Kidney Development - Bean Machine Genesis
- Three embryonic kidney systems:
- Pronephros: Week 4; cervical, non-functional, regresses.
- Mesonephros: Late week 4; thoracic/lumbar, interim kidney ~4 wks. Mesonephric (Wolffian) duct persists.
- Metanephros: Week 5; sacral, permanent kidney, from:
- Ureteric bud (off mesonephric duct).
- Metanephric mesenchyme/blastema (urogenital ridge origin).
- Reciprocal induction is key.
⭐ Ureteric bud gives rise to the collecting system (collecting ducts, calyces, renal pelvis, and ureter), while the metanephric blastema forms the nephrons (from glomerulus to distal convoluted tubule).
- 📌 Ureteric bud = Ureters & collecting system; Metanephric Mesenchyme = Makes nephrons.

Ducts & Bladder - Plumbing Predicaments
- Mesonephric (Wolffian) Duct:
- ♂ (Testosterone): Epididymis, ductus deferens, seminal vesicle, ejaculatory duct.
- ♀: Degenerates (Gartner's duct).
- Paramesonephric (Mullerian) Duct:
- ♀: Fallopian tubes, uterus, upper vagina.
- ♂ (AMH from Sertoli): Degenerates (appendix testis, prostatic utricle).
- Ureteric Bud (from Mesonephric Duct): Ureter, pelvis, calyces, collecting ducts.
- Interacts with metanephric mesenchyme.
- Bladder & Urethra:
- Urogenital Sinus (endoderm): Forms most of bladder, urethra.
- Trigone (mesoderm): From incorporated caudal mesonephric ducts.
- Urachus (allantois remnant) → median umbilical ligament.
⭐ A persistent urachus can lead to a urachal fistula (urine discharge from umbilicus), urachal sinus, or urachal cyst.
- Key Anomalies:
- Ureteropelvic Junction (UPJ) obstruction (commonest neonatal hydronephrosis).
- Duplex/ectopic ureter. Bladder exstrophy. Urachal defects.

Gonadal Development - Germ Cell Jamboree
- Primordial Germ Cells (PGCs):
- Origin: Epiblast (Wk 2) → Yolk sac (Wk 3).
- Migration: Dorsal mesentery → Gonadal ridges (Wk 5-6). 📌 PGCs "germinate" from yolk sac.
- Indifferent Gonad (Bipotential Stage):
- Gonadal ridge (from mesonephros) forms primitive sex cords.
- Undifferentiated until Week 7.
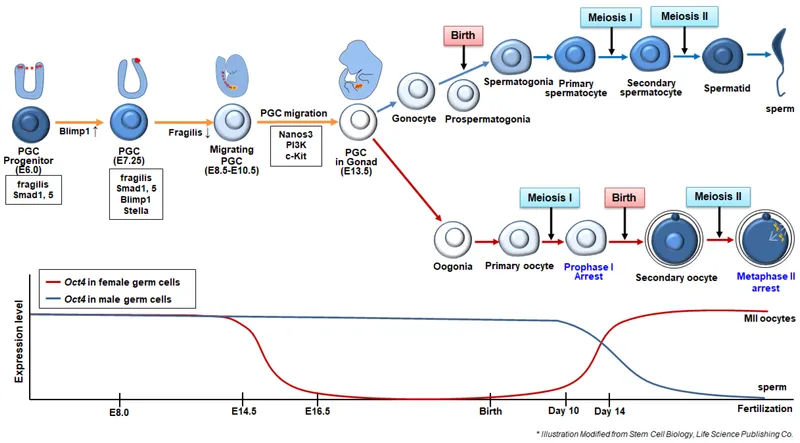
- Sex Determination:
⭐ The SRY gene (Sex-determining Region on Y chromosome) is the Testis Determining Factor (TDF) and is essential for initiating male gonadal differentiation into testes around the 7th week.
- Testis Development (SRY+):
- Primitive sex cords → Seminiferous cords. Sertoli cells (AMH). PGCs → Spermatogonia.
- Mesenchyme → Leydig cells (Testosterone from Week 8).
- Ovary Development (SRY-):
- Primitive sex cords degenerate.
- Cortical cords (from surface epithelium) → Follicular cells; PGCs → Oogonia.
External Genitalia - Finishing Touches
- Indifferent Stage (common primordia until ~7th week):
- Genital Tubercle
- Urogenital (Urethral) Folds
- Labioscrotal (Genital) Swellings
- Male Development (Dihydrotestosterone - DHT dependent):
- Genital Tubercle → Elongates to form phallus (glans & shaft of penis)
- Urogenital Folds → Fuse ventrally → Penile urethra (corpus spongiosum)
- Labioscrotal Swellings → Fuse → Scrotum
- Female Development (Estrogen influence, absence of DHT):
- Genital Tubercle → Clitoris
- Urogenital Folds → Remain unfused → Labia minora
- Labioscrotal Swellings → Remain unfused → Labia majora, mons pubis
⭐ Hypospadias, a common congenital anomaly, results from failure of the urethral folds to fuse on the ventral aspect of the penis; epispadias involves a urethral opening on the dorsal aspect.
High‑Yield Points - ⚡ Biggest Takeaways
- Mesonephric (Wolffian) duct forms male internal genitalia: epididymis, vas deferens, seminal vesicles, ejaculatory duct.
- Paramesonephric (Mullerian) duct forms female internal genitalia: fallopian tubes, uterus, upper vagina.
- Ureteric bud forms the kidney's collecting system: collecting ducts, calyces, renal pelvis, and ureter.
- Metanephric blastema (mesenchyme) forms nephrons from the glomerulus to the distal convoluted tubule.
- The SRY gene on the Y chromosome is crucial for testicular differentiation and subsequent male development.
- The cloaca divides into the urogenital sinus (future bladder, urethra) and the anorectal canal.
- The gubernaculum guides the descent of the testes in males and the ovaries in females.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

