch at 12, Dinner at 5 (twice for L, S).
- Enlargements: Supply limbs.
- Cervical (C5-T1): Brachial plexus (upper limb).
- Lumbosacral (L1-S3): Lumbosacral plexus (lower limb).
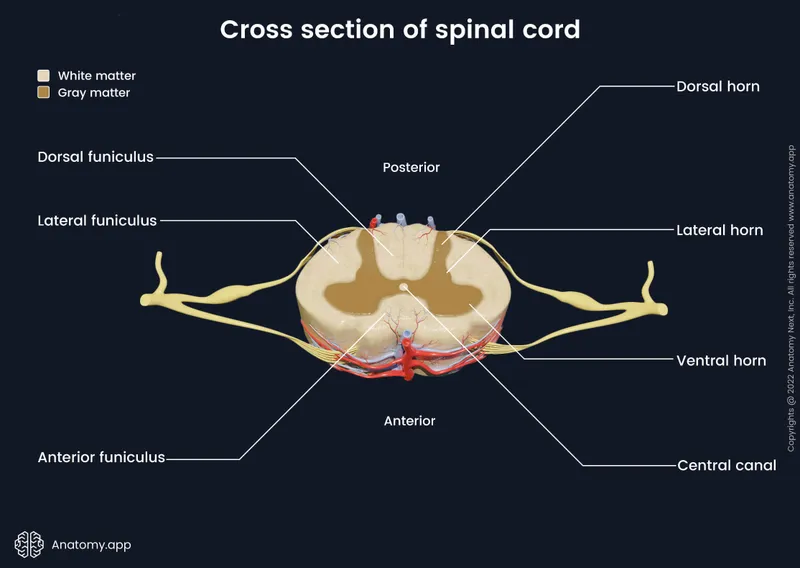
- Cross-section:
- Inner Grey Matter (H-shape): Cell bodies. Horns: Dorsal (sensory), Ventral (motor), Lateral (T1-L2, autonomic).
- Outer White Matter: Myelinated tracts. Funiculi/Columns: Dorsal, Lateral, Ventral.
⭐ Spinal cord ends at L1-L2 in adults, L3 in neonates. Critical for lumbar puncture site selection to avoid iatrogenic injury.
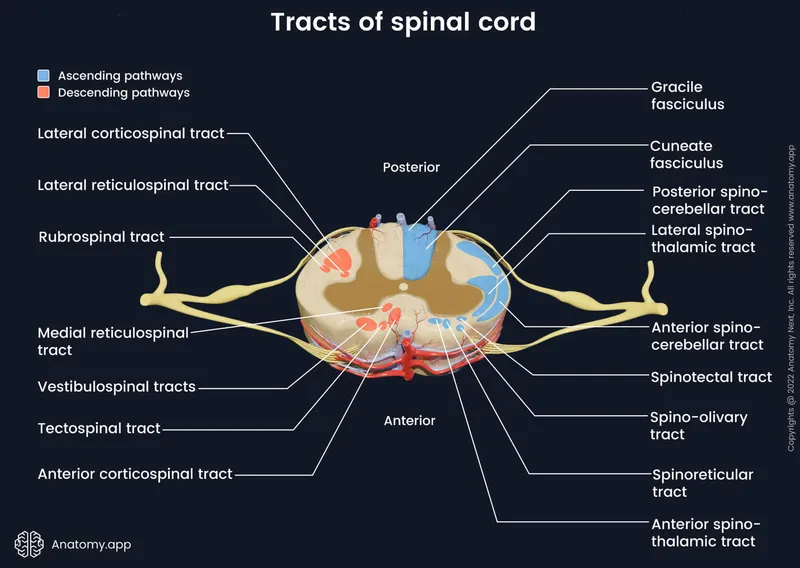
Ascending Tracts - Sensory Express Lane
- Dorsal Column-Medial Lemniscus (DCML): Fine touch, vibration, proprioception.
- 1st Order: DRG → Fasciculus Gracilis (T6↓, legs) / Fasciculus Cuneatus (T6↑, arms).
- 2nd Order: Nucleus Gracilis/Cuneatus (Medulla). Decussates → Medial Lemniscus.
- 3rd Order: VPL (Thalamus) → Somatosensory Cortex.
- 📌 Mnemonic: "Dorsal columns for Dolce & Gabbana (D&G) - Fine things."
- Spinothalamic Tract (Anterolateral System - ALS): Pain, temperature, crude touch.
- 1st Order: DRG → Dorsal Horn (e.g., Substantia Gelatinosa).
- 2nd Order: Dorsal Horn. Decussates (Anterior White Commissure) → Ascends.
- 3rd Order: VPL (Thalamus) → Somatosensory Cortex.
⭐ Lesion causes contralateral loss of pain & temperature 1-2 segments below the lesion level.
- Spinocerebellar Tracts: Unconscious proprioception to cerebellum.
- Dorsal (DSCT), Ventral (VSCT), Cuneocerebellar, Rostral. Mostly ipsilateral input to cerebellum.

Descending Tracts - Motorway Mania
-
Pyramidal Tracts (Voluntary Movement)
- Corticospinal (CST): Cerebral Cortex. Precise, skilled voluntary movements.
- Lateral CST: ~80-90% fibers; decussates medulla (pyramidal decussation) → limbs.
- Anterior CST: ~10-20% fibers; uncrossed/decussates spinal level → axial/proximal.
⭐ UMN lesion (e.g., CST): spastic paralysis, hyperreflexia, Babinski sign.
- Corticospinal (CST): Cerebral Cortex. Precise, skilled voluntary movements.
-
Extrapyramidal Tracts (Involuntary/Postural Control)
- Rubrospinal: Red Nucleus; decussates midbrain. Flexors ↑, extensors ↓ (upper limb).
- Vestibulospinal: Vestibular Nuclei.
- Lateral: Ipsilateral; balance, extensor tone.
- Medial: Bilateral; head/neck position.
- Reticulospinal: Reticular Formation.
- Pontine (Medial): Ipsilateral; extensors ↑, posture.
- Medullary (Lateral): Bilateral; extensors ↓, muscle tone ↓.
- Tectospinal: Superior Colliculus; decussates midbrain. Reflex head/neck to visual stimuli. 📌 Mnemonic (Origins): "Red Vest Really Tough" (Red Nucleus, Vestibular Nuclei, Reticular Formation, Tectum)
Blood & Damage - Cord SOS
- Arterial Supply:
- Anterior Spinal Artery (ASA): supplies anterior 2/3rds.
- Posterior Spinal Arteries (PSAs): supply posterior 1/3rd.
- Artery of Adamkiewicz: major supply to lumbosacral cord, typically T9-L2.
- Key Syndromes & Lesions:
- Anterior Cord Syndrome: ASA occlusion. Loss of motor, pain, temperature. Proprioception/vibration spared.
⭐ Most common spinal cord infarction.
- Central Cord Syndrome: Cervical hyperextension. Upper limb > lower limb weakness. Sacral sparing.
- Brown-Séquard Syndrome: Hemisection. 📌 Ipsilateral: motor, vibration, proprioception loss. Contralateral: pain, temperature loss. oka
- Anterior Cord Syndrome: ASA occlusion. Loss of motor, pain, temperature. Proprioception/vibration spared.
High‑Yield Points - ⚡ Biggest Takeaways
- Spinal cord typically terminates at L1-L2 in adults, and L3 in newborns.
- There are 31 pairs of spinal nerves: 8C, 12T, 5L, 5S, 1Co.
- Cervical (C5-T1) and Lumbar (L2-S3) enlargements correspond to limb innervation.
- Anterior Spinal Artery supplies the anterior 2/3; Posterior Spinal Arteries (paired) supply posterior 1/3.
- Key tracts: Dorsal columns (vibration, proprioception), Spinothalamic (pain, temperature), Corticospinal (voluntary motor).
- Lumbar puncture is safely done at L3-L4 or L4-L5, accessing CSF in the cauda equina.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

