Cranial Nerve Clinicals - Nerve Wreckers
- CN III (Oculomotor): Ptosis, mydriasis, eye "down & out". Pupil involved: compression (e.g., PCOM aneurysm).
- CN IV (Trochlear): Vertical diplopia (worse reading/stairs), head tilt away. 📌 SO4.
- CN V (Trigeminal): Trigeminal neuralgia; ↓ corneal reflex (V1 afferent).
- CN VI (Abducens): Horizontal diplopia (worse lateral gaze); esotropia. 📌 LR6.
- CN VII (Facial):
- CN IX (Glossopharyngeal): ↓ Gag (afferent), ↓ taste/sensation post. 1/3 tongue.
- CN X (Vagus): Uvula deviates away; hoarseness, dysphagia, ↓ gag (efferent).
- CN XI (Accessory): Shoulder droop; weak head turn away, weak shrug.
- CN XII (Hypoglossal): Tongue deviates towards lesion (LMN); fasciculations. 📌 "Tongue licks lesion."
⭐ Bell's Palsy (idiopathic LMN CN VII palsy) is the most common cause of acute unilateral facial paralysis.
Head Trauma & Hemorrhages - Brain Bleed Basics
- ICH Types & Features:
- Epidural (EDH): Arterial (MMA); temporal fracture common. CT: Biconvex (lens), no suture cross. Lucid interval.
- Subdural (SDH): Venous (bridging veins). CT: Crescent, crosses sutures. Risks: elderly, alcohol, anticoagulants.
- Subarachnoid (SAH): Arterial (aneurysm rupture). CT: Blood in sulci/cisterns. "Thunderclap headache."
- Intracerebral (ICH): Parenchymal bleed. Causes: Hypertension, AVM.
- Key Assessments:
- GCS: Consciousness. Eye (E4), Verbal (V5), Motor (M6). Score 3 (coma) - 15 (normal).
- Cushing's Triad (↑ICP): Hypertension, bradycardia, irregular respirations.
⭐ EDH: Arterial bleed (Middle Meningeal Artery), often with skull fracture. CT shows biconvex (lens) shape, doesn't cross sutures. Lucid interval is classic.
Infections & Pathways - Danger Zone Patrol
- Danger Area of Face:
- Triangle: Nasal bridge to mouth corners.
- Venous path: Facial v. → Angular v. → Ophthalmic vv. → Cavernous Sinus.
- Valveless veins: Retrograde infection spread.
- Risk: Cavernous Sinus Thrombosis (CST) from facial furuncles.
- Danger Area of Scalp (Loose Areolar Tissue - 4th layer):
- Easy spread of infection.
- Emissary veins connect to dural sinuses.
- Risk: Meningitis, osteomyelitis, dural sinus thrombosis.
- Infection Spread Routes:
- Direct: e.g., Sinusitis → Pott's puffy tumor.
- Venous: Facial, ophthalmic, emissary, diploic veins.
- Lymphatic.
- Key Conditions:
- CST: Proptosis, ophthalmoplegia, CN III, IV, V1, V2, VI palsies.
- Ludwig's Angina: Submandibular/sublingual cellulitis; airway risk.
⭐ Facial infections (danger area) can reach the cavernous sinus via valveless ophthalmic veins, causing Cavernous Sinus Thrombosis with multiple cranial nerve palsies.

Key Regional Clinicals - Head Hotspots
- Temporomandibular Joint (TMJ) Dysfunction:
- Pain (otalgia, facial), clicking/popping, limited jaw opening.
- Etiology: Myofascial pain, internal derangement, arthritis.
- Paranasal Sinusitis:
- Maxillary sinus most commonly affected; pain referred to maxillary teeth.
- Frontal sinusitis: Tenderness over frontal sinus; risk of Pott's puffy tumor.
- Sphenoid sinusitis: Headache, retro-orbital pain; risk to cranial nerves.
- Salivary Gland Pathologies:
- Sialolithiasis: Most common in submandibular gland (Wharton’s duct).
- Sialadenitis: Parotid (mumps), submandibular (bacterial).
- Frey’s Syndrome: Gustatory sweating post-parotidectomy (auriculotemporal nerve injury).
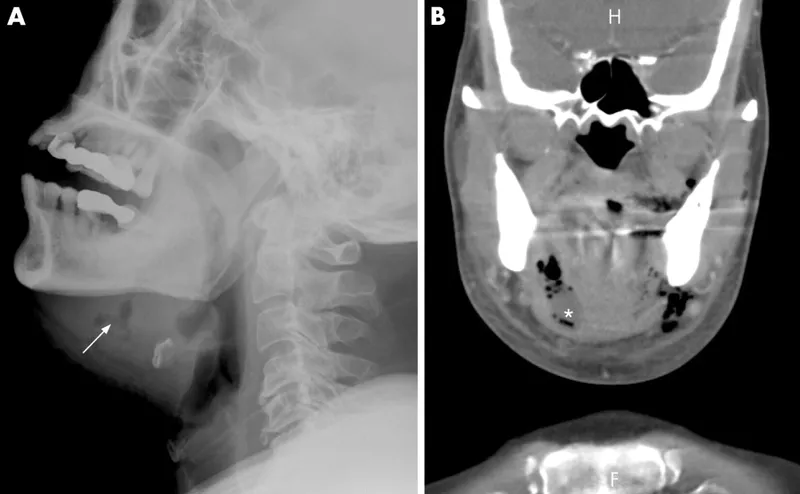
⭐ Ludwig's Angina: Aggressive, rapidly spreading cellulitis of the floor of the mouth (sublingual, submylohyoid, submandibular spaces); often odontogenic. Airway compromise is a major concern. Critical to secure airway early!
High‑Yield Points - ⚡ Biggest Takeaways
- Danger triangle of face infections can spread to the cavernous sinus via ophthalmic veins.
- Cavernous sinus thrombosis presents with ophthalmoplegia (CN III, IV, VI) and V1/V2 sensory loss.
- Frey's syndrome involves gustatory sweating post-parotidectomy due to auriculotemporal nerve injury.
- Trigeminal neuralgia causes severe, lancinating pain in CN V distribution; carbamazepine is key.
- Bell's palsy is an idiopathic LMN CN VII palsy, causing ipsilateral facial paralysis.
- Pterion fracture risks middle meningeal artery tear, potentially leading to epidural hematoma.
- Kiesselbach's plexus in Little's area is the commonest site for epistaxis (nosebleeds).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

