Intro to CT - Body's Framework
- Connective Tissue (CT): Body's framework, providing structural & metabolic support to organs and other tissues.
- Origin: Predominantly mesodermal.
- Key Functions:
- Binding & Supporting (e.g., tendons, ligaments)
- Protecting (e.g., bone, cartilage)
- Insulating (e.g., adipose tissue)
- Transporting substances (e.g., blood)
- Two Main Components:
- Cells: Diverse population (e.g., fibroblasts, adipocytes, chondrocytes, osteocytes, blood cells).
- Extracellular Matrix (ECM): Non-living material surrounding cells, produced by them.
- Fibers: Collagen (tensile strength), Elastic (recoil), Reticular (delicate framework).
- Ground Substance: Hydrated, amorphous gel (proteoglycans, glycosaminoglycans (GAGs), adhesive glycoproteins like fibronectin).
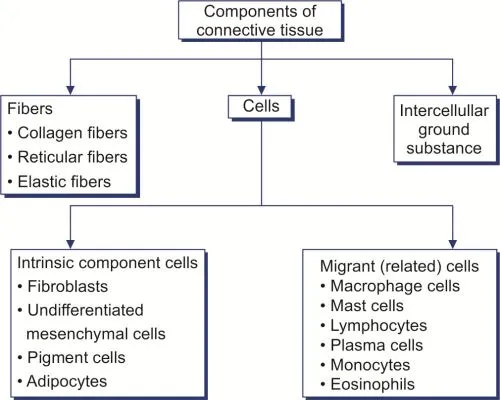
⭐ The Extracellular Matrix (ECM), comprising fibers and ground substance, dictates the specialized physical properties of each connective tissue type (e.g., rigidity of bone, resilience of cartilage).
CT Components: Cells - The Living Units
- Fixed Cells (Resident): 📌 FAMM
- Fibroblasts/Fibrocytes: Most common. Synthesize ECM (collagen, elastin). Fibroblast (active, RER) vs. Fibrocyte (inactive). Myofibroblasts: wound contraction.
- Adipocytes: Store triglycerides. Unilocular (white fat): single large droplet, signet ring. Multilocular (brown fat): multiple droplets, thermogenesis.
- Mast Cells: Oval; granules (histamine, heparin). IgE receptors. Allergic reactions. Metachromasia.
- Macrophages (Histiocytes): Phagocytic; antigen presentation. From monocytes. Kidney-shaped nucleus. (e.g., Kupffer).
- Wandering Cells (Transient):
- Plasma Cells: From B-lymphocytes. Antibody (Ig) synthesis. Eccentric "clock-face" nucleus, basophilic cytoplasm, Golgi halo.
- Leukocytes: Neutrophils, Lymphocytes. Immune response via blood migration.

⭐ Mast cell granules contain preformed mediators like histamine (vasodilator, ↑ vascular permeability) and heparin (anticoagulant).
CT Fibers & Matrix - Matrix Marvels
Fibers: The Framework
- Collagen Fibers: Most abundant protein; tensile strength.
- Type I: Bone, Skin, Tendon, Dentin, Cornea. (Strongest)
- Type II: Cartilage, Vitreous body (📌 Cartwolage)
- Type III: Reticular fibers (skin, vessels) (📌 R3ticular)
- Type IV: Basement membrane (📌 Type 4 on the floor)
- Vit C needed for synthesis; deficiency → Scurvy.
- Elastic Fibers: Elastin + Fibrillin; stretch & recoil.
- Locations: Large arteries, lungs, skin.
- Fibrillin-1 defect → Marfan Syndrome.
- Reticular Fibers: Type III collagen; delicate meshwork.
- Locations: Liver, spleen, lymph nodes. Argyrophilic.
Ground Substance: The Gel
- Amorphous, hydrated gel. Components:
- Glycosaminoglycans (GAGs): Long unbranched polysaccharides.
- Hyaluronic acid: Largest, non-sulfated. Synovial fluid, vitreous.
- Sulfated GAGs: Chondroitin, Dermatan, Heparan, Keratan sulfates.
- Proteoglycans: Core protein + GAGs (e.g., Aggrecan).
- Multiadhesive Glycoproteins: Link cells to ECM (e.g., Fibronectin, Laminin).
- Glycosaminoglycans (GAGs): Long unbranched polysaccharides.
⭐ Osteogenesis Imperfecta ("Brittle Bone Disease") is primarily due to defects in Type I collagen synthesis, leading to fragile bones, blue sclerae, and hearing loss.

Classification of CT - The Tissue Tapestry
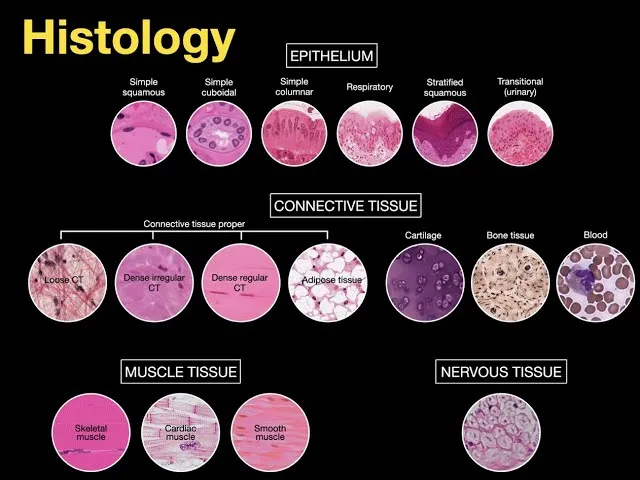
Connective tissues are diverse, classified by cell type, fiber density, and matrix.
- Embryonic CT:
- Mesenchyme: Undifferentiated; gives rise to all other CT types.
- Mucoid CT: Gelatinous; e.g., Wharton's jelly (umbilical cord).
- CT Proper:
- Loose CT: Fewer fibers, more ground substance. (Areolar, Adipose, Reticular)
- Dense CT: More fibers, less ground substance. (Regular, Irregular, Elastic)
- Specialized CT:
- Cartilage: Avascular; (Hyaline, Elastic, Fibrocartilage).
- Bone: Mineralized matrix; (Compact, Spongy).
- Blood: Fluid matrix (plasma).
⭐ Wharton's jelly, a type of mucoid connective tissue, is rich in hyaluronic acid and proteoglycans, providing cushioning to umbilical cord vessels.
High‑Yield Points - ⚡ Biggest Takeaways
- Connective tissue, derived from mesoderm, is the most abundant in the body.
- Collagen Type I is the most common, found in bone, skin, and tendon.
- Elastic fibers (elastin, fibrillin) provide recoil; Marfan syndrome involves fibrillin-1 defect.
- Reticular fibers (Collagen Type III) form supportive networks in organs like liver, spleen.
- Ground substance consists of GAGs (e.g., hyaluronic acid), proteoglycans, and glycoproteins.
- Fibroblasts are the principal cells, responsible for ECM synthesis.
- Mast cells contain histamine and heparin, mediating allergic and inflammatory responses.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

